Background
Nearly 50 million people worldwide live with dementia, a figure expected to reach 74.7 million by 2030 (Prince, Wimo, Guerchet, Wu, & Prina, Reference Prince, Wimo, Guerchet, Wu and Prina2015). Older adults with a dementia often have multiple chronic conditions that increase their need for 24-hour care (Prince, Comas-Herrera, Knapp, Guerchet, & Karagiannidou, Reference Prince, Comas-Herrera, Knapp, Guerchet and Karagiannidou2016; Wong, Gilmour, & Ramage-Morin, Reference Wong, Gilmour and Ramage-Morin2016). That care takes place largely in nursing homes and senior citizens’ residences, where over 400,000 Canadians live (Statistics Canada, 2016). Nursing home residents have complex health and social care needs (Estabrooks et al., Reference Estabrooks, Poss, Squires, Teare, Morgan, Stewart and Norton2013; Hirdes, Mitchell, Maxwell, & White, Reference Hirdes, Mitchell, Maxwell and White2011), a complexity that requires a sufficient and adequately trained workforce.
The largest workforce in the Canadian nursing home sector is care aides (also known as personal support workers, continuing care assistants, or resident assistants) (Statistics Canada, 2004). They provide 80 per cent or more of direct care to residents in nursing homes (Andersen, Reference Andersen2009; Berta, Laporte, Deber, Baumann, & Gamble, Reference Berta, Laporte, Deber, Baumann and Gamble2013; Hewko et al., Reference Hewko, Cooper, Huynh, Spiwek, Carleton, Reid and Cummings2015; Janes, Sidani, Cott, & Rappolt, Reference Janes, Sidani, Cott and Rappolt2008). Care aides are typically female, over the age of 40, and speak English as a second language (Health Employers Association of BC, 2014; Hewko et al., Reference Hewko, Cooper, Huynh, Spiwek, Carleton, Reid and Cummings2015). Despite providing most of the direct care to nursing home residents, they have the lowest level of education, they receive the lowest salary, and they have the least autonomy (Andersen, Reference Andersen2009; Caspar, Ratner, Phinney, & MacKinnon, Reference Caspar, Ratner, Phinney and MacKinnon2016). Care aides are not included in the Regulated Health Professions Act and therefore not accountable to or tracked by an external professional regulatory organization (Hewko et al., Reference Hewko, Cooper, Huynh, Spiwek, Carleton, Reid and Cummings2015; Kelly & Bourgeault, Reference Kelly and Bourgeault2015).
In 2015, the Translating Research in Elder Care (TREC) program of research published the first profile of Western Canadian care aides (Estabrooks, Squires, Carleton, Cummings, & Norton, Reference Estabrooks, Hoben, Poss, Chamberlain, Thompson, Silvius and Norton2015). In that report, we described the demographics and work-related outcomes of care aides in nursing homes and detailed the existing provincial care aide directories (Estabrooks, Squires, Carleton, et al., Reference Estabrooks, Hoben, Poss, Chamberlain, Thompson, Silvius and Norton2015). Because there are no national statistics with which to follow care aides in Canadian nursing homes, these directories are one way to track the number of care aides working in nursing homes (Kelly & Bourgeault, Reference Kelly and Bourgeault2015). Since our original publication in 2015, the number of provincial directories has fallen (Table 1). Currently only four provinces – compared to five in 2015 – have a care aide directory or registry. Ontario’s directory closed amid concerns around inadequate background checks (Zlomislic, Reference Zlomislic2016).
Table 1: Canadian provinces with a care aide registry

Note. a No = Alberta has a care aide “directory”. Alberta is currently transitioning from their previous directory system that included only Alberta Health Service (AHS) organizations and not the private for-profit or voluntary not-for-profit facilities. The previous directory is still collecting information; however, the new directory will be in partnership with Alberta Health and the College of Licensed Practical Nurses of Alberta (CLPNA). The new directory will remain voluntary and launched spring 2017. (Alberta Health Care Aide Directory; retrieved from http://www.albertahcadirectory.com/).
b No = There are no standard minimum education requirements; however, care aides must demonstrate they have the core competencies identified in the Government of Alberta Health Care Aide Competency Profile (2001) (Alberta Health: Health care aide provincial curriculum; retrieved from https://open.alberta.ca/publications/health-care-aides-competency-profile).
c Yes = Employers can verify if care aide is in the directory, but only if the care aide has listed them as their employer.
d Yes = To work in publicly funded organizations, care aides must register; privately funded organizations do not require registration (British Columbia [BC] Care Aide & Community Health Worker Registry; retrieved from https://www.cachwr.bc.ca/Registrants.aspx).
e Yes = Publicly funded organizations can view the registry. Private organizations can view the registry only if they have set up an account with the registry. (BC Care Aide & Community Health Worker Registry; retrieved from https://www.cachwr.bc.ca/Employers.aspx).
Only in British Columbia is enrolment in a registry mandatory, and then only for care aides who work in publicly funded organizations. All other provincial directories are voluntary. In 2016, Nova Scotia’s voluntary directory had 1,261 members, 35 per cent of whom worked in nursing homes (Continuing Care Assistant Program, 2016). Alberta’s re-established directory has approximately 300 care aides (T. Richter, personal communication, March 4, 2018). We were unable to assess the number of care aides currently enrolled in the Quebec directory. Beyond the four existing directories, no new provincial or territorial initiatives are emerging to systematically track or describe the care aide workforce. Without systematic tracking of care aides, it is nearly impossible to conduct the workforce planning that is needed to supply Canada’s growing and increasingly complex nursing home system (Berta et al., Reference Berta, Laporte, Deber, Baumann and Gamble2013). The need for long-term care will continue to grow across the country. If we do not act to implement rigorous documentation and planning for the long-term care workforce, we are jeopardizing the care of our most vulnerable citizens.
Because care aides have the most frequent contact with residents, they also have the most opportunity to monitor and influence care processes and the effects of care. However, there are no nationally recognized educational standards for care aides working in nursing homes (Association of Canadian Community Colleges, 2012). Care aide training varies between and within provinces (Association of Canadian Community Colleges, 2012). Individual provinces (e.g., British Columbia, Alberta) have introduced standardized curricula to define the core competencies required by care aides working in their province (Government of Alberta, 2001; Government of British Columbia, 2014). Examples of core competencies include communication, safety, positioning lifts and transfers, documentation and preparation of reports, and dementia care.
Nova Scotia and Ontario have distinct provincial curricula that must be followed by public and private educators who train care aides (Ministry of Training, Colleges and Universities, 2014; Nova Scotia Department of Health and Wellness, 2014).
