The recent Bradley report Reference Bradley1 has renewed interest in the mental healthcare of offenders. In response, the government launched an ambitious delivery plan making a commitment to increase support for the growing number of people with mental illness in prison and elsewhere in the criminal justice system. 2 Central to the plan are the notions of working in partnership, continuity of care, and equivalence - the premise that prisoners have the right to the same standard and quality of healthcare as the wider community.
Medication is a cornerstone of modern psychiatric care. Reference Bullmore, Fletcher and Jones3 Appropriate prescribing in prisons can have a positive impact on individual patients and the prison regime as a whole by helping to reduce symptom severity, violence and aggression and illicit drug taking so that individuals can participate in purposeful activity. Reference Dolan, Shearer, MacDonald, Mattick, Hall and Wodak4,5 Current UK prison mental health policy states that prescribed medication should not be automatically stopped on entry to prison without proper psychiatric assessment. 6 Indeed, abrupt cessation of psychiatric medicines may precipitate discontinuation symptoms and even relapse. Reference Bullmore, Fletcher and Jones3,Reference Haddad and Anderson7 Nonetheless, a common complaint among prisoners is that medication for mental health problems is frequently either withheld temporarily or stopped completely when they are received into custody. Reference Plugge, Douglas and Fitzpatrick8-Reference Condon, Hek, Harris, Powell, Kemple and Price10 This problem should not be dismissed lightly given the increased risk of self-harm and suicide during the early period of custody. Reference Shaw, Baker, Hunt, Moloney and Appleby11
This study aimed to identify all prisoners who reported being prescribed psychiatric medication at prison reception and estimate the proportion of prescriptions for psychiatric medications that were continued on entry to prison. It also sought to establish the factors associated with discontinuation of medication.
Method
Sample
We undertook a retrospective case-note review at five prisons (A-E) located in northern England, all of which accepted remand and convicted prisoners directly from court. Data were collected between June 2008 and March 2009. Sites participated on a voluntary and confidential basis and were selected to represent a range of prisoner populations (Table 1).
Table 1 Sampling
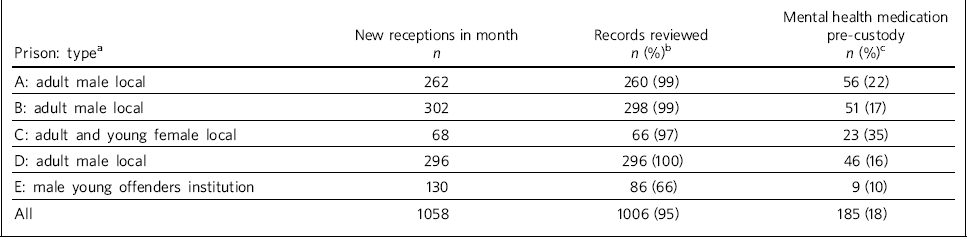
At each prison, a different calendar month was chosen during which prison records were sampled. Prison reception records were used to generate a list of all prisoners newly received into custody within that month. Prisoners transferred from other establishments were excluded. We gathered and reviewed clinical records, with assistance from prison healthcare staff. In total, 95% (n = 1006) of the records eligible for inclusion were successfully reviewed (Table 1). Availability of records was lowest in prison E, the only prison at which an electronic records system had not yet been introduced.
Procedure
Using reception health screening records, we identified all cases where a prisoner reported being on psychiatric medication before being placed in custody. This was defined as any prescribed antidepressant, antipsychotic, hypnotic, anxiolytic and/or central nervous system (CNS) stimulant medication, as listed in the British National Formulary (BNF) chapter 4.1-4.4. 12 A total of 185 records (18% of the total) met this criterion (Table 1).
