19 results
Carbapenem-resistant Acinetobacter baumannii and Carbapenem-resistant Enterobacterales in US Dialysis Populations, 2016-2021
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s87-s88
-
- Article
-
- You have access
- Open access
- Export citation
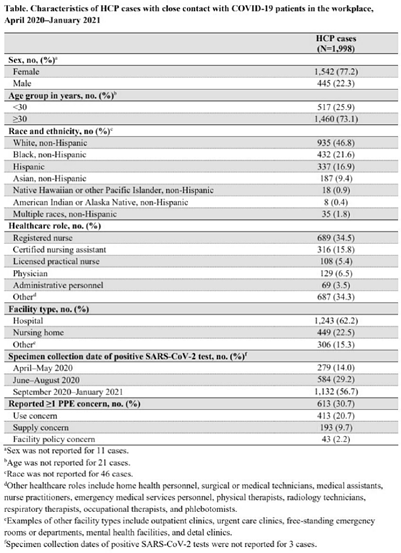
Characteristics of healthcare personnel with SARS-CoV-2 infection: 10 emerging infections program sites in the United States, April 2020–December 2021
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 21 May 2024, pp. 1-9
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Epidemiology of carbapenem-resistant organisms in Alameda County, California, 2019–2021
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 29 April 2024, e64
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
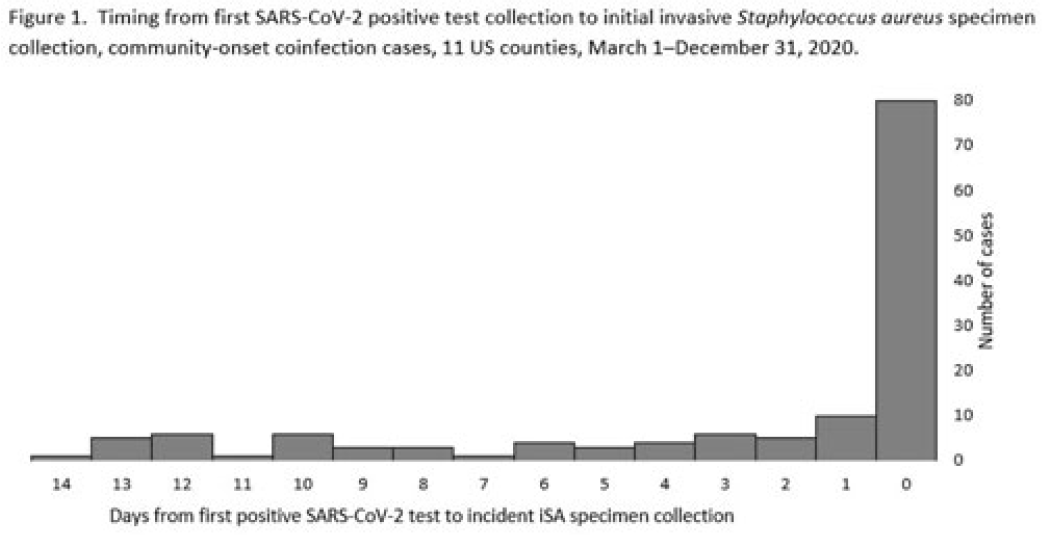
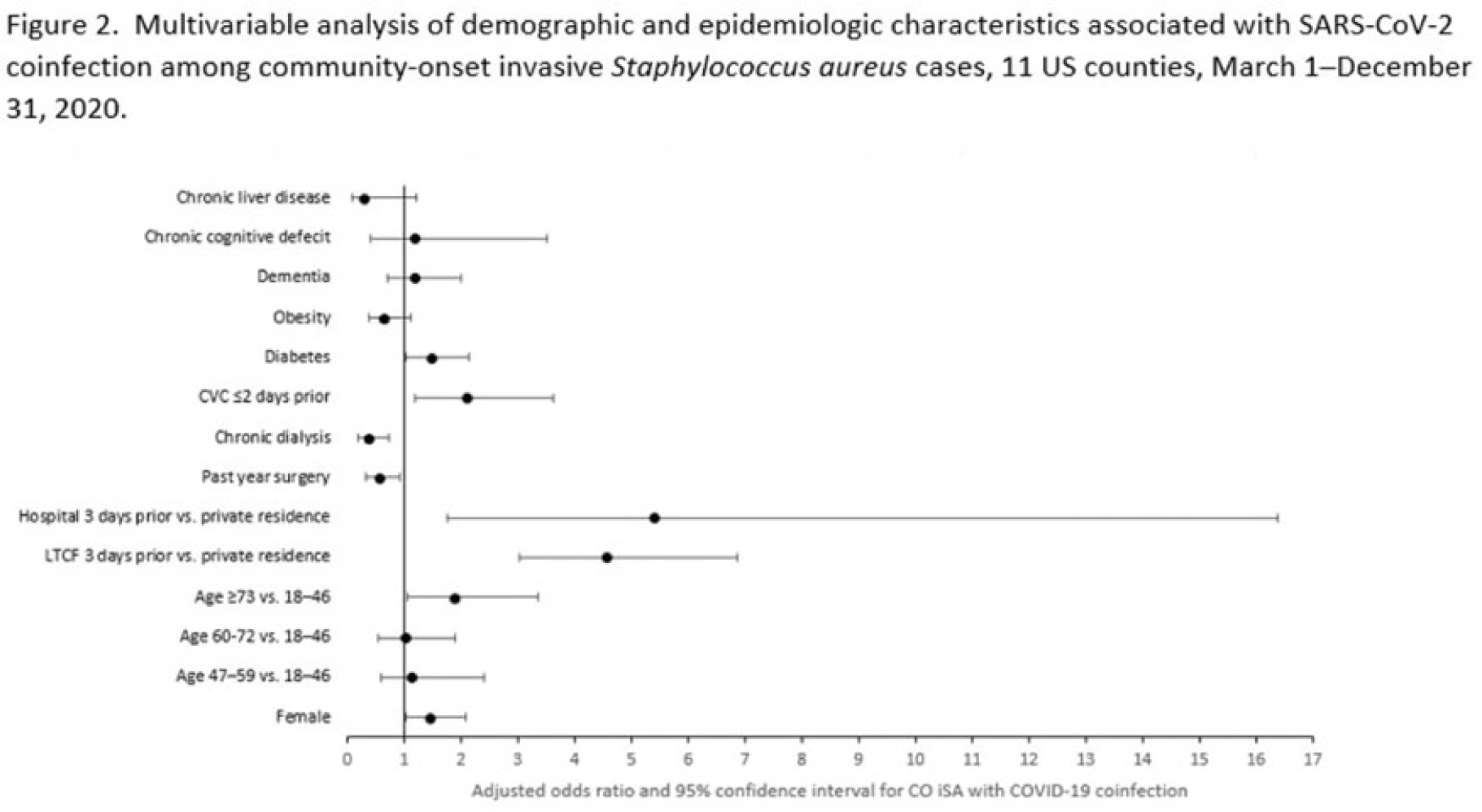
Factors associated with SARS-CoV-2 and community-onset invasive Staphylococcus aureus coinfection, 2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s84-s85
-
- Article
-
- You have access
- Open access
- Export citation
Epidemiology of carbapenem-resistant and extended-spectrum beta-lactamase-producing Enterobacterales in US children, 2016–2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s16
-
