There is now convincing evidence that stressors may trigger the onset of a depressive episode in vulnerable women. Two pathways of vulnerability have been identified, the first emphasising the risk associated with environmental vulnerability such as lack of support and disadvantaged socio-economic conditions (Reference Harris, Brown and BifulcoHarris et al, 1987; Reference Brown, Harris and EalesBrown et al, 1993), and the second emphasising psychological vulnerability such as low self-esteem and helplessness (Reference Bifulco, Brown and HarrisBifulco et al, 1987; Reference Harris, Brown and BifulcoHarris et al, 1990). Several major studies of perinatal emotional disorders have employed the vulnerability—stress model and findings have confirmed its relevance in this specific field. Stressful life events (Reference Paykel, Emms and FletcherPaykel et al, 1980; Reference Bernazzani, Saucier and DavidBernazzani et al, 1997), environmental factors such as support and marital relationships (Reference Cowan, Cowan, Michaels and GoldbergCowan & Cowan, 1988) and maternal attitudes and feelings (Reference Affonso, Lovett and PaulAffonsoet al, 1991) have all been found to contribute significantly to the woman's adjustment to pregnancy and the post-partum period (for a review of risk factors see Reference O'Hara and SwainO'Hara & Swain, 1996). In recent years there has been growing interest in transcultural studies in the field of perinatal mental illness (Reference KumarKumar, 1994). Increasingly, psychosocial factors have been tested and found to be risk factors for postnatal depression in cross-cultural studies assessing both Western and non-Western women (Reference Aderibigbe, Gureje and OmigbodunAderibigbeet al, 1993; Reference Cooper, Tomlinson and SwartzCooperet al, 1999; Reference Lee, Yip and LeungLeeet al, 2000; Reference Danaci, Dinc and DeveciDanaciet al, 2002). The Contextual Assessment of the Maternity Experience (CAME) is designed for the assessment of women during the period encompassing up to 1 year before their expected date of delivery and up to 1 year following delivery. It is based on the contextual interview approach developed by Brown and colleagues (Reference Brown and HarrisBrown & Harris, 1978; Reference Bifulco, Brown and HarrisBifulcoet al, 1994), which has proved to be highly relevant for exploratory work in different cultural settings (Reference Broadhead and AbasBroadhead & Abas, 1998), given that it aims to capture detailed biographical circumstances in people's lives. The psychometric qualities of the CAME have been tested in two samples of women at high risk living in inner London (further details available from the authors upon request).
Structure of the CAME
The CAME provides a detailed picture of a woman's life during the transition to motherhood and enables the assessment of major risk factors for emotional disturbances, especially depression, in women during pregnancy and post-partum, using the same instrument and within a coherent methodological framework. The CAME has three main components: recent life adversity; the quality of social support and key relationships including partner relationship; and maternal feelings and attitudes towards pregnancy, motherhood and the baby. Demographic information is also obtained during the interview.
Recent life adversity
The recent life adversity assessment provides a continuous measure of stressors throughout the pregnancy and post-partum period. This assessment was derived from two specific interview measures: the Adult Life Phase Interview (Reference Bifulco, Bernazzani and MoranBifulcoet al, 2000) and the Life Events and Difficulties Schedule (Reference Brown and HarrisBrown & Harris, 1978). In the tradition of these measures, the recent life adversity component focuses on the level of ‘adversity’ or the intensity of stressors, which is an objective, interviewer assessment of relevant circumstances. The component combines the assessment of both life events and chronic stressors within eight domains: marital/partner relationship; reproduction and parenthood, which includes medical or health complications posing a threat to the pregnancy or to the foetus, and problems concerning the woman's children; the social arena; work and education; housing and finances; the woman's health, including pregnancy and birth complications posing a threat to the mother's health; criminal or legal involvement; and miscellaneous or geopolitical issues (other potential stressors including geopolitical difficulties). Adversity is scored on a four-point scale of intensity: 1, marked; 2, moderate; 3, some; 4, little or none). Each change in adversity level during the study period is recorded and dated, and categories of problems are recorded to give further information about the adversity.
