Introduction
There is a growing realization that the careful elucidation and measurement of intermediate biological characteristics is central to refining and improving existing psychiatric classification and treatment. As highlighted in the NIMH Research Domain Criteria (RDoC) strategic plan, it is necessary to identify intermediate markers, cutting across related psychiatric disorders, and continuous with relevant markers of variability in the general population (Cuthbert & Insel, Reference Cuthbert and Insel2013). The concepts of impulsivity and compulsivity are highly relevant clinically, but also represent fruitful heuristics in the search for intermediate markers of psychiatric disease. Impulsivity refers to behaviors or actions that are inappropriate, premature, unduly thought out, risky, and that lead to untoward outcomes (Evenden, Reference Evenden1999). Compulsivity refers to a tendency toward repetitive, habitual actions, repeated despite adverse consequences (Robbins et al. Reference Robbins, Gillan, Smith, de Wit and Ersche2012). It has been suggested that impulsivity and compulsivity might constitute opposite ends of a spectrum (Stein et al. Reference Stein, Hollander and Liebowitz1993). However, impulsive and compulsive symptoms can co-occur within the same individual, hence the suggestion that they may be driven by common neurobiological processes (such as lack of top–down executive control, or ‘disinhibition’) (Chamberlain et al. Reference Chamberlain, Blackwell, Fineberg, Robbins and Sahakian2005). Impulsivity–compulsivity constitutes one of several candidate dimensional models in psychiatry. Other key examples include internalizing (depression, generalized anxiety) v. externalizing (e.g. substance use, antisocial personality) symptoms (Khan et al. Reference Khan, Jacobson, Gardner, Prescott and Kendler2005); and depression v. mania (the ‘mood spectrum’) (McElroy et al. Reference McElroy, Pope, Keck, Hudson, Phillips and Strakowski1996). These different frames of references can be viewed as being partly related.
At the level of symptoms, impulsive behaviors are explicitly listed in the diagnostic criteria for attention-deficit hyperactivity disorder (ADHD), and several other conditions formally listed as ‘Impulse Control Disorders’ in the Diagnostic and Statistical Manual Version 5 (DSM-5) (American Psychiatric Association, 2013). Symptoms reaching formal diagnostic criteria for ADHD are evident in up to 7% of children and 2.5% of adults (Simon et al. Reference Simon, Czobor, Balint, Meszaros and Bitter2009). Compulsivity is well represented in obsessive–compulsive disorder (OCD; intrusive thoughts and/or repetitive rituals) and in obsessive–compulsive personality disorder (OCPD; e.g. rigid, perfectionistic approach to life with reluctance to delegate) (American Psychiatric Association, 2013). Formal OCD affects 1–3% of the population, and OCPD up to 8% (Grant et al. Reference Grant, Chamberlain and Odlaug2014; Diedrich & Voderholzer, Reference Diedrich and Voderholzer2015). Obsessive–compulsive traits exist in milder forms and can be quantified using questionnaires designed for this purpose (Sanavio, Reference Sanavio1988). Compulsivity is also a core behavioral feature in gambling disorder or substance use disorders – conditions now listed together in the DSM-5 category of ‘Substance Related and Addictive Disorders’. These disorders are also common (prevalence of 8.5% for alcohol use disorder and up to 3.1% for gambling disorder) (Grant et al. Reference Grant, Dawson, Stinson, Chou, Dufour and Pickering2004a ; Ferguson et al. Reference Ferguson, Coulson and Barnett2011).
Impulsivity and compulsivity can be conceptualized not only in terms of overt psychopathology, such as described above, but also in terms of personality- and laboratory-based neurocognitive measures. There is an extensive literature on the development and validation of questionnaire-based measures of personality related to impulsivity (e.g. the Barratt Impulsiveness Questionnaire), and compulsivity (e.g. the Padua Obsessive–Compulsive Inventory) (Barratt, Reference Barratt1965; Sanavio, Reference Sanavio1988). These measures are well suited for use at the level of the general population, but are also sensitive to more extreme levels of impulsivity and compulsivity as manifested in ADHD and OCD, respectively (Malloy-Diniz et al. Reference Malloy-Diniz, Fuentes, Leite, Correa and Bechara2007; van den Heuvel et al. Reference van den Heuvel, Remijnse, Mataix-Cols, Vrenken, Groenewegen, Uylings, van Balkom and Veltman2008). From a cognitive perspective, facets of impulsivity can be captured using tests of premature motor response (stop-signal tasks), and gambling paradigms examining tendency for making risky decisions (Grant & Chamberlain, Reference Grant and Chamberlain2014). Similarly, aspects of compulsivity can be fractionated using tests of flexible responding, especially set-shifting (Robbins et al. Reference Robbins, Gillan, Smith, de Wit and Ersche2012), and measures of rigidity on other tests. Inroads have been made in eliciting the neural and neurochemical substrates underlying normal performance on these tasks across species (Robbins, Reference Robbins2005; Dalley et al. Reference Dalley, Everitt and Robbins2011; Bari & Robbins, Reference Bari and Robbins2013; Fineberg et al. Reference Fineberg, Chamberlain, Goudriaan, Stein, Vanderschuren, Gillan, Shekar, Gorwood, Voon, Morein-Zamir, Denys, Sahakian, Moeller, Robbins and Potenza2014). Dysfunction of these fronto-striatal systems is central to neurobiological models and treatment of impulsive and compulsive conditions (Denys et al. Reference Denys, Zohar and Westenberg2004; Biederman & Faraone, Reference Biederman and Faraone2005; Del Campo et al. Reference Del Campo, Chamberlain, Sahakian and Robbins2011; Seixas et al. Reference Seixas, Weiss and Muller2012).
