INTRODUCTION
Human norovirus is a common cause of foodborne outbreaks [Reference Lopman1]. Contamination of the food products might occur in different ways: during farming, harvesting, processing or serving [Reference Richards2]. Modern practices of the food industry often involve international distribution, and thus, contaminated food items may cause international outbreaks [Reference Koopmans3]. Such outbreaks have been described to have occurred due to, e.g. shellfish [Reference David4–Reference Ng7] and raspberries [Reference Falkenhorst8–Reference Pönkä12]. The role of kitchen workers in shedding norovirus during symptomatic or asymptomatic infection has also been well described [Reference Sala13–Reference Daniels17], and this possible source of transmission should always be taken into consideration when investigating norovirus outbreaks.
In 2009, the Epidemiologic Surveillance and Response Unit of the National Institute for Health and Welfare (THL), Helsinki, Finland, was notified of an increased number of foodborne outbreaks compared to previous years. Many of the outbreaks were caused by norovirus and seemed to be associated with raspberries. The first of these outbreaks was a large one affecting hundreds of people, and induced an investigation with an analytical study. The aim of this report is to describe the series of outbreaks and the investigation of the first large outbreak in this series.
School outbreak
On 23 March 2009 THL was notified of a large cluster of cases of gastroenteritis in school children and teachers at several primary schools in Seinäjoki in western Finland. Early reports suggested that the first people had fallen ill on Friday, 20 March in the afternoon and that new cases were still developing at the time of notification. More than 500 people had fallen ill by 24 March. The main symptoms reported were nausea, vomiting, diarrhoea, fever, and abdominal cramps. Many had visited a doctor during the weekend, and several people had tested positive for norovirus. The central school kitchen delivers nearly 2000 portions of lunch daily to the canteens of three schools, four kindergartens, and the canteen of Seinäjoki city office employees. The staff of the central kitchen included nine employees, two of which had become symptomatic at the same time as the pupils, teachers, and city office personnel.
Notifications of food- and waterborne outbreaks in Finland
Food- and waterborne outbreaks are notified by the local authorities to both THL and the Finnish Food Safety Authority Evira. Notification is mandatory, and the local authorities are also obliged to send a report to Evira after the outbreak investigation has been completed. The Epidemiologic Surveillance and Response Unit at THL is responsible for nationally coordinating investigations of those outbreaks which affect people in broader areas, for counselling the local authorities, and occasionally for providing practical help with outbreak investigations if needed. There are typically between 60 and 100 notifications of suspected food- or waterborne outbreaks annually in Finland.
MATERIALS AND METHODS
Investigation of the school outbreak
Epidemiological investigation
The local primary healthcare services together with the local environmental health unit collected information on the number of school children and personnel as well as the city employees who had had acute gastroenteritis between 20 and 24 March. Based on the results of the initial case finding, we decided to conduct a retrospective cohort study to determine the source of the outbreak. To exclude the possible secondary cases, we restricted the time-frame to cover transmission on 19 or 20 March only, with a maximum incubation period of 48 h. A case was defined as someone who had eaten lunch at the school centre or at the canteen for city office employees on 19 and/or 20 March, and who had had at least one symptom of gastroenteritis (nausea, vomiting, abdominal cramps, or diarrhoea, with or without fever) with an onset of symptoms between 20 and 22 March.
A standardized questionnaire was distributed to city employees, school personnel, and secondary school pupils within 1 week after the onset of the outbreak. The kindergartens and the primary schools (grades 1–6) were excluded from the analytical study, because completing the questionnaire was thought likely to be too difficult for the youngest children. Demographic data, data on the food items and beverages consumed during lunch on 19 and 20 March, as well as information on the onset and variety of symptoms were collected.
Laboratory and environmental investigation
Stool specimens from 10 symptomatic patients had been obtained for norovirus antigen test by the primary healthcare during the first days of the outbreak. Five of these specimens were sent to the Department of Virology, Helsinki University Hospital, Laboratory Services (HUSLAB), for PCR confirmation and three of them thereafter to THL for genotyping. No stool samples were obtained from kitchen staff.
The local environmental health unit conducted a site inspection at the central school kitchen on 21 March. They focused on food processing, hygiene conditions, efficacy of in-house control, and the health status of kitchen staff. They also collected samples of leftover food items served on 19 and 20 March for microbiological analyses. Samples of sausage pan, lettuce, cucumber pickles, fresh tomatoes, and frozen raspberries used for the berry dessert were cultured for Clostridium perfringens, Staphylococcus spp., Salmonella spp., and Bacillus cereus, and also investigated for norovirus.
