3 results
Major depression, cardiovascular risk factors and the Omega-3 index
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 603
-
- Article
-
- You have access
- Export citation
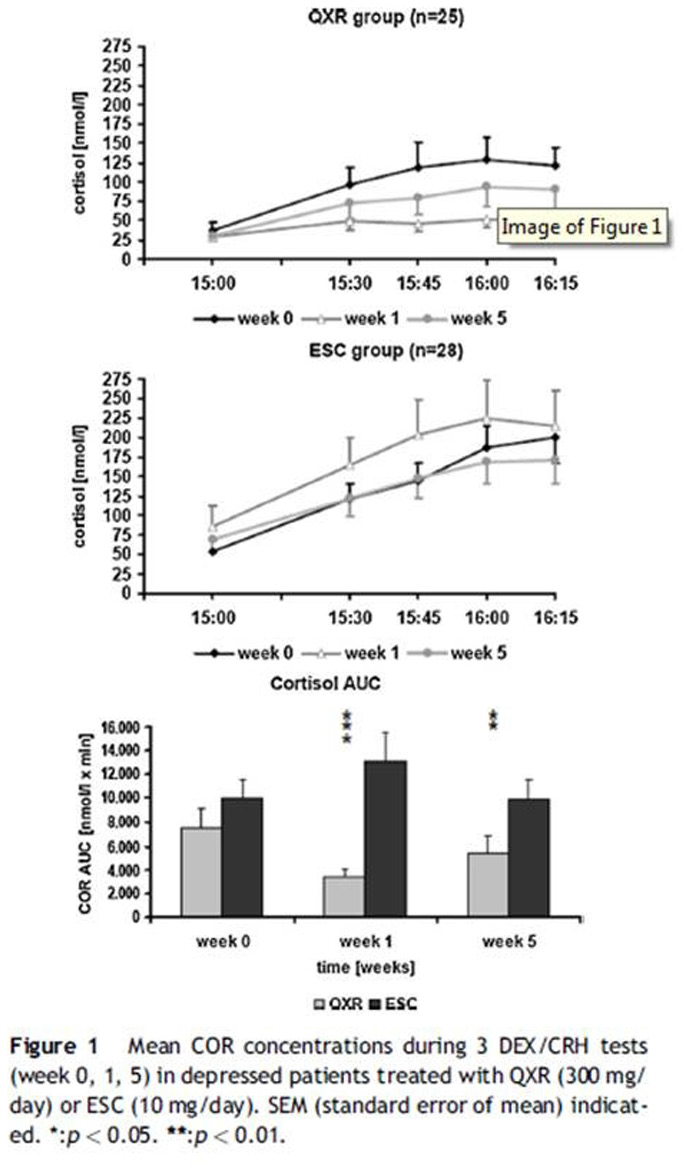
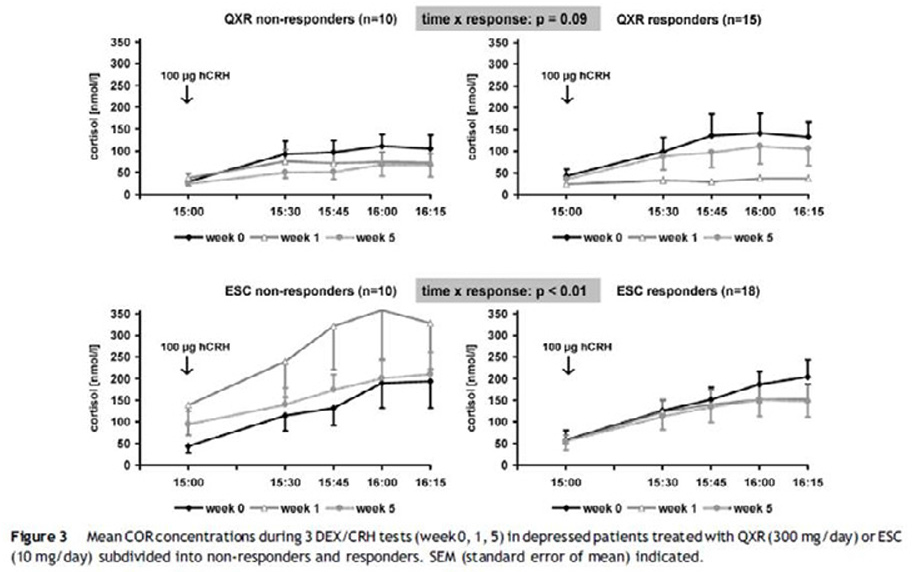
EPA-1654 – Impact on Cortisol and Antidepressant Efficacy of Quetiapine and Escitalopram in Depression
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, pp. 1-2
-
- Article
-
- You have access
- Export citation
Brain pathway differences between Parkinson's disease patients with and without depressive symptoms
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, p. S349
-
- Article
-
- You have access
- Export citation