Provincial variability in training may contribute to deficiencies in quality of care that are experienced by nursing home residents across the country (Hirdes et al., Reference Hirdes, Mitchell, Maxwell and White2011). Variability in quality of care should be the exception rather than the rule. It should not be aspirational to hope that Canadians receive the best quality of late-life and end-of-life care, regardless of their background or geographic location (Feldman & Estabrooks, Reference Feldman and Estabrooks2017).
Translating Research in Elder Care: A Longitudinal Program of Research in Western Nursing Homes
Systematically collecting data on care aide demographics, education, and work life is essential to tracking workforce characteristics that can signal issues of variability in quality care. TREC is a longitudinal health services research program examining the quality of work environments (organizational context), quality of care, quality of work life, and quality of end of life in nursing homes (Chamberlain et al., Reference Chamberlain, Gruneir, Hoben, Squires, Cummings and Estabrooks2017; Estabrooks, Hoben, et al., Reference Estabrooks, Hoben, Poss, Chamberlain, Thompson, Silvius and Norton2015; Estabrooks, Hutchinson, et al., Reference Estabrooks, Hutchinson, Squires, Birdsell, Cummings, Degner and Norton2009; Estabrooks, Squires, Cummings, Teare, & Norton, Reference Estabrooks, Hutchinson, Squires, Birdsell, Cummings, Degner and Norton2009). Since 2009 we have collected demographic, health, and work life data from care aides in nursing homes in the Western provinces. In 2009–2010, we collected 1,381 surveys from care aides in 30 urban nursing homes. This initial cohort included nursing homes from Alberta, Saskatchewan, and Manitoba and is known as TREC 1. Our partnered program of research requires provincial and regional health authority support. Saskatchewan did not participate in the recent nursing home data collection. Although we no longer collected data in Saskatchewan, we expanded our initial cohort of homes to 91 and by expanding to British Columbia, collected an additional 4,057 surveys from care aides in Alberta, Manitoba, and British Columbia. This is TREC 2. British Columbia is an essential addition to our Western province cohort because it has the second largest number of citizens aged 75 and older, and one-sixth of British Columbia’s population is over 65 years of age (Government of British Columbia, 2017; Statistics Canada, 2017).
We continue to collect information about care aide demographics and the work environment because they affect quality of care (Degenholtz, Castle Nicholas, & Rosen, Reference Degenholtz, Castle Nicholas and Rosen2006; Edvardsson et al., Reference Edvardsson, Sandman, Nay, Karlsson, Edvardsson, Sandman and Karlsson2008; Estabrooks, Hoben, et al., Reference Estabrooks, Hoben, Poss, Chamberlain, Thompson, Silvius and Norton2015; Hunter, Hadjistavropoulos, Thorpe, Lix, & Malloy, Reference Hunter, Hadjistavropoulos, Thorpe, Lix and Malloy2016; Jenkins & Allen, Reference Jenkins and Allen1998; Schmidt, Dichter, Bartholomeyczik, & Hasselhorn, Reference Schmidt, Dichter, Bartholomeyczik and Hasselhorn2014; Spence Laschinger, Shamian, & Thomson, Reference Spence Laschinger, Shamian and Thomson2001; Zúñiga et al., Reference Zúñiga, Ausserhofer, Hamers, Engberg, Simon and Schwendimann2015). Here we describe the care aides in our expanded cohort of 91 nursing homes and identify trends in their demographics, health, and work life in our cohort of 18 nursing homes that took part in both TREC 1 and TREC 2.
Methods
TREC nursing homes also participate in a longitudinal observational study that generates measures at the resident, staff, unit, and facility levels (Estabrooks et al., Reference Estabrooks, Morgan, Squires, Bostrom, Slaughter, Cummings and Norton2011). From 2014 to 2015, we collected 4,057 surveys from care aides in the 91 participating nursing homes in British Columbia, Alberta, and Manitoba. In this article, we examine data collected from care aides and data collected on nursing home size, owner-operator model, and health region. Additionally, we use three descriptors to identify the three cohorts:
1. The “initial” cohort is the 30 nursing homes in TREC that participated in Phase 1 of the program.
2. The “expanded” cohort refers only to the 91 facilities in TREC 2.
3. The “stable” cohort is the 18 nursing homes that are common to TREC 1 and TREC 2. This cohort is our longitudinal cohort of nursing homes.
The expanded cohort includes facilities that were in TREC 1 as well as additional facilities that were not in TREC 1. Our data collection methods and sampling were consistent from TREC 1 to TREC 2.
Sampling
We selected nursing homes using stratified (facility bed size, owner-operator model, health region) random sampling of urban facilities in British Columbia, Alberta, and Manitoba. Alberta is governed by one health authority, Alberta Health Services, and is divided into five health zones. Our sample of nursing homes is drawn from the Edmonton, Calgary, and Central zones. For this article, we refer to nursing homes from all three Alberta health zones as “Alberta” because they are governed by one health authority.
British Columbia has five health regions that function as separate health authorities and two are part of TREC: Interior Health and Fraser Health. Due to the separate governance structure in British Columbia, we examined Interior Health and Fraser Health separately. All sampled Manitoba facilities are located in the Winnipeg Regional Health Authority. We refer to all Manitoba facilities as “Winnipeg” for the purposes of this article.
Care aides completed self-report structured surveys using computer-assisted personal interviews (Squires et al., Reference Squires, Hutchinson, Bostrom, Deis, Norton, Cummings and Estabrooks2012). Care aides were eligible to complete the survey if they (a) had been working in the facility for more than three months, (b) could identify a unit they worked on at least 50% of the time, and (c) worked at least six shifts a month on the unit.
Measures
The care aide survey is designed to measure care aide demographics, organizational context, work life, mental and physical health, and use of best practices (Chamberlain, Hoben, Squires, & Estabrooks, Reference Chamberlain, Hoben, Squires and Estabrooks2016; Estabrooks, Squires, Hayduk, et al., Reference Estabrooks, Hoben, Poss, Chamberlain, Thompson, Silvius and Norton2015; Hoben, Knopp-Sihota, et al., Reference Hoben, Knopp-Sihota, Nesari, Chamberlain, Squires, Norton and Estabrooks2017).
Care Aide Demographics
Demographic information includes care aide sex, age, education (high school certificate, care aide certificate), first language (English, Filipino, Tagalog, other), and shift worked most of the time (day, evening, night).
Care Aide Work Life
We assessed care aide job satisfaction with the Michigan Organizational Assessment Questionnaire Job Satisfaction Subscale (MOAQ-JSS-3), a measure of job satisfaction that demonstrates scale scores that are reliable and valid (Ginsburg et al., Reference Ginsburg, Berta, Baumbusch, Rohit Dass, Laporte, Reid and Taylor2016; Schleicher, Hansen, & Fox, Reference Schleicher, Hansen, Fox and Zedeck2010). The three items were each measured on a 5-point Likert scale (1 = strongly disagree to 5 = strongly agree). We derived the overall score for job satisfaction by averaging the three scale items.
