Obesity is a primary threat to public health. Childhood obesity strongly tracks with age( Reference Singh, Mulder and Twisk 1 ), raising the risk of mortality, CVD, certain cancers and osteoarthritis, as well as other conditions in adulthood( Reference Calle, Rodriguez and Walker-Thurmond 2 – Reference Pischon, Boeing and Hoffmann 5 ). In adults a key driver of the metabolic consequences of excess fat is that located abdominally, or central adiposity, which predicts mortality and CVD independent of BMI( Reference Pischon, Boeing and Hoffmann 5 – Reference Huxley, Mendis and Zheleznyakov 7 ). Currently 32 % and 17 % of children and adolescents in the USA are overweight and obese, respectively( Reference Ogden, Carroll and Kit 8 ). Moreover, waist circumference (WC) of children has increased over time and some evidence suggests that the rate of increase in WC has outpaced that of BMI( Reference McCarthy, Ellis and Cole 9 – Reference Griffiths, Gately and Marchant 13 ). Therefore, it is paramount to identify modifiable risk factors of excess total and abdominal weight gain in children to help prevent or reverse obesity and its related co-morbidities both in childhood and later life.
To date it remains unclear as to whether intake of sugar-sweetened beverages (SSB) has specific effects on central adiposity above and beyond those for total adiposity. Few studies in older children have obtained WC measurements( Reference Althuis and Weed 14 – Reference Williams, Strobino and Brotanek 16 ). One prospective observational study of 170 girls found that greater consumption of SSB at age 5 years was related to higher WC at each biennial follow-up until the age of 15 years( Reference Fiorito, Marini and Francis 15 ). Conversely, in a trial of thirty-two girls (11–15 years) on a 12-week diet supplying 6276 kJ/d (1500 kcal/d), soda consumption was not related to changes in either BMI or WC( Reference Williams, Strobino and Brotanek 16 ). Neither of these studies reported standardized estimates, however, which prevents the direct comparison of effect sizes between different adiposity outcomes (BMI v. WC). As well, they did not adjust models predicting changes in WC for total body fat or BMI. Because of the important role central adiposity plays in disease development, understanding whether SSB intake has detrimental effects on abdominal weight gain independent of total body fat is critical to further our understanding of the relationship of SSB intake to metabolic disease risk( Reference Bray 17 ).
In US children and adolescents, SSB are a major source of added sugars( Reference Ervin and Ogden 18 ) and contribute greatly to total energy intake( Reference Reedy and Krebs-Smith 19 ). Consumption of these products has increased in parallel to the obesity epidemic both in the USA and abroad( Reference Wang, Bleich and Gortmaker 20 – Reference Popkin, Adair and Ng 22 ). From a life-course approach, a key developmental period for targeted obesity prevention efforts regarding beverage intake may be among older children, since secular trend data indicate that the largest increases in SSB consumption have occurred in this age group( Reference Wang, Bleich and Gortmaker 20 ). The seminal work by Ludwig et al. provided the first evidence supporting the relationship between SSB intake and excess weight gain in late childhood( Reference Ludwig, Peterson and Gortmaker 23 ), replicated in some studies( Reference Fiorito, Marini and Francis 15 , Reference Berkey, Rockett and Field 24 – Reference Laska, Murray and Lytle 28 ), but not others( Reference Laurson, Eisenmann and Moore 29 – Reference Mundt, Baxter-Jones and Whiting 31 ). Methodological differences including small sample sizes, lack of repeated measures, consideration of dietary reporting errors and adjustment for total energy may partly account for these inconsistent results. Moreover, few prospective studies used gold-standard measures of total adiposity such as dual-energy X-ray absorptiometry (DXA)( Reference Fiorito, Marini and Francis 15 , Reference Mundt, Baxter-Jones and Whiting 31 ) and no studies examined independent effects on central adiposity.
As the current evidence on the relationship between SSB intake and central obesity is limited and lacking, and no data have examined this association with adequate control for changes in total adiposity, our study objectives were to: (i) examine the association between change in SSB intake from ages 10 to 13 years and WC, BMI and body fat at 13 years; and (ii) determine whether the relationship with WC is independent of total adiposity. We hypothesized that change in SSB intake would be related to all measures of adiposity but would not have any additional effects on WC.