In all 185 cases, the following details were extracted from the notes: name and dose of pre-custody medication (as reported by the prisoner); details of communication between prison healthcare staff and community prescribers to verify prescriptions; name and dose of medications prescribed in prison; evidence of psychiatric assessment in prison; and evidence of reasons documented for non-prescription, where applicable. Following discussions within the study team, a cut-off of 1 week from reception into prison was chosen for prescriptions to be continued or evidence of reasons for discontinuation to be ascertained. Thus, only entries made in records during the first week of custody were considered.
Analysis
Data were analysed using SPSS version 16 for Windows. Individual medications were categorised in line with the BNF. Descriptive statistics (frequencies and percentages) were used to describe reported prescribed medication use prior to and during custody. We calculated 95% confidence intervals for key findings. Chi-squared tests were used to test for associations between categorical variables. Significance was set at the P>0.05 level.
Results
Prescribed medication prior to custody
Of newly received prisoners, 18% (95% CI 16-21) reported being prescribed psychiatric medication prior to custody (Table 1). Women were more likely to report being in receipt of psychiatric medication than men (χ2 = 12.7, P>0.001). Prisoners arriving at the male young offenders institution were less likely than those at other prisons to report being in receipt of psychiatric medication (χ2 = 3.9, P = 0.047).
In total, the 185 prisoners identified 240 separate psychiatric medications at prison reception (Table 2). Of these, antidepressants accounted for approximately half of all medications (52%), followed by hypnotics/anxiolytics (34%) and antipsychotics (14%). No prisoners in the sample reported being in receipt of CNS stimulants. Most prisoners (58%) reported being in receipt of only one psychiatric medication, 28% said they received two different medications and 15% reported three or more (Table 3). Women were more likely than men to report being prescribed two or more psychiatric medications (70% v. 40%; χ2 = 16.4, P>0.001).
Table 2 Psychiatric medications reported at prison reception, by BNF chapter
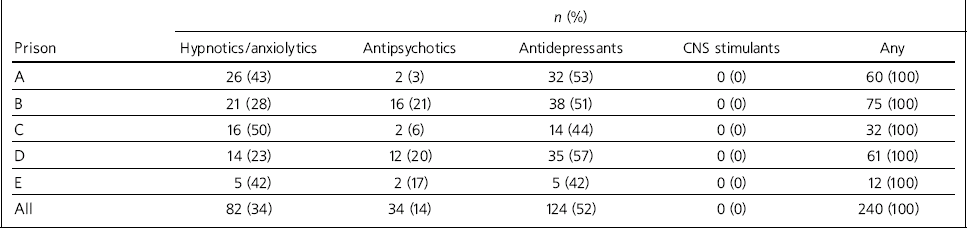
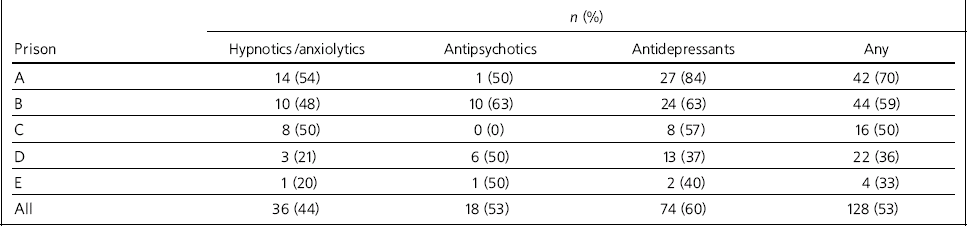
Table 3 Proportion of psychiatric medication continued within 7 days of reception into custody, by BNF chapter
Prescriptions during custody
For each of the individual psychiatric medications identified at prison reception, we determined whether the medication was continued within 1 week of reception into custody. It appeared that 53% (95% CI 47-60) of all prescriptions were continued within 1 week of reception into custody, although prescribing rates varied between prisons (33-70%) (Table 3). Hypnotics/anxiolytics were less likely to be continued than other medication types (χ2 = 4.5, P = 0.035). Women were no more likely than men to have their medication continued (χ2 = 0.2, P = 0.685).