We measured care aide burnout with the Maslach Burnout Inventory (MBI) 9-item Short Form. The short form MBI has three subscales of three items each, scored from 0 to 6, that measure emotional exhaustion, cynicism, and professional efficacy (Maslach & Jackson, Reference Maslach and Jackson1981, Reference Maslach, Jackson and Oskamp1984; Maslach, Schaufeli, & Leiter, Reference Maslach, Schaufeli and Leiter2001). Burnout is characterized by high emotional exhaustion, high cynicism, and low professional efficacy.
We assessed whether care aides experienced dementia-related responsive behaviours from residents. Care aides responded to six questions, indicating yes or no if in the last five shifts they had experienced yelling or screaming, hurtful remarks or behaviours, spitting/biting/pinching/pushing, unwanted comments or actions of a sexual nature, sexual touching, or verbal threats from residents. The score was calculated as the sum of the six binary items. We included dementia-related responsive behaviours under the umbrella of care aide work life because it reflects an experience on the unit or facility environment in which care aides work (as opposed to a demographic characteristic or educational achievement). Our previous research has found that care aides who experience a higher frequency of dementia-related responsive behaviours exhibit higher emotional exhaustion and cynicism (Chamberlain et al., Reference Chamberlain, Gruneir, Hoben, Squires, Cummings and Estabrooks2017).
Care Aide Mental and Physical Health
We assessed care aide health status with the 8-Item Short Form Survey (SF-8), a measure of mental and physical health (Ware, Kosinski, Dewey, & Gandek, Reference Ware, Kosinski, Dewey and Gandek2001). The SF-8 consists of eight items that are scored on a 5- or 6-point Likert scale (depending on the item). We generated physical and mental health summary scores, using a proprietary algorithm obtained with permission from the scale developers. SF-8 summary scores have a possible range of 0 (worst possible health) to 100 (best possible health).
Nursing Home Characteristics
We collected data on facility size and owner-operator model in a survey completed by the nursing home director of care or their equivalent. Facilities were classified by number of beds as small (35–79 beds), medium (80–120 beds), or large (> 120 beds). Owner-operator model was classified as public not-for-profit, voluntary not-for-profit (e.g., faith based), or private for-profit.
Ethics
We obtained ethics approvals from research ethics boards at all universities of participating investigators (University of Alberta, Pro00037937; University of British Columbia, H14-00942; University of Manitoba, H2015:164). Regional health authority and operational approvals were obtained from all necessary regional authorities and nursing homes.
Analysis
We calculated descriptive statistics (mean, standard deviation) for all variables. To assess regional differences in the expanded (n = 91) facility cohort, we conducted one-way analysis of variance (ANOVA) and chi-squared tests of difference with a post-hoc test (Bonferroni correction). To assess regional, owner-operator, and facility-size differences, we conducted a one-way ANOVA and reported the p-value and effect sizes using Cohen’s f 2.
Analysing the Stable Cohort of 18 Nursing Homes
We have a stable cohort of 18 nursing homes that participated in TREC 1 (2009–2010) and TREC 2 (2014–2015). We assessed differences between care aide demographics, health status, and work life in these 18 facilities using two separate tests of significance. Our stable cohort includes facilities from Alberta and Winnipeg only. We examined differences between TREC 1 and TREC 2 in Alberta and Winnipeg using independent sample t-tests and chi-squared tests of difference.
We could not determine which individual care aides in TREC 1 also completed the survey in TREC 2. However, we expected substantial dependence in care aide responses in the stable cohort, given that the average work tenure of care aides exceeded the time between data collection waves. We used a linear mixed model analysis to assess the differences in care aide demographics and work life. We generated a variable to indicate if the facility had been in the stable cohort. We used this variable as a fixed effect and assessed differences in care aide demographics and work life. We used a linear mixed model in addition to t-tests and chi-square tests of difference because this analysis method controls for non-independent observations. In general, values generated from a linear mixed model are the most conservative test of significance and demonstrate the statistically significant differences between the samples, given dependence (Krueger & Tian, Reference Krueger and Tian2004; Singer, Reference Singer1998). We calculated p-values from the linear mixed model.
Sensitivity Analysis
Although we had 18 facilities in our stable cohort, there were facilities that participated in our initial cohort TREC 1 that did not participate in TREC 2. We aimed to assess the potential differences between facilities that remained in the stable cohort and those that were not in the stable cohort. We conducted a sensitivity analysis to (1) assess statistically significant differences between facilities in the stable cohort and facilities that were only in TREC 1; (2) assess statistically significant differences between facilities in the stable cohort and facilities that were only in TREC 2. We only assessed facilities from TREC 1 that were located in Alberta and Winnipeg; we did not include facilities from Saskatchewan. For the sensitivity analysis, we used chi-squared tests for categorical variables and one-way ANOVA’s for continuous variables (results in Supplementary Files, Tables 10–13). We reported the p-value for the chi-squared and ANOVA’s.
Results
Demographic Characteristics of the Expanded 91-facility TREC 2 (2014–2015) Care Aide Cohort
We surveyed 4,057 care aides from 91 nursing homes in British Columbia, Alberta, and Winnipeg (Table 2), from September 2014 through May 2015. We had a 69 per cent care aide survey response rate. We calculated the response rate by dividing the number of surveys completed by the number of care aides who were eligible to complete the survey during the data collection period. Most care aides surveyed were female (89.7%), 40 years of age or older (67%), and spoke English as a second language (60.6%). Almost 30% worked at two or more nursing homes, and 92.9% held a care aide certificate.