Social support and relationships
The social support and key relationships component was adapted from the Self-Evaluation and Social Support (SESS) measure (Reference O'Connor and BrownO'Connor & Brown, 1984). Women are asked about their relationship with two supportive figures named as being ‘very close’ or confidants; if the woman has a partner, his level of support is automatically assessed whether or not he was chosen as a confidant. Antenatally, for each relationship, seven key topics are assessed: confiding, emotional support, positive and negative interactions, joint activity, feelings of attachment, and overall quality of relationship. The overall quality of relationship scale takes into account and ‘summarises’ the other ratings; it is a seven-point scale, combining a four-point rating scale of supportiveness (very good, good average, poor average and poor) with an assessment of either the conflicting or indifferent tone for all but the ‘very good’ rating. At the postnatal interview, for each relationship, assessments are made of changes in overall quality of relationships since the antenatal interview and changes in emotional support since the baby's birth. Additionally, global assessments are made of the emotional support received from all others in the woman's social network since the baby's birth.
Maternal feelings and attitudes
The component evaluating maternal feelings and attitudes towards pregnancy, motherhood and the baby was adapted from the SESS measure and the Childhood Experience of Care and Abuse scale (Reference Bifulco, Brown and HarrisBifulcoet al, 1994). As emotional reactions may fluctuate during the pregnancy, key sub-scales are rated for two periods: the beginning of pregnancy, and currently (around the time of prenatal interview). Three topics, measured on a four-point scale, are included: commitment to the current pregnancy; positive feelings about the pregnancy; and negative and anxious feelings about the pregnancy. Positive feelings are assessed separately from negative ones to allow the recording of potentially contradictory feelings related to maternity. Factual information about the pregnancy is also recorded, including whether it was planned, if so, whose decision it was, and the time from the decision being made to becoming pregnant. Postnatally, this section focuses on the woman's feelings and attitudes about her baby and motherhood, and provides specific information about the perinatal context. There are six topics, measured on a four-point scale: fulfilment in the motherhood role; closeness with the baby; antipathy towards the baby; how far the baby is perceived as difficult; competence as a mother; and incompetence as a mother. Information is also obtained about feelings and attitudes of the woman's partner towards the baby. Key scales are rated for two periods: the first few weeks following birth, and around the time of postnatal interview. Information is also collected about the birth and breast-feeding.
Transcultural Study of Postnatal Depression
The aim of the Transcultural Study of Postnatal Depression (TCS—PND) was to develop (or modify), translate and validate research instruments that could be used in future studies of postnatal depression in different countries and cultures. The instruments were chosen to assess key aspects of the maternity experience, namely clinical diagnosis, the psychosocial context of pregnancy and motherhood, maternal attachment style, mother-infant interaction, the child's environment, and health service structure, use and its associated costs. The modified and translated research tools were piloted to test how well they worked in a perinatal setting and in different languages and populations. The use of the CAME to assess the psychosocial context of pregnancy and motherhood, reported in this paper, is part of the TCS—PND.
METHOD
Study sites
Ten centres in eight countries participated: Bordeaux and Paris (France), Dublin (Ireland), Florence (Italy), Iowa City (USA), Keele and London (UK), Porto (Portugal), Vienna (Austria) and Zurich (Switzerland). Details are given by Asten et al (Reference Asten, Marks and Oates2004, this supplement).
Sample
Eligible women were approached in antenatal clinics and classes by a researcher who obtained informed consent from those who agreed to take part. Antenatally 296 women were interviewed, of whom 249 also completed a postnatal interview. Demographic characteristics of the sample are described by Astenet al (Reference Asten, Marks and Oates2004, this supplement).
Procedure
Participants were first interviewed during the third trimester of pregnancy (mean 7.97 months, s.d.=0.91) and again at around 6 months following delivery (mean 25.83 weeks, s.d.=6.54), except in the Zurich sample where the mean was 17.02 weeks (s.d.=1.57).
Other measures
The Structured Clinical Interview for DSM—IV Axis I Disorders (SCID—I; Reference First, Spitzer and GibbonFirstet al, 1994) is a semi-structured interview for making the major DSM—IV diagnoses (American Psychiatric Association, 1994). A research version designed for use with non-patient populations, the SCID—I/NP (Reference First, Gibbon and SpitzerFirstet al, 1996), was modified for this study to produce an instrument for assessing postnatal depression in different cultural contexts: the SCID—PND (Reference Gorman, O'Hara and FigueiredoGorman et al, 2004, this supplement). The SCID—PND was administered at both antenatal and postnatal interviews, thus providing a continuous assessment of depressive disorder from the beginning of pregnancy up to 6 months postnatally; DSM—IV diagnoses were made of both major and minor depression, and time of onset was recorded. The SCID—PND was administered at the same time as the CAME at both antenatal and postnatal interviews. Complete data from both interviews at both time points are available for 238 participants, and the analyses reported here are based on this subsample.
