Introduction
Primary care providers and commissioners are being alerted to the growing numbers of people with dementia in England and the consequences of this rise for their services [Department of Health (DH), 2009, 2010]. The numbers of people with dementia are expected to double globally by 2030, and more than triple by 2050 [World Health Organization (WHO), 2012]. One consequence of this is a steady rise in the estimated numbers of people who will die with dementia and who will require end of life or palliative care. These are estimated at around 66 000 people per year in England, based on a population benchmark of around 800 per 100 000 people aged 65 and older, per year (NICE, 2012).
The cognitive changes that occur in dementia can make providing palliative or end of life care considerably more challenging for primary care practitioners than when they are providing it to patients with other conditions, for several reasons. Communication difficulties increase as the disease unfolds, prognosis is uncertain and prediction of death is difficult. Close collaboration is needed across service and sector boundaries to overcome these difficulties (Mathie et al., Reference Mathie, Goodman, Froggatt, Crang, Iliffe, Manthorpe and Barclay2012). These difficulties compound pressure on health and social care providers, who are already facing a legacy of inequitable resource allocation for older people, the stigma of dementia and the low status of people providing their care.
Primary care commissioners who are already under pressure to raise the standards of end of life care for people with dementia and enhance their dignity in the face of a progressive degenerative disease may seek guidance about best service configurations, but they will find it sparse. They will note the frequent overlap of palliative and end of life care debates (in this review we use the terms as employed by the authors, recognizing that they are used often interchangeably and that several definitions are used). There is a wide gap between knowledge about the principles of end of life or palliative care and their use in every day practice with people with dementia. To optimally promote the quality of life and death of a person affected by a complex, incurable and life-threatening health problem like dementia, care systems need to address the person's physical, emotional, psychosocial and spiritual needs, as summarized in the WHO definition of palliative care (Sepulveda et al., Reference Sepulveda, Marlin, Yoshida and Ullrich2002). Translating these aspirations into existing service provision or modifying practice will encounter service dislocations, gaps and duplications. NICE (2010) has provided a commissioning and benchmarking tool to aid commissioners of end of life care for people with dementia that identifies the interconnectedness of decision making at service level. However, given current cost pressures in England, commissioners will not be able to maintain dual systems and shore up professional boundaries, or to develop new services without decommissioning existing provision.
This paper analyses published reviews of palliative and end of life care services for people with dementia to provide an overview of the evidence for primary care providers and commissioners. This synthesis was undertaken to inform the IMPACT study – a four-year European Commission (EC)-funded project (2011–2015) whose aim is to develop and test optimal implementation strategies to improve palliative care for people with dementia care, using quality indicators as levers for change (Campbell et al., Reference Campbell, Braspenning, Hutchinson and Marshall2003).
Methods
A rapid appraisal methodology underpinned our review of the literature. This approach was chosen because of the need for the study to keep pace with the speedy evolution of policy in health and care systems for people with dementia and for end of life care. This review of reviews, rather than systematically aggregating data, adopted a critical interpretive approach (Dixon-Woods et al., Reference Dixon-Woods, Cavers, Agarwal, Annandale, Arthur, Harvey, Hsu, Katbamna, Olsen, Smith, Riley and Sutton2006). The purpose of this was to construct theories grounded in research, and to generate practical methods to evaluate these effects.
Critical interpretive synthesis does not demand a comprehensive search of literature as required by a systematic review, but rather seeks to identify publications of ‘likely relevance’. The focus is on reconceptualizing the phenomena of interest rather than presenting an exhaustive summary of the literature. Although the aim of this review was to be as inclusive as possible of the current relevant literature and time frame for the chosen reviews, we nevertheless recognized the importance of setting boundaries about which papers to include (Dixon-Woods et al., Reference Dixon-Woods, Cavers, Agarwal, Annandale, Arthur, Harvey, Hsu, Katbamna, Olsen, Smith, Riley and Sutton2006).