Table 2: Expanded cohort: TREC 2 (2014-2015) care aide demographic characteristics by region
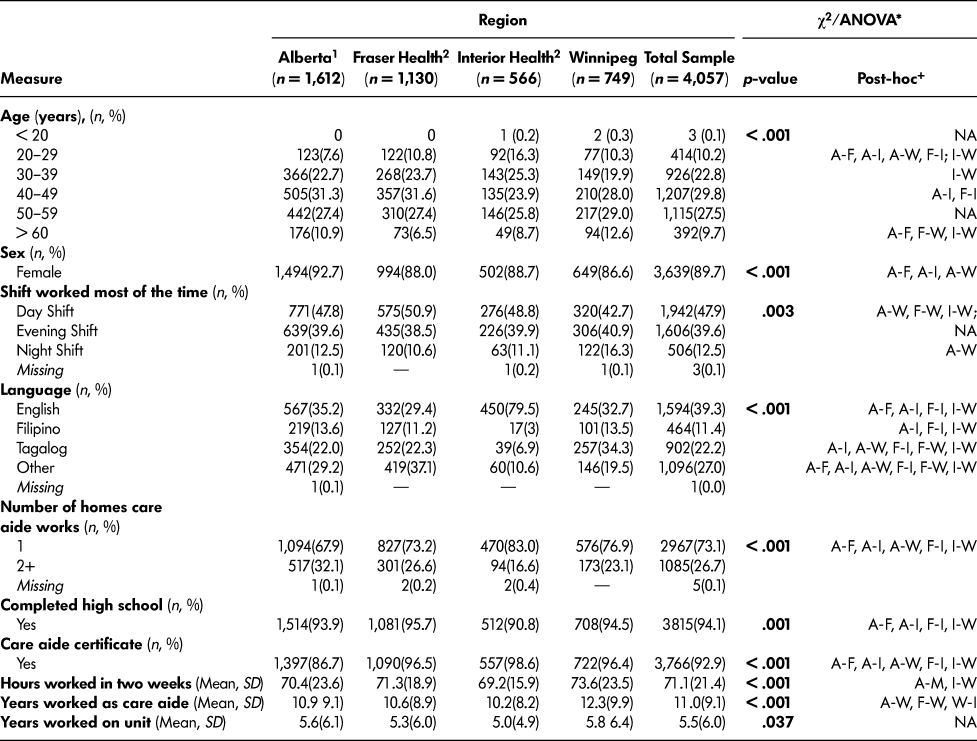
Note. TREC = Translating Research in Elder Care. * χ2 test used for categorical variables and one-way ANOVA for continuous variables.
+ Post-hoc tests for significant difference were examined using Bonferroni correction for continuous variables and binary or multinomial logistic regression for categorical outcomes. A, F, I, M denote the post-hoc test for multiple comparisons between the regions (A = Alberta, F = Fraser Health, I = Interior Health, W = Winnipeg). Significant differences are provided between the regions (e.g., A–F implies a significant difference between Alberta and Fraser Health). NA denotes not applicable.
1 = Alberta is reported as one region. Facilities from Alberta were primarily located in Edmonton and Calgary. We chose to report it as one region due to its singular regional health authority governance structure.
2 = Interior Health and Fraser Health are separately functioning health authorities in British Columbia. We report these are two separate regions due to their separate funding and operating structure.
We observed statistically significant regional differences in care aide demographic characteristics. Care aides in Winnipeg region had worked more years as a care aide than those in all other regions (Alberta, Fraser Health, Interior Health) and worked more hours in the last two weeks than in Alberta and Interior Health. Care aides in Interior Health were significantly different statistically in reported first language than aides in all other regions – nearly 80 per cent spoke English as their first language compared to 29 per cent in Fraser Health, 32 per cent in Winnipeg, and 35 per cent in Alberta.
Health Status and Work-related Outcomes in the Expanded 91-facility TREC 2 Care Aide Cohort
Care aide quality of work life and health status differed significantly by region (Table 3). We found medium differences in effect size, as determined by Cohen’s f 2, in care aide burnout, specifically emotional exhaustion and cynicism. Winnipeg region care aides reported the highest emotional exhaustion and cynicism (higher is worse) and the lowest professional efficacy (lower is worse). We found a number of statistically significant differences among health regions in professional efficacy and job satisfaction but the effect sizes were small, indicating questionable clinical significance.
Table 3: Expanded cohort: Comparison of work-related and health outcomes among care aides by region in TREC 2 (2014–2015)
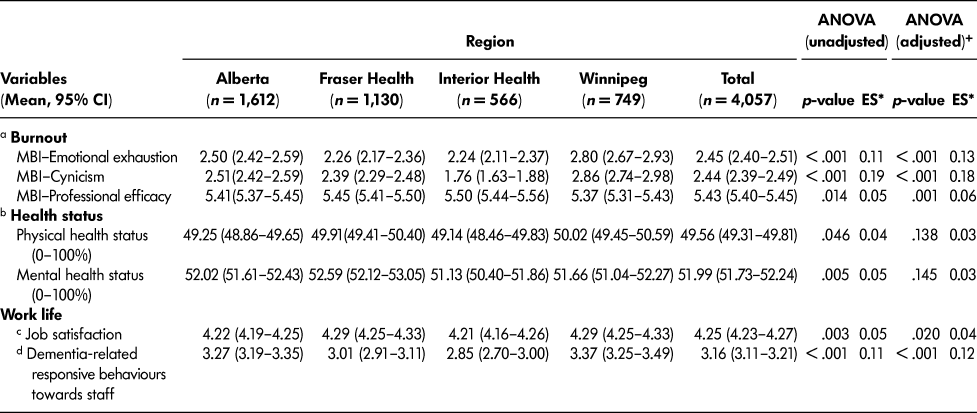
Note. ES = effect size; MBI = Maslach Burnout Inventory; TREC = Translating Research in Elder Care. 95% CI: lower and upper confidence interval.
a Emotional exhaustion, cynicism, and professional efficacy were measured using the Maslach Burnout Inventory. Each scale included three items and their scoring was derived by taking the average of the three items. The items were measured on a 7-point (0–6) Likert scale (0 = never to 6 = daily). Higher scores on emotional exhaustion and cynicism indicate more burnout, and higher scores on professional inefficacy indicate lower burnout. We calculated Cronbach’s alpha for each burnout subscale, emotional exhaustion (α = 0.755), cynicism (α = 0.649), and efficacy (α = 0.471).
b Physical and mental health were measured using the Health Status Short Form (SF-8). Responses are on a 5- or 6-point scale, and scoring is completed using a proprietary algorithm obtained when permission to use the scale is granted. Higher scores indicate better perceived health status.
c Job satisfaction was measured by asking care aides to indicate their agreement with three items measuring their satisfaction with their job, liking their work, and liking working in the facility. The overall score for job satisfaction was derived by taking the average of the three items. The three items were measured on a 5-point Likert scale (1 = strongly disagree to 5 = strongly agree). Cronbach’s alpha for the job satisfaction scale was (α = 0.810).
d Dementia-related responsive behaviours towards staff was measured by asking care aides to indicate if they have or have not (Yes/No) experienced instances of resident responsive behaviours (yelling or screaming, hurtful remarks or behaviours, spitting/biting/pinching/pushing, unwanted comments or actions of a sexual nature, sexual touching, verbal threats) in their last five shifts. The score for responsive behaviours is derived by taking the sum of the six items.
* Effect size (Cohen’s f 2): small effect = 0.02, medium effect = 0.15, large effect = 0.35.
+ Region effect after adjusting for sex, care aide certificate, and English as a first language.