A fifth of the participants (22%; 53 of 238) had an onset of major or minor depression during pregnancy or within 6 months of delivery. Rates of onset differed significantly between centres (χ2=23.12, P<0.006), from 5% in Zurich to 40% in Bordeaux. Seventeen women (7%) had an onset of depression in pregnancy, with no significant difference between centres (range 0% in Dublin and Vienna to 20% in Bordeaux); 41 (17%) had a post-partum onset, with significant differences between centres (χ2=23.83,P<0.007; range 0% in Florence to 35% in Paris).
Training and reliability
Interviewers were trained in the use of the CAME at a 4-day workshop at the University of Keele, with refresher training provided at subsequent workshops. Each team translated the interview and rating schedules where necessary into their own language (French, German, Portuguese and Italian). As with other contextual interviews, the CAME did not require systematic back-translation, but translators were required to be familiar with the rating system to ensure that questions would elicit the appropriate material required for rating. Translations were closely discussed with O.B. and minor adjustments were made to optimise the clarity of concepts and the flow of the interview in each language. The English reference manual was retained, as all team members read English.
Each team provided complete ratings for at least five cases (nearly a fifth of the sample), which were checked for consistency by O.B. The ratings were then discussed in detail in face-to-face meetings between O.B. and each team, and clarifications were made regarding difficult or unclear issues. Subsequent cases were rated on a consensus basis within local teams. Teams kept in close touch with O.B., referring back difficult cases for checking and further consensus. This type of supervision has proved successful in ensuring reliability between raters in other studies using contextual assessments (Reference Broadhead and AbasBroadhead & Abas, 1998; Reference Bifulco, Bernazzani and MoranBifulcoet al, 2000).
Analyses
Data were entered into an Access database prepared by the coordinating centre and subsequently converted into the Statistical Package for the Social Sciences for analysis. Analyses were initially conducted separately for the three CAME components using two strategies. First, comparisons between centres were carried out using one-way analysis of variance or χ2 to check for significant differences between centres. Second, analyses were conducted on the pooled data, using t-tests orχ2, and controlling if necessary for centre differences, in order to verify whether well-known associations between risk factors and depression were replicated using the CAME. (Data from two participants interviewed in Keele were included with the London data.) In addition, relationships between CAME components were examined and a preliminary logistic regression was applied to estimate the impact of the three CAME components on the occurrence of perinatal depression.
RESULTS
Recent life adversity
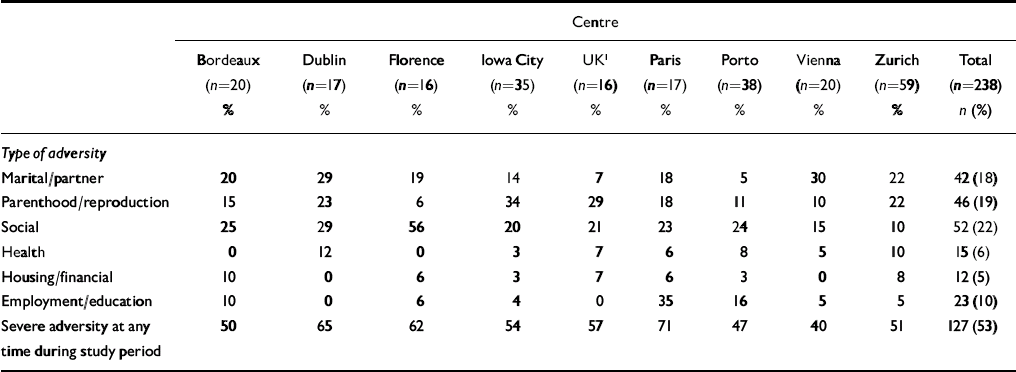
At the antenatal interview, 37% of women (87 of 238) had experienced severe adversity (either ‘marked’ or ‘moderate’ on the rating scale) in at least one life domain during the prenatal study period — that is, 12 months prior to the expected date of delivery. At the postnatal interview, overall 36% of women (86 of 238) had experienced severe adversity since the antenatal interview. Altogether 53% (127 of 238) experienced severe adversity at some point during the study period (12 months prior to the expected date of delivery up to the time of the postnatal interview). Although the proportions of women with any severe adversity during the study period varied between centres (Table 1) the differences were not statistically significant. Consistent with results of other studies, severe adversity occurred most frequently in the marital, social and parenthood domains. Overall, 18% of women had adversity in the marital domain, 22% in the social domain and 19% in the parenthood domain. There was no severe adversity in the geopolitical domain, virtually none in the criminal or legal domain and 10% or less overall in each of the employment/education, health and financial/housing domains. A notable exception was the Paris centre, where 35% of women had severe adversity in the employment/education domain.
