Molecular Nutrition
Full Papers
Long-term chronic caloric restriction alters miRNA profiles in the brain of ageing mice
-
- Published online by Cambridge University Press:
- 07 April 2021, pp. 641-652
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Metabolism and Metabolic Studies
Full Papers
Bacillus amyloliquefaciens ameliorates high-carbohydrate diet-induced metabolic phenotypes by restoration of intestinal acetate-producing bacteria in Nile Tilapia
-
- Published online by Cambridge University Press:
- 16 April 2021, pp. 653-665
-
- Article
-
- You have access
- HTML
- Export citation
Myo-inositol improves growth performance and regulates lipid metabolism of juvenile Chinese mitten crab (Eriocheir sinensis) fed different percentage of lipid
-
- Published online by Cambridge University Press:
- 29 April 2021, pp. 666-678
-
- Article
-
- You have access
- HTML
- Export citation
Genetically determined variations of selenoprotein P are associated with antioxidant, muscular, and lipid biomarkers in response to Brazil nut consumption by patients using statins
-
- Published online by Cambridge University Press:
- 05 May 2021, pp. 679-686
-
- Article
-
- You have access
- HTML
- Export citation
Acute exercise improves glucose and TAG metabolism in young and older adults following high-fat, high-carbohydrate meal intake
-
- Published online by Cambridge University Press:
- 17 June 2021, pp. 687-695
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Human and Clinical Nutrition
Full Papers
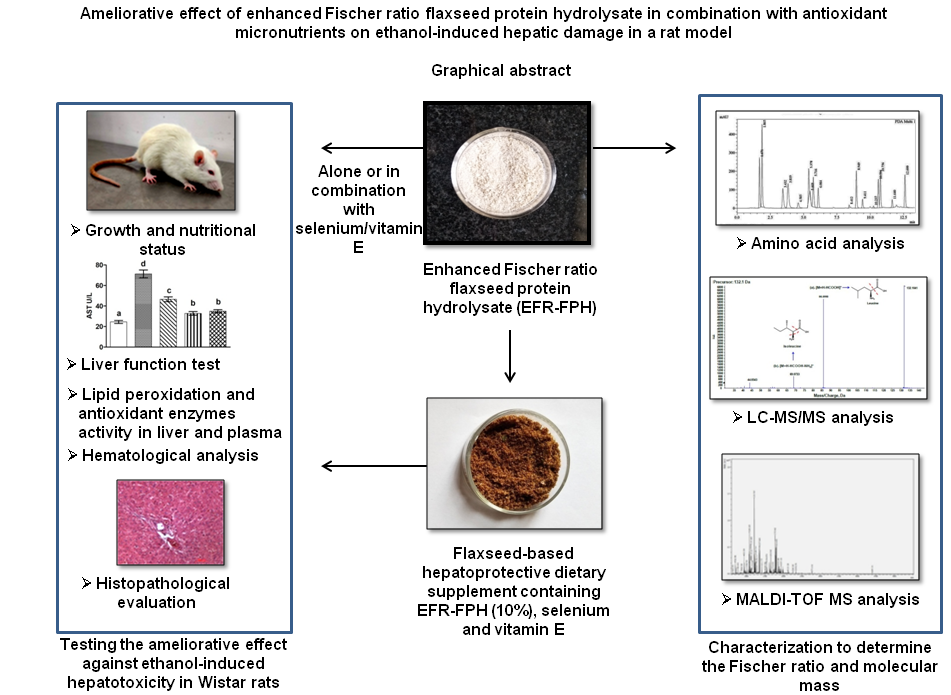
Ameliorative effect of enhanced Fischer ratio flaxseed protein hydrolysate in combination with antioxidant micronutrients on ethanol-induced hepatic damage in a rat model
-
- Published online by Cambridge University Press:
- 05 April 2021, pp. 696-710
-
- Article
-
- You have access
- HTML
- Export citation
Homogenised and pasteurised human milk: lipid profile and effect as a supplement in the enteral diet of Wistar rats
-
- Published online by Cambridge University Press:
- 27 April 2021, pp. 711-721
-
- Article
-
- You have access
- HTML
- Export citation
The use of alternate vertebral levels to L3 in computed tomography scans for skeletal muscle mass evaluation and sarcopenia assessment in patients with cancer: a systematic review
-
- Published online by Cambridge University Press:
- 29 April 2021, pp. 722-735
-
- Article
-
- You have access
- HTML
- Export citation
Reflecting on ‘Selenium in Global Food Systems’
-
- Published online by Cambridge University Press:
- 15 November 2021, pp. 736-738
-
- Article
-
- You have access
- HTML
- Export citation
Policy-Relevant Paper
Diagnosing undernutrition children and adults: new French criteria. Why, for what and for whom? A joint statement of the French National Authority for Health and French Federation of Nutrition
-
- Published online by Cambridge University Press:
- 07 May 2021, pp. 739-751
-
- Article
-
- You have access
- HTML
- Export citation
Dietary Surveys and Nutritional Epidemiology
Full Papers
Consumption of dairy products and CVD risk: results from the French prospective cohort NutriNet-Santé
-
- Published online by Cambridge University Press:
- 29 April 2021, pp. 752-762
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Dietary patterns of 5-year-old children and their correlates: findings from a multi-ethnic Asian cohort
-
- Published online by Cambridge University Press:
- 29 April 2021, pp. 763-772
-
- Article
-
- You have access
- HTML
- Export citation
The relationship between Dietary Inflammatory Index and disease severity and inflammatory status: a case–control study of COVID-19 patients
-
- Published online by Cambridge University Press:
- 23 August 2021, pp. 773-781
-
- Article
-
- You have access
- HTML
- Export citation
Behaviour, Appetite and Obesity
Full Papers
The effects of different temperatures of post-exercise protein-containing drink on gastric motility and energy intake in healthy young men
-
- Published online by Cambridge University Press:
- 27 April 2021, pp. 782-790
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Food sources of iodine in schoolchildren and relationship with 24-h urinary iodine excretion in Victoria, Australia
-
- Published online by Cambridge University Press:
- 29 April 2021, pp. 791-799
-
- Article
-
- You have access
- HTML
- Export citation
Corrigendum
Diagnosing undernutrition children and adults: new French criteria. Why, for what and for whom? A joint statement of the French National Authority for Health and French Federation of Nutrition – Corrigendum
-
- Published online by Cambridge University Press:
- 25 November 2021, p. 800
-
- Article
-
- You have access
- HTML
- Export citation
Front Cover (OFC, IFC) and matter
BJN volume 127 issue 5 Cover and Front matter
-
- Published online by Cambridge University Press:
- 25 February 2022, pp. f1-f2
-
- Article
-
- You have access
- Export citation
Back Cover (OBC, IBC) and matter
BJN volume 127 issue 5 Cover and Back matter
-
- Published online by Cambridge University Press:
- 25 February 2022, pp. b1-b2
-
- Article
-
- You have access
- Export citation