The concepts of impulsivity and compulsivity have contributed to the latest nosological classification systems in psychiatry, and are critical concepts when considering treatments for mental disorders. Yet, it is not yet known whether latent phenotypes of impulsivity and compulsivity exist; if so, whether they are related; and if so, how. Therefore, we quantified whether impulsive and compulsive data were optimally explained by there being one underlying latent factor, two underlying unrelated latent factors, or two underlying related latent factors. It was hypothesized that impulsive and compulsive variables would load onto two largely separable, but positively correlated latent traits.
Materials and methods
Participants
Participants, aged 18–29 years, were recruited using media advertisements in two US cities. Adverts asked subjects to participate in a research study exploring impulsive/compulsive behaviors. Subjects were excluded if they were unable to give informed consent, were unable understand/undertake the study procedures, or were seeking treatment for any mental disorders. All study procedures were carried out in accordance with the Declaration of Helsinki. The Institutional Review Boards of the Universities of Minnesota and Chicago approved the study and the consent statement. Participants were compensated with a $50 gift card for a local department store for taking part.
Clinical assessments
Assessments were conducted in a quiet testing room with a trained rater, and included objective clinical interview, completion of questionnaires, and neuropsychological assessment using a touch-screen computer. An overview of the measures is provided in Table 1 below. We focused on measures of impulsivity and compulsivity, categorized as such a priori on the basis of current psychiatric models and nosology.
Table 1. Overview of outcome measures collected as part of the study
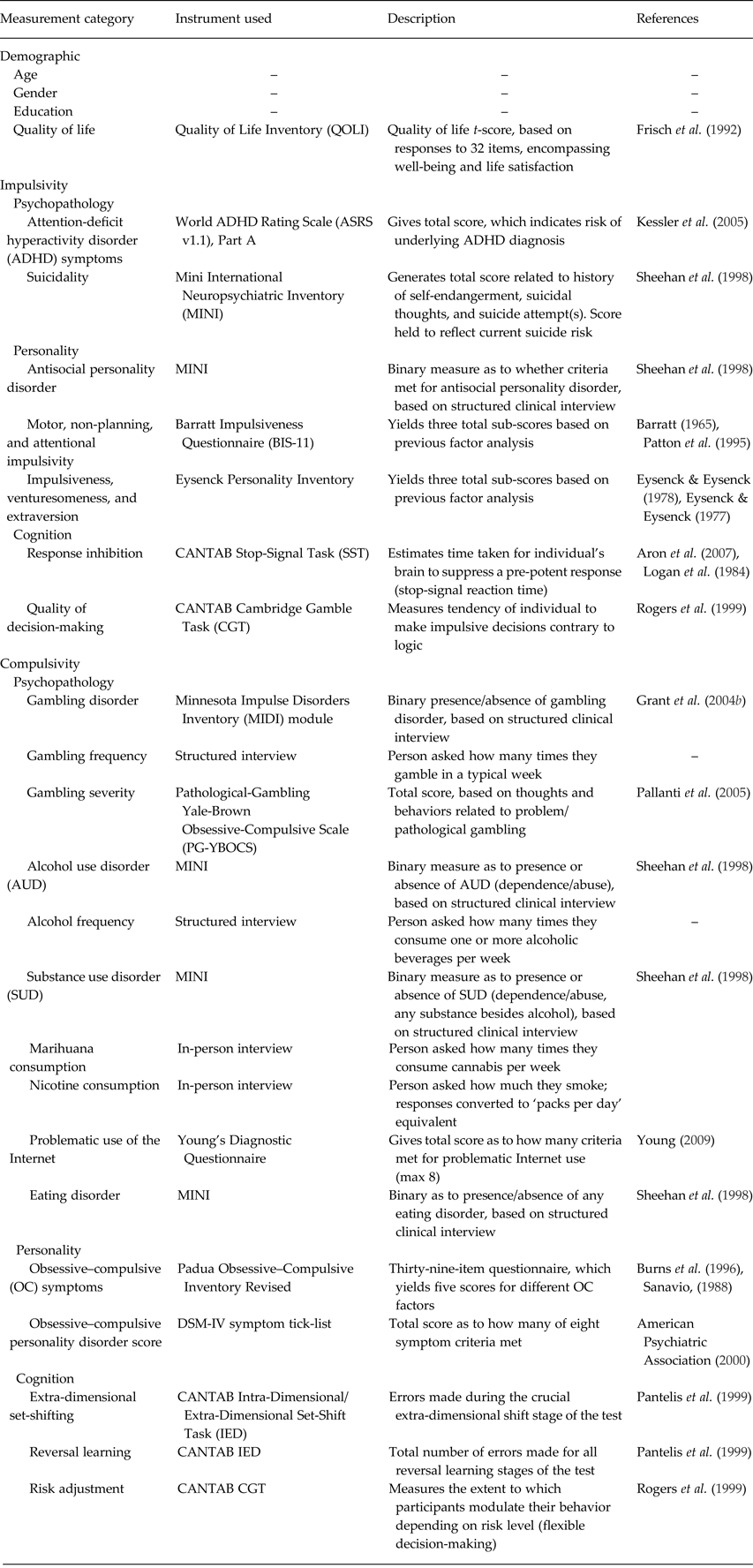
Psychopathological measures of impulsivity comprised ADHD symptom scores, occurrence of antisocial personality disorder (ASPD), and suicidal tendencies. Impulsive symptoms are listed explicitly in the diagnostic criteria for ADHD and ASPD, whereas many studies have reported strong – even heritable – associations between impulsivity and suicide-related behaviors (Chistiakov et al. Reference Chistiakov, Kekelidze and Chekhonin2012). For personality-related measures of impulsivity, we included the Barratt Impulsivity and Eysenck personality questionnaires, which are widely used and accepted for such purposes (Gomez & Corr, Reference Gomez and Corr2014; Stanford et al. Reference Stanford, Mathias, Dougherty, Lake, Anderson and Patton2016). For cognitive measures of impulsivity, we focused on the inhibition of pre-potent motor responses on the Stop-Signal Test (SST), and the tendency to make irrational decisions to the detriment of longer term performance on the Cambridge Gamble Test (CGT). Decisional and motor impulsivity are widely recognized as distinct cognitive manifestations of impulsivity (Dalley et al. Reference Dalley, Everitt and Robbins2011; MacKillop et al. Reference MacKillop, Weafer, C Gray, Oshri, Palmer and de Wit2016). See online Supplementary file for more detailed description of the cognitive tasks.