We found several statistically significant differences in care aide demographics by owner-operator model (Table 4). A higher proportion of care aides working in public not-for-profit facilities spoke English as their first language (46.5%) than care aides in private for-profit (34.5%) or voluntary not-for-profit facilities (42.1%). Private for-profit facilities had the largest proportion of care aides who spoke either Filipino or Tagalog as their first language (38.6%).
Table 4: Expanded cohort: TREC 2 (2014-2015) care aide demographic characteristics by owner-operator model
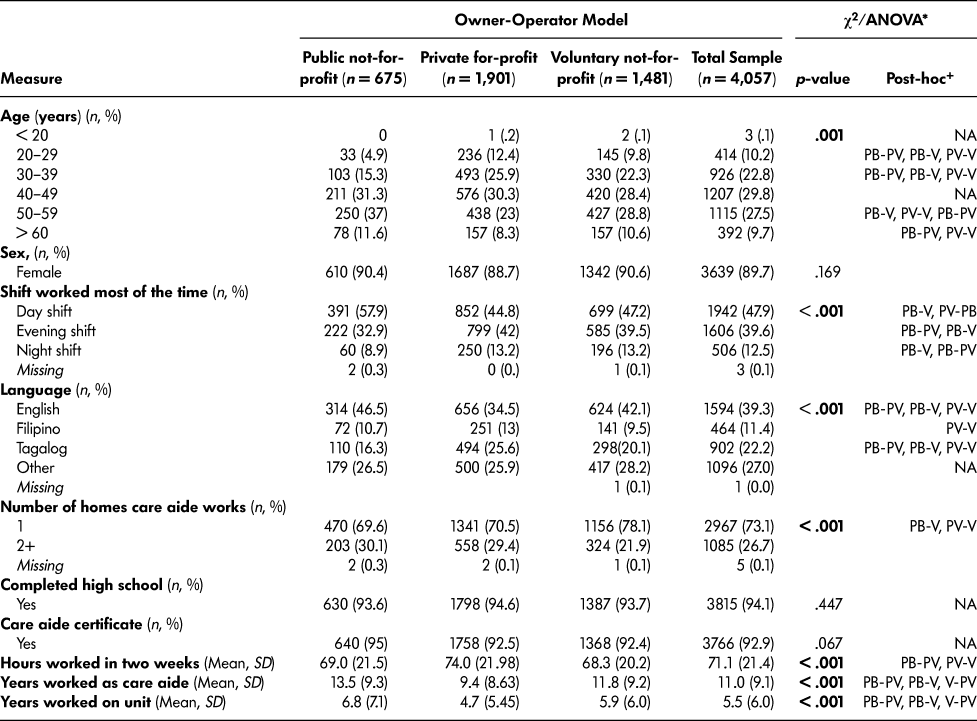
Note. TREC = Translating Research in Elder Care. * χ2 test used for categorical variables and one-way ANOVA for continuous variables.
+ Post-hoc tests for significant difference were examined using Bonferroni correction for continuous variables and binary or multinomial logistic regression for categorical outcomes. PB, PV, V denote the post-hoc test for multiple comparisons between the regions (PB = Public not for profit, PV = Private for profit, V = Voluntary not for profit). Significant differences are provided between the regions (e.g., PB-PV implies a significant difference between Public and Private). NA denotes not applicable.
Voluntary not-for-profit facilities had a statistically higher proportion of care aides working in only one facility (78.1%) than public not-for-profit (69.6%) and private for-profit facilities (70.5%). Care aides working in public not-for-profit facilities had on average worked more years as a care aide than those in private for-profit and voluntary not-for-profit facilities. Care aides working in private for-profit facilities had worked significantly more hours in the last two weeks than those in not-for-profit facilities.
We found statistically significant differences in measures of work life for care aides (emotional exhaustion, job satisfaction, experience of dementia-related responsive behaviours) and health status (physical, mental) across owner-operator models (Table 5). However, the effect sizes are small.
Table 5: Expanded cohort: TREC 2 (2014-2015) comparison of work related and health outcomes among care aides by owner-operator
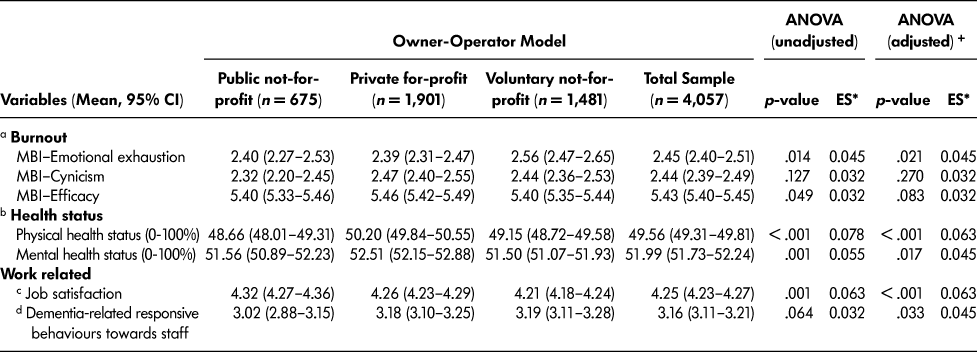
Note. ES = effect size; MBI = Maslach Burnout Inventory; TREC = Translating Research in Elder Care. 95% CI: lower and upper confidence interval.
a Emotional exhaustion, cynicism, and professional efficacy were measured using the Maslach Burnout Inventory. Each scale included three items, and their scoring was derived by taking the average of the three items. The items were measured on a 7-point (0–6) Likert scale (0 = never to 6 = daily). Higher scores on emotional exhaustion and cynicism indicate more burnout, and higher scores on professional inefficacy indicate lower burnout.
b Physical and mental health were measured using the Health Status Short Form (SF-8). Responses are on a 5- or 6-point scale, and scoring is completed using a proprietary algorithm obtained when permission to use the scale is granted. Higher scores indicate better perceived health status.
c Job satisfaction was measured by asking care aides to indicate their agreement with three items measuring their satisfaction with their job, liking their work, and liking working in the facility. The overall score for job satisfaction was derived by taking the average of the three items. The three items were measured on a 5-point Likert scale (1 = strongly disagree to 5 = strongly agree).
d Dementia-related responsive behaviours towards staff was measured by asking care aides to indicate if they have or have not (Yes/No) experienced instances of resident-responsive behaviours (yelling or screaming, hurtful remarks or behaviours, spitting/biting/pinching/pushing, unwanted comments or actions of a sexual nature, sexual touching, verbal threats) in their last five shifts. The score for responsive behaviours is derived by taking the sum of the six items.
* Effect size (Cohen’s f 2): small effect = 0.02, medium effect = 0.15, large effect = 0.35.
