Disability is defined as difficulty performing activities in an independent fashion due to physical and/or cognitive impairment( Reference Verbrugge and Jette 1 ). Disability generally affects older individuals due to the accumulation of chronic diseases; it has a negative effect on quality of life, is a predictor of hospitalization, institutionalization and death, and increases the burden placed on social and health-care systems( Reference Li 2 , Reference Andrade, Guevara and Lebrão 3 ).
Instrumental activities of daily living (IADL) have been widely studied in recent years, as such activities help maintain individuals in the social and cultural realms of life. The loss of function in IADL can lead to a loss of autonomy (especially with regard to household management), confinement and social isolation. Studies have shown that functional impairment occurs in a hierarchical manner, beginning with IADL and culminating in impaired performance of basic activities of daily living which are related to personal care( Reference Verbrugge and Jette 1 ).
Changes in one's nutritional status contribute toward an increase in illness and mortality rates. Excess weight and obesity have been associated with a number of co-morbidities in all phases of life, especially chronic, non-transmittable conditions( Reference Bray 4 , Reference Zamboni, Mazzali and Zoico 5 ). In recent years, studies have demonstrated that obesity is associated with limitations regarding the performance of IADL, independently of the presence of disease( Reference Jensen and Friedmann 6 , Reference Lang, Llewellyn and Alexander 7 ). Underweight has also been described as a risk factor for disability due to its strong association with sarcopenia( Reference Willett 8 , Reference Lang, Streeper and Cawthon 9 ).
However, the literature reports divergent finings regarding the association between nutritional status and disability. In some studies, underweight and obesity were not found to be independent risk factors of disability( Reference Imai, Gregg and Chen 10 , Reference Larrieu, Pérès and Letenneur 11 ). Moreover, this association has not yet been explored in developing countries, in which the process of epidemiological and nutritional transition is ongoing and the coexistence of increasing obesity and a still high proportion of underweight has a considerable impact on health-care services.
The aim of the present study was to examine the association between nutritional status and the incidence of disability regarding the performance of IADL among older adults in the city of São Paulo (Brazil) over a 6-year period.
Methods
Sample and procedures
The data originated from the SABE (Saúde, Bem-Estar e Envelhecimento; Health, Wellbeing and Ageing) Study, which is a longitudinal study that began in 2000 involving a probabilistic sample of older adults (aged ≥60 years) residing in the city of São Paulo (n 2143). The baseline sample was obtained with a two-stage stratified sampling method, following the framework of the 1995 National Household Survey based on geographic areas of the city. Individuals aged ≥75 years were oversampled to compensate for the greater mortality rate in this age group( Reference Andrade, Guevara and Lebrão 3 ). A second wave of the study was carried out in 2006, in which 1115 of the participants from the first wave were interviewed again. Details on the methodology of the study are described elsewhere( Reference Andrade, Guevara and Lebrão 3 , Reference Lebrão and Laurenti 12 ).
The data in the first wave of the study were collected in two stages. The first stage was a household interview conducted by a single interviewer using a standardized questionnaire addressing the living conditions and health status of the older adult. The second stage was a household visit by a pair of interviewers for the measurement of anthropometric data and the determination of physical performance( Reference Andrade, Guevara and Lebrão 3 ).
Among the 2143 individuals initially interviewed, 1034 reported no difficulties in performing IADL. However, losses to follow-up occurred (114 individuals had moved to other cities or were not located, 190 had died, four had been institutionalized and 115 individuals refused to participate in the second wave). Thus, 611 individuals were eligible to be followed up.
The study was conducted in compliance with the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects/patients were approved by a human research ethics committee. The first wave of the SABE Study was approved by the National Research Ethics (CONEP), and the second wave was approved by the Research Ethics Committee (COEP) of the Faculty of Public Health, University of São Paulo. Written informed consent was obtained from all participants.
Measures
Disability was the dependent variable and was recorded when the participant reported difficulty on one or more IADL in 2006 for which no difficulty was reported in 2000 (baseline). The following activities were analysed: managing finances, use of transportation within the community, shopping, ability to use the telephone and responsibility for one's own medications. All of the other independent variables and parameters included in the analysis were baseline measures.
