Clinical scenario
You are a core trainee in a community mental health team, working in an out-patient clinic. You come out to call your next patient when you see a 40-year-old woman lying on her back on the ground with her eyes closed in the waiting room, with people crowding around her. The receptionist informs you that she arrived a few minutes late in a distressed state and was asked to take a seat. Within a minute she was seen slumping in her chair and then sliding down to the ground, jerking all four limbs while crying. When you approach her and try to talk, she responds to your questions and soon opens her eyes and her shaking stops, but she then slips back into jerking all four limbs again. You see on her wrist that she has a medical alert bracelet, which reads ‘medical alert: non-epileptic attacks’.
• What would be your immediate management of the situation?
• What are the principles of assessment and management in functional non-epileptic attacks (FNEA)?
• What are the differences between epileptic seizures and non-epileptic attacks?
Evidence base in FNEA
FNEA are when people present with what looks like epileptic seizures but they do not have epilepsy or associated electroencephalogram (EEG) changes or a physiological condition that may mimic seizures such as syncope. This condition is also known as psychogenic non-epileptic seizures (PNES), non-epileptic attack disorder (NEAD), psychogenic seizures, hysterical seizures and so on. In ICD-10 (1992) they are classified as ‘dissociative convulsions’, in ICD-11 (2018) as ‘dissociative neurological symptom disorder’ and in DSM-5 (2013) as ‘functional neurological symptom disorder – with attacks or seizures’. The change in terminology over the years reflects the changes in theoretical underpinning and clinical understanding. FNEA have been described in multiple cultures without a specific diagnostic label for 4000 years, the term hysteria was then used for the next 2500 years,Reference Trimble and Reynolds1 followed by conversion, dissociation and now FNEA, which is theoretically neutral from a psychological standpoint and considered to be acceptable to patients.Reference Ding and Kanaan2
FNEA are commonly seen in neurological and accident and emergency (A&E) settings. Up to one in five patients in epilepsy clinics present with FNEA and 20–40% of patients in epilepsy-monitoring in-patient units have FNEA.Reference Asadi-Pooya and Sperling3 These patients or their carers will often initially call an ambulance and present to A&E departments. Indeed, nearly a quarter of FNEA patients report an episode of FNEA status,Reference Asadi-Pooya, Emami, Emami and Sperling4 which may in some cases even lead to intubation in the intensive treatment unit. The estimated prevalence of FNEA is 2–30/100 000 in the general populationReference Benbadis and Allen-Hauser5 and population incidence has been estimated to be 1.4–4.9/100 000/year.Reference Asadi-Pooya and Sperling3 By contrast, the median estimated population incidence of multiple sclerosis is 4.2/100 000/year and that of epilepsy is 48/100 000/year.Reference Hirtz, Thurman, Gwinn-Hardy, Mohamed, Chaudhuri and Zalutsky6 FNEA most commonly present in young adulthood and in women, but can occur in children, older adults and men.Reference Asadi-Pooya and Sperling3
The aetiology of FNEA, as with functional neurological disorders in general, is thought to be multifactorial. Risk factors include female gender, childhood abuse and neglect, avoidant coping styles, previous functional disorders and somatisation, and recent stressful event which may itself be ‘organic’ – such as a head injury or syncope.Reference Bodde, Brooks, Baker, Boon, Hendriksen and Mulder7 In addition, FNEA are associated with neuropsychological deficits and alexithymia.Reference Bodde, Brooks, Baker, Boon, Hendriksen and Mulder7 Often overlooked is a family history of functional disorders, although there have been no positive genetic findings to date.Reference Frodl8 There is an association with personality disorder, especially cluster B and cluster C personality disorders,Reference Lacey, Cook and Salzberg9 and a number of patients have other psychological comorbidities such as affective disorders and anxiety disorders,Reference Kanner, Schachter, Barry, Hersdorffer, Mula and Trimble10 which may act as predisposing, precipitating or perpetuating factors. Symptoms of panic and dissociation are common leading up to an attack, and patients may even ‘bring on’ an attack to rid themselves of these symptoms.Reference Stone and Carson11
Distinguishing epileptic from non-epileptic attacks can be difficult, and it is important to remember that there are no clinical signs that never occur in epilepsy, and the only certain diagnostic feature of epileptic versus non-epileptic attacks is video EEG (vEEG) confirming epileptic or non-epileptic seizures.Reference Kanner, Schachter, Barry, Hersdorffer, Mula and Trimble10 If this shows the absence of epileptiform activity in the presence of the patient's typical attacks, it confirms the diagnosis of FNEA. vEEG is of course only diagnostic if the attack occurs during monitoring and can be falsely negative on scalp EEG if there is an ictal focus deep in the frontal lobe. However, vEEG is expensive and is carried out in only some cases. Diagnosis is largely clinical, based on good history and clinical observation of an attack, ideally supplemented by clinician-viewed video of the attack. Table 1 helps distinguish clinical features of epileptic versus non-epileptic attacks, but should not be used in isolation to make a diagnosis either way.