- Article
-
- You have access
- Open access
- Export citation
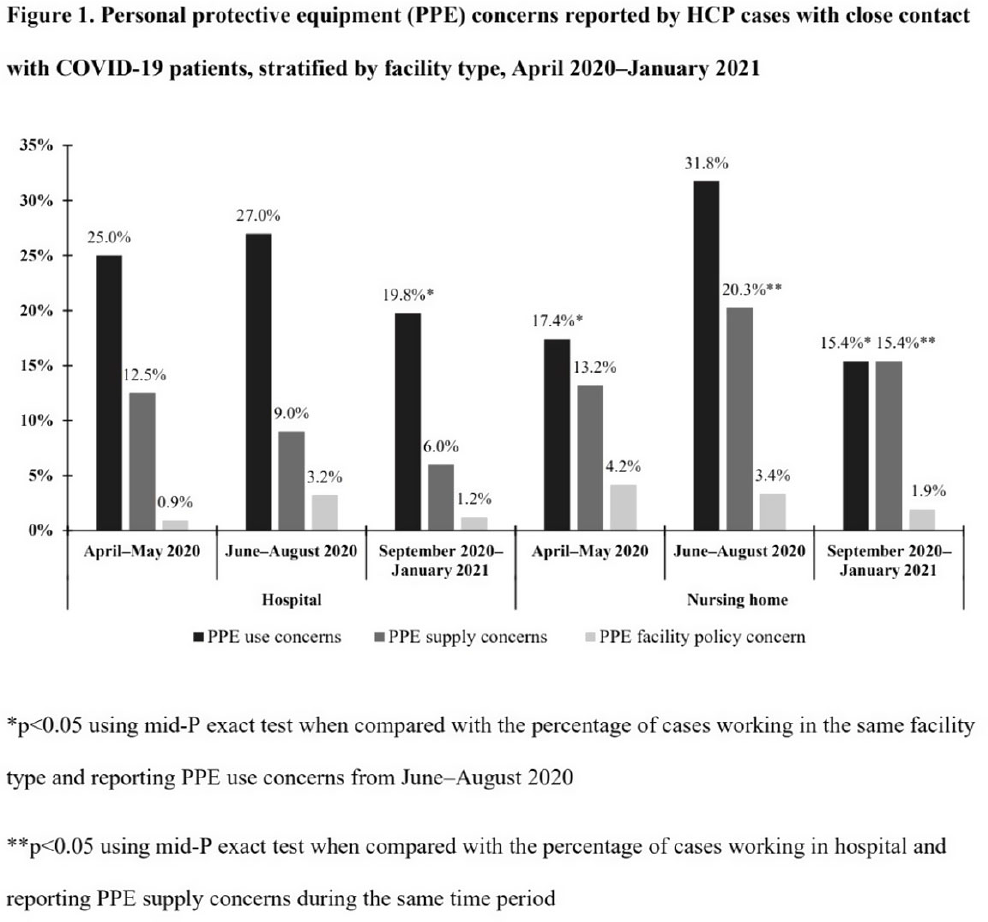
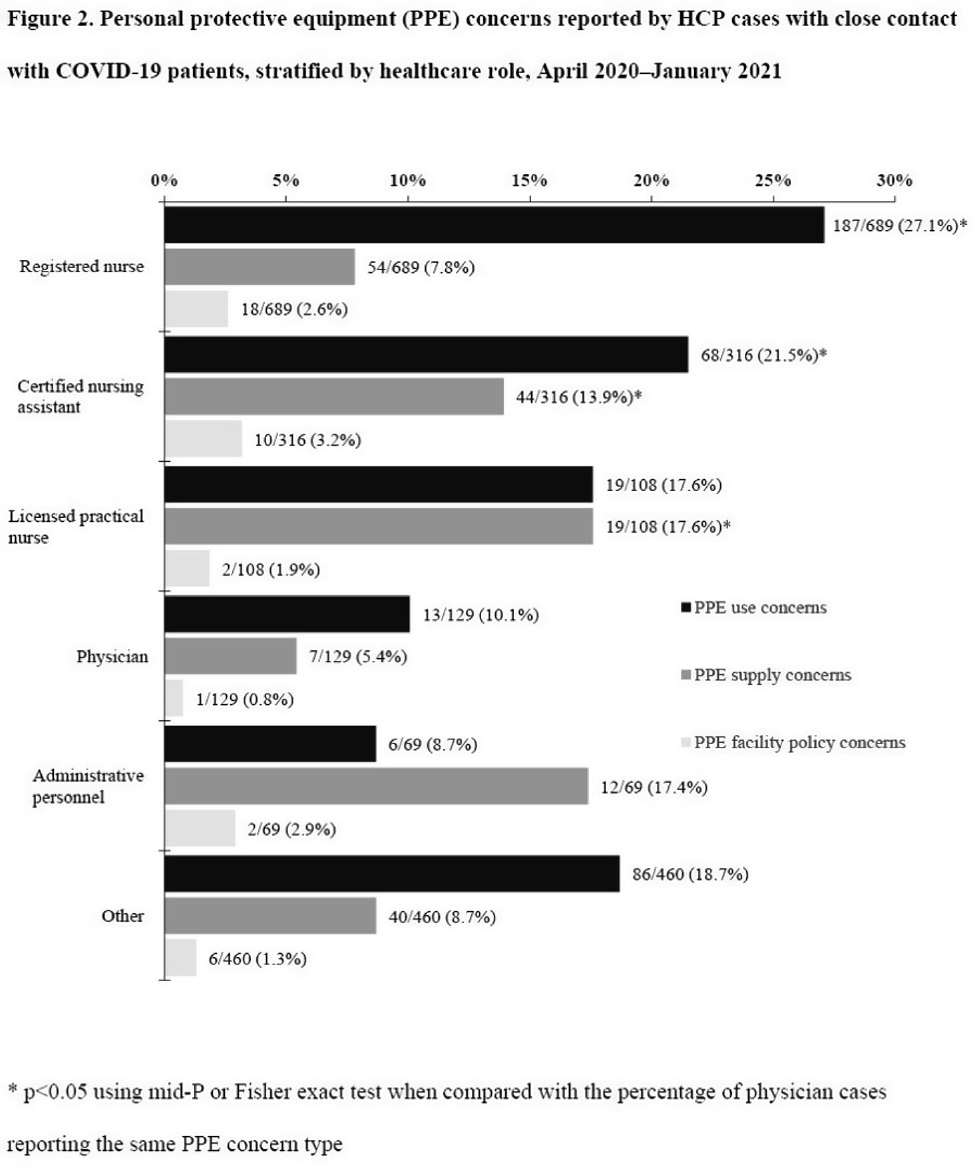
Characteristics of healthcare personnel who reported concerns related to PPE use during care of COVID-19 patients
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s8-s9
-
- Article
-
- You have access
- Open access
- Export citation
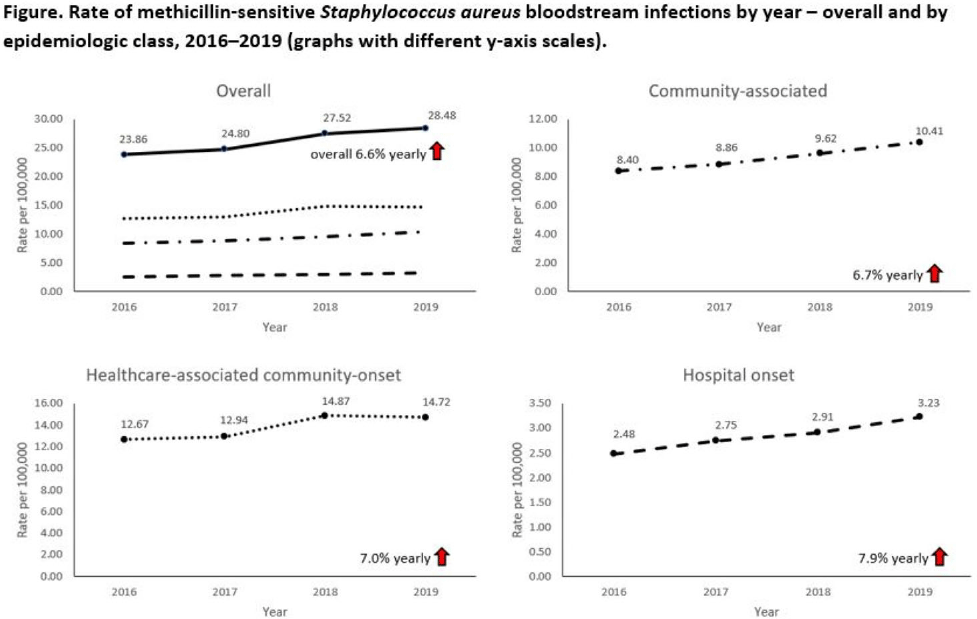
Increases in methicillin-sensitive Staphylococcus aureus bloodstream infection incidence, 2016–2019
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s63-s64
-
- Article
-
- You have access
- Open access
- Export citation
Practices and activities among healthcare personnel with severe acute respiratory coronavirus virus 2 (SARS-CoV-2) infection working in different healthcare settings—ten Emerging Infections Program sites, April–November 2020
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 8 / August 2022
- Published online by Cambridge University Press:
- 02 June 2021, pp. 1058-1062
- Print publication:
- August 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Improving Surveillance of Pneumonia in Nursing Homes
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s290-s291
