59 results
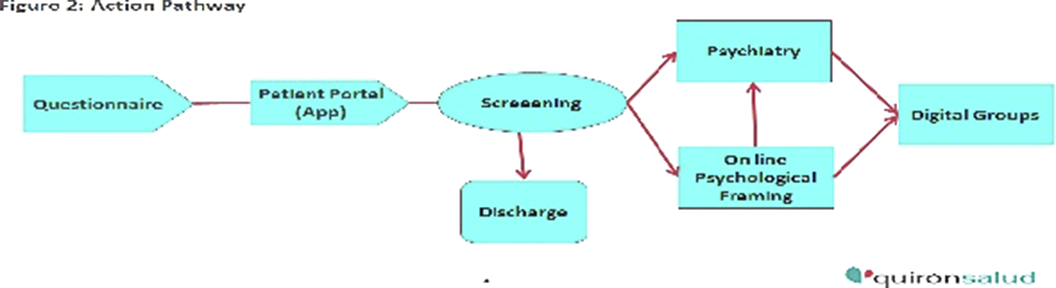
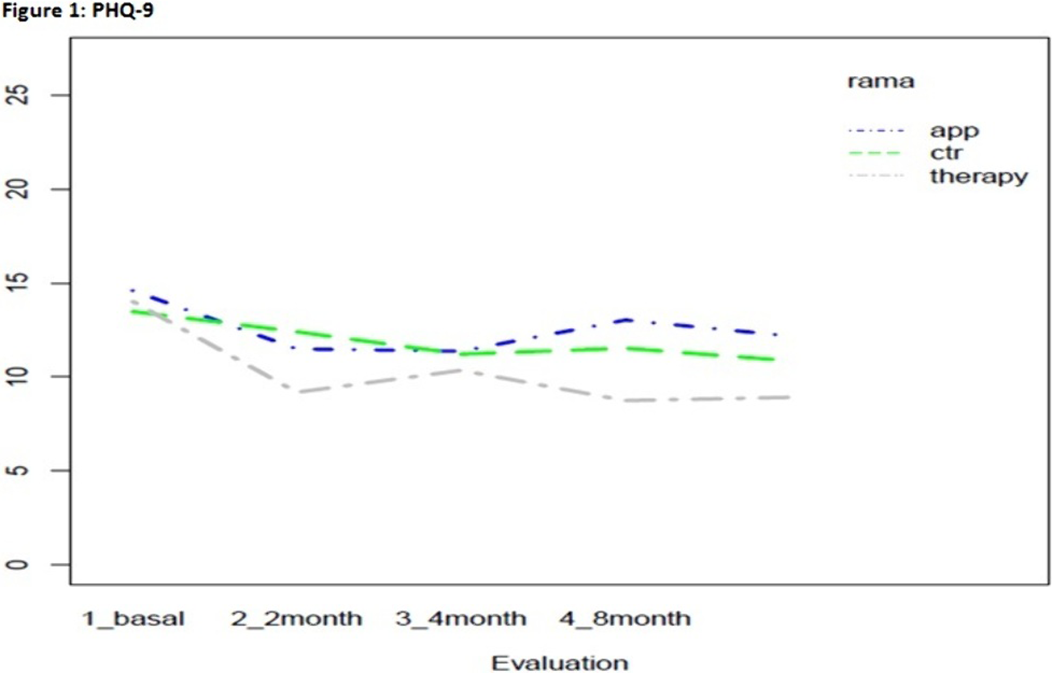
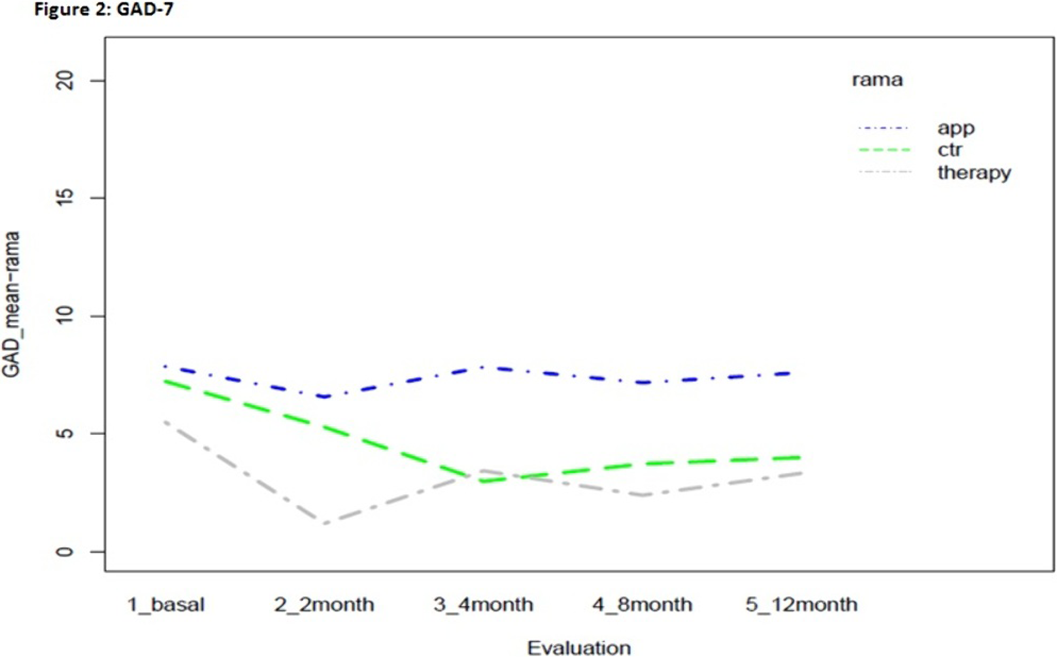
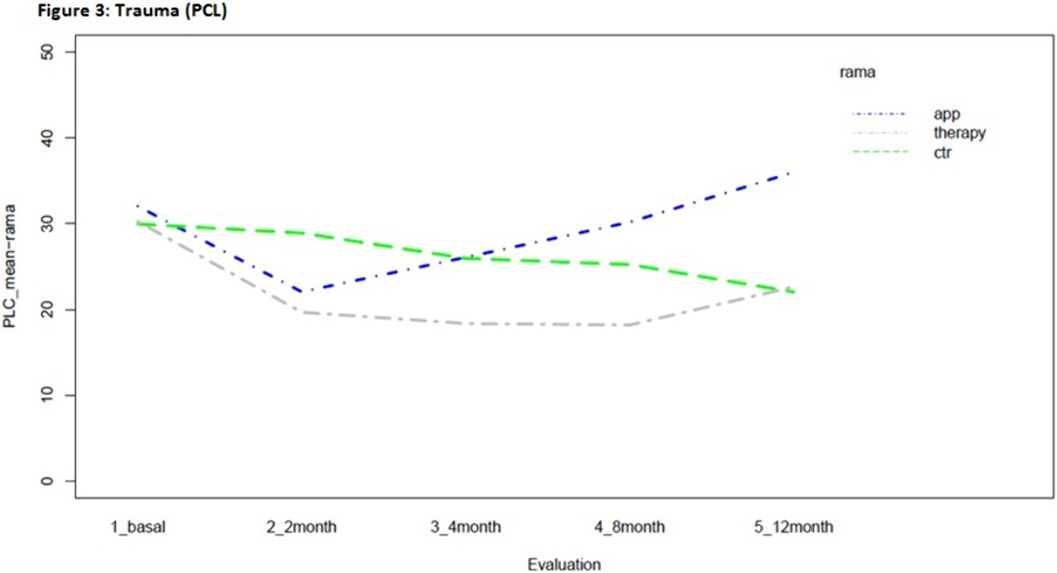
Mental Health and Addictions in Pregnancy: Feasibility and Acceptability of a Computerized Clinical Pathway and Prevalence Rates
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S66-S67
-
- Article
-
- You have access
- Open access
- Export citation
Differences in adherence to treatment, relapses and healthcare costs between delusional disorder and paranoid personality disorder
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S128
-
- Article
-
- You have access
- Open access
- Export citation
Association between loneliness in childhood and first-episode psychosis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S88-S89
-
- Article
-
- You have access
- Open access
- Export citation
Factors associated with first suicide attempt vs. re-attempt in children and adolescents: A systematic review and meta-analysis
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S584
-
- Article
-
- You have access
- Open access
- Export citation
Alternative initiations with 6-monthly paliperidone palmitate. A retrospective study
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S488-S489
-
- Article
-
- You have access
- Open access
- Export citation
Clinical experiences with 6-monthly paliperidone palmitate after 12 months of use. A retrospective study
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S488
-
- Article
-
- You have access
- Open access
- Export citation
Clinical experiences with 6-monthly paliperidone palmitate beyond the diagnosis of schizophrenia. A retrospective study