BMI was calculated by dividing body mass (in kilograms) by the square of height (in metres; kg/m2). Nutritional status was classified based on BMI cut-off points adopted by the Pan American Health Organization for the SABE Study( 13 ): ≤23·0 kg/m2 = underweight; >23·0 and <28·0 kg/m2 =normal range (reference); ≥28·0 and <30·0 kg/m2 = overweight; and ≥30·0 kg/m2 =obesity.
The following sociodemographic characteristics were included in the analysis: gender; age (grouped into two categories: 60–74 years and ≥75 years); household arrangement (living alone or accompanied); income perceived as adequate for expenses; and schooling (in years of formal education).
Health status was assessed based on self-reported diabetes, hypertension, CVD, osteoarthritis, chronic respiratory disease, stroke, osteoporosis, and reported falls and hospitalization in the 12 months preceding the interview.
Cognitive status was evaluated using the modified version of the Mini Mental State Examination (MMSE)( Reference Folstein, Folstein and McHugh 14 ) validated for the SABE Study, due to the low level of schooling of the South American elderly population. This measure has thirteen items that are less dependent upon schooling and the cut-off point is a score of 12 or less( Reference Icaza and Albala 15 ). The Brazilian version of the Geriatric Depression Scale was used to assess depressive symptoms, with a score of 6 or more as the cut-off point( Reference Sheikh and Yesavage 16 , Reference Paradela, Lourenço and Veras 17 ).
Statistical analysis
For the descriptive analysis, means and their standard errors were calculated for the continuous variables and proportions were calculated for the categorical variables. Differences between groups were estimated using the Wald test of mean equality and the Rao–Scott test, which considers sample weights for estimates with population weights( Reference Rao and Scott 18 ).
Forward stepwise logistic regression analysis was performed for the assessment of factors associated with the development of disability in the period studied and the dependent variable was positive answer of difficulty in at least one IADL in 2006. Variables that remained significant (P < 0·05) or that adjusted the odds ratio by at least 10 % were maintained in the model. The inferences considered the design effect. The data analysis was performed using the statistical software package Stata® version 11.
Results
Among the older adults who were independent with regard to IADL in 2000, 611 were interviewed again in 2006. In the comparative analysis between those who were re-interviewed and those lost to follow-up, significant differences were found regarding osteoarthritis and osteoporosis, with higher baseline prevalences in the group lost to follow-up: 35·0 % v. 20·3 % for osteoarthritis (P < 0·001) and 18·3 % v. 12·9 % for osteoporosis (P = 0·031). No statistically significant differences were found for the other variables analysed (data not shown).
Table 1 displays the baseline characteristics of the participants at the beginning of the study (total sample) and according to functional status at follow-up. At baseline, most of the individuals were between 60 and 74 years of age, had an average of 7·8 years of schooling and a score of 17 on the MMSE. Obesity was identified in ∼20 % and 73·1 % reported at least one chronic disease.
Table 1 Sample characteristics at baseline and after follow-up period according to outcome regarding IADL; SABE Study, city of São Paulo, Brazil, 2000 and 2006
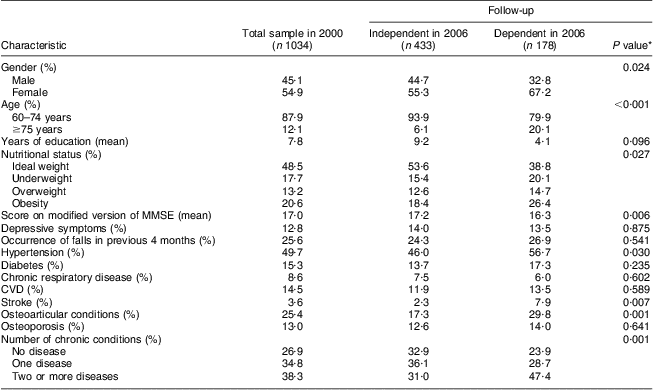
IADL, instrumental activities of daily living; SABE, Saúde, Bem-Estar e Envelhecimento (Health, Wellbeing and Ageing); MMSE, Mini Mental State Examination.