We conducted a search of electronic databases of English language papers published in peer-reviewed journals, 2000–2011 inclusive, using broad terms related to palliative care and dementia. The search terms were palliative care, terminal care, attitude to death, or dying, end of life care, comfort care, symptom control, end stage disease, living will, advance directive, palliate, palliative, and Alzheimer's disease, dementia, neurodegenerative diseases, Parkinson's disease, aphasia. We identified 6167 papers. Titles and abstracts were read by two authors (A.W. and M.R.). Papers were included if they were literature reviews of palliative or end of life care for people with dementia/Parkinson's disease/Lewy body dementia/cognitive impairment/Alzheimer's disease or any other cognitive impairment, in any setting (hospital, care home, community) and covering people of all ages. Papers were excluded if they covered palliative care focusing on other conditions, or were about an aspect of dementia care and treatment not related to palliative care, for example, diagnosis. A broad range of papers was sought initially and a third author (S.I.) read papers if there were doubts over their inclusion.
We identified 99 papers as relevant to a synthesis of evidence on the management of dementia at the end of life. Those papers reviewing only one aspect of palliative care, for example pain control, were excluded. Only reviews presenting an overview of palliative care as a process were retained. This left 36 papers that were overviews of some or most aspects of palliative care in dementia. Of these 36, eight met all the Oxman and Guyatt (Reference Oxman and Guyatt1991) quality criteria for a review (see Table 1). These papers were then summarized and analysed using a data extraction tool (see Table 2).
Table 1 Criteria for assessing the scientific quality of research reviews

Table 2 Overview of papers

The provenance of the final selection of publications is shown in a PRISMA chart (Figure 1) (Moher et al., Reference Moher, Liberati, Tetzlaff and Altman2009). All authors were involved in reviewing selected papers, and discussing their contents and conclusions. Themes were discussed in face-to-face meetings between M.R. and S.I., refined and circulated to all authors.

Figure 1 PRISMA diagram.
Findings
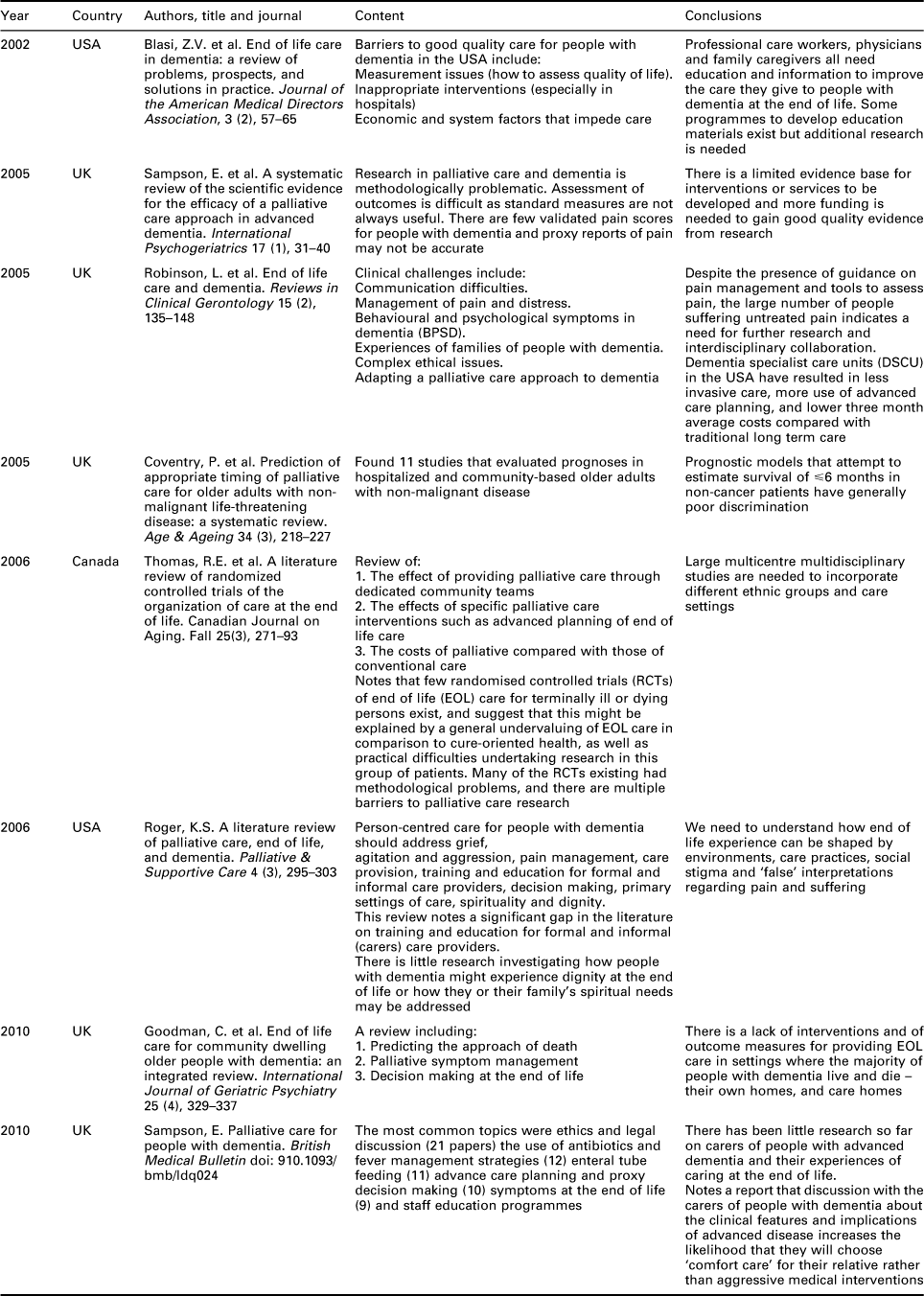
