INTRODUCTION
The Canadian Association of Emergency Physicians (CAEP) Academic Section was created in 2013 to promote high-quality emergency patient care through education and research. Improvements in emergency medicine practice benefit all Canadians, as the emergency department (ED) is often the access point to the medical system.
Emergency medicine is a relatively new specialty in Canada, with the first certificates being awarded by the Royal College of Physicians and Surgeons of Canada in 1983.1,2 For this young, rapidly growing specialty, it is essential that resources and infrastructure are available to help academic programs further develop, and to prepare our physicians, leaders, researchers, and educators to meet the many challenges of emergency care. Not only are there new diagnostic tools and procedures to incorporate into practice, but there are also pressures, including ED crowding, an aging population, and resource limitations. Canadians will benefit from an investigation of the current resources allotted to our academic emergency medicine programs, where young clinicians are trained and new evidence generated. These programs are integral to improving the emergency health care of Canadians, who benefit from well-trained physicians, continuing education for these physicians, and high-quality evidence generated by clinician scientists.
There are four major areas of focus to support the mission of university academic departments: administration/leadership, education, research, and funding. The variability in infrastructure, support, and productivity of emergency medicine research programs across Canada was discussed at the 2014 CAEP Academic Symposium on Research, where recommendations were refined and published to improve research funding, resident research, and training for career researchers.Reference Stiell, Artz and Perry 3 - Reference Calder, Abu-Laban and Artz 6 The importance of education and its development was addressed at the 2013 CAEP Academic Section Consensus Conference on Education Scholarship. Recommendations centered on improvements to teaching and learning, as well as the support and development of education scholars.Reference Sherbino, Van and Bandiera 7 - Reference Bhanji, Cheng and Frank 9 Although the need for these recommendations is generally accepted among academics, an environmental scan that characterizes each medical school in the areas of leadership/administration, education, research, and funding will clearly articulate the specific strengths to build on and weaknesses to address. Key areas to investigate include the overarching administration of the academic unit to ensure that there is strength in the emergency medicine voice within the university. Funding and access to the resources for education and research are necessary to achieve an effective academic unit.
The mission of the CAEP Academic Section is threefold: 1) to improve emergency care of patients by enhancing academic emergency medicine primarily at Canadian medical schools and teaching hospitals; 2) to foster and develop education, research and academic leadership amongst Canadian emergency physicians, residents and students; and 3) to provide mentorship in academic emergency medicine. Two specific objectives within the Section’s Terms of Reference are to: 1) create a database of academic activities, physician leaders, infrastructure, and resources at each Canadian medical school; and 2) support academic emergency departments, divisions, or units at each medical school and teaching hospital to ensure appropriate status, resources, and infrastructure. Towards achieving these goals and to better understand local strengths and weaknesses, we conducted an environmental scan of academic emergency medicine activities at all Canadian medical schools and major teaching hospitals.
METHODS
We developed an 84-question questionnaire, focusing on the four domains of governance/administration, education, research, and funding (see Appendix). The questionnaire was comprised of yes/no and numerical responses as well as boxes for comments, pilot tested amongst members of the CAEP Academic Section Executive, and revised for clarity. The final questionnaire was distributed electronically to the heads (or equivalent) of each emergency medicine unit at the 17 Canadian medical schools. While we identified the presence of pediatric emergency medicine at the universities, we did not collect detailed information about these units. We plan to do so in the near future. University of Ottawa staff members conducted follow-up calls to ensure that all of the questions were answered and recorded into a Microsoft Excel® 2013 (Microsoft Corp., Redmond, WA) spreadsheet for analysis. The lead author (IS) validated the individual site data with each head (or equivalent) in a series of one-hour telephone discussions. Descriptive statistics including proportions, means, medians, and ranges were calculated. Data collection was complete except that one site was unable to provide funding data.
RESULTS
While emergency medicine has full departmental status at eight of 17 universities, it has no academic designation at two others (Table 1). We also note that pediatric emergency medicine has university status at 65% of Canadian medical schools. Canadian academic emergency medicine is conducted at 46 major teaching hospitals (defined as those that have a full complement of residency programs and a research institute) and at a further 13 specialized pediatric hospitals (Table 2). Another 69 Canadian hospital EDs regularly take clinical clerks and emergency medicine residents. There are 31 full professors of emergency medicine in Canada, representing 2% of physicians at major teaching hospitals.
Table 1 University status of emergency medicine at the 17 Canadian medical schools.