*Rao–Scott and Wald tests were used.
Among the 611 individuals re-evaluated in 2006, 178 reported difficulty on at least one IADL. Those with incident disability differed from those who did not develop disability with regard to some baseline characteristics (Table 1). The incidence of difficulty regarding IADL was greater among women, individuals aged 75 years or older, those with a lower MMSE score, those with reported hypertension, history of stroke or joint disease and those with a greater number of chronic illnesses. With regard to nutritional status, a greater proportion of either underweight or obesity at baseline was found among those individuals who developed difficulties regarding IADL in comparison to those who did not develop disability.
Table 2 displays the results of the logistic regression analysis for the incidence of disability regarding IADL. Both underweight and obesity were associated with risk of disability in the unadjusted analysis. After controlling for age, MMSE score, report of history of stroke or joint disease and number of reported chronic diseases, both conditions remained independent risk factors for developing functional disability.
Table 2 Results of the logistic regression model for incidence of disability on IADL in a 6-year period among non-disabled participants at baseline; SABE Study, city of São Paulo, Brazil, 2000 and 2006
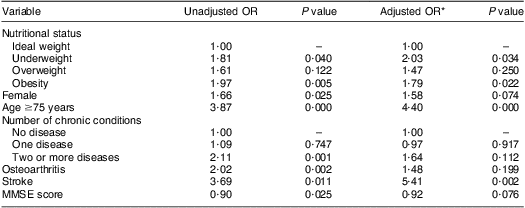
IADL, instrumental activities of daily living; SABE, Saúde, Bem-Estar e Envelhecimento (Health, Wellbeing and Ageing); MMSE, Mini Mental State Examination, modified.
*Hosmer–Lemeshow goodness-of-fit test (P = 0·468).
Discussion
The results of the present cohort study demonstrate that both underweight and obesity are independent risk factors for functional disability. Underweight was associated with a 100 % greater risk of disability in comparison to the ideal weight range (OR = 2·03; P = 0·034). This finding may be explained by the loss of muscle mass (sarcopenia), which is known to compromise functionality( Reference Lang, Streeper and Cawthon 9 ). Underweight is a multifactor condition among elderly individuals, but has two main causes. The first is inadequate nutrient intake due to factors such as anorexia, oral and dental problems, dysphagia and altered sense of smell and taste, leading to weight loss and, if prolonged, malnutrition. Catabolic diseases or associated conditions, such as lung disease, cancer and frailty, constitute the other major cause of underweight( Reference Hickson 19 – Reference Visvanathan and Chapman 21 ). Both mechanisms are associated with sarcopenia.
It was not possible to include the adequacy of food intake in the analyses of the present study, as data on food consumption were not addressed on the questionnaires. The same is true regarding frailty and sarcopenia. The other catabolic diseases were not associated with disability in the unadjusted analyses. Although this is suggestive of a relatively greater survival rate (individuals with catabolic diseases and weight loss are believed to have a greater mortality rate), the analysis did not reveal statistically significant differences in these diseases between those re-interviewed and those lost to follow-up or among the deaths having occurred in the sample (data not shown).
Previous studies have also reported underweight to be an independent risk factor for disability, such as a study carried out in the USA( Reference Imai, Gregg and Chen 10 ) which found an association between underweight (BMI ≤ 18·5 kg/m2) and disability; the same association was also found in a study carried out in Canada( Reference Gadalla 22 ). In a study conducted in France, in which a BMI between 23·0 and 27·0 kg/m2 was considered to be the reference category, an effect was found only for elderly individuals with a BMI of <21·0 kg/m2, whereas those with a BMI between 21·0 and 23·0 kg/m2 were not at increased risk( Reference Larrieu, Pérès and Letenneur 11 ).