Table 1 Distinguishing clinical features in FNEA and epilepsy.
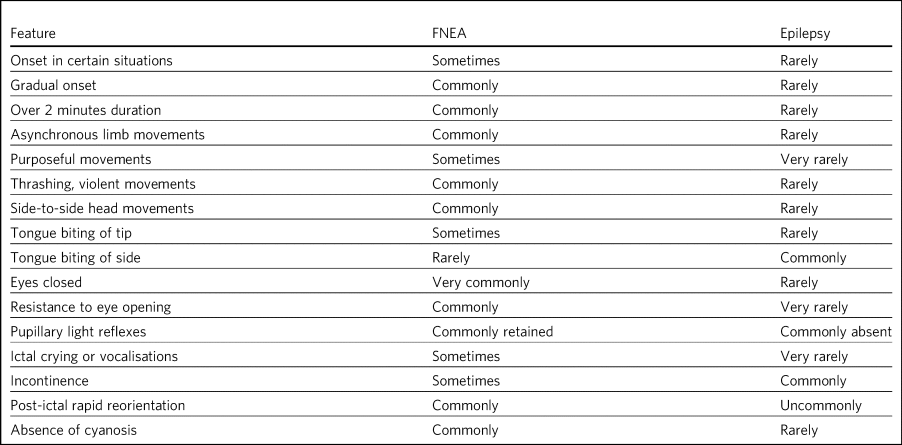
Adapted from Reuber & ElgerReference Reuber and Elger12 and Mellers.Reference Mellers13 FNEA, functional non-epileptic attacks.
Confusingly, some patients with epileptic seizures may also have non-epileptic attacks. What is important in this case is the semiology (clinical features of the seizure) and whether it is different from the patient's normal epileptic seizures. Epileptic seizures tend to be short, stereotyped and highly consistent, although of course they can take different forms in the same patient, e.g. simple and complex. However, in the case of the emergence of a new seizure type in a patient with stable epilepsy, FNEA should be considered.
In terms of prognosis and outcomes, data suggest that 4 years after diagnosis around a third of patients will be attack free.Reference Reuber, Mitchell, Howlett and Elger14 However, being attack free alone does not result in greatly improved levels of psychopathology or recovery of social function, as nearly half of patients who are attack free are still in receipt of state benefits.Reference Reuber, Mitchell, Howlett and Elger14 These data suggest that social interventions aimed at recovery of social function, e.g. going back to work, may be efficacious in improving quality of life more than aiming for patients to be attack free; however there are no studies examining social interventions alone and this is a gap in the literature. Furthermore, there is a general lack of long-term follow-up studies of patients with FNEA. Features associated with a favourable prognosis include lack of past psychiatric history, identifiable recent stressor, short duration of FNEA, higher socioeconomic class, normal IQ, lower age, less vigorous seizures, absence of comorbid epilepsy and no ongoing use of anticonvulsant medication.Reference Bodde, Brooks, Baker, Boon, Hendriksen and Mulder7,Reference Reuber and Elger12
Multiple treatments have been trialled including cognitive–behavioural therapy (CBT) (both individual and group based), paradoxical treatment, psychodynamic therapy, group therapy, family therapy, case management, eye movement desensitisation and reprocessing, acceptance and commitment therapy and multimodular approaches.Reference Bodde, Brooks, Baker, Boon, Hendriksen and Mulder7,Reference Reuber and Elger12,Reference Cope, Mountford, Smith and Agrawal15–Reference Agrawal, Gaynor, Lomax and Mula18 However, the evidence base is hampered by lack of control groups, small numbers of patients in trials and also the highly variable population and presentation of FNEA. We would suggest that the individualised treatment approach as described in 2014 by Agrawal et al Reference Agrawal, Gaynor, Lomax and Mula18 helps address this problem of the high variability in FNEA patients.