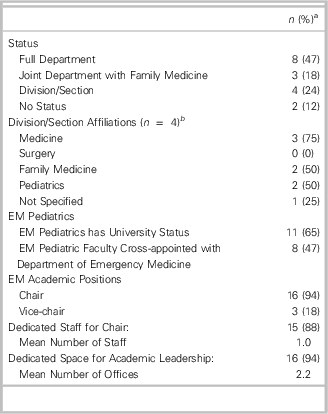
a Percentages may not add up to 100% due to rounding.
b Three respondents reported multiple affiliations.
Table 2 Teaching hospitals and emergency medicine faculty at the 17 Canadian medical schools.

a Major teaching hospitals defined as those that have a full complement of residency programs and a research institute.
Teaching programs are a mainstay of academic emergency medicine in Canada, with clerkships offered at 16/17 of universities, CCFP(EM) programs at 17/17, and RCPSC residency programs at 14/17 (Table 3). All medical schools offer emergency training for off-service residents and 11/17 offer specialized fellowship training.
Table 3 Undergraduate, residency, and fellowship programs at the 17 Canadian medical schools.

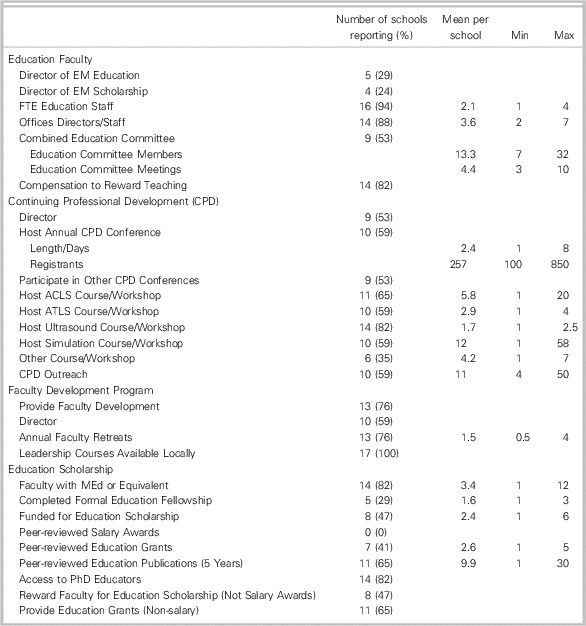
Continuing professional development (CPD) and education scholarship are two important domains in Canadian academic emergency medicine (Table 4). Ten sites report hosting an annual CPD conference for community physicians, and 13 have faculty development programs for their own physicians. While only four sites have a designated director of education scholarship, 14 have at least one physician with a Master’s degree in education. Across Canada there is only a modest output of education publications.
Table 4 Education scholarship and CPD at the 17 Canadian medical schools.
Research activity is considered to be a key indicator of academic performance, and there are now 55 researchers with salary support, based at 13 universities (Table 5). Amongst these, 17 currently have peer-reviewed salary awards and 48 grants are held from Canadian Institutes of Health Research or Heart and Stroke Foundation of Canada. Sixteen sites have published peer-reviewed papers in the past five years, ranging from four to 235 per site.
Table 5 Research activities and resources at the 17 Canadian medical schools.

Sixteen sites were able to share details of their academic funding (Table 6), and we can see that the annual budget ranges greatly, from $200,000 to $5,900,000, a far greater range than would be expected from the size of the programs. Sources of funding also vary greatly, with 10 sites receiving support from a provincial alternate funding plan, and university contributions ranging from 2% to 100% of local budgets.
Table 6 Funding for academic activities at the 17 Canadian medical schools.
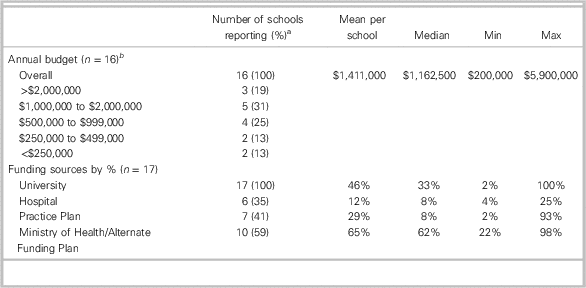
a Percentages may not add up to 100% due to rounding.
b One medical school did not provide an annual budget, but did supply their funding resources by percent.