Norovirus detection and typing
Patients' stool specimens were examined with norovirus real-time RT–PCR method as previously described [Reference Kanerva18]. Viral RNA was extracted from stool samples using the E.Z.N.A.® Total RNA kit (Omega Bio-Tek Inc., USA). Norovirus real-time RT–PCR was performed targeting to polymerase–capsid junction gene region as previously described [Reference Maunula19]. In norovirus typing the sequence analysis was performed from the polymerase region [Reference Vinje, Hamidjaja and Sobsey20]. Amplified DNA was purified by a commercial procedure (Elchrom Scientific AG, Switzerland) before sequencing (ABI Prism BigDye terminator cycle sequencing, Applied Biosystems, USA). The electropherograms were examined using the Vector NTI Advance software program (Invitrogen Corporation, USA) and the sequences compared to the sequence database in FBVE (RIVM, The Netherlands). For norovirus analyses, virus was extracted from food samples using a modified method of Dubois et al. [Reference Dubois21], which is based on virus concentration by polyethylene glycol precipitation. After nucleic acid extraction with Nuclisens magnetic silica (bioMérieux, France), amplification of a polymerase–capsid junction gene region was performed with specific primers for genogroup I and II [Reference Loisy22] by real–time one–step RT–PCR (Quantitect probe kit, Qiagen, Germany).
Statistical analysis
Attack rates (AR) and relative risks (RR) with 95% confidence intervals (CI) were calculated for lunch on 19 and 20 March as well as for individual dishes and food items. Fisher's exact test was used to check probability. The possible interactions between individual exposures were assessed by testing the difference in RR in groups of exposures. Multivariate analysis was conducted using logistic regression, the model used included all variables with a P value <0·05 in the univariate analyses. The results of multivariate analyses are reported as adjusted odds ratios (aOR) with 95% CI. Data were analysed by Stata version 10.1 (Stata Corporation, USA).
Review of the notifications and reports regarding food- and waterborne outbreaks in Finland in 2007–2009
We reviewed all notifications and reports regarding foodborne outbreaks in the files of THL and Evira during 2007–2009. Outbreaks were considered to be caused by norovirus if (i) the epidemic curve was consistent with a point-source, (ii) the incubation period was 12–48 h and the symptoms reported by the affected people were typical for norovirus infection, and (iii) norovirus had been detected in either stool samples of affected individuals and/or in food samples; outbreaks involving a batch of food which had been tested positive for norovirus during another outbreak investigation were also considered to fulfil the last criterion. For the outbreaks fulfilling all three criteria, we collected the information on the source, number of affected people, and genotyping results. Outbreaks with evidence suggesting that infected food handlers had been the most likely source were excluded.
RESULTS
Investigation of the school outbreak
Epidemiological investigation
According to the initial case finding on 24 March, there were at least 525 people with symptoms of acute gastroenteritis among the school children, school personnel and the city office employees. A total of 613 completed questionnaires were obtained; 260 (42%) respondents reported gastrointestinal symptoms.
The epidemic curve (Fig. 1) shows the number of symptomatic people according to the date of symptom onset. The onset of symptoms for the majority of people who fell ill was during a 2-day period (20–21 March). The symptoms most commonly reported were nausea (88%), vomiting (77%), abdominal cramps (72%), headache (57%), diarrhoea (48%), and fever (39%).
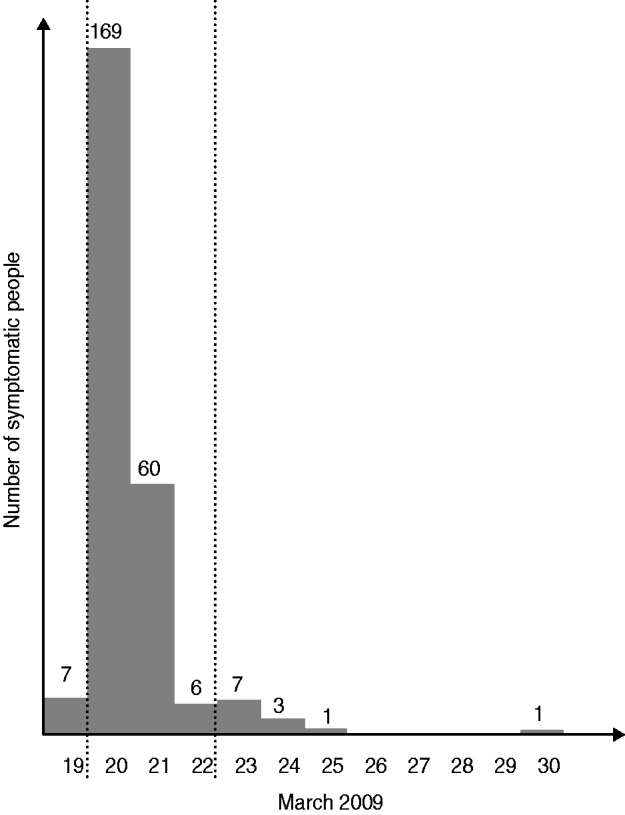
Fig. 1. Norovirus outbreak at a school centre, Seinäjoki, Finland, March 2009. Epidemic curve; number of symptomatic people by day of onset of symptoms. The dotted lines show the cases included in the analytical study.