Methods
Participants
The Avon Longitudinal Study of Parents and Children (ALSPAC) was designed to examine the effects of environmental factors on the health and development of children( Reference Golding, Pembrey and Jones 32 , Reference Fraser, Macdonald-Wallis and Tilling 33 ). Recruitment of pregnant women with expected delivery dates between April 1991 and December 1992 and living in the County of Avon located in South-West England started in 1990 with 14541 participants. At age 7 years, children were invited to clinical examinations where more detailed information was collected. Dietary, anthropometric, body composition by DXA and physical activity data were available at various ages. Anthropometry was obtained approximately at ages 10, 11 and 13 years, body fat mass by DXA at ages 11 and 13 years and physical activity at age 13 years.
For the present study, participants were excluded if missing anthropometric, DXA, dietary and/or physical activity information, our main variables of interest. Anthropometry and DXA measures were available on 5102 children. Of these, 2455 (48 %) individuals also had dietary and physical activity information available. Those missing dietary and physical activity data (n 2647) were slightly older (0·3 (sd 2·7) months) at baseline than those with complete data (P<0·0001). There were no differences in height (P=0·70), BMI (P=0·89) and WC (P=0·89) and in the prevalence of overweight at 10 years (P=0·57) and maternal overweight/obesity (P=0·44) between groups. A higher proportion of mothers had an advanced level or college degree (49 % v. 42 %) among children with complete data compared with those with missing data (P<0·0001; data not shown).
The study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human participants were approved by the ALSPAC Law and Ethics Committee and the Local Research Ethics Committees and the Institutional Review Board of Boston University Medical Center. Parents provided written informed consent at the time of enrolment and for any additional measures.
Dietary assessment and sugar-sweetened beverages
Three-day dietary records were obtained prior to the clinic visits at ages 10 and 13 years. Children were asked to record all foods and beverages consumed in household measures with parental assistance, as needed. At clinic visits, records were reviewed for completeness by a nutrition fieldworker. Food codes were assigned and weights applied to all foods and beverages using the Diet In Data Out (DIDO) system developed by the MRC Human Nutrition Research Unit in Cambridge, UK( Reference Price, Paul and Key 34 ). This software allows for the entry of portion sizes and cooking method (e.g. frying). Portion sizes were calculated from those reported in dietary records. Average daily nutrient intakes were determined using the nutrient analysis program BRIGADE, based on the fifth edition of McCance and Widdowson’s food tables and supplements( Reference Holland, Welch and Unwin 35 ). SSB were defined as full-sugar fruit squashes, cordials and fizzy drinks (i.e. soda) with added sugar, whereas reduced-sugar or artificially sweetened versions were considered diet beverages. Squashes and cordials were coded either as full volume, which includes syrup and added water, or as concentrate without water. Consistent with a previous ALPSAC study( Reference Johnson, Mander and Jones 36 ), 140g of water was assumed for every 40 g of concentrate to equal 180g (1 cup). A serving of SSB was defined as 180g.
Anthropometry and body composition
Adiposity was assessed using the same protocols at ages 10 and 13 years. Weight was measured in kilograms using a Tanita body fat analyser (model TBF 305) and height in millimetres using a Harpenden stadiometer. BMI was calculated as weight divided by the square of height (kg/m2). WC was measured to the nearest millimetre at the midpoint between the lowest rib and the top of the iliac crest. For the current analysis, those having a BMI corresponding to a predicted BMI at age 18 years ≥25kg/m2, based on International Obesity Task Force age- and sex-specific weight categories, were grouped into an overweight/obese category( Reference Cole, Bellizzi and Flegal 37 ). Total body fat mass (TBFM) was measured by DXA using a Lunar Prodigy narrow fan beam densitometer to the nearest 0·01g.
Physical activity and dietary reporting errors
Physical activity was collected at age 13 years. Children wore a uniaxial accelerometer (Actigraph, Fort Walton Beach, FL, USA) around their waist during waking hours for 7d( Reference Ness, Leary and Mattocks 38 ), which measured activity in counts per minute (cpm). Participants with ≥3d of at least 10h of data daily were used in all analyses. Dietary reporting errors were assessed at age 13 years when both diet and physical activity were collected at the same time point. As described elsewhere( Reference Noel, Mattocks and Emmett 39 ), objectively measured physical activity levels were applied to physical activity coefficients in energy requirement equations building upon the methods developed by Huang et al.( Reference Huang, Howarth and Lin 40 ).