The main contents and conclusions of the eight papers identified for this review (Blasi et al., Reference Blasi, Hurley and Volicer2002; Coventry et al., Reference Coventry, Grande, Richards and Todd2005; Robinson et al., Reference Robinson, Hughes, Daley, Keady, Ballard and Volicer2005; Sampson et al., Reference Sampson, Ritchie, Lai, Raven and Blanchard2005; Roger, Reference Roger2006; Thomas et al., Reference Thomas, Wilson and Sheps2006; Goodman et al., Reference Goodman, Evans, Wilcock, Froggatt, Drennan, Sampson, Blanchard, Bissett and Iliffe2010; Sampson, Reference Sampson2010) are summarized in Table 2.
Our critical synthesis generated five main themes from this review of the reviews: (1) carers’ (family caregivers’) experiences; (2) person-centred care; (3) practice (including advance care planning, pain and comfort, nutrition, medical complications and minimizing the distress of behavioural symptoms); (4) system factors, including ethical dilemmas, decision making, information and training; and (5) research priorities.
Carers’ experiences
Despite many decades of research into family carers’ experiences, there has been comparatively little research on carers of people with advanced dementia and their experiences of caring at the end of life according to Sampson's (Reference Sampson2010) review. Research that evaluates the effect of general and specialist palliative care on psychosocial outcomes in people with dementia and their carers needs to take account of different relationship structures and social networks (Goodman et al., Reference Goodman, Evans, Wilcock, Froggatt, Drennan, Sampson, Blanchard, Bissett and Iliffe2010).
Person-centred care
According to Sampson (Reference Sampson2010) maintaining person-centred care involves providing a high standard of care and finding positive and meaningful ways in which to interact with the person with dementia. There was little discussion of person-centred care within the literature reviewed for this paper. This may be because definitions vary and the concept is hard to operationalize. Sampson's (Reference Sampson2010) review notes the claims that loss of personhood ‘often’ occurs before bodily death, with the cognitive deterioration associated with dementia (Meuser and Marwit, Reference Meuser and Marwit2001). Some people continue to be expressive in many ways that are non-verbal but are nevertheless a form of communication. Roger's (Reference Roger2006) review suggests that staff and family carers should be person-centred (Post, Reference Post1995) because if care tasks are better understood then people with dementia seem to respond favourably and carers experience a decrease in stress (Roger, Reference Roger2006). Such a finding has relevance to the commissioning of training.
