Methadone was initially developed for pain relief but since 1960 it has been used as an opioid-substitution therapy to relieve narcotic craving, suppress abstinence symptoms and block the euphoric effects of heroin. To our knowledge, there was no systematic review available until 2003 Reference Faggiano, Vigna-Taglianti, Versino and Lemma1 reporting the effective dose of methadone for substitution therapy. The organisation and regulation of methadone substitution therapy varied widely, which possibly left many service users on a wide range of doses of methadone.
QTc interval prolongation in electrocardiogram (ECG, above 500 ms) can increase the risk of torsade de pointes, otherwise known as polymorphic ventricular tachycardia, with often fatal outcomes. Reference Botstein2 There have been a number of reports published Reference De Bels, Staroukine and Devriendt3-Reference Sala, Anguera and Cervantes11 after the first report Reference Gil, Sala, Anguera, Chapinal, Cervantes and Guma12 associating QTc interval prolongation and torsade de pointes with methadone use. Some of these reports showed that increase in QTc interval is dose related Reference Sala, Anguera and Cervantes11,Reference Decerf, Gressens, Brohet and Liolios13 and high-dose methadone and concomitant use of agents that increase serum methadone levels are the most prevalent risk factors for torsade de pointes. Reference Almehmi, Malas, Yousufuddin and Rosencrance14 Medicines and Healthcare Products Regulatory Agency guidelines Reference Sticherling, Schaer, Ammann, Maeder and Osswald15 have, therefore, recommended increased cardiac monitoring of service users who are on high-dose methadone (⩾100 mg/day) and with other risk factors, i.e. heart or liver disease, electrolyte abnormalities, and concomitant treatment with CYP 3A4 inhibitors. Reference Faggiano, Vigna-Taglianti, Versino and Lemma1,Reference Peles, Bodner, Kreek, Rados and Adelson16 Although the Department of Health guidelines Reference Routhier, Katz and Brooks17 do not recommend blanket use of ECG for every service user, it advises that ECGs should be considered in users with the above risk factors. The aims of this audit were to explore the extent to which three substance misuse services adhered to the Department of Health guidelines for arranging ECGs for service users receiving high-dose methadone prescriptions. We also explored the reasons for non-adherence to guidelines (if any) and the prevalence of QTc interval prolongation.
Method
All service users being prescribed high-dose (⩾100 mg/day) methadone by Portsmouth and South East Hampshire substance misuse services were included in this audit. These teams cover a city and its suburbs and are responsible for prescribing methadone to 580 service users. Names of service users were collected from the computerised database of the prescribing team. Two of the authors (S.G. and A.K.) collected the data (between June and July 2008) from service users' clinical notes using a simple data-collection tool. Data from September 2007 onwards was collected as Department of Health guidelines were updated at that time. The data collected included: demographic details of service users, present dose of methadone, duration of present dose prescribed, pre-existing cardiac conditions (if any), evidence of cardiac monitoring, date of last monitoring, findings of monitoring, professional/s involved in monitoring, how the results were communicated between services, the reasons for any communication failure and the measures taken to address it. At the beginning of the audit we decided to implement recommendations immediately following the presentation of the audit results. This allowed us to prospectively explore our hypothesised reasons for non-adherence to the guidelines.
Results
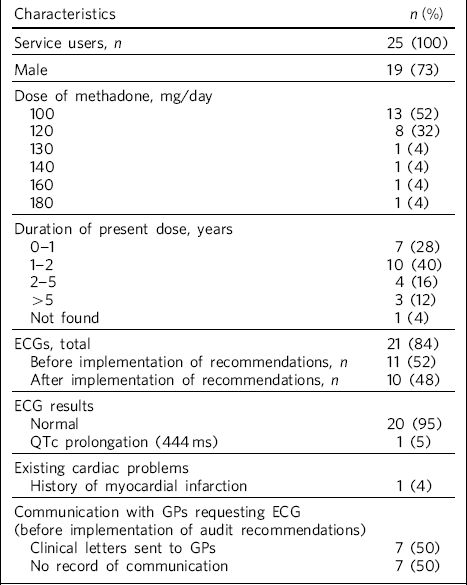
We identified 25 (4%) service users (19 male, 6 female) on a wide range of high doses of methadone (100–180 mg daily) for a varying period of time (2 months to 30 years). Overall, 13 (52%) service users were on 100 mg methadone, 8 (32%) on 120 mg and 1 (4%) each on 130, 140, 160 and 180 mg daily (Table 1).
Table 1 Basic demographics and outcomes
| Characteristics | n (%) |
|---|---|
| Service users, n | 25 (100) |
| Male | 19 (73) |
| Dose of methadone, mg/day | |
| 100 | 13 (52) |
| 120 | 8 (32) |
| 130 | 1 (4) |
| 140 | 1 (4) |
| 160 | 1 (4) |
| 180 | 1 (4) |
| Duration of present dose, years | |
| 0–1 | 7 (28) |
| 1–2 | 10 (40) |
| 2–5 | 4 (16) |
| >5 | 3 (12) |
| Not found | 1 (4) |
| ECGs, total | 21 (84) |
| Before implementation of recommendations, n | 11 (52) |
| After implementation of recommendations, n | 10 (48) |
| ECG results | |
| Normal | 20 (95) |
| QTc prolongation (444 ms) | 1 (5) |
| Existing cardiac problems | |
| History of myocardial infarction | 1 (4) |
| Communication with GPs requesting ECG (before implementation of audit recommendations) | |
| Clinical letters sent to GPs | 7 (50) |
| No record of communication | 7 (50) |
A total of 11 (44%) service users were found to have had ECGs. Except for one ECG where the QTc interval was slightly increased (444 ms), all other ECGs were normal. However, this service user continued to receive a prescription for methadone. One service user had a history of myocardial infarction. Of the remaining 14 service users who had no record of having an ECG, 7 (50%) had evidence of clinic letters sent to general practitioners (GPs) requesting them to arrange ECGs. For the other 7, no evidence of any communication from secondary care services was found. However, of these, two had been advised to contact their GPs to have an ECG.