Compulsive measures of psychopathology included those reflecting gambling, substance use, compulsive use of the Internet, and eating disorders. Compulsivity is central to understanding the neurobiology of gambling and substance use disorders, in that they are characterized by maladaptive repetitive engagement in habitual behaviors that are reinforcing (implicating dysfunctional reward circuitry) (Grant & Chamberlain, Reference Grant and Chamberlain2016). Symptoms of dependence and withdrawal are extremely common in substance and gambling disorders, serving to perpetuate narrowing of the behavioral repertoire (Wareham & Potenza, Reference Wareham and Potenza2010). While not yet regarded as a formal psychiatric disorder, problematic Internet use is relatively commonplace. Its working diagnostic criteria incorporate compulsive use (based on parallels with substance use disorders) (Young, Reference Young2009). Based on an extensive review of available literature, compulsive use has been highlighted as a core symptom of Internet addiction (Kuss et al. Reference Kuss, Griffiths, Karila and Billieux2014). Compulsivity has emerged as a key construct in understanding eating disorders – pathological overeating (Degortes et al. Reference Degortes, Zanetti, Tenconi, Santonastaso and Favaro2014; Moore et al. Reference Moore, Sabino, Koob and Cottone2017), as well as in anorexia nervosa (Tenconi et al. Reference Tenconi, Santonastaso, Degortes, Bosello, Titton, Mapelli and Favaro2010; Degortes et al. Reference Degortes, Zanetti, Tenconi, Santonastaso and Favaro2014; Treasure et al. Reference Treasure, Cardi, Leppanen and Turton2015). For compulsive personality, obsessive–compulsive symptom traits on the Padua Inventory revised (Burns et al. Reference Burns, Keortge, Formea and Sternberger1996; Sanavio, Reference Sanavio1988), and OCPD traits (based on number of DSM criteria met), were quantified. We used Padua Inventory rather than the OCD Yale-Brown Obsessive Compulsive Disorder Scale (YBOCS) because the Padua Inventory is designed to explore obsessive–compulsive traits and symptoms at the population level; using the YBOCS in a normative population would likely have yielded very limited variation in scores, with most participants scoring zero. For compulsive cognition, we measured reversal learning and extra-dimensional set-shifting on the Intra-Dimensional/Extra-Dimensional Set-Shift Task (IED); along with risk adjustment on the Cambridge Gamble Task (CGT). Reversal learning and extra-dimensional set-shifting are two key, separable components of behavioral flexibility germane to understanding compulsivity (Clarke et al. Reference Clarke, Walker, Crofts, Dalley, Robbins and Roberts2005; Clarke et al. Reference Clarke, Walker, Dalley, Robbins and Roberts2007; Chamberlain & Menzies, Reference Chamberlain and Menzies2009; Dalley et al. Reference Dalley, Everitt and Robbins2011). It was hypothesized that difficulty adjusting behavior as a function of risk on the CGT would constitute a measure of decision-making sensitive to rigid response styles. See online Supplementary file for more detailed description of the cognitive tasks.