Roger (Reference Roger2006) advocates developing a better understanding of how communication and daily interactions between carers and people with dementia may increase the latter's well-being. He also recommends that behavioural and non-verbal communication be encouraged at the late stage, as a combination of interpersonal strategies. For funders of care there is the relevant point that contact time spent with people with dementia who are dying should be explicit and valued.
Advance care planning
Discussion in the reviews about advance care plans is generally uncritical and the status of such plans is not always clear. Sampson (Reference Sampson2010) describes one form of advance care planning in the United Kingdom and Australia, where Lasting Powers of Attorney (LPAs) legal powers and advance decision records, such as the Let Me Decide programme, enable the appointment of a proxy decision maker who can make decisions in the event that a person no longer has the capacity to do so. In Australia this led to a significant decrease in the transfer of nursing home residents to hospital with no changes in overall mortality (Caplan et al., Reference Caplan, Meller, Squires, Chan and Willett2006). There has been little research so far on carers of people with advanced dementia and their experiences of caring at the end of life in this context of proxy decision making, according to Sampson's (Reference Sampson2010) review. This is not surprising in England and Wales since LPAs and advance decisions under the Mental Capacity Act 2005 (implemented in 2007) were comparatively unknown at that time. There is some evidence that informing family carers of people with dementia about the clinical features and implications of advanced disease increases the likelihood that they will choose ‘comfort care’ for their relative rather than aggressive medical interventions (Volandes et al., Reference Volandes, Paasche-Orlow, Gillick, Cook, Shaykevich, Abbo and Lehmann2009).
McCarthy et al. (Reference McCarthy, Addington-Hall and Altmann1997) argue that early identification of patients with future palliative care needs should improve their end of life care. Not surprisingly, the reviews portray advance care plans as more likely to be initiated and managed in centres with a specialised interest in palliative care, but this is a rare care setting for people with dementia (Sampson, Reference Sampson2010). Shega's (Reference Shega2003) review notes the limited access to hospices for people with dementia, which the authors attribute to a lack of awareness that dementia is a terminal illness, and anxiety among hospice professionals about not being able to manage behavioural symptoms associated with dementia.
Pain and comfort
Pain is often difficult to assess in people with advanced dementia. Sampson et al. (Reference Sampson, Ritchie, Lai, Raven and Blanchard2005) and Sampson (Reference Sampson2010) found that people with dementia's communications about pain are not always heard or interpreted. Communication difficulties were also identified by Goodman et al. (Reference Goodman, Evans, Wilcock, Froggatt, Drennan, Sampson, Blanchard, Bissett and Iliffe2010) as presenting a challenge to practitioners as there may be several possible causes of distress and possibly no particular behaviours or signs associated with an individual's pain. An array of assessment tools (such as the Abbey Tool) has been developed to address this problem (Abbey et al., Reference Abbey, Piller, De Bellis, Esterman, Parker, Giles and Lowcay2004). While Sampson (Reference Sampson2010) also found no evidence that pain produces any particular or unique signs or behaviours (see Regnard et al., Reference Regnard, Mathews, Gibson and Clarke2003), she suggests tools such as the Disability Distress Assessment Tool may be useful (Regnard et al., Reference Regnard, Mathews, Gibson and Clarke2003). Robinson et al. (Reference Robinson, Hughes, Daley, Keady, Ballard and Volicer2005) note that assessment tools have mainly been used in small scale trials, but some appear to be valid and easy to complete. There is consensus among the reviews that optimal management of pain in dementia is poorly understood, suggesting a need for more research.
The importance of non-pharmacological responses to pain is highlighted in Robinson et al.'s (Reference Robinson, Hughes, Daley, Keady, Ballard and Volicer2005) review but this reported evidence that these are not routinely or explicitly incorporated into care. A stepwise approach to pharmacological management such as the WHO analgesic ladder has been used to guide pharmacological treatment in some settings and adjuvant treatments, such as antidepressants, can also be tried (Robinson et al., Reference Robinson, Hughes, Daley, Keady, Ballard and Volicer2005).
