To The Editor—Varicella zoster virus (VZV) reactivation is a common complication of a weakened immune system, which can occur due to advanced age or various immunocompromising conditions. The VZV incidence in the general population is 4.82 cases per 1,000 person years, Reference Chen, Suaya and Galindo1 but this rate increases in populations with predisposing conditions. Solid-organ transplant recipients are estimated to have a VZV incidence of 22.2 cases per 1,000 patient years, with heart transplant recipients having the highest organ-specific incidence of 40.0 per 1,000 patient years. Reference Pergam, Forsberg and Boeckh2 Hematopoietic stem cell transplant recipients have reported incidence rates of 43–60 cases per 1,000 person years. Reference Chen, Suaya and Galindo1,Reference Sahoo, Hill and Xie3 With high incidence and subsequent healthcare utilization in these populations, there is an important need to prevent occupational exposure to VZV.
Recommendations for isolation precautions differ by extent of VZV involvement and immunocompromised status. For immunocompetent patients, the Centers for Disease Control and Prevention recommend contact isolation for localized VZV and concurrent airborne and contact isolation for disseminated VZV. Reference Siegel, Rhinehart, Jackson and Chiarello4 In immunocompromised patients with apparent localized disease, contact and airborne isolation are recommended until disseminated disease has been ruled out. However, it is not known whether instituting airborne isolation in this population reduces occupational exposure to VZV. At our facility, we only institute contact isolation in cases of localized VZV, regardless of immunocompromised status. We reviewed cases of disseminated VZV to evaluate whether this change in policy increased the likelihood of occupational exposure.
We performed a retrospective, descriptive review of occupational exposure investigations related to VZV. We included patients from January 2016 through December 2018 and excluded those with primary chicken pox. Demographic and clinical data were abstracted from the electronic medical record. Records were evaluated to determine whether the exposure was due to a delay in airborne precaution initiation or a progression of localized disease at presentation to disseminated VZV.
In total, 23 patients met our inclusion and exclusion criteria; 12 patients (52.2%) were female, with a median age of 64 years (interquartile range, 57–70.5 years). Also, 20 patients (87.0%) had an immunocompromising condition. This cohort included 8 patients (34.8%) with a hematologic disorder or malignancy, 4 patients (17.4%) with a solid-organ malignancy, 3 patients (13.0%) with a bone marrow transplant, 3 patients (13.0%) receiving immunosuppressing medication, and 1 patient (4.3%) with a solid-organ transplant. One patient had a solid-organ malignancy and was receiving an immunosuppressing medication. Other comorbidities included 4 (17.4%) with diabetes mellitus, and 1 patient (4.3%) had end-stage renal disease. 78.3% of cases were managed in the inpatient setting. Cases are further detailed in Table 1.
Table 1. Patient List
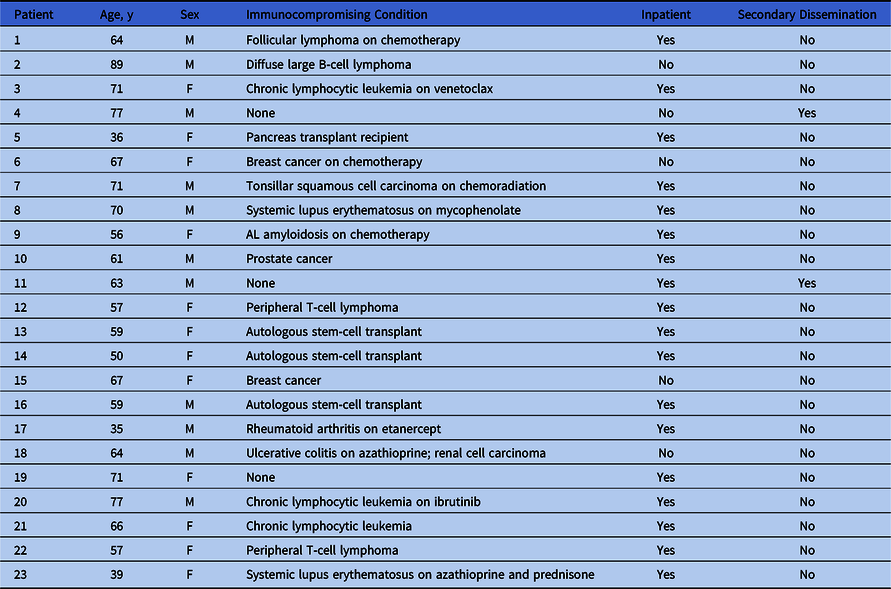
Occupational exposure occurred due to delayed diagnosis or institution of proper precautions in 21 patients (91.3%) and secondary dissemination in 2 patients (8.7%). Both patients with secondary dissemination were considered immunocompetent. Dissemination took place 2 days after healthcare presentation in both cases.
In our population, no immunocompromised patients experienced secondary dissemination after presenting with localized zoster. Instead, the exposures from immunocompromised patients were the result of delayed recognition of zoster, or failure to institute airborne isolation in recognized disseminated infection. Pre-emptive airborne isolation for immunocompromised patients with localized VZV appears unlikely to reduce occupational exposures.
Isolation precautions have been associated with numerous adverse effects. Isolated patients have increased feelings of depression, anxiety, anger, fear, and loneliness in addition to a perceived decrease in attention from healthcare staff. Furthermore, these patients have an increased risk of medical errors and preventable adverse events. Reference Abad, Fearday and Safdar5 Patients admitted for respiratory infections with associated isolation precautions have increased length of stay, expected length of stay, and hospital cost compared to nonisolated patients. Reference Tran, Bell and Stall6 Airborne isolation also imposes an institutional burden with potential adverse consequences; many healthcare facilities have few or no airborne infection isolation rooms (AIIRs). The current COVID-19 pandemic has further strained the availability of AIIRs. Presumptive airborne isolation of immunocompromised patients with localized VZV could lead to misuse of a finite resource or even unnecessary transfer to another institution.
Several alternatives to routine airborne precautions in localized disease could potentially reduce healthcare exposure. A longer time from symptom onset to antiviral treatment has been associated with dissemination of VZV. Reference Umezawa, Kakihana and Oshikawa7 This finding suggests that interventions to recognize VZV early in its course, such as patient and provider education, may promote early treatment, prevent dissemination, and reduce healthcare exposures. More information is needed regarding the best strategies to reduce occupational exposure to VZV. Finally, ensuring that healthcare workers are vaccinated against varicella would minimize the impact of exposures in the healthcare setting.
Acknowledgments
Financial support
No financial support was provided relevant to this article.
Conflicts of interest
All authors report no conflicts of interest relevant to this article.