Data analysis
All statistical analyses were undertaken using R software, MPlus, and IBM SPSS (v22.0) (Muthén & Muthén, Reference Muthén and Muthén2016; R Core Team, 2016).
Impulsive and compulsive measures of interest were analyzed using confirmatory factor analysis (CFA) to compare three models: one in which impulsive and compulsive measures were underpinned by a single underlying latent factor; one in which covariances among impulsive and compulsive measures were explained by two underlying unrelated latent factors; and one in which covariances were explained by two underlying related latent factors. Our aim was to test the relationship between these latent factors, rather than to explore the possible existence of other additional latent factors. As such, and in view of the extensive literature supporting the existence of these two latent types of measurement (impulsivity and compulsivity) (Robbins et al. Reference Robbins, Gillan, Smith, de Wit and Ersche2012; Guo et al. Reference Guo, Youssef, Dawson, Parkes, Oostermeijer, Lopez-Sola, Lorenzetti, Greenwood, Fontenelle and Yucel2017), CFA rather than exploratory factor analysis was appropriate. We included behavioral, personality, and cognitive measures on the same conceptual plane to maintain simplicity of the examined models but also because the distinction between these categories of measure is far from clear. DSM-5 places personality disorders and disorders formally regarded as being on ‘axis-I’ on the same conceptual plane, in recognition of overlap between them. Many measures can be argued to be in one category or another depending on vantage point. To assure comparability, the model fit was evaluated using Akaike Information Criterion (AIC) and Bayesian Information Criterion (BIC) (Akaike, Reference Akaike1974; Schwarz, Reference Schwarz1978).
Results
The sample comprised 576 individuals [mean age (s.d.) = 22.3 (3.6) years; 65.5% male]. The average quality of life, Barratt impulsiveness scores, Padua obsessive–compulsive scores, and cognitive scores were similar to those reported in previous normative datasets (for further discussion and distribution of individual measures see online Supplementary file). Correlations between individual measures of interest are summarized in Fig. 1.

Fig. 1. Heat map showing correlations between variables of interest. Left: positive correlations are shown in blue, and negative in red; larger dots are indicative of stronger correlations. Right: correlation coefficients (rounded to one decimal place in the interests of clarity). gamfreq, gambling frequency per week; alcfreq, alcohol frequency per week; marfreq, marihuana frequency per week; AUD, alcohol use disorder; SUD, substance use disorder; EIQI, Eysenck Inventory Impulsiveness; EIQV, Eysenck Inventory Venturesomeness; EIQE, Eysenck Inventory Extraversion; BISAI, Barratt Attentional Impulsiveness; BISMI, Barratt Motor Impulsiveness; BISNI, Barratt Non-Planning Impulsiveness; antisoc, antisocial personality disorder; suic, suicidality on the Mini International Neuropsychiatric Inventory; PADUACW, Padua Inventory Contamination and Washing subscale; PADUADG, Padua Inventory Dressing/Grooming subscale; PADUAC, Padua Inventory Checking subscale; PADUAT, Padua Inventory Thoughts of Harm to Self-others subscale; PADUAI, Padua Inventory Impulses to Harm Self/Others subscale; nOCPD, number of obsessive-compulsive personality disorder criteria met; ADHD, total score on attention-deficit hyperactivity disorder screen; Internet, total score on Young's Internet Addiction Test; MIDIPG, gambling disorder; SSRT, stop-signal reaction time on Stop-Signal Test; qualdec, quality of decision-making on the Cambridge Gamble Test; riskadj, risk adjustment on the Cambrige Gamble Test; eat_dis, eating disorder; pgybocs, Pathological Gambling Yale Brown Obsessive–Compulsive Disorder Scale; ederr, extra-dimensional errors on the set-shifting task.
Confirmatory factor analysis
Fit indices for the different confirmatory factor models are summarized in Table 2; it can be seen that the model with two correlated latent factors had the best fit (lowest information criteria scores). This model was re-estimated using weighted least squares to assess its absolute fit, which yielded parameters as follows: global fit index 0.977, root mean square error of approximation 0.064, and comparative fit index 0.86. These values are considered to indicate reasonably good fit, in view of conventional criteria, taking into consideration the sample size (Hu & Bentler, Reference Hu and Bentler2009). Comparing the hypothesized models using weight of evidence, the two-factor correlated model was the best fit (>99.9% probability).
Table 2. Maximum likelihood-based fit indices
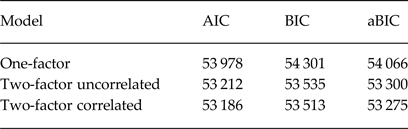
Lower scores indicate better model fit, and a reduction of 10 or more units from one model to another is generally held to indicate a superior model (Raftery, Reference Raftery1995).