Respondents who had not eaten lunch at the school centre or the city office canteen on 19 and/or 20 March (n=24), as well as those who had reported onset of symptoms before 20 March (n=7) or after 22 March (n=16) were excluded from the analysis. Moreover, respondents who did not provide the date of symptom onset (n=5) were excluded. Responses of 561 individuals were included in the study; 371 (66%) from the upper level of comprehensive school (grades 7–9), 164 (29%) from the high school (grades 10–12), and 26 (5%) from city employees, representing 70%, 66%, and 52%, respectively, of the total number of people linked to these places. A total of 232 (41%) respondents met the case definition.
The AR of gastroenteritis was higher in females than males (48% vs. 34%, P=0·002) and people aged >20 years compared to those younger (58% vs. 39%, P=0·004). Further, those who had eaten at the city office canteen had a higher AR than did those who had eaten at the school centre canteen (77% vs. 40%, P=0·0003).
Univariate analysis showed a statistically significant association between being a case and multiple different food items/dishes. The people who reported having eaten the raspberry-cranberry dessert (served on both 19 and 20 March), or the green salad (served on 20 March) were twice as likely to become a case than were the people who reported not having eaten these food items (Table 1). The berry dessert accounted for the highest proportion of cases (194/232). Our logistic regression model included all the variables which had a P<0·05 in the univariate analysis. The raspberry-cranberry dessert (aOR 2·6, 95% CI 1·5–4·3, P<0·001) and the green salad (aOR 2·7, 95% CI 1·7–4·3, P<0·001) remained statistically significant also in the multivariate analysis. Age and sex were not significant, and the location of eating (school canteen vs. city office canteen) was borderline significant (aOR 0·77, 95% CI, 0·59–1·00, P=0·05). No major interactions or confounders were found.
Table 1. Norovirus outbreak at a school centre, Seinäjoki, Finland, March 2009, univariate analysis
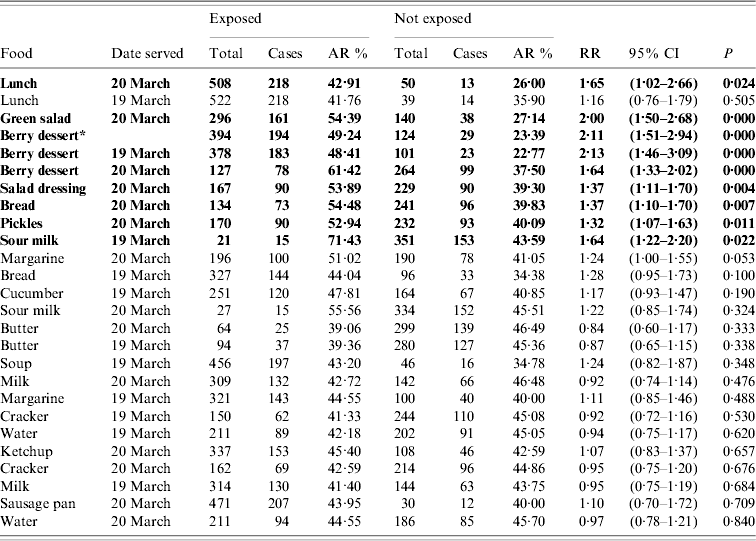
AR, Attack rate, RR, relative risk; CI, confidence interval.
The variables shown in bold were entered in the multivariate analysis.
* Data combined for 19 and 20 March: exposed=person who ate the berry dessert on either day or on both days; not exposed=person who did not eat the berry dessert on either day.
Laboratory and environmental investigations
Norovirus antigen test was positive in 9/10 stool samples. Five samples were sent for PCR confirmation, but two of them were destroyed during transportation. The three samples tested were PCR positive. Genotyping results showed norovirus genotype GII.b Hilversum/1999 in 2/3 samples; the quality of the third sample was not sufficient for successful typing.