The problem of small numbers in treatment trials is also being addressed: The largest randomised controlled trial (RCT) to date is in CBT. Goldstein et al Reference Goldstein, Chalder, Chigwedere, Khondoker, Moriarty and Toone19 conducted an RCT of CBT versus standard medical care (SMC), with 33 patients in both arms, and seizure frequency reduced significantly in the CBT arm. However, the statistical power reduced significantly (P = 0.086) due to patients being lost to follow-up. This CBT trial was extended and repeated and is currently evaluating data as the ‘COgnitive behavioural therapy versus standardised medical care for adults with Dissociative non-Epileptic Seizures’ (CODES) trial.Reference Goldstein, Mellers, Landau, Stone, Carson and Medford20 It aimed to allocate around 150 patients to each arm – SMC and SMC with CBT – and is due to report.
Only one double-blind placebo RCT of treatment has been published in FNEA, and this was of sertraline versus placebo.Reference LaFrance, Keitner, Papandonatos, Blum, Machan and Ryan21 A total of 33 patients were assessed and a non-significant reduction in seizure frequency was found in the sertraline versus placebo group. This was a feasibility study for a larger RCT which, to date, has not been undertaken.
Assessment of FNEA
There are some key elements to the assessment of FNEA that should never be forgotten.
(1) A clear history from both patient and an informant, ideally supplemented by video of the attack itself, is invaluable. Patients with non-epileptic attacks tend to talk about attacks in a different way to those with epilepsy (for example, talking about seizures by total negation and without context, i.e. ‘I feel nothing’, ‘I don't know anything has happened’), whereas those with epilepsy try to give detailed explanations of what they did experience before or after.Reference Plug and Reuber22 It is important to get a clear understanding of how the family react when a non-epileptic attack occurs as, in some cases, they may inadvertently be reinforcing or maintaining the attacks.
(2) A good history is essential, especially for any recent stressful events. Some patients' attacks are clearly temporally related to a stressful event, although this is no longer required for diagnosis.
(3) A full psychiatric history is required, assessing both past and current mental illness. Both patients with epilepsy, and with FNEA are more likely than the general population to have higher rates of depression and anxiety.Reference Kanner, Schachter, Barry, Hersdorffer, Mula and Trimble10 Treatment of any comorbidities is an important part of treatment for FNEA as – although the data are limited by small numbers – comorbid prevalence rates of 63% with affective disorders, 46% with personality disorders, 32.5% with somatoform disorders, and 19% with both anxiety disorders and post-traumatic stress disorder (PTSD) have been reported.Reference D'Alessio, Giagante, Oddo, Silva, Solís and Consalvo23
(4) A thorough general medical history must be taken. Patients with non-epileptic attacks have been found to be more likely than patients with epilepsy to have functional or medically unexplained symptoms in different organ systems, such as fibromyalgia, chronic pain and irritable bowel syndrome.Reference Dixit, Popescu, Bagić, Ghearing and Hendrickson24 The most common symptom combination distinguishing FNEA from epileptic seizures in one tertiary centre study was chronic pain, migraines and asthma in FNEA compared with diabetes and non-metastatic neoplasm in epilepsy.Reference Kerr, Janio, Braesch, Le, Hori and Patel25
(5) Determine the personal and social history of the patient. Patients with non-epileptic attacks are much more likely to report a history of abuse or neglect in childhood, and this should be sensitively asked about along with usual information such as birth trauma, developmental milestones, head injuries and details of schooling and relationships. Importantly however, some will not have this history of abuse or neglect. In some cases this may need to be asked about after developing rapport with the patient. They should also be asked whether they are still driving.
(6) The premorbid personality should be ascertained. Patients with non-epileptic attacks are more likely to have a personality disorder than the general population, especially cluster B and cluster C personality disorders, although there are methodological problems with much research in this area.Reference Lacey, Cook and Salzberg9,Reference D'Alessio, Giagante, Oddo, Silva, Solís and Consalvo23
(7) The patient's illness beliefs, concerns, wishes and expectations should be ascertained. Research has shown that patients who are confident in the diagnosis of FNEA have a better outcome.Reference Gelauff and Stone26 Lasting doubts about epilepsy should be dispelled and it must be emphasised that this condition is treatable and many patients fully recover.
(8) Finally, a biopsychosocial formulation encompassing the above factors should be composed, using predisposing, perpetuating, precipitating and protective format. This will guide management.