+ Owner-operator model effect after adjusting for sex, care aide certificate, and English as a first language.
In addition to differences by region and owner-operator model, we examined differences in care aide demographics and work life by facility size (small, 35–79 beds; medium 80–120 beds; large > 120 beds) (Supplementary Files, Tables 8 and 9). A higher proportion of care aides who worked in small facilities spoke English as their first language (50.5%) than did those in medium (42.9%) or large facilities (34.7%). Medium-size facilities had a higher proportion of care aides with a care aide certificate (96.2%) than in small (91.9%) or large facilities (91.3%). We found statistically significant differences in reported rates of experiencing dementia-related responsive behaviours across facilities of different sizes, but these differences had only small effect sizes.
TREC 1 and TREC 2: Comparing Care Aide Demographics in the Stable Cohort
We examined survey responses from the stable cohort of 18 facilities in Alberta and Winnipeg that have remained in the TREC cohort since 2009 (Table 6), and have found no statistically significant differences in their care aide age, sex, or first language between TREC 1 and TREC 2. A significantly higher percentage of care aides in Winnipeg held a care aide certificate in TREC 2 (98.3%) than in TREC 1 (93.8%). Care aides in Alberta had worked significantly more hours in the last two weeks (69.7%) in TREC 2 than in TREC 1 (61%). We found no statistically significant differences in the years worked as a care aide or years worked on the unit in Alberta or Winnipeg.
Table 6: Stable cohort: Comparison of care aide demographic characteristics among the care aides in the 18 facilities that are common to both TREC 1 (2009-2010) and TREC 2 (2014-2015)
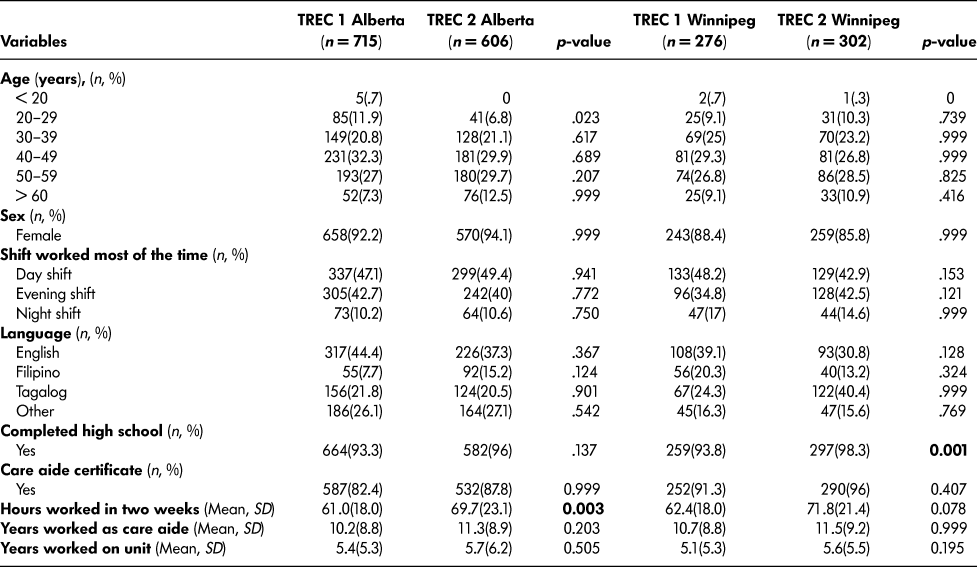
Note. TREC = Translating Research in Elder Care.
TREC 1 and TREC 2: Comparing Care Aide Work Life in the Stable Cohort
Care aides from Winnipeg in TREC 2 had significantly higher cynicism (M = 2.87) than in TREC 1 (M = 2.44) (Table 7). Care aides in Alberta also had higher cynicism in TREC 2 (M = 2.46) than in TREC 1 (M = 2.09), but the difference is not statistically significant. Professional efficacy was higher in Winnipeg facilities in TREC 2 (M = 5.37) than in TREC 1 (M = 5.17), but the difference is not statistically significant in mixed models. Emotional exhaustion, professional efficacy, and experiencing dementia-related responsive behaviours increased in Alberta and Winnipeg from TREC 1 to TREC 2. We found no differences in care aide physical health, mental health, or job satisfaction in Alberta or Winnipeg.
Table 7: Stable cohort: Comparison of care aide work life and health outcomes in TREC 1 (2009-2010) and TREC 2 (2014-2015) longitudinal cohort (n = 18 facilities)
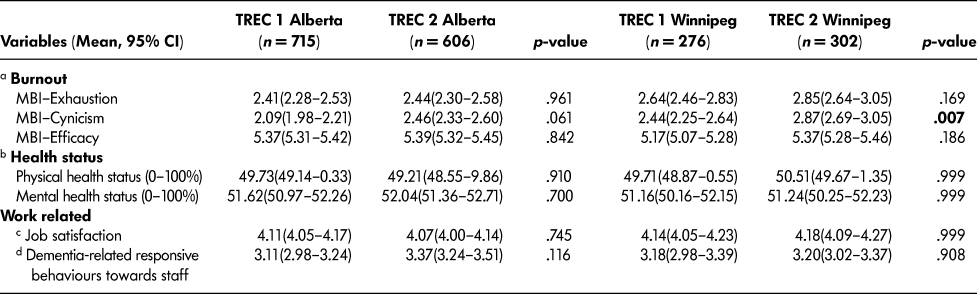
Note. ES = effect size; MBI = Maslach Burnout Inventory; TREC = Translating Research in Elder Care. 95% CI: lower and upper confidence interval.
a Emotional exhaustion, cynicism, and professional efficacy were measured using the Maslach Burnout Inventory. Each scale included three items and their scoring was derived by taking the average of the three items. The items were measured on a 7-point (0–6) Likert scale (0 = never to 6 = daily). Higher scores on emotional exhaustion and cynicism indicate more burnout, and higher scores on professional inefficacy indicate lower burnout.
b Physical and mental health were measured using the Health Status Short Form (SF-8). Responses are on a 5- or 6-point scale, and scoring is completed using a proprietary algorithm obtained when permission to use the scale is granted. Higher scores indicate better perceived health status.
c Job satisfaction was measured by asking care aides to indicate their agreement with one item measuring their satisfaction with their job. The item was measured on a 5-point Likert scale (1 = strongly disagree to 5 = strongly agree). TREC 1 included a single-item measure of overall job satisfaction, compared to TREC 2 which included the single item, and two additional items that could be averaged to a scale (reported in Tables 3 and 5). To allow for comparisons between TREC 1 and TREC 2, we compared only the single item measure of job satisfaction in the 18 homes common to both periods of data collection.
d Dementia-related responsive behaviours towards staff was measured by asking care aides to indicate if they have or have not (Yes/No) experienced instances of resident responsive behaviours (yelling or screaming, hurtful remarks or behaviours, spitting/biting/pinching/pushing, unwanted comments or actions of a sexual nature, sexual touching, verbal threats) in their last five shifts. The score for responsive behaviours is derived by taking the sum of the six items.