The central kitchen inspected was found to be in good hygienic condition. The in-house control worked properly. Two of the nine kitchen employees had fallen ill on 20 March, one of them had left home after working only 1 h in the morning because of the symptoms. During her short shift she had handled only the warm meal (sausage pan) served that day. The green salad was prepared by combining ready-cut packed lettuce and tomatoes, which were washed and sliced on site. The frozen raspberries used for the berry dessert were of Polish origin and had not been heated before use. All the food samples collected tested negative for both bacterial pathogens and norovirus.
Review of the outbreak notifications and reports
The number of notifications received at THL almost doubled from 2007 to 2009 (Table 2). Moreover, the proportion of norovirus outbreaks of all notified outbreaks increased. Genogroup GII was the most common finding in each year. In addition to the large school outbreak described here, at least 12 point-source outbreaks with microbiological and epidemiological evidence of norovirus spread via unheated imported raspberries occurred between March and August 2009 in different parts of Finland (Table 3). About 900 people were affected in these outbreaks. The raspberries were of Polish origin in 12/13 outbreaks. The genotyping results of 11 outbreaks showed GII to have caused 10 and GI one of them. In the two outbreaks without genotyping results, the raspberries were traced back to a batch which had tested positive for norovirus GII during another outbreak investigation.
Table 2. Summary of all notifications regarding food- and waterborne outbreaks in Finland during 2007–2009 and characteristics of norovirus outbreaks among them
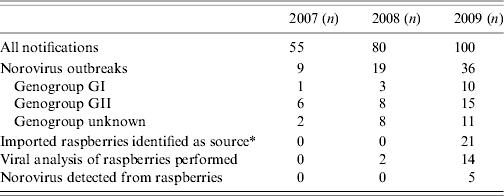
* Analytical study suggestive or virus detection from berries (or the same batch) positive.
Table 3. Norovirus (NoV) outbreaks linked to imported frozen raspberries during January–August 2009 in Finland
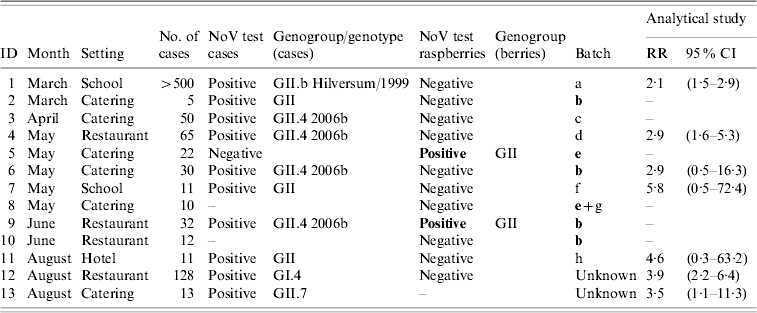
RR, Relative risk; CI, confidence interval; –, test/analysis not performed.
Raspberry batches with positive test for NoV shown in bold.
Investigations of these 13 outbreaks varied greatly. An analytical epidemiological study had been conducted in 7/13 outbreaks. All the seven studies showed an elevated RR for consumption of raspberries (Table 3). In addition to the epidemic curve consistent with a point-source outbreak and an incubation period fitting to norovirus infection, positive norovirus test from patients' stool samples was the crucial evidence in 10 outbreaks, a positive raspberry sample in one outbreak, and tracing back the batch of raspberries to one of the batches that had tested positive during another investigation in two outbreaks.
Control measures
Detection of norovirus in two samples of raspberries led to withdrawal of those batches (18 000 kg and 19 000 kg) from the market in May and June 2009. At the same time, the food handlers and the public were informed of the findings and advised to properly heat imported frozen raspberries before use. Evira also issued alerts regarding both positive batches through the Rapid Alert System for Food and Feed (RASFF) on 8 June and 3 July 2009 to inform other European Union countries.
DISCUSSION
Our report describes a large norovirus outbreak in a school associated with eating imported frozen raspberries. This association was supported by the shape of the epidemic curve which was consistent with a point-source outbreak: 88% of those affected fell ill within 48 h after the raspberry dessert had been served for the first time on 19 March. Norovirus was the only pathogen found in the stool samples of several affected persons, and the sequence analysis of two patient samples revealed the same genotype of norovirus in both suggesting a common source of infection. Norovirus analysis of the food samples remained negative; thus, no microbiological evidence was able to confirm the source of the outbreak. However, the analytical study suggested that raspberries and/or green salad were likely the source(s) of the outbreak. Frozen raspberries of Polish origin caused numerous other smaller norovirus outbreaks in Finland during the spring of 2009 (Table 3), and were therefore considered as the most likely source. Green salad could have been a plausible source as well; it is a freshly served food item, and it could have been contaminated by norovirus during farming, processing or serving. However, no observation other than the increased RR in the cohort study suggested that the salad could have been the vehicle for norovirus transmission. The kitchen worker who fell ill during the morning of 20 March did not handle the salad, and also the incubation period for the majority of the cases (symptom onset on 20 March) would have been ⩽12 h, as the salad was only served on 20 March. On the other hand, due to the fact that the kitchen basically had one choice for lunch on each day, most people who ate berry dessert also had salad. This link between the two exposures restricts the possibility of clarifying their roles in the outbreak by epidemiological means, and emphasizes the importance of microbiological investigations in this kind of situation.