Nutrition
The use of artificial nutrition for people with advanced dementia varies between countries and settings, as discussed by Goodman et al. (Reference Goodman, Evans, Wilcock, Froggatt, Drennan, Sampson, Blanchard, Bissett and Iliffe2010). These authors note that in the Netherlands artificial nutrition and hydration are used rarely because the course of dementia is considered ‘normal’. Robinson et al. (Reference Robinson, Hughes, Daley, Keady, Ballard and Volicer2005) highlight that weight loss in advanced dementia increases anxiety among care practitioners and family carers. People with severe dementia may refuse food, even if every assistance and encouragement is offered (Ouldred and Bryant, Reference Ouldred and Bryant2008). Sampson et al. (Reference Sampson, Candy and Jones2009) recommend that all possible options are considered for an individual and that assessments among people who are at nutritional risk should be conducted by swallowing specialists. Commissioners may wish to investigate the accessibility and availability of such specialists to work with people with dementia and with those supporting them, for example, in care homes or at home.
Interestingly the research reviews appear not to cover hydration as much as nutrition. Goodman et al.'s (Reference Goodman, Evans, Wilcock, Froggatt, Drennan, Sampson, Blanchard, Bissett and Iliffe2010) review found no research that focused on different ways of using nutrition and fluids as a means of providing comfort and enhanced quality of life.
Medical complications
Medical complications occur frequently in people with advanced dementia. The complications summarized by Robinson et al. (Reference Robinson, Hughes, Daley, Keady, Ballard and Volicer2005) are fever and infections, bladder and bowel incontinence, pressure sores and ulcers. The treatment options for these are independent of dementia, though the importance of symptom control is paramount. Preventive interventions or intensive treatment of chronic conditions at the end of life should be discouraged, according to Robinson et al. (Reference Robinson, Hughes, Daley, Keady, Ballard and Volicer2005).
Moreover, use of antibiotics to treat intercurrent infections (most frequently respiratory or urinary tract) is controversial. Sampson (Reference Sampson2010) notes evidence that treatment may not change mortality and antibiotic treatment may reduce discomfort; although may also potentially prolong suffering by delaying death.
Behavioural symptoms
Many people with dementia develop behavioural and psychological disturbances such as agitation, apathy, aggression, depression, delusions, wandering, sleep disturbances and hallucinations (Douglas et al., Reference Douglas, James and Ballard2004). There is evidence that as the severity of dementia continues, aggressive behaviours increase and this then affects end of life care (Roger, Reference Roger2006).
There is little information within the literature about behavioural symptoms of dementia and their effect on access to palliative care. As noted above, Sampson's (Reference Sampson2010) review states that people with advanced dementia will have difficulties in communicating that they are in pain, which may provoke behavioural changes such as agitation, distress, social withdrawal or resistive behaviour. Difficult behaviours for those providing care, such as aggression and resistance to care, may also be indicators of unmet needs such as under-detected or under-treated pain, delirium or infection.
Sampson's (Reference Sampson2010) review emphasises the importance of the environment or setting of end of life care. For example, she notes noisy environments may worsen agitation, whereas the chance to be outside during the day may help reduce it. Roger's (Reference Roger2006) review concludes that better communication strategies and strong positive social relationships may decrease agitation and aggression. He suggests that caring and supportive environments can diminish aggressive outbursts in people with dementia.
Ethical dilemmas
There is little explicit discussion of ethical dilemmas in the reviews. Decisions about when to initiate end of life care can vary from country to country (Goodman et al., Reference Goodman, Evans, Wilcock, Froggatt, Drennan, Sampson, Blanchard, Bissett and Iliffe2010). It is not clear if these are related to different ethical or cultural practices and beliefs. As noted above, artificial nutrition is a commonly discussed ethical dilemma in some countries. When a person with dementia is no longer able to eat, family members and clinicians may discuss whether to start artificial nutrition, but the evidence shows that there is no significant effect on morbidity or mortality (Sampson et al., Reference Sampson, Candy and Jones2009). People with dementia may receive unnecessary investigations and procedures and are more likely to be physically restrained compared with patients who are cognitively intact (Mitchell et al., Reference Mitchell, Kiely and Hamel2004). Advance wishes and instructions about nutrition (or other matters) at the end of life are reported to be poorly documented or not known by primary care providers in the United States (Gillick, Reference Gillick2000) but there is evidence that they are becoming better known in England (Manthorpe et al., Reference Manthorpe, Samsi and Rapaport2012).