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S489
-
- Article
-
- You have access
- Open access
- Export citation
Miss attending risk factors in gynecological prenatal care among pregnant women at risk for dual pathology
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S320
-
- Article
-
- You have access
- Open access
- Export citation
E-health treatments for Dual Disorders on pregnancy
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S92-S93
-
- Article
-
- You have access
- Open access
- Export citation
Pending challenges to e-mental health in the COVID-19 era: Acceptability of a smartphone-based ecological momentary assessment application among patients with schizophrenia spectrum disorders
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S343
-
- Article
-
- You have access
- Open access
- Export citation
Preliminary Evidence for Cannabis and Nicotine Urinary Metabolites as Predictors of Verbal Memory Performance and Learning Among Young Adults
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 27 / Issue 6 / July 2021
- Published online by Cambridge University Press:
- 15 July 2021, pp. 546-558
-
- Article
- Export citation
P03-37 - Testing A New Technique for the Rehabilitation of Schizophrenia and Other Psychoses Based on Viewing Fiction Films
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E1147
-
- Article
-
- You have access
- Export citation
S09-02 - Diagnostic Stability of Psychiatric Disorders
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E109
-
- Article
-
- You have access
- Export citation
P0133 - Comorbidity between personality disorders and bipolar disorders
-
- Journal:
- European Psychiatry / Volume 23 / Issue S2 / April 2008
- Published online by Cambridge University Press:
- 16 April 2020, p. S231
-
- Article
-
- You have access
- Export citation
Patients with suicidal ideation in primary care: Clinical characteristics
-
- Journal:
- European Psychiatry / Volume 22 / Issue S1 / March 2007
- Published online by Cambridge University Press:
- 16 April 2020, pp. S327-S328
-
- Article
-
- You have access
- Export citation
P0201 - Primary versus secondary chronic insomnia in primary care
-
- Journal:
- European Psychiatry / Volume 23 / Issue S2 / April 2008
- Published online by Cambridge University Press:
- 16 April 2020, pp. S359-S360
-
- Article
-
- You have access
- Export citation
Blood polyamine levels in drug-free schizophrenics
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 1492
-
- Article
-
- You have access
- Export citation
P0084 - Characteristics of patients with undetected psychiatric pathology in primary care
-
- Journal:
- European Psychiatry / Volume 23 / Issue S2 / April 2008
- Published online by Cambridge University Press:
- 16 April 2020, p. S327
-
- Article
-
- You have access
- Export citation
SAT-1 -1415T/C polymorphism and suicidal behavior
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 812
-
- Article
-
- You have access
- Export citation
Searching for Variables Associated with Familial Suicide Attempts Using Data Mining Techniques
-
- Journal:
- European Psychiatry / Volume 24 / Issue S1 / January 2009
- Published online by Cambridge University Press:
- 16 April 2020, 24-E730
-
- Article
-
- You have access
- Export citation