Table 1 Proportion of women interviewed both antenatally and postnatally who experienced severe adversity during the study period
| Centre | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Bordeaux (n=20) % | Dublin (n=17) % | Florence (n=16) % | Iowa City (n=35) % | UK1 (n=16) % | Paris (n=17) % | Porto (n=38) % | Vienna (n=20) % | Zurich (n=59) % | Total (n=238) n (%) | |
| Type of adversity | ||||||||||
| Marital/partner | 20 | 29 | 19 | 14 | 7 | 18 | 5 | 30 | 22 | 42 (18) |
| Parenthood/reproduction | 15 | 23 | 6 | 34 | 29 | 18 | 11 | 10 | 22 | 46 (19) |
| Social | 25 | 29 | 56 | 20 | 21 | 23 | 24 | 15 | 10 | 52 (22) |
| Health | 0 | 12 | 0 | 3 | 7 | 6 | 8 | 5 | 10 | 15 (6) |
| Housing/financial | 10 | 0 | 6 | 3 | 7 | 6 | 3 | 0 | 8 | 12 (5) |
| Employment/education | 10 | 0 | 6 | 4 | 0 | 35 | 16 | 5 | 5 | 23 (10) |
| Severe adversity at any time during study period | 50 | 65 | 62 | 54 | 57 | 71 | 47 | 40 | 51 | 127 (53) |
Analyses of the pooled data indicated a significant association between severe adversity and onset of perinatal depression (χ2=7.92,P<0.005); 29% (37 of 127) of women with severe adversity experienced a depressive episode compared with 14% (16 of 111) of women without severe adversity, a relative risk ratio of 2.44 (95% CI 1.27-4.69).
Quality of social support during pregnancy
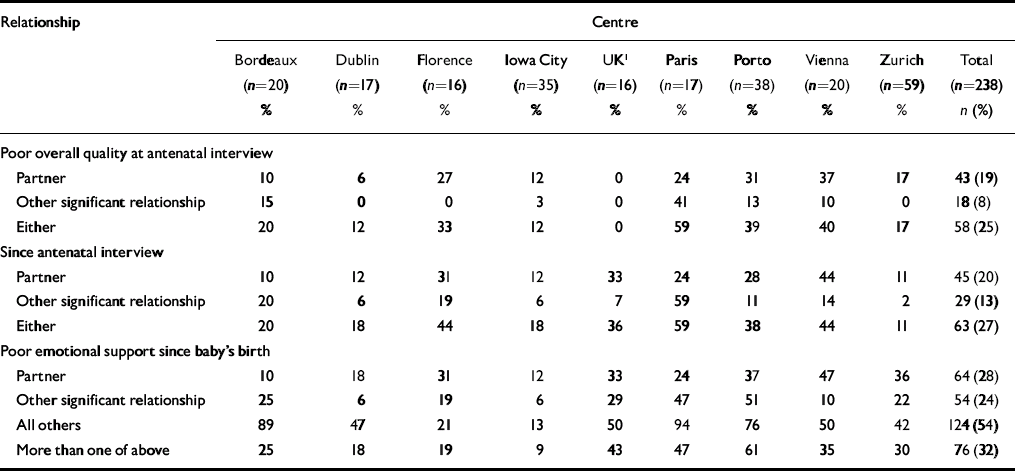
For purposes of comparison between prenatal and postnatal support, the rating of prenatal overall quality of relationships for each of the two significant relationships, dichotomised into good (score 1-3) and poor (4-7), was used in analyses (Table 2). A fifth (19%) of the women had a poor rating for their partner relationship, with not quite statistically significant differences between centres (χ2=15.38,P<0.052) and 8% had a poor rating for their other significant relationship, with significant differences between centres (χ2=40.39, P<0.001). Overall, 25% of women had a poor rating for either partner and/or their other relationship, with significant differences between centres (χ2=30.39, P<0.001). Only 2% of women had a poor rating for both relationships.