Covariates
Mothers self-reported their weight and height. Maternal overweight/obesity was defined as BMI ≥25kg/m2. Maternal educational attainment was defined as low (certificate of secondary education or vocational qualification), medium (O level) and high (A level, college degree or higher). This variable was strongly related to weekly family income (<£120, £120 to <£240, £240 to <£480, £480 to <£800 and ≥£800; P<0·0001). Adjustment of regression models for family income instead of maternal educational status did not change our results (data not shown). Therefore, maternal educational status was considered an adequate proxy for socio-economic status. Tanner stage (5-point scale) for pubic hair growth was self-reported by postal questionnaire sent to the parent of the child around the age of 13 years( Reference Morris and Udry 41 ). Tanner stage was collapsed to pubertal stages (pre=1, early=2–3 and late=4–5) to minimize the effect of potential misclassification. Pubertal assessment and attendance at the corresponding 13 years clinic visit were not necessarily concurrent; thus individuals whose questionnaires were completed 12 months or more before or after the clinic visit had pubertal stage set to missing. Dieting status at age 13 years was self-reported by questionnaire in response to the question ‘During the past year, did you go on a diet to lose weight or keep from gaining weight?’ (with response options of ‘always on diet’, ‘often’, ‘several times’, ‘a couple of times’ and ‘never’). This variable was collapsed to a dichotomous measure (no=never and yes=all other responses). Dietary covariates that may influence adiposity included change in intakes of fruit juice (100 % fruit juice without added sugar, g/d), fruit and vegetables (g/d) and percentage of energy from fat (% fat/d) from 10 to 13 years of age. Covariate information was available for most participants as follows: pubertal stage (n 2231, 91 %), maternal overweight/obesity (n 1880, 77 %), maternal educational attainment (n 2292, 93 %) and dieting at age 13 years (n 2135, 87 %). To account for missing status, dummy variables were created for each covariate and included in multivariable regression models (e.g. those with pubertal stage at age 13 years=0 and those missing pubertal stage at age 13 years=1).
Statistical analyses
Data were analysed using the SAS statistical software package version 9·2. Two-sided P values <0·05 were considered significant. To examine whether our final sample was biased, we compared baseline demographics between participants excluded because of missing dietary or physical activity information (n 2647) and those with complete data (n 2455) using Student’s t tests and χ 2 tests for sample means and proportions, respectively.
The main exposure variable was change in SSB consumption (SSB intake at age 13 years minus SSB intake at age 10 years). We examined several outcome variables of total adiposity at age 13 years: weight (kg), BMI (kg/m2) and TBFM (kg). Central fat was indirectly measured by WC (cm) at age 13 years. Separate sets of models were created using multivariable linear regression and a similar model building strategy employed for each outcome. Model 1 adjusted for sex and SSB intake, adiposity and age at baseline. In TBFM models, BMI at age 10 years was used for baseline adiposity adjustment because DXA was not measured at baseline. We also included terms for height and height2 at 10 years of age as previous work in the study population demonstrated quadratic relationships between height and fat mass( Reference Ness, Leary and Mattocks 38 ). Model 2 included model 1 factors and physical activity at age 13 years (cpm), pubertal stage at age 13 years, maternal overweight/obesity status, maternal education, dieting at age 13 years, and changes in intakes of fruit juice (g/d), fruits and vegetables (g/d) and total fat (% fat/d). In model 3, terms for dietary reporting errors (under-reporter, plausible reporter, over-reporter) were added. Our primary model (model 4) consisted of model 2 terms and excluded implausible dietary reporters as previously described. The unique effect of SSB on WC independent of total adiposity was examined by modelling WC at age 13 years as a function of change in SSB with terms for TBFM or BMI at age 13 years. As measures of central and total adiposity are correlated during ages 10 and 13 years, we tested for multicollinearity using variance inflation factors where values greater than 10 were considered evidence of multicollinearity( Reference Neter, Wasserman and Kutner 42 ).