The loadings of manifest measures onto the optimal two-factor model are shown in Fig. 2. Variable loadings were in the expected direction, such that higher impulsivity factor scores were associated with higher personality measures of impulsivity, higher impulsive symptomatology (ASPD, ADHD, suicidality), and worse quality of decision-making on the gambling task; and higher compulsivity factor scores were associated with higher personality measures of compulsivity (Padua Inventory), higher compulsive symptomatology (gambling, problematic Internet use, OCPD, substance use disorders), more extra-dimensional set-shifting errors on the set-shifting task, and less risk adjustment on the gambling task.
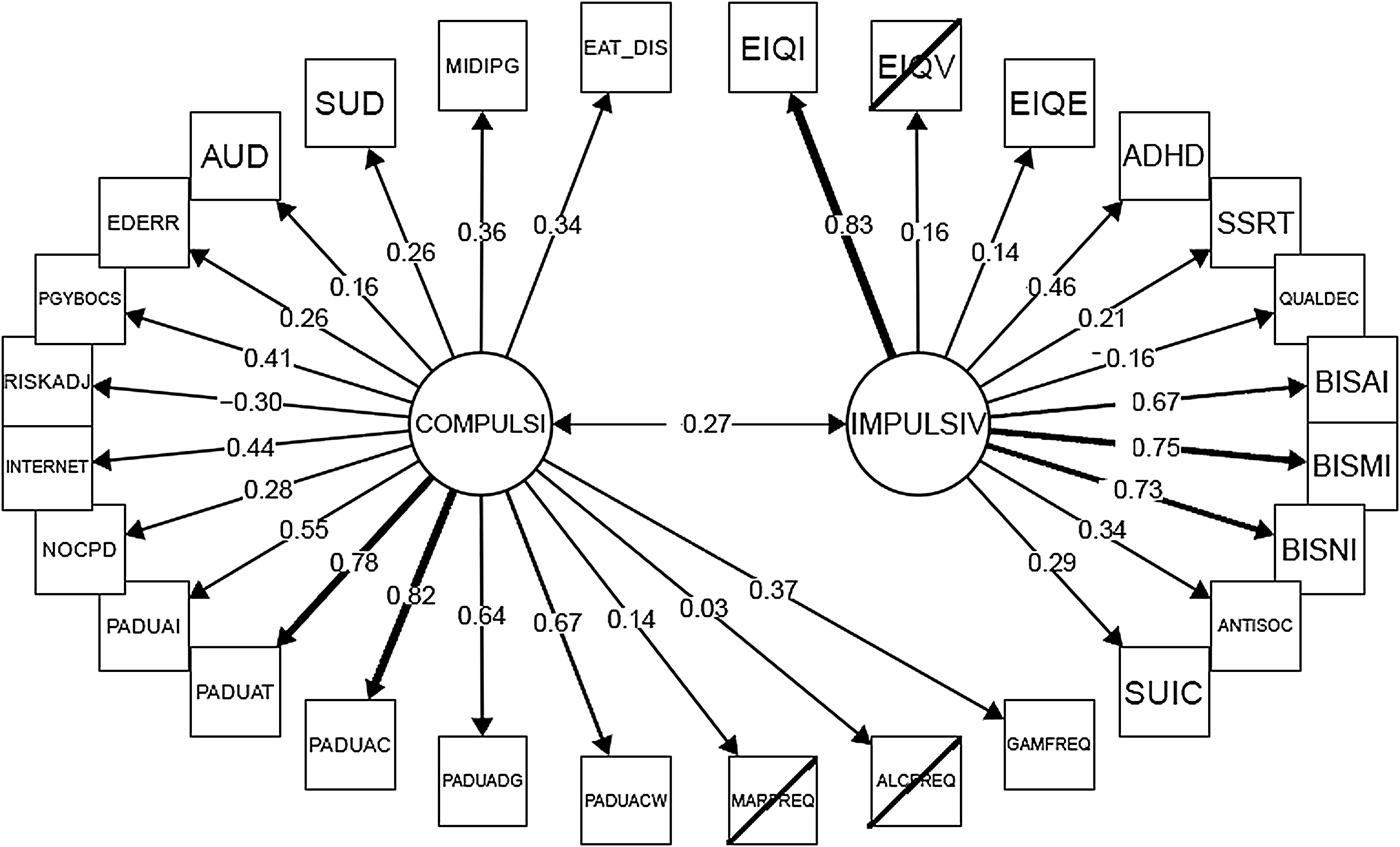
Fig. 2. Two-factor correlated model, showing factor loadings. Variables with non-statistically significant loading (p > 0.05) are shown in strike-through. Abbreviations – see footer to Fig. 1.
Higher scores on the impulsivity and compulsivity factors, respectively, were significantly correlated with worse quality of life on the Quality of Life Inventory (r = 0.27, p < 0.00001; and r = 0.30, p < 0.000001).