In 2009, a total of 21 raspberry-linked outbreaks were found (Table 2). These outbreaks alone accounted for the increase in the number of notifications regarding food- and waterborne outbreaks in 2009, compared to the previous year. They also explained the increased proportion of norovirus outbreaks of all notified outbreaks. Genotype GII.4 was the most common finding from the raspberry-linked outbreaks detected in Finland in the spring of 2009. This genotype has previously been linked mostly to person-to-person transmission [Reference Verhoef23]. In one of the outbreaks in August, norovirus genotype GI.4 was found in patient samples. Even if the result of the viral investigation of the raspberries remained negative in this investigation, Polish raspberries originating from the same wholesaler tested positive for norovirus GI.4 in October, and also proved to have caused several raspberry-linked outbreaks later in the same year [Reference Maunula11].
Epidemiological investigation was restricted to descriptive epidemiology in half of the raspberry-linked outbreaks. This might be due to lack of resources or knowledge in the local offices primarily responsible for investigation of foodborne outbreaks. Microbiological investigations were more commonly used, but quite often virological testing of patient and food samples was missing. The cause of the outbreaks without virological test results would have been impossible to verify without linking the raspberry batch consumed to one of those that had tested positive during another outbreak investigation. Increasing the awareness of the local authorities regarding diagnostic methods available for virus detection in food samples and strengthening the cooperation between environmental and human healthcare locally could facilitate collecting human samples in a more timely manner. Thus, rapid communication at the local level is crucial for improving the microbiological part of outbreak investigations in the future. For strengthening the epidemiological side of investigations, training courses in outbreak investigation are provided and a helpdesk at THL for the local authorities is already in place. However, improving communication between the national and the local level regarding these tools could also be useful.
Detection of norovirus in raspberries has been described as being difficult due to, e.g. PCR inhibitors and a low pH [Reference Le Guyader6]. In our material, four samples of raspberries from a single batch were analysed during the investigations of four different outbreaks, but only one of these samples tested positive. This might be due to uneven distribution of contaminated berries within the large batch, a hypothesis that is supported by the fact that the berries of a single batch may come from different farms [Reference Falkenhorst8]. In case of the first positive raspberry sample we detected, the wholesaler tried to trace back the farmer of these berries and discovered that the batch originated from 62 different farms. The point of introduction of the viruses into the berries remained unclear in our investigations. Manually handled fruits and berries are at a great risk of viral contamination if there are insufficiencies regarding, e.g. quality of water for irrigation or worker hygiene during farming. Moreover, using sewage as a fertilizer is a risk for contamination. Frozen raspberries seem to have been an effective vehicle for norovirus transmission, probably due to resistance of norovirus to certain food-processing procedures, including freezing [Reference Butot24, Reference Butot, Putallaz and Sanchez25]. As no effective means of decontamination of viral pathogens for contaminated berries exists during the processing (freezing and packing), the importance of good agricultural practices and good handling practices should be emphasized, also during farming and harvesting [Reference Koopmans and Duizer26]. However, more information on the source of contamination is needed to target control procedures effectively, and further studies focusing on these issues are warranted.
Imported frozen raspberries served as a vehicle for norovirus transmission for several months in Finland despite the withdrawal of the contaminated batches and repeatedly informing the food handlers and the public to properly heat imported raspberries before use. Raspberries seem to have served as an effective vehicle of transmission for norovirus, which suggests that more attention should be paid to recommended good practices early in the production chain. Our findings suggest that insufficiencies in both epidemiological and microbiological investigations of foodborne outbreaks exist in Finland. These different aspects of investigation are, however, complementary to each other, and microbiological results can sometimes compensate for missing epidemiological data, and vice versa. Strengthening both sides of outbreak investigations, as well as ensuring timely communication between the different authorities, should be pursued in the future in order to detect and control such outbreaks more effectively.
ACKNOWLEDGEMENTS
The authors thank Mikko J. Virtanen for help with the statistical analysis.
DECLARATION OF INTEREST
None.