Table 2 Proportion of women interviewed both antenatally and postnatally who had poor relationships
| Relationship | Centre | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Bordeaux (n=20) % | Dublin (n=17) % | Florence (n=16) % | Iowa City (n=35) % | UK1 (n=16) % | Paris (n=17) % | Porto (n=38) % | Vienna (n=20) % | Zurich (n=59) % | Total (n=238) n (%) | |
| Poor overall quality at antenatal interview | ||||||||||
| Partner | 10 | 6 | 27 | 12 | 0 | 24 | 31 | 37 | 17 | 43 (19) |
| Other significant relationship | 15 | 0 | 0 | 3 | 0 | 41 | 13 | 10 | 0 | 18 (8) |
| Either | 20 | 12 | 33 | 12 | 0 | 59 | 39 | 40 | 17 | 58 (25) |
| Since antenatal interview | ||||||||||
| Partner | 10 | 12 | 31 | 12 | 33 | 24 | 28 | 44 | 11 | 45 (20) |
| Other significant relationship | 20 | 6 | 19 | 6 | 7 | 59 | 11 | 14 | 2 | 29 (13) |
| Either | 20 | 18 | 44 | 18 | 36 | 59 | 38 | 44 | 11 | 63 (27) |
| Poor emotional support since baby's birth | ||||||||||
| Partner | 10 | 18 | 31 | 12 | 33 | 24 | 37 | 47 | 36 | 64 (28) |
| Other significant relationship | 25 | 6 | 19 | 6 | 29 | 47 | 51 | 10 | 22 | 54 (24) |
| All others | 89 | 47 | 21 | 13 | 50 | 94 | 76 | 50 | 42 | 124 (54) |
| More than one of above | 25 | 18 | 19 | 9 | 43 | 47 | 61 | 35 | 30 | 76 (32) |
Overall, poor prenatal overall quality of relationship with the partner was significantly associated with both antenatal and postnatal onset of depression. Women with a poor partner relationship were more than three times as likely to have an antenatal onset of depression (16% compared with 5%: χ2=7.03,P<0.008) and more than twice as likely to have a postnatal onset (30% compared with 14%: χ2=6.44, P<0.01) as women with a good partner relationship. Poor overall quality for the other significant relationship was also associated with onset of antenatal depression (χ2=5.58,P<0.01) and not quite significantly with onset of depression postnatally (χ2=3.42,P<0.06).
Quality of social support post-partum
The postnatal support ratings took into account changes in the two key relationships, and were therefore computed differently. First, any low rating for overall quality of relationship at any time between the antenatal interview and the postnatal interview was computed for both of the two key relationships (Table 2). Overall 20% of women had at least one poor rating for partner, with significant differences between centres (χ2=16.04, P=0.04) and 13% had at least one poor rating for their other significant relationship with significant differences between centres (χ2=42.90,P<0.001). A quarter of women (27%) had at least one poor rating for either of the two relationships, again with significant differences between centres (χ2=26.44,P<0.001). Only 5% of women overall had a poor rating for both relationships. Second, any low rating for emotional support since the baby's birth (3 or 4 on the rating scale) was computed for both of the two key relationships and for ‘all other relationships’. Overall, 28% of women had at least one poor rating for partner, with no significant differences between centres, and 24% had at least one poor rating for their other significant relationship, with significant differences between centres (χ2=30.89,P<0.001). Large and varying proportions of women in each centre had at least one poor rating for emotional support from others (χ2=44.63, P<0.001), with an overall rate of 54%. In order to distinguish women who consistently lacked emotional support, a variable was computed to take into account low ratings in both key relationships and ‘all other relationships’. Overall, 32% of women had a poor rating in at least two out of these three categories, with significant centre differences (χ2=29.56, P<0.001 and 6% had a low rating in all three. Overall, 34% of women had no poor ratings at all (range 6% in Paris to 60% in Iowa City).