Box 1 Patient experience of functional non-epileptic attacks
My dissociative seizures (NEAD) were precipitated by an episode of moderate depression and its treatment with Sertraline on transition to university. I also was experiencing panic disorder, GAD and depersonalisation–derealisation disorder.
Everyone was very panicked by my first seizures. I visited several A&E departments, had numerous ambulance visits and was bounced between psychiatric liaison, the A&E staff and the CMHT, even having an overnight stay in AMU. No one could give me a concrete diagnosis, or know where to refer me. I was dosed up on benzodiazepines, which did not stop the seizures, and just made the experience harder to cope with. I experienced PTSD following the traumatic nature of these interventions; and they were completely needless.
Psychiatrists at CMHT seemed very worried, even more so than I was, and this compounded the stress that was prolonging my condition. They were, however, helpful in sourcing CBT to treat my anxiety and depression.
Six months after my first seizure, I was officially diagnosed with dissociative seizures. The reassurance of a diagnosis itself, along with further research into the condition, was enough alone to cause a noticeable decrease in the severity of my seizures.
I then saw Dr Sheldon & Dr Agrawal at St George's. Dr Agrawal drew a diagram explaining how stress can build to cause my seizures, and I used a CBT diary to identify triggers over two months. I surprised myself with the diversity and number of my triggers on reviewing my diary, which I now manage.
A greater understanding of my condition gained through psychoeducation, and the use of grounding, distancing and distracting techniques, have all been instrumental in my recovery. I am now discharged, and almost seizure-free. I wonder how much better my experience could have been if doctors had known how to treat my acute presentation?
A&E, accident and emergency; AMU, acute medical unit; CBT, cognitive–behavioural therapy; CMHT, community mental health team; GAD, generalised anxiety disorder; NEAD, non-epileptic attack disorder; PTSD, post-traumatic stress disorder.
Management
The management for all patients will naturally be different due to the different nature of their attacks and their individual triggers, but there are important overarching principles. These include making the diagnosis clearly and early (and ideally soon coming off anticonvulsants); biopsychosocial formulation including the role others play in reaction to attacks; psychoeducation about non-epileptic seizures; the management of comorbidities; the development of personal insight and understanding triggers to attacks (which can be achieved by things such as attack diaries); offering trauma-focused therapy if appropriate; and the personal testing and utilisation of different techniques such as grounding, relaxation and mindfulness. The use of benzodiazepines and anticonvulsants can be harmful both in the short and longer term. An overview of one such pragmatic, individualised treatment pathway is provided in Agrawal et al.Reference Agrawal, Gaynor, Lomax and Mula18
The diagnosis should in most cases be made by a neurologist. However, many patients will benefit from neuropsychiatry-led sensitive and detailed exploration of illness beliefs, further explanation of the diagnosis and psychoeducation about triggers and management strategies. In some cases, patients will have been on anticonvulsants and will have lived with negative side-effects for years, not to mention the stigma of epilepsy and practical handicaps from the condition, such as being unable to drive. Some patients may only require a clear, sensitive diagnosis for the FNEA to stop; however, these patients are thought to be in the minority. In any case, the way a diagnosis is made is important (Box 1).
Four models about conveying a diagnosis have been published.Reference Mellers13,Reference Shen, Bowman and Markand27–Reference Hall-Patch, Brown, House, Howlett, Kemp and Lawton29 However, what is common between models are the principles of reassurance; discontinuation of anticonvulsants; providing a type of model for how FNEA come about – including the relationship with emotions; and that although symptoms are not consciously controlled, patients can learn to identify triggers for seizures and learn to intervene.
People with FNEA will ideally be seen by a psychiatrist with experience of the assessment of FNEA and epilepsy, i.e. a neuropsychiatrist. The multidisciplinary team is often helpful, for example in discussing difficult formulations, and the team can offer individual therapy tailored towards the FNEA or underlying factors as appropriate. Enough time should be set aside in clinic to explore symptoms and history as well as management. The clinic letter can itself be a useful tool to explore illness beliefs at the next consultation.
Whether or not patients should remain on the neurological caseload is an interesting topic and how helpful this is has not been explored prospectively. Given some of the similarities in interpersonal interactions with borderline personality disorder and patients with FNEA, some believe that consistency is key and patients should be kept in follow-up and that discharge should be slow and gradual.Reference Lacey, Cook and Salzberg9 Indeed, patients with FNEA often struggle to fit in within both neurology and psychiatry services and they bounce between teams with clinicians reluctant to take responsibility, similar to those with personality disorders in psychiatric services.