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Antibiotic Susceptibility of Common Organisms Isolated from Urine Cultures of Nursing Home Residents
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s118-s120
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Evaluation of Discrepancies in Carbapenem Minimum Inhibitory Concentrations Obtained at Clinical Laboratories Compared to a Public Health Laboratory
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s474-s476
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Characterization of Ceftazidime-Avibactam-Resistant Carbapenem-Resistant Enterobacteriaceae, United States, 2015–2017
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s465-s466
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Prevalence and Epidemiology of Healthcare-Associated Infections (HAI) in US Nursing Homes (NH), 2017
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s45-s46
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Evaluation of Care Interactions Between Healthcare Personnel and Residents in Nursing Homes Across the United States
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s36-s38
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Appropriateness of Initiating Antibiotics for Urinary Tract Infection Among Nursing Home Residents
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s127-s128
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Characteristics Associated With Invasive Staphylococcus aureus Infection Rates in Nursing Homes, Emerging Infections Program
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s60-s61
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Characteristics of Cases With Polymicrobial Bloodstream Infections Involving Candida in Multisite Surveillance, 2017
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s163
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Documentation of acute change in mental status in nursing homes highlights opportunity to augment infection surveillance criteria
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 7 / July 2020
- Published online by Cambridge University Press:
- 28 April 2020, pp. 848-850
- Print publication:
- July 2020
-
- Article
- Export citation
Completeness of Methicillin-Resistant Staphylococcus aureus Bloodstream Infection Reporting From Outpatient Hemodialysis Facilities to the National Healthcare Safety Network, 2013
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 37 / Issue 2 / February 2016
- Published online by Cambridge University Press:
- 11 November 2015, pp. 205-207
- Print publication:
- February 2016
-
- Article
- Export citation