While total energy is likely in the causal pathway between SSB intake and adiposity, we adjusted our models for baseline total energy (kcal/d) and change in total energy (kcal/d) from ages 10 to 13 years in secondary analyses. To test for effect modification by baseline SSB consumption or sex, as suggested by some literature, we included interaction terms for baseline SSB (i.e. SSB at age 10 years×change in SSB) or sex (i.e. sex×change in SSB) separately in models 3 and 4. Standardized β estimates were calculated by transforming each adiposity outcome into multiples of standard deviations. The standardized β thus represents the change in number of sd of the dependent variable per 1 sd change in the independent variable. This allows for the comparison of the effects of one predictor on multiple outcomes and accounts for differences in units.
Results
Children were 10·6 (sd 0·2) years at baseline (age 10 years; Table 1) and 13·8 (sd 0·2) years old at follow-up (age 13 years). Less than a quarter of participants were overweight or obese at baseline. About 60 % of boys and girls were consuming SSB at age 10 years. Baseline median SSB consumption was 0·4 (interquartile range 1·4) and 0·3 (interquartile range 1·0) servings/d for boys and girls, respectively. Servings of SSB increased from ages 10 to 13 years (mean 0·12 (sd 1·36) servings/d).
Table 1 Sample characteristics of 2455 children at baseline, stratified by sexFootnote *, Avon Longitudinal Study of Parents and Children (ALSPAC)

IQR, interquartile range; WC, waist circumference; TBFM, total body fat mass; cpm, counts per minute; SSB, sugar-sweetened beverage.
* Data are shown for baseline (age 10 years), unless otherwise noted.
† Overweight/obese was defined using International Obesity Task Force age- and sex-specific weight categories( Reference Cole, Bellizzi and Flegal 37 ).
‡ TBFM was obtained by dual-energy X-ray absorptiometry conducted at age 13 years.
§ Physical activity was measured by uniaxial accelerometer.
|| Sample sizes vary due to missing values as follows: pubertal stage (n 2231), maternal overweight/obesity (n 1880), maternal educational attainment (n 2292) and dieting at age 13 years (n 2135).
¶ 180 g=1 serving of SSB.
** Dietary reporting errors were defined using methods developed by Huang et al.( Reference Huang, Howarth and Lin 40 ) and modified to use accelerometer data( Reference Noel, Mattocks and Emmett 39 ).
Change in SSB consumption was positively associated with higher weight and BMI at age 13 years in models 1 and 2 (standardized β=0·028 to 0·030, P<0·05), while somewhat weaker effect magnitudes were seen for WC and TBFM (β=0·014 to 0·020, P≥0·05; Table 2). After accounting for dietary reporting errors (model 3), the associations between change in SSB and all measures of adiposity were strengthened (β=0·033 to 0·043, P<0·05 for all measures). In the primary model (model 4), we included only those 1059 participants considered to have plausible dietary intakes. The effects of SSB on total and central adiposity increased in magnitude by 53 % to 185 %. For example, among plausible energy reporters standardized estimates for WC increased from β=0·034 to 0·097 as compared with analyses in the full cohort (model 3).
Table 2 Effect of change in SSB intake from ages 10 to 13 years on central and total adiposity at age 13 years (n 2455)Footnote *, Avon Longitudinal Study of Parents and Children (ALSPAC)

SSB, sugar-sweetened beverages; WC, waist circumference; TBFM, total body fat mass.
* Change in SSB, ∆SSB=SSB (servings/d) at age 13 years – SSB (servings/d) at age 10 years. TBFM was obtained by dual-energy X-ray absorptiometry.
† Model 1: ∆SSB (servings/d), SSB at age 10 years (servings/d), sex, and baseline age, height and adiposity. For TBFM models, BMI at age 10 years was used for baseline adiposity adjustment. Model 2: model 1 + covariates (physical activity at age 13 years, pubertal stage at age 13 years, maternal overweight/obesity status, maternal education, dieting at age 13 years, and change in fruit juice, fruit and vegetable, and total fat intakes from ages 10 to 13 years. Model 3: model 2 + dietary reporting errors at age 13 years. Model 4: model 2 among plausible dietary reporters at age 13 years only (n 1059).
In models adjusted for total energy intake, standardized estimates for the effect of change in SSB consumption on adiposity at age 13 years were attenuated by 47 %, 25 % and 22 % for weight, BMI and WC, respectively, compared with models unadjusted for total energy. Estimates for TBFM remained similar after accounting for energy intake (data not shown).