Education and training
There is a chorus of claims (Blasi et al., Reference Blasi, Hurley and Volicer2002; Roger, Reference Roger2006; Goodman et al., Reference Goodman, Evans, Wilcock, Froggatt, Drennan, Sampson, Blanchard, Bissett and Iliffe2010; Sampson, Reference Sampson2010) that staff and carers would benefit from education about providing palliative care for people with dementia, and the needs of carers, and of staff. Many reviews state that health and social care staff lack specific and useful education on this topic and that this is reflected in their low confidence about the management of dementia and palliative care together (Birch and Draper, Reference Birch and Draper2008). Few of the reviews acknowledge that social care staff working with people with dementia generally have less access to training than other care staff, and are also poorly paid and have low status (Hussein and Manthorpe, Reference Hussein and Manthorpe2012). There is an unresolved tension in the reviews which call for more training without commenting that care for people with dementia rests on non-professionally qualified care staff among whom high turnover and staff shortages are endemic in many community settings. For primary care commissioners there are possible levers in paying more for quality markers or standards, as has been common in some English local authority contracts for residential care for many years.
Research priorities
One constant theme from the reviews is that there is a lack of research in palliative care for people with dementia. Thomas et al. (Reference Thomas, Wilson and Sheps2006) suggest that the lack of research is partly because of a lack of understanding of the need for palliative care for people with dementia, as well as methodological limitations in carrying out studies among this group of patients. As Moriarty et al. (Reference Moriarty, Rutter, Ross and Holmes2012) argue, research is needed to clarify what support, local arrangements and partnerships care homes need to improve end of life care for people with dementia. We suggest that the same observation could be made about the support needed by home care providers, particularly the growing group of directly employed care workers, who may be less experienced in end of life care. Larger studies of people with dementia from diverse backgrounds and settings, which follow participants to the end of life, are also needed (Moriarty et al., Reference Moriarty, Rutter, Ross and Holmes2012).
There may also be scope for more localized-specific audits and research. For example, Thomas et al. (Reference Thomas, Wilson and Sheps2006) found little evidence of bereavement support within palliative care services, specifically for staff and relatives who have been caring for a person with dementia. Locally commissioned bereavement services could be audited to establish their skills, confidence and capacity in providing bereavement support and those contracted to provide care services could be asked to report on their staff's access to human resources or workplace counselling.
Discussion
Current government policy in England, such as the National Dementia Strategy (DH, 2009) and the End of Life Care Strategy (DH, 2008), make little reference to dementia and palliative or end of life care together. The National Institute for Clinical Excellence (NICE) and SCIE guidelines (National Institute for Health and Clinical Excellence (NICE) and Social Care Institute for Excellence (SCIE), 2006) for dementia include recommendations on the use of the Gold Standards Framework and the Liverpool Care Pathway for the care of the dying, but note that these approaches, which were developed for palliative care for people with cancer, need to be modified for people with dementia. Health and social care commissioning is influenced by many factors other than research evidence, including political pressure, ideological stance and the need to take action. Influencing policy development and implementation is now a challenge for researchers in all those countries with government-driven dementia strategies (see Banerjee, Reference Banerjee2012). As Black (Reference Black2001) has pointed out timing is important: ‘Windows of opportunity to make change open up only rarely and briefly, when policy makers’ values happen to coincide with the implications of research’.