Overall, 47% of prescriptions (n = 112) were not continued within 1 week of arrival in prison. In two cases (2%) this was because prisoners refused their medication in prison. The following factors were positively and significantly associated with discontinuation of medication: response from a community prescriber stating there was no current valid prescription for the medication (21%, n = 23; χ2 = 18.1, P>0.001); prescription of a substitute medication from the same category of the BNF (17%, n = 19; χ2 = 23.6, P>0.001); and discharge (release/transfer) within the first week of custody (21%, n = 23; χ2 = 9.4, P = 0.002). Receiving a psychiatric assessment within the first week of custody was not associated with discontinuation of medication (11%, n = 12; χ2 = 0.2, P = 0.667). In 43% of cases where psychiatric medication was discontinued (n = 48), the prisoner remained in custody for at least 1 week and there was no evidence of patient refusal, disconfirmation from a community prescriber, provision of substitute medication or psychiatric assessment.
Discussion
Almost a fifth of prisoners entering prison (18%) reported that they were currently receiving prescribed psychiatric medication. However, prescriptions for 47% of the medications reported at prison reception were not continued during the first week of custody, in many cases (43%) without a discernable reason.
Strengths and limitations
Confidence can be drawn from the large number of patient records sampled in this study, comprising 95% of those eligible for inclusion. This was largely thanks to the assistance of local prison healthcare staff and availability of electronic record systems in all but one prison. Nonetheless, as only local prisons in the north of England were sampled, care must be taken when generalising our findings to other prison types or geographical regions. Furthermore, we were only able to capture entries made in clinical records during the first week of custody; unrecorded clinical activity or entries made outside this period would have been missed. Similarly, we did not seek to determine whether medication was actually dispensed or administered to the patient.
Our findings are consistent with those of previous studies, Reference Plugge, Douglas and Fitzpatrick8-Reference Condon, Hek, Harris, Powell, Kemple and Price10 confirming that the supply of psychiatric medicines is often interrupted for newly received prisoners. Previously published research in this area has been largely small scale and qualitative. Although such studies have the advantage of generating rich data on participant experiences, in doing so they necessarily focus on prisoner self-report. By using clinical records, our study was uniquely able to evidence and quantify the extent of continuity of prescribing between community and prison. In cases where prisoners were not prescribed the same medication in prison, we sought to discern the reasons behind this: for example, where clarification from outside services had revealed that a prisoner had not been prescribed that medication in the community or where a substitute medication had been prescribed in custody.
Discontinuation of medication on prison entry
Current UK best practice guidelines advise that stopping or reducing doses of psychiatric drugs should be done on a gradual basis and with careful monitoring. 13,14 Furthermore, prison mental health policy clearly states that medication for mental disorder should not be automatically withdrawn on entry into prison without proper clinical assessment. 6 Yet, the findings of this study indicate that in almost half of cases continuity of medicines’ supply was disrupted on entry into custody, often without any discernable reason recorded in the notes.
In some cases in this study we can logically infer that medication was discontinued as a result of active decision-making; this would include cases where substitute drugs were given, medications were disconfirmed by community prescribers, and/or psychiatric assessments were completed. In other cases, mitigating circumstances were present such as prisoners being in custody for very short periods, leaving prison staff insufficient time to verify and arrange prescriptions. However, in almost half of cases where medication was discontinued (43%), none of these conditions applied. It is not clear whether prescriptions were deliberately stopped for reasons not identified by this study or whether medication needs were simply overlooked. Notwithstanding, taken in the context of studies citing significant prisoner distress caused by changes to medication, Reference Plugge, Douglas and Fitzpatrick8-Reference Condon, Hek, Harris, Powell, Kemple and Price10 this finding is concerning.