Discussion
Mental disorders characterized by impulsive or compulsive symptoms constitute a huge burden for patients, family members, and society at large. Psychiatry is seeking methods of refining the definition of mental disorders, and of better understanding their etiology and neurobiological substrates. One way of tackling this challenge (Cuthbert & Insel, Reference Cuthbert and Insel2013), is to use a multi-tiered approach examining not just categorical mental disorders but also dimensional psychopathology, personality, and neurocognitive functioning (Chamberlain & Menzies, Reference Chamberlain and Menzies2009). Here, we examined such multi-tiered measures in a sample of young adults who were not treatment seeking. We found that impulsive and compulsive manifest measures were underpinned by distinct latent traits of impulsivity and compulsivity, which were positively correlated with each other. Furthermore, higher scores on each of these latent traits were significantly correlated with worse quality of life, thereby confirming their clinical relevance. The two correlated factor model was a better fit to the data than alternative conceptual models in which impulsive and compulsive manifest measures were mediated by a single latent factor of ‘disinhibition’; and the alternative conceptualizations that impulsive and compulsive latent traits were in opposition to each other (negatively correlated) or independent of each other. We focused on impulsivity and compulsivity, which we view as being complementary to other suggested frameworks for understanding mental disorders, such as the idea of externalizing v. internalizing symptoms; or the existence of a bipolar mood spectrum. Impulsivity and compulsivity are related to these other models but are not the same thing (Eisenberg et al. Reference Eisenberg, Valiente, Spinrad, Liew, Zhou, Losoya, Reiser and Cumberland2009). Ultimately, psychiatry may benefit from a more cohesive model that integrates multiple of these ideas (Lara & Akiskal, Reference Lara and Akiskal2006).
Manifest measures loading most strongly and significantly on the latent trait of impulsivity (see Fig. 2) were (in descending order of statistical significance): impulsiveness on the Eysenck Inventory, impulsiveness on the Barratt questionnaire, dimensional ADHD symptoms, presence of ASPD, suicide risk, longer stop-signal reaction times, and extraversion on the Eysenck Inventory. As a caveat, it should be noted that some of these loadings, while statistically significant, were relatively small in magnitude. These findings are consistent with studies in clinical populations, which have reported positive associations between such personality-based measures of impulsivity, and ADHD (Malloy-Diniz et al. Reference Malloy-Diniz, Fuentes, Leite, Correa and Bechara2007); and between such personality-based measures and ASPD (Swann et al. Reference Swann, Lijffijt, Lane, Steinberg and Moeller2009). There is also evidence that Barratt impulsiveness was associated with suicidality in the context of depressive symptoms (Swann et al. Reference Swann, Steinberg, Lijffijt and Moeller2008). Stop-signal reaction time impairment has been observed in meta-analysis of available cognitive studies comparing ADHD groups to healthy volunteers (Lijffijt et al. Reference Lijffijt, Kenemans, Verbaten and van Engeland2005; Chamberlain et al. Reference Chamberlain, Robbins, Winder-Rhodes, Muller, Sahakian, Blackwell and Barnett2011). In non-treatment-seeking adults with ASPD, stop-signal deficits were observed v. healthy controls (Heritage & Benning, Reference Heritage and Benning2013; Chamberlain et al. Reference Chamberlain, Derbyshire, Leppink and Grant2016).
In contrast to research regarding impulsivity, the exploration of compulsivity has received relatively little research attention (Robbins et al. Reference Robbins, Gillan, Smith, de Wit and Ersche2012). Manifest measures of compulsivity that loaded significantly onto the latent factor of compulsivity were as follows (in descending order of statistical significance): obsessive–compulsive symptoms on the Padua Inventory, problematic Internet use, problem gambling symptoms, presence of an eating disorder, less risk adjustment on the CGT, OCPD traits, more extra-dimensional set-shift errors on the Set-Shift Task (IED), and presence of substance/alcohol use disorder. Again, some of these variables had relatively low loading onto the latent construct, albeit they were significant. Compulsivity has been defined, hypothetically, as an intermediate phenotype or trait characterized by persistence of habitual/repetitive actions despite untoward consequences (Robbins et al. Reference Robbins, Gillan, Smith, de Wit and Ersche2012). Our data are supportive of the view that compulsivity can be conceptualized as such a trait, and demonstrate that it is largely separable from impulsivity. Relatively impaired set-shifting has been identified in patients with OCD (Veale et al. Reference Veale, Sahakian, Owen and Marks1996; Watkins et al. Reference Watkins, Sahakian, Robertson, Veale, Rogers, Pickard, Aitken and Robbins2005; Chamberlain et al. Reference Chamberlain, Fineberg, Menzies, Blackwell, Bullmore, Robbins and Sahakian2007), and in those with eating disorders (Kanakam & Treasure, Reference Kanakam and Treasure2013; Aloi et al. Reference Aloi, Rania, Caroleo, Bruni, Palmieri, Cauteruccio, De Fazio and Segura-Garcia2015; Perpina et al. Reference Perpina, Segura and Sanchez-Reales2016), compared with healthy controls. Set-shifting errors, and reduction of behavioral adjustment as a function of risk, are both indicative of inflexible or habitual response styles. One interpretative model is that these response patterns may be due to a tendency toward habitual behaviors at the expense of goal-directed behaviors (Gillan & Robbins, Reference Gillan and Robbins2014). In a large-scale Internet-based study, deficits in goal-directed control were strongly associated with compulsive behaviors and intrusive thoughts, but were also associated to a lesser degree with impulsivity on the Barratt questionnaire (Gillan et al. Reference Gillan, Fineberg and Robbins2017).