There was no evidence of effect modification by sex (P=0·13 to 0·99) for total and central adiposity models among the full cohort and plausible energy reporters or by baseline SSB consumption (P=0·38 to 0·74) among plausible energy reporters. In the full cohort, baseline SSB intake did not modify the effect of change in SSB consumption on weight, WC and TBFM (P=0·08 to 0·74), but did so for BMI (P=0·03). Due to the lack of effect modification among plausible reporters – our main model – alongside inconsistent findings in the total cohort analyses, in addition to considerations regarding detection of interaction due to chance following multiple testing, we did not stratify analyses by baseline SSB intake.
In simple and multivariable models with and without adjustment for dietary reporting errors, there was no evidence that the relationship between change in SSB intake and WC at 13 years was independent of total adiposity as assessed by BMI and TBFM (Table 3). Conversely, among plausible reporters (model 4), change in SSB intake was positively associated with WC after accounting for BMI (β=0·042, P=0·02) and TBFM (β=0·048, P=0·01), although effects were attenuated by 57 % and 51 %, respectively, compared with similar models unadjusted for total adiposity. Although WC at age 10 years was correlated with BMI (r=0·78) and TBFM (r=0·77) at age 13 years, variance inflation factors for these terms were <3·1 in their respective models, thus supporting the validity of these models (data not shown).
Table 3 Effect of change in SSB intake from ages 10 to 13 years on WC at age 13 years adjusted for total adiposity (n 2455)Footnote *, Avon Longitudinal Study of Parents and Children (ALSPAC)
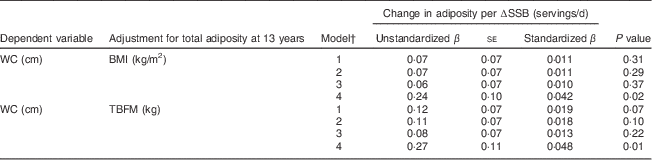
SSB, sugar-sweetened beverages; WC, waist circumference; TBFM, total body fat mass.
* Change in SSB, ∆SSB=SSB (servings/d) at age 13 years – SSB (servings/d) at age 10 years.
† Model 1: ∆SSB (servings/d), SSB at age 10 years (servings/d), sex, BMI or TBFM at age 13 years, and baseline age, height and WC. For TBFM models, BMI at age 10 years was used for baseline adiposity adjustment. Model 2: model 1 + covariates (physical activity at age 13 years, pubertal stage at age 13 years, maternal overweight/obesity status, maternal education, dieting at age 13 years, and change in fruit juice, fruit and vegetable, and total fat intakes from ages 10 to 13 years. Model 3: model 2 +dietary reporting errors at age 13 years. Model 4: model 2 among plausible dietary reporters at age 13 years only (n 1059).
Discussion
In the present study, increased consumption of SSB over 3 years was related to higher central and total adiposity at age 13 years as ascertained by WC and directly measured TBFM, respectively. Moreover, the positive relationship between SSB consumption and WC remained after accounting for total adiposity. To our knowledge, the present study is the first one to demonstrate that SSB intake in older children has unique effects on adipose tissue distribution with a greater preference for central fat accumulation.
Previous studies have examined the relationship between SSB intake and WC in older children, but only one reported standardized estimates as employed in our analysis( Reference Collison, Zaidi and Subhani 43 ). In that large cross-sectional study of Saudi Arabian children aged 10–19 years (n 9433), Collison et al.( Reference Collison, Zaidi and Subhani 43 ) found similar and positive associations between carbonated SSB (servings/week) and BMI and WC (standardized β=0·10, 95 % CI 0·19, 0·39 for BMI and β=0·10, 95 % CI 0·09, 0·17 for WC; P<0·0001) among boys (n 5033); no association was detected among girls (n 4400). Perhaps in part because of our rigorous methods, including use of a prospective study design, unlike the aforementioned study, we found that WC had a stronger association with SSB consumption compared with BMI among plausible dietary reporters. Importantly, no other study has determined whether SSB intake may affect WC independent of changes in total adiposity in older children.