DISCUSSION
This report is the first comprehensive review of academic emergency medicine activities at Canadian medical schools and major teaching hospitals. A report on pediatric emergency medicine will be forthcoming. We found that emergency medicine has a strong presence in patient care and teaching at all 17 Canadian medical schools. While university status varies across the country, sites are actively involved in teaching: undergraduate clerkship programs (16), CCFP(EM) residency programs (17), RCPSC residency programs (14), off-service residents (17), fellowships (11), and CPD (10). Education scholarship is becoming well established, with half of sites providing salary support for this endeavor. Peer-reviewed metrics for education scholarship in emergency medicine are weak overall, but there are some very strong sites. Clinical researchers in emergency medicine have protected time at three-quarters of Canadian sites, and some groups have been very successful with peer-reviewed funding and publications. Academic activities require adequate funding, and we can see that there is a twenty-fold range in annual budgets amongst universities. Those with provincial alternate funding programs often have the strongest funding. Overall, this report has found a great many strengths in Canadian academic emergency medicine, along with weaknesses and opportunities for improvement.
Emergency medicine is a relatively new discipline, with specialty status being recognized in the early 1980s (U.S. and Canada) and 1990s (UK, Australia, New Zealand). Our report shows how far Canadian academic emergency medicine has come in thirty years, but also how far it has yet to go to be on an equal footing with more traditional specialties like medicine and surgery. There are relatively few full professors of emergency medicine, with some universities having none. While teaching activities are very strong across Canada, education scholarship and research have much room for growth at many sites. In only a few Canadian universities would emergency medicine be considered a strong academic performer.
Our scan found a range of university governances, with 47% of emergency medicine units reporting full departmental status and 12% reporting no status at all. The three Quebec Francophone universities are unique in that they have combined Departments of Family and Emergency Medicine (Départements de médecine familiale et de la médecine d’urgence). US data show that establishment of academic departments of emergency medicine is strongly associated with many positive academic metrics.Reference Gallagher and Henneman 10 , Reference Derlet 11 Emergency medicine academic activity appears to have matured more rapidly in the US compared to Canada.Reference Gallagher 12 The current report will serve as a benchmark against which to judge future progress of academic emergency medicine in Canada.Reference Carpenter, Cone and Sarli 13
Moving forward, we hope that lessons learned from the more successful sites can be used to assist those that want to improve upon their present circumstances. Each emergency unit can know how it compares to the national average, can identify their areas of relative weakness, and can set priorities for change. In some cases these data can be used in discussions with university leadership to argue for stronger status, higher budgets, or more teaching and research positions. Towards this end, CAEP has recently agreed to help fund consultations for Canadian academic units, with expertise being provided by the Academic Section in governance funding, education scholarship, and research. 14
Why do our findings matter to Canadian emergency physicians? Academic emergency medicine, based at the universities and teaching hospitals, has a very broad influence on ED care across the country. All emergency physicians, of course, went to medical school and undertook postgraduate training, primarily at these Canadian centres. Many ED physicians, even in small hospitals, are actively involved in teaching our current medical students and residents. The academic centres produce the latest information on teaching methods and provide ongoing CPD for community physicians. New advances in patient care are developed through clinical research at the university sites and disseminated through traditional publications and presentations, as well as through social media.
In conclusion, this report provides a comprehensive review of academic activities in emergency medicine across Canada, identifying areas of strengths as well as many opportunities for improvement. CAEP and the Academic Section hope we can learn from each other and, by sharing best academic practices, become stronger teachers, educators, and researchers, and ultimately improve patient care in our EDs.
Acknowledgments
We particularly thank three staff members from Ottawa who worked tirelessly to obtain responses from each medical school (Angela Marcantonio, Ann Kasaboski, Rachel Baril) and Kelly Wyatt from CAEP for arranging telephone interviews. In addition, we are very grateful for the cooperation of emergency medicine leaders from each university: British Columbia (Jim Christenson), Alberta (Brian Holroyd, Brian Rowe), Calgary (Eddy Lang, Grant Innes), Saskatchewan (James Stempian, Rob Woods), Manitoba (Alecs Chochinov), Northern Ontario (Gary Bota, Lee Toner), Western (Gary Joubert, Shelley McLeod), McMaster (Margaret Ackerman), Toronto (Anil Chopra, Eric Letovsky, Laurie Morrison), Queens (Gord Jones), Ottawa (Ian Stiell), McGill (Jean-Marc Troquet, Marc Afilalo), Montreal (Pierre Désaulniers, Jean Pelletier), Laval (Renée Turgeon), Sherbrooke (Marie Giroux), Dalhousie (David Petrie), and Memorial (Tia Renouf).
Competing Interests: None declared.
Supplementary Material
To view supplementary material for this article, please visit http://dx.doi.org/10.1017/cem.2016.346










