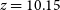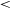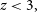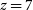35 results
The nature and likely redshift of GLEAM J0917–0012
- Part of
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 38 / 2021
- Published online by Cambridge University Press:
- 21 September 2021, e049
-
- Article
-
- You have access
- HTML
- Export citation
17 - Psychiatric Evaluation in the Medical Setting
-
-
- Book:
- Introduction to Psychiatry
- Published online:
- 22 July 2021
- Print publication:
- 12 August 2021, pp 415-447
-
- Chapter
- Export citation
Chapter 15 - Approach to the Treatment of Medication-Resistant Epilepsy
-
-
- Book:
- Medication-Resistant Epilepsy
- Published online:
- 20 August 2020
- Print publication:
- 10 September 2020, pp 171-178
-
- Chapter
- Export citation
Contributors
-
- Book:
- Medication-Resistant Epilepsy
- Published online:
- 20 August 2020
- Print publication:
- 10 September 2020, pp ix-xii
-
- Chapter
- Export citation
Chapter 20 - Stimulation Treatment for Medication-Resistant Epilepsy
-
- Book:
- Medication-Resistant Epilepsy
- Published online:
- 20 August 2020
- Print publication:
- 10 September 2020, pp 219-240
-
- Chapter
- Export citation
Dedication
-
- Book:
- Medication-Resistant Epilepsy
- Published online:
- 20 August 2020
- Print publication:
- 10 September 2020, pp v-vi
-
- Chapter
- Export citation
Index
-
- Book:
- Medication-Resistant Epilepsy
- Published online:
- 20 August 2020
- Print publication:
- 10 September 2020, pp 269-274
-
- Chapter
- Export citation
Contents
-
- Book:
- Medication-Resistant Epilepsy
- Published online:
- 20 August 2020
- Print publication:
- 10 September 2020, pp vii-viii
-
- Chapter
- Export citation
Copyright page
-
- Book:
- Medication-Resistant Epilepsy
- Published online:
- 20 August 2020
- Print publication:
- 10 September 2020, pp iv-iv
-
- Chapter
- Export citation
Medication-Resistant Epilepsy
- Diagnosis and Treatment
-
- Published online:
- 20 August 2020
- Print publication:
- 10 September 2020
Chapter 16 - Intracranial EEG Monitoring
-
-
- Book:
- Understanding Epilepsy
- Published online:
- 11 October 2019
- Print publication:
- 21 November 2019, pp 304-325
-
- Chapter
- Export citation
Problems in the Diagnosis of Progressive Supranuclear Palsy (Steele — Richardson — Olszewski Syndrome)
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 5 / Issue 2 / May 1978
- Published online by Cambridge University Press:
- 18 September 2015, pp. 167-173
-
- Article
-
- You have access
- Export citation
Circuit Editing and Failure Analysis Applications using a Three-Ion-Beam (Ga, He and Ne) System and Gas Injection System (GIS)
-
- Journal:
- Microscopy and Microanalysis / Volume 21 / Issue S3 / August 2015
- Published online by Cambridge University Press:
- 23 September 2015, pp. 1165-1166
- Print publication:
- August 2015
-
- Article
-
- You have access
- Export citation
Contributors
-
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Environmental Transmission of Clostridium difficile: Association Between Hospital Room Size and C. difficile Infection
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 36 / Issue 5 / May 2015
- Published online by Cambridge University Press:
- 05 February 2015, pp. 564-568
- Print publication:
- May 2015
-
- Article
- Export citation
Advantages of Helium and Neon Ion Beams for Intelligent Imaging
-
- Journal:
- Microscopy and Microanalysis / Volume 20 / Issue S3 / August 2014
- Published online by Cambridge University Press:
- 27 August 2014, pp. 338-339
- Print publication:
- August 2014
-
- Article
-
- You have access
- Export citation
Notes on contributors
-
-
- Book:
- Moving Shakespeare Indoors
- Published online:
- 05 March 2014
- Print publication:
- 06 March 2014, pp x-xii
-
- Chapter
- Export citation
Contributors
-
-
- Book:
- Shakespeare Survey
- Published online:
- 05 December 2013
- Print publication:
- 07 November 2013, pp vi-vi
-
- Chapter
- Export citation
What's so insidious about “Peace, Love, and Understanding”? A system justification perspective
-
- Journal:
- Behavioral and Brain Sciences / Volume 35 / Issue 6 / December 2012
- Published online by Cambridge University Press:
- 20 November 2012, pp. 438-439
-
- Article
- Export citation
Contributors
-
-
- Book:
- Britain's Oceanic Empire
- Published online:
- 05 June 2012
- Print publication:
- 31 May 2012, pp viii-x
-
- Chapter
- Export citation