In the present study, the risk of disability was very high among individuals with obesity (79 % higher in comparison to those within the ideal weight range, after controlling for other variables: OR = 1·79; P = 0·022). This association is less controversial in the literature. It seems to be well established that obesity is associated with a greater incidence of disability in different domains, including the execution of IADL, as reported in a review carried out by Zamboni et al.( Reference Zamboni, Mazzali and Zoico 5 ). In other previously cited studies, obesity was also found to be a risk factor for disability( Reference Larrieu, Pérès and Letenneur 11 , Reference Gadalla 22 ). In the American study, however, class I obesity (BMI between 30·0 and 35·0 kg/m2) proved to be a protection factor against disability in men( Reference Imai, Gregg and Chen 10 ). Unlike obesity, overweight appears to play a protective role against diseases and complications among elderly individuals( Reference Imai, Gregg and Chen 10 ). Other studies have not found a significant association between overweight and disability( Reference Gadalla 22 ). Only the study carried out in France found overweight to be a risk factor for disability regarding IADL – and only among men( Reference Larrieu, Pérès and Letenneur 11 ). In the present study, overweight was not significantly associated with the incidence of disability.
The analysis of nutritional status was controlled for previously known risk factors of disability. Among the variables that remained in the multivariate model, high odds ratios were found for individuals aged 75 years or older and those who reported a history of stroke – both of which are recognized risk factors for functional disability( Reference Kaplan, Haan and Wallace 23 , Reference Fried, Bandeen-Roche and Kasper 24 ). Osteoarthritis, number of chronic conditions and gender did not achieve statistical significance in the final model, but were maintained due to the fact that these variables adjust the estimates and are commonly reported risk factors in the literature( Reference Fried, Bandeen-Roche and Kasper 24 , Reference Stuck, Walthert and Nikolaus 25 ).
The findings presented herein contribute to the understanding of the association between nutritional status among elderly individuals and an impaired ability to live an independent life in the community, as measured by difficulties regarding the performance of IADL, especially in developing countries, which are going through a later but faster process of epidemiological and nutritional transition, with a considerable impact on health-care services. In Brazil, the accelerated growth in the prevalence of obesity and the reduction in malnutrition have been following the same patterns as those described for Americans( Reference Popkin 26 ). In this context, older adults merit special attention due to the increase in the prevalence of obesity, which can contribute towards an increase in illness and disability in this age group, along with the problem of malnutrition at more advanced ages( Reference Myers, Lamb and Agree 27 ), as mentioned above. However, like other developing countries, Brazil does not have a sufficiently organized health-care structure or policies to cope with this rapid process of epidemiological and nutritional transition.
The present study has limitations that should be addressed. Disability was measured using self-reported information. While this may be a source of bias, methodological studies have demonstrated that self-reported data on functional disability have adequate validity and are consistent with medical diagnoses and/or physical tests( Reference Reuben, Siu and Kimpau 28 ). Another limitation is the high proportion of losses, but the analysis demonstrated no statistically significant differences in the baseline characteristics of the individuals interviewed a second time and those lost to follow-up, with the exception of the prevalence of osteoarthritis and osteoporosis. However, this difference tends to underestimate measures of the association of joint disease as a risk factor of disability, as a lower prevalence rate was found among the individuals evaluated a second time in comparison to those lost to follow-up.
Conclusions
Based on the findings of the present study, obesity and underweight are independent risk factors of impairments regarding an autonomous life in the community, as measured by the development of difficulties in the performance of IADL. These findings corroborate data found in the literature and help clarify the role of underweight in the incidence of disability. The understanding of the influence of nutritional status on this process allows the establishment of preventive strategies aimed at the elderly population, contributing to the reformulation of health-care policies and the organization of health services with the aim of diminishing the incidence of disability and favouring quality of life among this portion of the population.
Acknowledgements
Sources of funding: This study was funded by São Paulo Research Foundation (Fundação de Amparo à Pesquisa do Estado de São Paulo – FAPESP). Conflicts of interest: The authors have no conflicts of interests. Authors’ contributions: Study conception and design: L.P.C.; analysis and/or interpretation of data, drafting of the manuscript: L.P.C., D.P.N., T.R.P.d.B. and T.d.S.A.; revision of the manuscript and approval of the final version of the manuscript: J.L.F.S., Y.A.d.O.D. and M.L.L.; main study (SABE) coordinators: J.L.F.S., Y.A.d.O.D. and M.L.L.