We conducted a sensitivity analysis to examine the potential differences in those facilities that participated in TREC 1 and TREC 2 (Supplementary Files, Tables 10-13). For Alberta facilities that participated only in TREC 1, we found no statistically significant differences in care aide demographics (sex, age, shift worked most of the time) compared to our stable cohort. For facilities that participated only in TREC 2, we found some differences in care aide demographics (e.g., completed high school) and quality of work life (e.g., job satisfaction, dementia-related responsive behaviours) compared to our stable cohort.
Discussion
We report here both new and expanded data on characteristics of care aides in Canadian nursing homes and, perhaps of greater importance, broader trends in care aide demographics and work life in a stable cohort of nursing homes. Trends are from the stable cohort of 18 nursing home facilities in Alberta and Winnipeg that have participated in TREC since its inception.
Longitudinal Trends: Care Aide Demographics in Stable 18-Facility Cohort
In the stable cohort of 18 facilities, we found no statistically significant differences in care aide age, sex, or first language. Most care aides in Alberta and Winnipeg are female, older, and speak English as an additional language, which is consistent with the literature on unregulated health care workers (Institute of Medicine, 2008; Khatutsky, Wiener, & Anderson, Reference Khatutsky, Wiener and Anderson2010; Stone & Wiener, Reference Stone and Wiener2001). Five years after our first wave of data collection, we found that care aides in Alberta worked significantly more hours.
Longitudinal Trends: Care Aide Work Life in Stable 18-Facility Cohort
In the stable cohort of 18 facilities, we found no statistically significant differences (positive or negative) in care aide physical health, mental health, job satisfaction, or experience of dementia-related responsive behaviours. Care aides in Alberta had no change in their reported emotional exhaustion, cynicism, or professional efficacy. However, care aides in Winnipeg reported statistically significant increases in cynicism. These results suggest that quality of work life for care aides has not improved. On some dimensions (e.g., higher cynicism), their work life has worsened. This is troubling given the rapidly rising demands for nursing home staff (Fujisawa & Colombo, Reference Fujisawa and Colombo2009; Institute of Medicine, 2008). Estabrooks, Squires, Carleton, et al. (2015) in their first profile of Western Canadian care aides, raised care aide burnout as a significant and troubling finding. Because care aide burnout has an important impact on staff health and resident care, we must systematically attend to it (Bakker, Demerouti, & Sanz-Vergel, Reference Bakker, Demerouti and Sanz-Vergel2014; de Rooij, Luijkx, Declercq, Emmerink, & Schols, Reference de Rooij, Luijkx, Declercq, Emmerink and Schols2012; Jenkins & Allen, Reference Jenkins and Allen1998).
Without major changes in staffing and resident acuity on the horizon, we must look to innovative ways to reduce care aide burnout. Research suggests that improving the organizational context (work environment) could improve staff work life and resident care (Chamberlain et al., Reference Chamberlain, Gruneir, Hoben, Squires, Cummings and Estabrooks2017; Chamberlain et al., Reference Chamberlain, Hoben, Squires and Estabrooks2016; Estabrooks, Hoben, et al., Reference Estabrooks, Hoben, Poss, Chamberlain, Thompson, Silvius and Norton2015). Our future research will examine these data to assess care aide, unit (i.e., organizational context), and facility level predictors of care aide work life in the expanded cohort. Care aides interact with residents more frequently than any other care providers and are an untapped resource for care aide–led quality improvement initiatives in nursing homes. Interventions to improve elements of the organizational context, such as involving care aides in formal meetings about resident care (Hoben, Norton, et al., Reference Hoben, Knopp-Sihota, Nesari, Chamberlain, Squires, Norton and Estabrooks2017) and having them lead quality improvement initiatives (Cranley et al., Reference Cranley, Hoben, Yeung, Estabrooks, Norton and Wagg2018; Cranley et al., Reference Cranley, Norton, Cummings, Barnard, Batra-Garga and Estabrooks2012; Cranley, Norton, Cummings, Barnard, & Estabrooks, Reference Cranley, Norton, Cummings, Barnard and Estabrooks2011), have the potential to improve staff work life.
From TREC 1 to TREC 2 a higher percentage of care aides in Winnipeg reported holding a care aide certificate. This could be attributed to the fact that older care aides who did not have a certificate have retired, and organizations hiring care aides now require a certificate. Although we might expect better training to decrease burnout, we did not find an association between care aides’ training and their job satisfaction or burnout (Chamberlain et al., Reference Chamberlain, Gruneir, Hoben, Squires, Cummings and Estabrooks2017; Chamberlain et al., Reference Chamberlain, Hoben, Squires and Estabrooks2016). A relationship has yet to be established between care aide education and quality of work life, but research with registered nurses indicates that education level and opportunities for continuing education have a positive impact on quality of work life (e.g., job satisfaction) (Nowrouzi et al., Reference Nowrouzi, Giddens, Gohar, Schoenenberger, Bautista and Casole2016). A relationship also has yet to be established between level of care aide education and quality of care. However, a review by Hoben, Clarke, et al. (2017) found that lack of education and training – especially with respect to residents with dementia-related responsive behaviours – is one of the highest and most prevalent barriers to providing residents with oral health care. This suggests that insufficient training may negatively affect quality of care. Further research is needed with care aides to critically examine their educational opportunities and how those opportunities affect quality of work life and quality of care.
Resident social and health needs continue to be complex, with that complexity rising. Residents routinely enter nursing homes with multiple chronic conditions and in later stages of dementia with accompanying heavy care needs that can contribute to care aide burnout (Chamberlain et al., Reference Chamberlain, Gruneir, Hoben, Squires, Cummings and Estabrooks2017; Estabrooks et al., Reference Estabrooks, Poss, Squires, Teare, Morgan, Stewart and Norton2013; Marventano et al., Reference Marventano, Ayala, Gonzalez, Rodríguez-Blázquez, Garcia-Gutierrez and Forjaz2016; Schüssler & Lohrmann, Reference Schüssler and Lohrmann2015). Alberta, British Columbia, and Manitoba have all implemented policies, in response to increased demand for nursing home beds and changes in resident acuity, to increase the number and availability of less intensive care settings (home care or assisted living) (Alberta Health and Wellness, 2000, 2008; Cohen, Murphy, Nutland, & Ostry, Reference Cohen, Murphy, Nutland and Ostry2005; Manitoba Health, 2006). As a consequence, residents enter nursing homes at even later and more complex stages of their care trajectories (Hogan et al., Reference Hogan, Amuah, Strain, Wodchis, Soo, Eliasziw and Maxwell2014; Hollander, Miller, MacAdam, Chappell, & Pedlar, Reference Hollander, Miller, MacAdam, Chappell and Pedlar2009). Despite increasing resident complexity, there are still no national standards on minimum staffing requirements, and funding has not kept pace with resident complexity (McGregor et al., Reference McGregor, Tate, Ronald, McGrail, Cox, Berta and Broemeling2010).
