47 results
Contact precautions as a barrier to hand hygiene: The Plan–Do–Study–Act (PDSA) framework to improve compliance with gloved hand hygiene
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 29 February 2024, pp. 1-2
-
- Article
- Export citation
Chapter 38 - Termination of Pregnancy
- from Section 2B - Sexual and Reproductive Healthcare: Termination of Pregnancy
-
-
- Book:
- Textbook of Contraception, Sexual and Reproductive Health
- Published online:
- 16 January 2024
- Print publication:
- 25 January 2024, pp 233-238
-
- Chapter
- Export citation
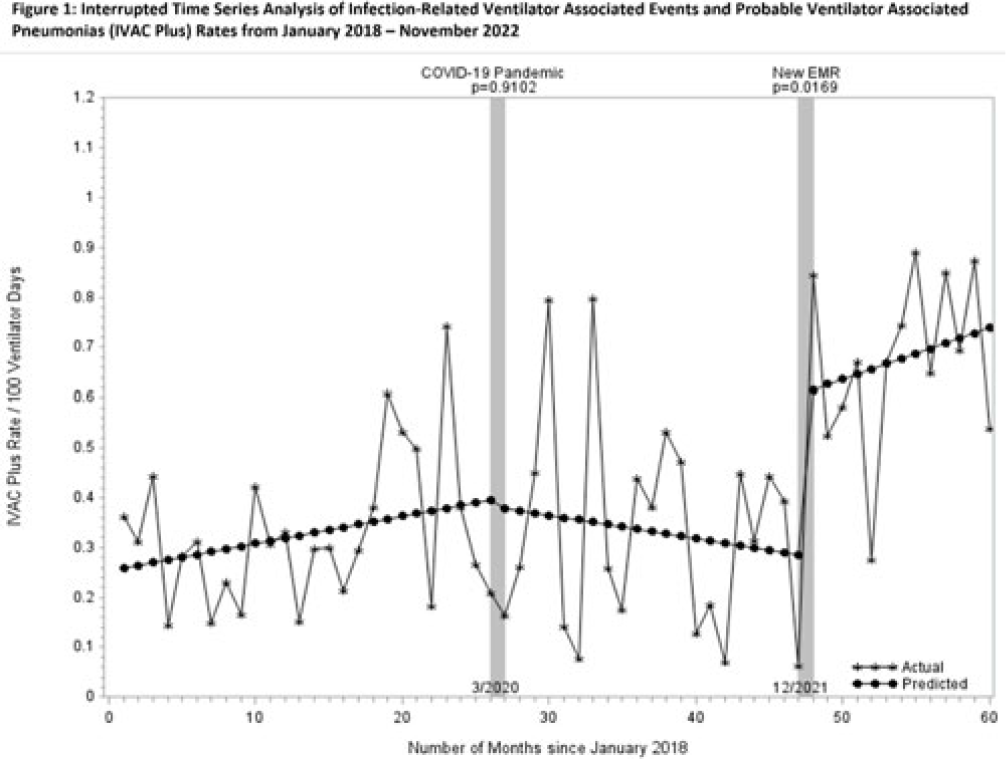
Increasing rates of ventilator-associated events: Blame it on COVID-19?
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s105-s106
-
- Article
-
- You have access
- Open access
- Export citation
An Audit on the Uptake of Psychosocial Interventions in a Nationally Accredited Memory Service
-
- Journal:
- BJPsych Open / Volume 9 / Issue S1 / July 2023
- Published online by Cambridge University Press:
- 07 July 2023, p. S188
-
- Article
-
- You have access
- Open access
- Export citation
338 The Alabama Genomic Health Initiative: Integrating Genomic Medicine into Primary Care
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue s1 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, pp. 100-101
-
- Article
-
- You have access
- Open access
- Export citation
Staphylococcal decolonization to prevent surgical site infection: Is there a role in colorectal surgery?
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 11 July 2022, e116
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Chapter 52 - Prevention of Unintended Pregnancy
- from Section 11 - Public Health Issues in Gynaecology
-
-
- Book:
- The EBCOG Postgraduate Textbook of Obstetrics & Gynaecology
- Published online:
- 24 November 2021
- Print publication:
- 02 December 2021, pp 449-456
-
- Chapter
- Export citation
Healthcare worker perceptions of hand hygiene monitoring technologies: Does technology performance matter?
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 12 / December 2021
- Published online by Cambridge University Press:
- 23 July 2021, pp. 1519-1520
- Print publication:
- December 2021
-
- Article
- Export citation
Impact of coronavirus disease 2019 (COVID-19) on healthcare-associated infections: An update and perspective
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 6 / June 2022
- Published online by Cambridge University Press:
- 12 March 2021, pp. 813-815
- Print publication:
- June 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Healthcare-associated COVID-19: The experience of an academic medical center
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 1 / January 2022
- Published online by Cambridge University Press:
- 07 December 2020, pp. 118-120
- Print publication:
- January 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The impact of coronavirus disease 2019 (COVID-19) on provider use of electronic hand hygiene monitoring technology
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 8 / August 2021
- Published online by Cambridge University Press:
- 20 November 2020, pp. 1007-1009
- Print publication:
- August 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Staphylococcal Decolonization to Prevent Surgical Site Infection: Is There a Role in colorectal surgery?
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s497
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Prevalence of Carbapenem-Resistant Enterobacteriaceae (CRE) at a Tertiary-Care Center in the United States
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s494-s495
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Accuracy of the NHSN Central-Line–Associated Bloodstream Infections (CLABSIs) Definition: The Experience of Two Geographically Proximal Hospitals
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s457-s458
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Universal screening for the SARS-CoV-2 virus on hospital admission in an area with low COVID-19 prevalence
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 10 / October 2020
- Published online by Cambridge University Press:
- 23 July 2020, pp. 1231-1233
- Print publication:
- October 2020
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
A call for collective crisis leadership
-
- Article
-
- You have access
- HTML
- Export citation
Chasing the rate: An interrupted time series analysis of interventions targeting reported hospital onset Clostridioides difficile, 2013–2018
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 10 / October 2020
- Published online by Cambridge University Press:
- 04 June 2020, pp. 1142-1147
- Print publication:
- October 2020
-
- Article
- Export citation
Utility of retesting for diagnosis of SARS-CoV-2/COVID-19 in hospitalized patients: Impact of the interval between tests
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 7 / July 2020
- Published online by Cambridge University Press:
- 11 May 2020, pp. 859-861
- Print publication:
- July 2020
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Impact of COVID-19 on traditional healthcare-associated infection prevention efforts
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 8 / August 2020
- Published online by Cambridge University Press:
- 16 April 2020, pp. 946-947
- Print publication:
- August 2020
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Novel coronavirus and hospital infection prevention: Preparing for the impromptu speech
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 5 / May 2020
- Published online by Cambridge University Press:
- 03 March 2020, pp. 592-593
- Print publication:
- May 2020
-
- Article
-
- You have access
- HTML
- Export citation