Problematic Internet use is not yet considered a mental disorder in DSM-5, but has been highlighted as a concept in need of further study (in this and other narrower guises, such as ‘Internet Gaming Disorder’) (Grant & Chamberlain, Reference Grant and Chamberlain2016). Studies report high rates of mental disorders including OCD in people with pathological Internet use (Carli et al. Reference Carli, Durkee, Wasserman, Hadlaczky, Despalins, Kramarz, Wasserman, Sarchiapone, Hoven, Brunner and Kaess2013; Durkee et al. Reference Durkee, Carli, Floderus, Wasserman, Sarchiapone, Apter, Balazs, Bobes, Brunner, Corcoran, Cosman, Haring, Hoven, Kaess, Kahn, Nemes, Postuvan, Saiz, Varnik and Wasserman2016). In an Internet-based survey, some types of obsessive–compulsive symptoms (impulses to harm self/others and checking compulsions) were the most important variables across impulsive–compulsive measures in terms of classifying participants as having moderate–severe Internet addiction (Ioannidis et al. Reference Ioannidis, Chamberlain, Treder, Kiraly, Leppink, Redden, Stein, Lochner and Grant2016). Research into OCPD is scant, but data indicate disproportionately worse set-shifting impairment in OCD patients with this comorbidity (Fineberg et al. Reference Fineberg, Sharma, Sivakumaran, Sahakian and Chamberlain2007; Fineberg et al. Reference Fineberg, Day, de Koenigswarter, Reghunandanan, Kolli, Jefferies-Sewell, Hranov and Laws2015). Our finding that substance use disorders loaded significantly and positively onto the latent compulsivity factor is unsurprising. Criteria for substance use disorders includes features such as narrowing of the behavioral repertoire, persistently engaging in use despite negative consequences, and unsuccessful attempts to cut back, which fit the concept of compulsivity closely.
To our knowledge, no previous studies have explored the latent structure of impulsivity and compulsivity measures within one setting, using such a broad range of measures. However, there is an extensive body of literature, mostly focusing on psychopathology, suggesting the existence of an underlying ‘internalizing’ dimension (predisposition to anxiety/depressive disorders) and an ‘externalizing’ dimension (predisposition to, e.g. substance use, antisocial personality, ADHD) (Caspi et al. Reference Caspi, Houts, Belsky, Goldman-Mellor, Harrington, Israel, Meier, Ramrakha, Shalev, Poulton and Moffitt2014). OCD symptoms have not been consistently included in studies exploring the structure of psychopathology (Caspi et al. Reference Caspi, Houts, Belsky, Goldman-Mellor, Harrington, Israel, Meier, Ramrakha, Shalev, Poulton and Moffitt2014). In a large sample of adolescents (IMAGEN consortium), the best-fit model for selected psychopathological measures comprised two factors (compulsivity and externalizing behaviors) (Montigny et al. Reference Montigny, Castellanos-Ryan, Whelan, Banaschewski, Barker, Buchel, Gallinat, Flor, Mann, Paillere-Martinot, Nees, Lathrop, Loth, Paus, Pausova, Rietschel, Schumann, Smolka, Struve, Robbins, Garavan, Conrod and Consortium2013). The compulsivity factor showed strong associations with OCD and eating disorders, whereas the externalizing behaviors factor showed strong associations with substance misuse, conduct disorder, and (to a lesser degree) ADHD symptoms. In another paper by the same research consortium (IMAGEN), psychopathological measures were first entered into initial CFA (Castellanos-Ryan et al. Reference Castellanos-Ryan, Briere, O'Leary-Barrett, Banaschewski, Bokde, Bromberg, Buchel, Flor, Frouin, Gallinat, Garavan, Martinot, Nees, Paus, Pausova, Rietschel, Smolka, Robbins, Whelan, Schumann and Conrod2016). The relationships between resulting factors and other measures, such as cognitive functioning were then explored. The authors opted for a bi-factor model incorporating three factors. It was found that a general psychopathology factor correlated with worse response inhibition and greater temporal discounting; an externalizing factor correlated with high risk taking on a gambling task; and that an internalizing factor correlated with attentional bias toward negatively valenced verbal stimuli. This study measured impulsivity with a go/no-go task (rather than a stop-signal task), and did not quantify attentional set-shifting.