Onset of depression in the post-partum period was more than twice as likely where there was poor overall quality of relationship with the partner (29% v.13%; χ2=6.86,P=0.009), with the other significant relationship (34% v.15%;χ2=6.59, P=0.01) or with either (30% v.12%; χ2=10.24,P<0.001). Onset was also more than twice as likely where there was a low rating for emotional support from the other significant relationship (32% v.13%; χ2=10.38,P<0.001). A low rating for emotional support from the partner, however, was not associated with onset of post-partum depression, and neither was a low rating for support from all others. Where there was a rating of low emotional support from more than one source (partner, other significant relationship and others), onset of depression was more than twice as likely: 29% v.12% (χ2=11.11, P<0.001).
Maternal feelings and attitudes
Antenatally, the internal consistency of the component assessing feelings at the beginning of pregnancy was good (pooled sample α=0.82) and that for assessing feelings at interview was adequate (pooled sample α=0.75). For individual centres, α for the scale assessing feelings at the beginning of pregnancy ranged from 0.64 (Zurich) to 0.89 (Dublin and Florence), and α for feelings at interview ranged from 0.63 (Iowa City) to 0.90 (Dublin).
Raw scores were summed to obtain a continuous score reflecting negative feelings. Two separate indices were computed, each on a scale of 3 to 12, the sum of three variables rated 1 to 4. Analysis of variance showed that mean scores varied between centres, with post hoc tests indicating that scores for both initial and current indices were significantly lower in Florence and Zurich than those in all the other centres except Bordeaux. As might be expected, scores on both indices were higher where the pregnancy was not planned: initial index, planned 4.54 (s.d.=1.48) v. unplanned 7.99 (s.d.=2.52), t=12.09, P<0.001; current index, planned 4.51 (s.d.=1.54)v.unplanned 5.73 (s.d.=2.06), t=5.02, P<0.001. Mean scores for the group of women whose pregnancies were unplanned were lower for the current index than the initial index, indicating more positive feelings as the pregnancy progressed. Scores on the current index were significantly higher where there was an onset of depression during pregnancy: 6.29 (s.d.=2.39) v.4.66 (s.d.=1.68), t=2.77, P=0.01. Interestingly, scores on both initial and current indices were also higher where there was postnatal onset of depression: initial index, 6.50 (s.d.=2.12) v.5.28 (s.d.=2.31), t=2.26, P=0.02; current index, 5.44 (s.d.=2.07)v.4.64 (s.d.=1.70), t=2.63, P=0.01.
Postnatally, 16 items reflected feelings occurring at different time periods: feelings during the first few weeks following birth about motherhood (three items) and towards the child (three items); and feelings around the time of postnatal interview about motherhood (three items) and towards the child (seven items). Internal consistency of the whole component for the pooled sample was good (α=0.83) with all items contributing. For the individual centres,α was 0.73 or above for all centres except Iowa City where it was 0.66. The whole component was used in this study to reflect negative feelings about motherhood and the child both soon after birth and at interview. As with the antenatal maternal feelings/attitudes component, the index was a continuous score, computed by summing raw scores on individual items (reversed as appropriate). Thus, the overall index was on a scale of 16 to 64, the sum of 16 items each rated 1 to 4. Analysis of variance revealed a difference in mean scores between centres, withpost hoc tests showing that the Zurich group scores were lower than those of five other centres and that scores in Porto were lower than those in Bordeaux. For the pooled sample, scores were significantly higher (indicating more negative feelings) where the mother had a post-partum onset of depression (t=6.26, P<0.001) and also where there was an onset of depression in pregnancy (t=2.48, P=0.01).
Relationships between CAME components
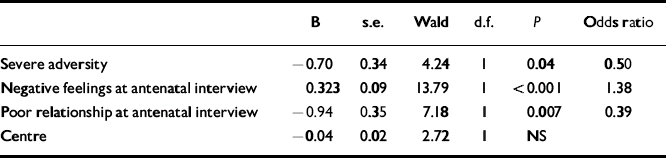
Since there were correlations between CAME components, for example, adversity with antenatal negative feelings (r s=0.17, P=0.007) and with a poor relationship at antenatal interview (r s= 0.12, P=0.05), logistic regression was conducted to test the effects of each of the components while controlling for the effects of the others and for study centre. This analysis confirmed that adversity, poor relationship with partner or significant other and negative feelings about the pregnancy at the antenatal interview all predicted onset of depression during the perinatal period, when controlling for study centre (Table 3).