The need to take action is driven in part by clinical needs, which are great in a domain (like this one) where evidence to guide practice is sketchy. Combined with clinical experience, the limited evidence does suggest important research questions. For example, we know little about how best to support family carers of a person dying with or from dementia, but we do know that carer coping abilities are very variable, with some able to deal with complex comorbidities in addition to dementia, while others struggle with medical problems that at first glance appear less onerous. We do not know how helpful specialist mental health services could be in end-of-life care, or whether a dedicated nurse specialist in dementia would improve the experience of either the person with dementia or their family carer at the end of life. Antibiotic use may relieve symptoms (see above) but at the expense of extending life of limited quality, and we do not know to manage this dilemma, except on a case-by-case basis. Admission to hospital may be undesirable at the end of life, but may still occur in situations where there is great diagnostic and prognostic uncertainty. We may have to accept that strengthening the evidence base for palliative care for people with dementia may be a slow process; the paucity of evidence may in part be due to the complexity of managing patients with advanced dementia, the needs for multiple skills and the involvement of a range of disciplines. A ‘one size fits all’ pathway may be appealing to commissioners but may simply not work.
Strengths and limitations of the study
Critical interpretative synthesis can be criticized as a method of marshalling and interpreting evidence that depends on the subjective judgements of its authors. Given the need to assist primary care commissioners’ practice and policy we see this method as a way of bringing practitioner and policy-maker perspectives to bear on the problem of contextualization in systematic reviews. We consider this subjectivity to be a strength because it promotes debate about practical action. For primary care practitioners, making sense of sometimes contradictory evidence has become increasingly difficult (Tranfield et al., Reference Tranfield, Denyer and Smart2003) Like researchers they may struggle to understand complex, fuzzy and contested problems and to systematically review and synthesize complex interventions designed to address them (Shepperd et al., Reference Shepperd, Lewin, Straus, Clarke, Eccles, Fitzpatrick, Wong and Sheikh2009). Aggregative review methods, typified by meta-analysis, are not currently useful for analysing evidence about the care of people with dementia at the end of life because of the lack of trials, and would be problematic even when trial results are published because meta-analysis produces decontextualized lessons (Pawson, Reference Pawson2002). Narrative reviews are often used to manage heterogeneous forms of evidence, but tend to produce over-contextualised recommendations like ‘more inter-agency working is needed’ that are superficial and unhelpful (Pawson, Reference Pawson2002). Our review of reviews notes the tendency to call for more research (eg, Blasi et al., Reference Blasi, Hurley and Volicer2002; Robinson et al., Reference Robinson, Hughes, Daley, Keady, Ballard and Volicer2005; Sampson et al., Reference Sampson, Ritchie, Lai, Raven and Blanchard2005; Thomas et al., Reference Thomas, Wilson and Sheps2006) but there is a surprising lack of specificity about research questions and priorities.
This overview may be limited only because it focused on reviews of palliative care in dementia. Other reviews specifically investigating, for example, nutrition, may provide a wider range of evidence on the subject. Reviews that are broad, such as the Cochrane review of nursing home care (Hall et al., Reference Hall, Kolliakou, Petkova, Froggatt and Higginson2011) may not be conclusive and not be useful to practitioners or commissioners. Rapid appraisal always runs the risk of missing useful evidence, but given the limitations of the evidence presented by the reviews summarized here, we doubt there is a substantial review that has escaped our search.
Conclusion
We do not claim to have developed a theory of palliative care for people with dementia, but suggest that this review has credible implications for primary care commissioners and researchers. There is a risk of palliative care and dementia research following increasingly divergent pathways while at the level of primary care practice and commissioning there are converging pressures. Primary care commissioners could influence the bridging of these divides by informing research funders that they would welcome interventions-based research with a strong theoretical framework that would have medium term impact on decision making. Primary care providers could encourage conversations between palliative care and dementia professional groups and networks. They could influence post qualifying and other in-service training to ensure that services and professionals learn together with the positive informal contact that this brings. Primary care professionals and funders could work collaboratively across sectors to make local preparations for the growing numbers of people with dementia who might benefit from palliative care. They can be assured that there is no research evidence that will as yet answer their problems but that research is emerging to link concepts and patient experiences.
Acknowledgments
The research leading to these results has received funding from the (European Union's) (European Atomic Energy Community's) Seventh Framework Programme [(FP7/2007–2013) (FP7/2007—2011)] under grant agreement no. (258883).