Adverse effects of abrupt medication discontinuation
We do not dispute that managed discontinuation of medication may, where appropriate, have the potential to benefit a patient. Indeed, patients themselves might request to reduce or stop their medication (two patient refusals were noted in this study). Abrupt withdrawal of psychiatric medication without proper clinical management, however, can have potentially serious health consequences. Discontinuation symptoms can include marked psychological and somatic symptoms (e.g. anxiety, insomnia, dizziness) and can start abruptly within a few days of stopping medication. Reference Moncrieff15-Reference Moncrieff17 Moreover, there may be a risk of relapse of the underlying condition. If medication is withdrawn against the wishes of the patient, it may also contribute to feelings of powerlessness and mistrust, and could discourage prisoners from taking responsibility for managing their illness. Reference Bowen, Rogers and Shaw9 Denial of medication immediately following entry to prison also potentially adds to risk at an already distressing time; indeed, a third of all deaths by suicide in UK prisons occur within the first week in custody. Reference Shaw, Baker, Hunt, Moloney and Appleby11
We recognise that prison healthcare staff work in high-pressure environments, with the added challenge of balancing security needs with prisoners’ health needs. Newly received prisoners frequently arrive at reception en masse, often outside of normal general practice hours and without any physical evidence of existing treatment plans or prescriptions. Furthermore, because of the high incidence of illicit drug use in prisons, certain medications can become ‘currency’. There is also a commonly held perception among staff that some prisoners may make false claims in order to extract valued medication from prescribers. Reference Bowen, Rogers and Shaw9 This might explain why this study found that hypnotics/anxiolytics were the least likely medication type to be continued in custody. Complete discontinuation, however, may be a clinically risky strategy given that abrupt cessation of some medications of this type has been associated with severe discontinuation symptoms, including seizures. Reference Fialip, Aumaitre, Eschalier, Maradeix, Dordain and Lavarenne18
Systemic issues
In highlighting the specific case of the prescription of psychiatric medication, the findings of this study allude to issues arguably endemic in prison healthcare: risk, mistrust, role conflict and poor information-sharing systems. Such factors complicate the process of continuing prescriptions for those genuinely in receipt of psychiatric medication: in the words of an ex-prisoner, ‘not all prisoners are addicts or skivers, yet we are treated as if we are’. Reference Mellor19 Nonetheless, we noted differences in prescribing rates between establishments, which suggests local variation in practices and procedures. If individual prisons have developed systems that better support continuity and equivalence of care for prisoners with mental illness, this may be a cause for some optimism, and fuller exploration of such local strategies is warranted to determine whether these ostensibly successful practices can be replicated elsewhere. Usefully, there appears to be a wealth of existing guidance (under the heading of medicines reconciliation) relevant to developing effective systems for recording medication information among patients being admitted to hospital, which could readily be applied to prison settings. 20,21 Recommendations for standardising information-gathering procedures, establishing minimum data-sets of medication information and clarifying the roles and responsibilities of staff involved would appear to hold as much relevance for healthcare staff working in prisons as in hospitals.
In summary, imprisonment represents an opportunity for reviewing, continuing or improving therapeutic interventions in an otherwise transient and difficult-to-engage patient population. However, all too often it is experienced by prisoners as a disruption in care. This study has shown that continuity of psychiatric medicines’ supply is not assured on entry into prison. This is concerning in light of known high rates of self-harm and suicide in early custody. Given that most prisoners serve short sentences and that all but a few are returned to the community eventually, interest in the findings of this study should not just be limited to prison-based practitioners. Although responsibility for providing patient care might initially be assumed by prisons, this will usually be short lived, immediately ceasing on release. Community and prison-based prescribers must therefore recognise their shared duty for ensuring continuity of care if medicines’ supply for offenders with mental illness is to be maintained across setting boundaries.
Acknowledgement
We express our sincere thanks to the prisons that participated in this study and gratefully acknowledge the healthcare staff that facilitated work at individual sites.








eLetters
No eLetters have been published for this article.