Table 3 Variables predicting onset of perinatal depression
| B | s.e. | Wald | d.f. | P | Odds ratio | |
|---|---|---|---|---|---|---|
| Severe adversity | -0.70 | 0.34 | 4.24 | 1 | 0.04 | 0.50 |
| Negative feelings at antenatal interview | 0.323 | 0.09 | 13.79 | 1 | <0.001 | 1.38 |
| Poor relationship at antenatal interview | -0.94 | 0.35 | 7.18 | 1 | 0.007 | 0.39 |
| Centre | -0.04 | 0.02 | 2.72 | 1 | NS |
DISCUSSION
The study demonstrated successful use of the CAME in ten centres and in five different languages. The CAME enabled adequate assessment of the major domains relevant to the psychosocial context of the maternity experience in different cultures, and was described by interviewers as a useful instrument yielding a substantial amount of information on women's lives. Overall, the instrument showed acceptable psychometric properties in its first use in different cultural settings.
The concurrent validity, and to a lesser extent the predictive validity, of the CAME components were evidenced by their association with perinatal depression. Poor prenatal relationships, especially with partner, were associated with onset of depression both prenatally and postnatally. Prenatal scales reflecting feelings towards the pregnancy were related to onset of depression both antenatally and postnatally, as were the postnatal scales reflecting feelings towards motherhood and the child. Overall adversity was related to the presence of perinatal depression. Logistic regression confirmed that adversity, poor social support and negative feelings toward pregnancy all contributed to the onset of perinatal depression.
The CAME also yielded interesting preliminary results regarding similarities and differences between centres. Rates of severe adversity were high in all samples, ranging from 40% to 71% with a rate of 53% in the pooled sample, possibly reflecting the high risk of women in inner-city areas. A fifth of the sample had a poor relationship with their partner; the lowest rates of poor partner relationship were found in Bordeaux, Zurich and Dublin. More striking differences between centres were found in the quality of relationships with confidants chosen by the women themselves, with prenatal rates of poor relationships ranging from 0% in several centres to an unexpectedly high rate of 41% in Paris. Centre differences among these small, unrepresentative samples cannot be taken to indicate real differences between populations of pregnant and post-partum women. The high rates of employment/education adversity and poor relationships in Paris, for example, may be a spurious finding because of the small numbers in each centre and bias in the selection of cases.
Internal consistency for the component of maternal feelings and attitudes towards pregnancy, motherhood and the baby was adequate for both the prenatal and postnatal scales in the pooled and individual samples. As expected, scores of negative feelings for women with unplanned pregnancies were higher at the beginning of pregnancy than at current interview, suggesting an adjustment to the pregnancy recorded by the CAME.
The CAME is relatively demanding in terms of interview and rating time. It integrates several assessments within the same instrument, based on a coherent theoretical background, thus providing a significant amount of information unavailable elsewhere in a single instrument. This study constitutes a first step in the piloting of the instrument for use in different cultural settings. At this stage, its flexibility and psychometric properties appear sufficiently promising to justify its use to assess the maternity experience in different cultures. Clearly, however, further assessments of the instrument are required in larger, more representative samples of the cultures examined in this study.
In summary, this study indicates that the CAME works well as a means of exploring psychosocial risk factors relevant to the maternity experience in different countries and cultures. These preliminary analyses were carried out in a spirit of piloting and exploration on small samples from a range of countries. Although additional, larger studies are required, our results underscore the potential of the instrument for researchers aiming to study in detail and compare the maternity experience in different settings and cultures.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The Contextual Assessment of the Maternity Experience (CAME) provides an assessment of major risk factors for emotional disturbances in women during pregnancy and post-partum.
-
▪ Adversity, poor support and negative feelings towards pregnancy all contribute to onset of perinatal depression.
-
▪ Reliable use of the CAME across several European and one US centre indicates it can be used as an assessment of risk for perinatal depression in varied international contexts.
LIMITATIONS
-
▪ Samples may not be representative of women generally in each centre.
-
▪ The CAME is demanding in terms of interview and rating time.
-
▪ Larger samples are required to disentangle the relative effects of contributing factors to onset of perinatal depression.
Acknowledgements
The development of the CAME measure was supported by a research fellowship. to Dr Odette Bernazzani from the Fonds de Recherche en Santé du. Québec and by additional support from the Fernand Seguin Research. Centre in Montréal, Canada. We also wish to thank Geneviève. Mailloux, Isabelle Ménard and Marie-Noëlle Gagnon for their. contribution to the training manuals.








eLetters
No eLetters have been published for this article.