Few prospective studies in older children have related SSB intake to directly measured body fat by DXA( Reference Fiorito, Marini and Francis 15 , Reference Mundt, Baxter-Jones and Whiting 31 ). In one examination of girls, intake at age 5 years was associated with higher body fat at each subsequent visit during 10 years of follow-up( Reference Fiorito, Marini and Francis 15 ). Conversely, Mundt et al.( Reference Mundt, Baxter-Jones and Whiting 31 ) found among 8–15-year-old boys and girls that prospective intake of SSB did not relate to changes in body fat over 7 years. The smaller sample size of these studies (<300) compared with our study of more than 2000 older children may explain the conflicting observations as it increases the chance of type 2 errors. As well, our study, which shows that SSB intake is associated with greater fat mass accumulation in children transitioning into adolescence, is consistent with a recent well-designed randomized controlled trial conducted in overweight and obese adolescents who regularly consume SSB( Reference Ebbeling, Feldman and Chomitz 44 ). In that study, Ebbeling et al.( Reference Ebbeling, Feldman and Chomitz 44 ) found that those assigned to receive non-caloric beverage provisions for 1 year had smaller gains in BMI compared with those assigned to the control group. Interestingly, body fat did not relate to the experimental condition, but it was obtained by bioelectrical impedance (as opposed to DXA as in our study), which has been shown to inaccurately measure body fat in overweight individuals( Reference Sun, French and Martin 45 ).
Novel to our work here is the examination of dietary reporting errors, a key variable in diet–obesity research often overlooked in many epidemiological studies. Errors in dietary assessment may partly explain the null association between SSB intake and BMI previously reported in other prospective studies that did not consider this issue( Reference Laurson, Eisenmann and Moore 29 , Reference Mundt, Baxter-Jones and Whiting 31 ). In particular, children with higher levels of adiposity are more likely to under-report total energy( Reference Noel, Mattocks and Emmett 39 , Reference Huang, Roberts and Howarth 46 , Reference Savage, Mitchell and Smiciklas-Wright 47 ) and this bias can attenuate associations. Together, the extant body of literature on diet and adiposity in children as well as adults underscores the importance of accounting for dietary reporting errors.
Our findings also build upon previous work conducted in ALSPAC( Reference Johnson, Mander and Jones 36 ). In one study, SSB intake at age 5 or 7 years was not associated with TBFM at age 9 years( Reference Johnson, Mander and Jones 36 ). However, the contradictory findings to our study may stem from several methodological differences. Johnson et al.( Reference Johnson, Mander and Jones 36 ) utilized a smaller sample of children (n 521–682) and they did not examine change in SSB intake as we did in our analysis. Alternatively, null findings in that study may also suggest that in this cohort of British children, SSB–body fat associations may be more important in older childhood as compared with early childhood. Although speculative, this may be related to the dramatic rise in SSB consumption that occurs during older childhood and adolescence. This suggests that targeted obesity prevention efforts to reduce SSB intakes during this life stage may be of particular importance.
Several mechanisms may lead to increased weight gain due to SSB intake. There is evidence for reduced dietary compensation when energy is consumed in liquid as opposed to solid form( Reference Mourao, Bressan and Campbell 48 ) and at meals following consumption of caloric beverages( Reference Ranawana and Henry 49 ), resulting in higher absolute energy intakes among those consuming SSB. These beverage products are energy-dense yet nutrient-poor and data from our study, along with those from others, relate their consumption to higher adiposity. In contrast, energy-dense foods that are nutrient-rich, such as dairy, may be protective against excess weight gain( Reference Bigornia, LaValley and Moore 50 , Reference Kratz, Baars and Guyenet 51 ). Moreover, in our study SSB consumption was positively associated with adiposity independent of total energy intake, suggesting mechanisms beyond (or in addition to) increased energy consumption. Sucrose, the primary sweetener of beverages in Europe, is composed of a 1:1 ratio of glucose and fructose. Fructose has been implicated in weight gain( Reference Stanhope 52 ) and may have differential effects on central v. total adiposity( Reference Stanhope, Schwarz and Keim 53 , Reference Maersk, Belza and Stodkilde-Jorgensen 54 ). Stanhope et al.( Reference Stanhope, Schwarz and Keim 53 ) found that overweight and obese adults consuming fructose-sweetened beverages along with their usual diet for a 10-week period gained more intra-abdominal adipose volume compared with the glucose group despite similar changes in total fat mass. In a recent study, overweight individuals randomized to drink sucrose-sweetened soda over 6 months had significant increases in intra-abdominal fat, but not total fat mass, relative to those in the isoenergetic milk condition( Reference Maersk, Belza and Stodkilde-Jorgensen 54 ). In contrast, among healthy adults (BMI=20–35kg/m2) participating in a 4-week weight maintenance feeding study of a diet supplemented with fructose or glucose 150 g/d (approximately 21 % of daily energy expenditure), Silbernagel et al.( Reference Silbernagel, Machann and Unmuth 55 ) found no significant differences in changes in weight (kg), total body fat (kg) and visceral fat (kg) between diets. Additional research is needed to establish a definitive role of fructose in central fat accumulation( Reference Bray and Popkin 56 ).