The current study has several limitations, which merit consideration. Our sample did not exclude people with mental disorders. This can be viewed as being beneficial to exploring latent traits of impulsivity and compulsivity since it would have yielded a broader set of data for the purposes of measuring covariance, and is also parsimonious with the RDoc concept. Our sample showed average impulsive and compulsive personality questionnaire scores, and cognitive performance, akin to that reported in previous normative populations. However, the findings may not generalize to other populations, such as patients in clinical settings. We treated personality, symptoms, and cognition as being on the same conceptual plane, with a view to maintaining model simplicity and avoiding unnecessary assumptions. We used confirmatory rather than exploratory factor analysis because the concepts of impulsivity and compulsivity are well established in the literature (Hollander & Cohen, Reference Hollander and Cohen1996; Robbins et al. Reference Robbins, Gillan, Smith, de Wit and Ersche2012) and our research question pertained to the relationship between them, rather than the separate issue of whether more latent factors exist. For pragmatic reasons, we did not include all possible measures of relevance to impulsivity and compulsivity. For example, we did not assess reflection–impulsivity, or tasks of ‘incremental’ habit learning (Gillan & Robbins, Reference Gillan and Robbins2014; Hauser et al. Reference Hauser, Eldar and Dolan2016). It would be valuable to include such parameters in future work. Lastly, some recent studies of personality and psychopathology have explored bi-factor models. In bi-factor models, a general factor or ‘p’ (analogous to the historical ‘g’ factor in intelligence quotient research) is included, on the assumption that a proportion of covariance across all measures may measure a common trait (Caspi et al. Reference Caspi, Houts, Belsky, Goldman-Mellor, Harrington, Israel, Meier, Ramrakha, Shalev, Poulton and Moffitt2014). The findings from the two correlated factor model suggest against using a bi-factor structure for the current data, because the proportion of shared variance between the impulsivity and compulsivity factors was only ~7%. Furthermore, bi-factor models may be intrinsically biased toward yielding superior model fit parameters over non bi-factor models, as a consequence of unmodeled complexity (Murray & Johnson, Reference Murray and Johnson2013). In post hoc analysis, furthermore, we found that the ω coefficient was inferior when a bi-factor model fit was applied to the data (ω < 0.7 for the general factor), v. the two correlated factor model (ω impulsivity = 0.74; ω compulsivity = 0.79) (Reise, Reference Reise2012). The biological and clinical plausibility and interpretation of ‘g’ or ‘p’ factor may be problematic (Vanheule et al. Reference Vanheule, Desmet, Groenvynck, Rosseel and Fontaine2008) – for example, ‘p’ could represent response style rather than containing substantial meaning.
In summary, this study used a range of psychopathological, personality, and cognitive measures to demonstrate the existence of two separable but positively correlated latent traits of impulsivity and compulsivity, in a sample of young adults recruited from the background population. Higher scores on each latent trait was significantly correlated with worse quality of life, and was associated with greater risk of having one or more relatives with a behavioral or substance addiction, supporting the clinical relevance of these traits.
We do not suggest that all manifest measures of impulsivity and compulsivity are ‘two things’; there is evidence, for example, that different measures of impulsivity can be fractionated (Meda et al. Reference Meda, Stevens, Potenza, Pittman, Gueorguieva, Andrews, Thomas, Muska, Hylton and Pearlson2009; MacKillop et al. Reference MacKillop, Weafer, C Gray, Oshri, Palmer and de Wit2016). However, the current findings do support the notion that latent forms of impulsivity and compulsivity exist in a dimensional or continuous sense that they are largely separable from each other, and that higher impulsivity tends to associate with higher compulsivity (rather than the opposite). Treatments targeting impulsivity and compulsivity at the conceptual level, or in terms of specific manifest forms (such as neurocognitive impairment), would be potentially valuable. Future work should identify neural and neurochemical underpinnings of these latent dimensions with a view to informing nosological and neurobiological models; and should also attempt to integrate multiple candidate dimensions besides impulsivity and compulsivity.
Supplementary Material
The supplementary material for this article can be found at https://doi.org/10.1017/S0033291717002185.
Acknowledgements
This work was funded by a Wellcome Trust Clinical Fellowship to Dr Chamberlain (UK; Reference 110049/Z/15/Z) and by a Center of Excellence in Gambling Research grant from the National Center for Responsible Gaming to Dr Grant (USA). Dr Stochl was partly supported by Charles University PRVOUK program number P38. The authors would like to thank all study participants.
Declaration of Interest
Dr Chamberlain consults for Cambridge Cognition. Dr Grant has received research grants from NIMH, National Center for Responsible Gaming, and Forest and Roche Pharmaceuticals. He receives yearly compensation from the Springer Publishing for acting as Editor-in-Chief of the Journal of Gambling Studies and has received royalties from the Oxford University Press, American Psychiatric Publishing, Inc., Norton Press, and McGraw Hill.