Adherence to recommendations
This audit identified three factors leading to non-adherence to guidelines. First, for half the service users no referral was made by secondary care services to primary care services for an ECG. Second, for the other half, a referral was made by secondary care services to primary care services for an ECG but there was no record available in the individuals' notes showing that this had been carried out. Third, lack of motivation among service users may be a reason for ECGs not being carried out. Our recommendations were that clinicians and key workers should establish effective communication with primary care services, spread awareness about the guidelines and be proactive to increase the motivation of service users.
Audit findings with recommendations were presented at a joint meeting of all three services. In order to establish effective communication, key workers and clinicians were encouraged to liaise more closely with primary care services for arranging ECGs. This was achieved by ensuring that where indicated a referral for ECG was always made, and by making telephone calls to the GP surgery to follow up any referrals that had been made to ensure that the ECG is carried out. In addition to this, clinicians were asked to spread awareness of the guidelines among GPs where required and to inform them about their role in helping secondary care services to follow the guidelines. Key workers were asked to take a proactive role in motivating service users by helping them to understand the importance of attending their ECG appointment and in the case of more reluctant service users, to accompany them to surgeries. We received an extremely positive response from primary care services. Ten more service users had ECGs within 1 month; all 10 ECGs were normal.
Discussion
The audit showed that only a small proportion of service users (4% of total prescription) were being prescribed high-dose methadone; only 4 of whom were prescribed in excess of 120 mg per day. The rest of the service users were on a methadone substitution therapy with a dose of methadone below 100 mg per day.
Audit findings revealed that non-adherence to guidelines was often as a result of a lack of effective communication between primary and secondary care services in the catchment area of these three services. Substantial improvement in adherence to guidelines following the implementation of our recommendations confirmed that the factors identified in the audit were the reasons for non-adherence.
The three substance misuse services in this audit are dependent on primary care services for the arrangement and interpretation of ECGs. This is because they are neither equipped to carry out ECGs nor do they have adequate expertise to interpret them. Substance misuse teams are usually led by a consultant psychiatrist with very little or no direct input from other specialists. A recent survey showed that only 5% of trainees and consultant psychiatrists could correctly indicate QTc intervals. Reference Krantz, Kutinsky, Robertson and Mehler18 Computer-assisted ECG interpretation is not completely reliable Reference Krantz, Kutinsky, Robertson and Mehler18 and errors are common, Reference Krantz, Lewkowiez, Hays, Woodroffe, Robertson and Mehler19 so interpretation should not be accepted without a visual inspection of the ECG, preferably by an expert. Reference Krantz, Lewkowiez, Hays, Woodroffe, Robertson and Mehler19 Therefore, in order to adhere to guidelines, psychiatrists in substance misuse teams would need to have expertise in ECG interpretation. This would require making basic training of reading ECG tracing mandatory for psychiatrists at all levels; particularly for psychiatric trainees. Reference Krantz, Kutinsky, Robertson and Mehler18,Reference Krantz, Martin, Stimmel, Mehta and Haigney20 The other option would be to provide easy access to cardiologists Reference Krantz, Martin, Stimmel, Mehta and Haigney20 or GPs with special interest in cardiology. As indicated by the findings, the other possible solution is to increase collective commitment and effective communication between primary and secondary care services. The number of primary care services prescribing substitution medication is growing. Reference Justo, Gal-Oz, Paren, Goldin and Zeltser21,22 This, we hope will increase contact between service users and their GPs. It could possibly ensure that most of the issues related to drug use, including cardiac monitoring as per the guidelines, will be successfully managed in general practice. The difficulty of non-adherence to the guidelines may become less of an issue in the future.
The ECG results in our audit showed that the prevalence of QTc interval prolongation was very low among the service users. However, the result does not deflect from the importance of taking a cautious approach before prescribing high-dose methadone. We find the recently published cardiac safety recommendations Reference Almehmi, Malas, Yousufuddin and Rosencrance14 to be highly appropriate. These are: informing service users about the risk of arrhythmia; taking a clinical history of structural heart problems, arrhythmia and syncope; obtaining ECGs for all service users before prescribing methadone; considering discontinuation and reduction of dose in individuals with QTc prolongation (>500 ms); elimination of risk factors; and being aware of drugs that interact with methadone.
Limitations
Other risk factors contributing to QTc interval prolongation were not recorded in this audit. However, normal ECG findings indirectly ruled out the contribution of these factors in prolonging QTc interval. The number of service users included in the audit is small and there was a relatively small number of service users on a very high dose of methadone. Nevertheless, we were able to identify areas requiring improvement in order to provide the standard of care compliant with the published standards.






eLetters
No eLetters have been published for this article.