Our future work will examine resident data, using routinely collected resident assessment (RAI-MDS, 2.0) data to examine regional differences in resident complexity and the links between facility characteristics (e.g., ownership model, bed size), organizational context (e.g., leadership, culture, feedback [evaluation]), and resident outcomes.
Care Aide Demographics and Work Life in Expanded 91-Facility Cohort
We found significant regional variation in care aide demographics and work life in our expanded cohort of 91 facilities. Most care aides in Interior Health do speak English as their first language in contrast to the other health regions (Fraser Health, Alberta, Winnipeg). Research indicates that the majority of the care aide population speaks English as a second language (Hewko et al., Reference Hewko, Cooper, Huynh, Spiwek, Carleton, Reid and Cummings2015; Khatutsky et al., Reference Khatutsky, Wiener and Anderson2010; Stone & Wiener, Reference Stone and Wiener2001). The high proportion of English speakers in Interior Health most likely reflects the regional demography of primarily English-speaking Caucasians (Statistics Canada, 2012).
Care aides with the Winnipeg Regional Health Authority had the highest reported emotional exhaustion and cynicism (higher is worse) and the lowest reported professional efficacy (lower is worse) of all our study regions. A regression analysis examining predictors of care aide burnout is beyond the scope of this article. Our previous research with the initial TREC 1 cohort found that care aide age is negatively associated with care aide cynicism (i.e., every one-year increase in age resulted in a decrease in care aide cynicism) (Chamberlain et al., Reference Chamberlain, Gruneir, Hoben, Squires, Cummings and Estabrooks2017). However, our future research will assess predictors of care aide burnout. Care aides in Winnipeg had worked the highest number of years compared to all of the other health regions. The associations between care aide age or tenure in position and increased risk of burnout are inconsistent (Cooper et al., Reference Cooper, Carleton, Chamberlain, Cummings, Bambrick and Estabrooks2016). Our future research will aim to more thoroughly assess the predictors of burnout across the three Western provinces in the expanded cohort.
The regional variation in emotional exhaustion and cynicism could also be attributed to differences in residential care systems. Estabrooks et al. (Reference Estabrooks, Poss, Squires, Teare, Morgan, Stewart and Norton2013) examined health and functional status of nursing home residents and found that, compared to Alberta, Manitoba residents were older and a higher proportion had a dementia. We did not examine resident data, but we hypothesize that increased resident care needs could contribute to the observed differences in care aide emotional exhaustion and cynicism (Chamberlain et al., Reference Chamberlain, Gruneir, Hoben, Squires, Cummings and Estabrooks2017). In a previous study, we found that public not-for-profit facilities tended to have residents with higher cognitive impairment and dementia-related responsive behaviours (Estabrooks et al., Reference Estabrooks, Poss, Squires, Teare, Morgan, Stewart and Norton2013). Canada’s nursing home system is regulated by provinces and territories, leading to jurisdictional differences in services, coverage of costs, level and type of care offered, and ownership/governance of facilities (Government of Canada, 2004). These jurisdictional differences may lead to different organizational context conditions, which in turn may differently affect quality of care aides’ work life (e.g., burnout). However, more research is needed on how differences in nursing home policies among Canadian health regions lead to regional differences in care aides’ work life.
Strengths and Limitations
Strengths of this study include the large sample size of 4,057 care aides in our cohort of 91 randomly selected nursing homes. Our longitudinal cohort included a sample size of 1,899 care aides from 18 nursing homes. We used robust and conservative statistical methods to examine the potential dependency between the TREC 1 and TREC 2 care aide cohorts. Limitations of our study analysis include our inability to link responses of care aides who took part in both waves of data collection. This limited our ability to assess changes at the level of individual care aides. We also were able only to assess change between two time points, which limited our ability to track robust temporal changes in care aide demographics and work life. We conducted a sensitivity analysis to assess if there were systematic differences in facilities that were in the initial cohort only versus those that remained in the stable cohort and were added in the expanded cohort. Because we did find some differences in demographics and work life for care aides in facilities that chose to participate in an ongoing research program and those that chose not to continue, our results should be interpreted keeping in mind potential selection effects.
Conclusion
Worryingly, we saw no improvement in scores and in some cases, worsening scores on work life and individual care aide attributes such as care aide health, burnout, and job satisfaction. Trends were visible both between TREC 1 and TREC 2 data and within the cohort of nursing homes that participated in both waves of data collection. We also found regional variation in care aide demographics and reported characteristics of their work life. Regional variation signals a need for more empirical research examining the impact of jurisdictional policies on staff and resident outcomes.
This is a workforce under increasing stresses – some inherent in their demographic profile and many brought on by a rapidly shifting and more complex resident population and, significantly, minimal changes in resources. This workforce is predominantly female, older, at the bottom of a rigid hierarchy, and with nearly 30 per cent working more than one job. They are already vulnerable and they are caring directly for an increasingly dependent, medically and socially complex population – frail and highly vulnerable seniors with advanced cognitive impairment who cannot communicate even their most basic needs. The care aide workforce needs sufficient knowledge, skills, and resources to care appropriately for these seniors. Yet in this high-income country and with our putatively advanced health and social care system, we are still not acting on these needs.
Care aides are as vulnerable as regulated nursing has been to the historical perception of their work as “domestic” and thus as of less importance and value. Care aides are an essential workforce in this setting – the perception that their work is “domestic”, unskilled, and thus of lesser importance and value is counterproductive to actions that will improve their working conditions and the quality of care nursing home residents receive. We do not even count care aides, making workforce planning at a national level more the purview of divination than of evidence-informed public policy. And this is the case even as we face unrelenting increases in the numbers of older adults with dementia–related diseases, for which we have no effective treatments, certainly no cure, and a still-early understanding of prevention. In the face of the need to care effectively for a significant and increasing proportion of older adults with advancing dementia (the major driver of nursing home admission), our continued inaction as a country purporting to value the oldest among us is incomprehensible.
Supplementary Material
To view supplementary material for this article, please visit https://doi.org/10.1017/S0714980818000338









