11 results
P03-66 - Real causes of some psychotic disorders
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E1176
-
- Article
-
- You have access
- Export citation
Cabbamazepine Addition in Antidepressant-resistant Unipolar Elderly Depressed Patients
-
- Journal:
- European Psychiatry / Volume 11 / Issue S4 / 1996
- Published online by Cambridge University Press:
- 16 April 2020, p. 377s
-
- Article
-
- You have access
- Export citation
EPA-1572 - Schizophrenias Frequently are not Primary Cerebral Disorders
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access
- Export citation
Tripolar Affective Disorder – the Old/new Clinical and Nosological Category
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access
- Export citation
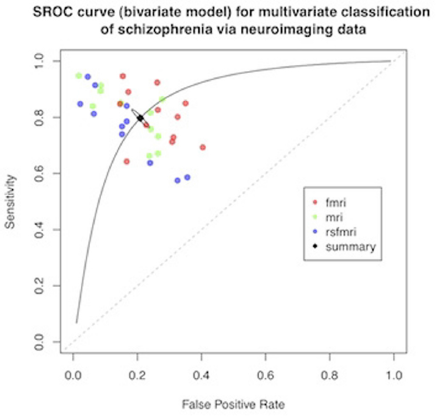
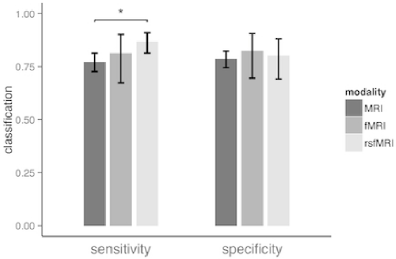
EPA-1671 – Diagnosing Schizophrenia Using Neuroimaging: A Meta-analysis of Multivariate Pattern Recognition Studies
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, pp. 1-2
-
- Article
-
- You have access
- Export citation
EPA-1579 - Classifying Schizophrenia using Joint Multivariate Pattern Recognition Analysis of Brain Function and Structure
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access
- Export citation
EPA-1680 – Tripolar Affective Disorders - a New Clinical Concept
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access
- Export citation
EPA-1644 – Differential Diagnosis of Schizophrenia vs. Borderline Personality Disorder Using Pattern Classification Methods in Structural Mri Images
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access
- Export citation
EPA-1668 - Differential Diagnostic Classification of Schizophrenia and Depression Using Mri-based Pattern Recognition
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access
- Export citation
Extracerebral or Secondary Cerebral Schizophrenias
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access
- Export citation
Large cava septi pellucidi in schizophrenic patients, alcoholics, head-traumatized, and normal individuals: morpholgical features and forensic implications. A postmortem study
-
- Journal:
- Acta Neuropsychiatrica / Volume 18 / Issue 1 / February 2006
- Published online by Cambridge University Press:
- 24 June 2014, pp. 15-20
-
- Article
- Export citation