Our study has several notable strengths. The large sample size provided adequate power to detect modest dietary effects and the longitudinal design minimized chances of reverse causation. We adjusted for dietary reporting errors, which can mask diet–adiposity associations( Reference Huang, Howarth and Lin 40 ), using a rigorous method employing objectively measured physical activity( Reference Noel, Mattocks and Emmett 39 ). Our use of standardized estimates allowed for direct comparison of SSB effects on adiposity between WC, BMI and TBFM. Importantly, WC models were adjusted for measures of total fat to determine the unique effect of SSB on central adiposity.
A limitation of the study is that baseline diet was not measured concurrent with the DXA scans (i.e. diet at age 10 years and DXA at age 11 years). However, correlations between TBFM at 11 years, BMI at 10 years and BMI at 11 years were strong (≥0·90), indicating that body fat differences at age 10 years were adequately accounted for by use of BMI at age 10 years. Residual confounding is a potential concern in part due to the multifactorial aetiology of weight gain, difficulty in measuring diet and the observational nature of our study. Although we adjusted for a number of potential confounders, some were not available for analysis. Specifically, out-of-home eating has been positively associated with obesity( Reference Nago, Lachat and Dossa 57 ) and SSB intake( Reference Park, Blanck and Sherry 58 ), but constraints of the food coding software precluded derivation of this variable. As well, complete data for all potential confounders were not available for the full cohort (n 2455). To preserve the sample size we dummy coded for missing data, which can also contribute to residual confounding and underestimation of some of our results. Some caution is necessary in interpreting our findings. The magnitude of the association between SSB intake and WC was reduced by 50 % after accounting for variation in BMI or TBFM. Even so, it is unclear whether these small independent changes in WC associated with SSB are clinically relevant. For instance, our data indicate that an increase in SSB consumption of one 180 g serving/d over 3 years could result in a 0·24cm higher WC at 13 years of age. However, median WC measures among normal weight (n 1972), overweight (n 90) and obese (n 393) adolescents at age 13 years were 69, 82 and 95 cm respectively. Thus, further research employing our methods – i.e. adjusting both for total adiposity in models of central adiposity as well as dietary reporting errors – is needed to reproduce this finding.
Conclusion
In summary, prospective studies examining the relationship between SSB consumption and central adiposity in older children, who are large consumers of SSB, are lacking and limited. In the present study, increase in SSB intake over 3 years was associated with higher WC at age 13 years after accounting for total adiposity. We also provide evidence that SSB consumption in children influences total fat mass accumulation as determined by DXA. Our findings add further support to recommendations( 59 ) to curtail intakes of SSB as a means to combat excess weight gain in children and suggest that they have a modest additional effect on central adiposity.
Acknowledgements
Acknowledgements: The authors would like to thank the families who participated in ALSPAC, the midwives for their help in recruiting participants and the ALSPAC team, which includes interviewers, computer and laboratory technicians, clerical workers, research scientists, volunteers, managers, receptionists and nurses. Core support for ALSPAC comes from the UK Medical Research Council (grant ref. 74882), the Welcome Trust (grant ref. 076467) and the University of Bristol. A grant from the American Diabetes Association awarded to P.K.N. funded the present study (grant ref. 708JF41). The funders had no role in the design, analysis or writing of this article. Conflict of interest: None. Authorship: The research project was designed by P.K.N. and S.J.B.; A.R.N. was responsible for data acquisition; S.J.B. analysed the data with statistical support from M.P.L.; P.K.N., S.J.B., M.P.L., S.E.N., L.L.M. and A.R.N. wrote the manuscript; and P.K.N. and S.J.B. had primary responsibility for the final content. All authors read and approved the final manuscript. Ethics of human subject participation: The study was approved by the ALSPAC Law and Ethics Committee, Local Research Ethics Committees and the Institutional Review Board of Boston University Medical Center.