In an acute situation such as the above, the importance is in differentiating from an epileptic seizure. First, getting people to stand aside and leave the area is important to be able to assess the patient and manage the scenario. If your assessment is that this is a non-epileptic seizure, which from the description is likely, then some techniques can be used to arrest the seizure. For example, if a small mirror (or the front-facing camera on a smartphone) is brought to the patient's face, observe if the pupils converge on it (this is highly unlikely in an epileptic seizure). This mirror technique can in some cases stop the FNEA.Reference Mellers13 However, if this is unsuccessful, it does not mean that this is not a functional seizure. If the patient's eyes are closed, it can be helpful to open their eyes to see if they resist eye opening, which would be very unusual in an epileptic seizure. If the patient can be spoken to and they respond emotionally to your voice (which, again, is common in FNEA), then you can talk to them and calm them. You could try asking them to tell you the day of the week, and to open their eyes and look at something in the room and describe it in detail. An example of such a grounding technique might be: ‘tell me three things you can see, two things you can hear, one thing you can smell’. If the situation continues despite your best efforts, then be reassured the FNEA will stop eventually. It would be helpful to still see the patient despite the attack in the waiting room, if time allows. What is key is that the ambulance should not be called – unless the patient has seriously injured themselves – as a result of the FNEA and no acute pharmacological treatment is indicated.
Such acute treatment may not only reinforce a need for benzodiazepines or anticonvulsants, but has the potential to increase levels of dissociation by reducing alertness. Indeed it has been postulated that the variation in FNEA symptoms is due to the effect of anticonvulsantsReference Krumholz and Niedermeyer30 and that other drugs inducing altered awareness states, such as anaesthetic agents, can induce FNEA.Reference Lichter, Goldstein, Toone and Mellers31
Patients may ask about driving. Current Driver and Vehicle Licensing Agency (DVLA) guidance in the UK dictates that people with FNEA should cease driving and inform the DVLA of their condition. To resume driving, people with FNEA should have episodes that are ‘sufficiently controlled’ for 3 months as long as there are ‘no mental health issues’. If there are ‘high-risk features’ then 6 months of control and a ‘specialist opinion’ is required before resumption of driving. This is the case for both group-1 and group-2 licences.32
Conclusion
We have discussed the acute and chronic management of a patient with FNEA, highlighting the importance of individualised assessment and management based on biopsychosocial formulation. We would recommend that all patients with FNEA are referred to neuropsychiatric services, but also appreciate that due to service provision and funding gaps this is not always possible, and furthermore many patients have significant psychiatric comorbidity requiring the skills and resources of general psychiatry. Patients with FNEA can often seem as if they do not fall neatly within the responsibility of neurology or psychiatry; however a joint approach is likely to be the most productive given the degree of comorbidity. Their often-arduous journey towards diagnosis and treatment demonstrates why neurologists and psychiatrists should work, and train, in collaboration.
The extensive gaps in the literature that have been mentioned include the paucity of comparative studies between other episodic psychiatric syndromes such as panic attacks and FNEA (with these studies tending to compare FNEA patients with epileptic seizure patients), the lack of large-scale neuroimaging studies and genetic studies. The difficulty of establishing what abnormalities in studies are related to childhood trauma, comorbid psychiatric illness or the effect of chronic functional symptoms makes such studies difficult to perform. Studies assessing interventions focusing on purely social function are missing, as are large epidemiological studies, large personality disorder studies and studies examining the effect of being on or off a neurological caseload. Double-blind RCTs are extremely few in number, although this is not surprising as most studies are of psychological interventions which cannot provide a true placebo.
The earlier the diagnosis is made and biopsychosocial assessment and management put in place, the better the outcome, including a full resolution of symptoms. A neuropsychiatrist is ideally placed to do this, but a general psychiatrist, if following the basic principles discussed, can achieve good outcomes with these patients.
Acknowledgements
The authors thank Rowan Munson for his contribution to this article.
About the authors
Rollo J. G. Sheldon, ST7 in Neuropsychiatry, South West London and St George's Mental Health NHS Trust, UK; Niruj Agrawal, Consultant Neuropsychiatrist, South West London and St George's Mental Health NHS Trust; Honorary Consultant Neuropsychiatrist, Atkinson Morley Regional Neurosciences Centre, St George's Hospital; and Honorary Senior Lecturer, St George's University of London, UK






eLetters
No eLetters have been published for this article.