The purpose of this article is to describe the regulated nursing workforce providing skilled care to frail older persons in Western Canadian residential long-term care (LTC) facilities. We first provide background on the Canadian LTC-regulated nurse (registered nurses, licenced practical nurses) workforce and the methods of our study, including a description of the Translating Research in Elder Care (TREC) program, which our study comes from. In our results, we report on the demographic characteristics (e.g., age, experience) as well as on selected work (e.g., work engagement, empowerment) and health-related (e.g., health status, burnout) outcomes of this important workforce. This article follows a previously published article in which we described the unregulated nursing (i.e., health care aide/personal support worker) workforce in Western Canadian LTC facilities (Estabrooks, Squires, Carleton, Cummings, & Norton, Reference Estabrooks, Squires, Carleton, Cummings and Norton2015). Combined, both articles will provide a comprehensive picture of the LTC nursing (regulated and unregulated) workforce in Western Canada.
Background
Residential LTC facilities, also known as nursing homes in Canada, are generally understood to be residences that provide 24-hour skilled nursing care for frail, older adults. Although unregulated health care workers (i.e., care aides or personal support workers) provide up to 80 per cent of personal care in LTC facilities (Berta, Laporte, Deber, Baumann, & Gamble, Reference Berta, Laporte, Deber, Baumann and Gamble2013), the skilled component of the nursing care provided is by regulated nurses, meaning registered nurses (RNs) and licensed practical nurses (LPNs; LPNs are also referred to as registered practical nurses [RPNs] in some parts of Canada). Currently, in Canada, each province or territory is responsible for licensure of nurses within their jurisdiction, and sets their own standards of practice (Canadian Nurses Association, 2015). All regulated nurses must meet a minimum educational requirement; RNs complete a 4-year baccalaureate degree in nursing, whereas LPNs complete a 2-year diploma in practical nursing (College of Nurses of Ontario, 2016). Both RNs and LPNs study from the same knowledge base and focus on clinical skills; however, RNs study longer and have a stronger theoretical base in nursing and other related content areas with a significant emphasis on the development of critical thinking and decision-making skills (Boblin, Baxter, Alvarado, Baumann, & Akhtar-Danesh, Reference Boblin, Baxter, Alvarado, Baumann and Akhtar-Danesh2008; College of Nurses of Ontario, 2014). Therefore, RNs’ scope of practice is wider, enabling care provision to complex and unpredictable patient/resident populations whereas LPNs practice within a more restricted scope of practice, caring for more predictable patient/resident populations.
In 2016, 15 per cent of all regulated nurses in Canada worked in LTC facilities (Canadian Institute for Health Information, 2017). Although the overall distribution of regulated nurses has remained stable over the past 10 years at a national level, at the provincial level there have been some notable shifts. For example, in British Columbia, the percentage of RNs working in long-term care dropped from 11.1 per cent in 2006 to 7.3 per cent in 2016; during the same period, the percentage of LPNs working in long-term care rose from 35.2 per cent to 44.2 per cent. In Alberta, there was a smaller shift, with RNs going from 7.8 per cent to 6.3 per cent and LPNs only changing from 27 per cent to 27.7 per cent between 2006 and 2016. These shifts reflect complex evolving staffing models that have been implemented over the past decade in long-term care to try to address economic (cost-cutting), human resource, and patient acuity concerns in the LTC sector (Harris & McGillis Hall, Reference Harris and McGillis Hall2012). Evidence to date, however, does not suggest that any specific nursing-model or skills-mix model is effective at improving patient and/or staff outcomes in long-term care settings (Hodgkinson, Haesler, Nay, O’Donnell, & McAuliffe, Reference Hodgkinson, Haesler, Nay, O’Donnell and McAuliffe2011).
There is wide variation in how LTC facilities utilize regulated nurses (McCloskey, Donovan, Stewart, & Donovan, Reference McCloskey, Donovan, Stewart and Donovan2015). RNs in long-term care tend to hold a variety of positions from director of care, nursing supervisor, and clinical nurse for the LTC facility with their main responsibilities being supervising and delegating the work of LPNs and care aides (Chu, Ploeg, Wong, Blain, & McGilton, Reference Chu, Ploeg, Wong, Blain and McGilton2016; McGilton et al., Reference McGilton, Bowers, Heath, Shannon, Dellefield, Prentice and Mueller2016). The responsibility of RNs in long-term care is typically more managerial with providing direction, consultation, and liaising with external care professionals (e.g., medical director, hospital staff related to admission and transfer) (Manning, Reference Manning2010; Ottem & Overton, Reference Ottem and Overton2000). In contrast, LPNs function in more of a clinical role at the resident care unit level; they supervise care aides and provide resident care through administration of medications and monitoring resident progress (e.g., dressing changes) (Corazzini, Anderson, Mueller, Thorpe, & McConnell, Reference Corazzini, Anderson, Mueller, Thorpe and McConnell2013; Manning, Reference Manning2010; McGilton et al., Reference McGilton, Bowers, Heath, Shannon, Dellefield, Prentice and Mueller2016). In general, regulated nurses (RNs and LPNs) in LTC facilities tend to focus more on care coordination than on providing direct care in long-term care, which is the role of care aides (McGilton, Bowers, McKenzie-Green, Boscart, & Brown, Reference McGilton, Bowers, McKenzie-Green, Boscart and Brown2009).
In addition to variations in regulatory practices and roles, the requirements around staffing levels (i.e., how many) and staffing mix (i.e., who) of regulated nurses working in Canadian LTC facilities is different both across and within provinces. For example, British Columbia has no requirement for RN presence in the LTC facility (B.C. Regulations, 2009), whereas two provinces, New Brunswick and Nova Scotia, require an RN to be on duty 24/7 only if the LTC facility has more than 30 beds (Bryan et al., Reference Bryan, Murphy, Doyle-Waters, Kuramoto, Ayas, Baumbusch and McGregor2010). The majority of provincial legislations stipulate a minimum of one RN be available 24/7 (Ontario, Saskatchewan, Manitoba, Quebec, Prince Edward Island, Newfoundland, and Labrador). However, this requirement is interpreted as one RN regardless of the size of the LTC facility and is not based on resident care needs. The Registered Nurses’ Association of Ontario recently proposed that the following skill mix and staffing levels be adopted by Ontario: 20 per cent RNs, 25 per cent LPNs, and no more than 55 per cent health care aides (Grinspun, Harripaul-Yhap, Jarvi, & Lenartowych, Reference Grinspun, Harripaul-Yhap, Jarvi and Lenartowych2011).
In summary, there are significant jurisdictional differences in staffing and roles, along with a very limited body of research describing regulated nurses working in the LTC sector in Canada. This lack of descriptive knowledge has greatly reduced our ability to undertake effective workforce planning in Canadian LTC facilities which is critical to enable monitoring of progress towards better quality of work life for LTC nurses and, in turn, which should result in better quality of care and health outcomes for frail older persons who reside in Canadian residential LTC facilities. This descriptive knowledge is also needed to prioritize which outcomes to focus on in subsequent multivariate modelling of LTC nurses’ work- and health-related outcomes. Therefore, the purpose of this initial study was to describe the regulated nursing (RNs and LPNs) workforce providing skilled care to older adults living with frailty in Western Canadian residential LTC facilities. We will expand on these findings in a series of planned future studies by exploring inferentially and using multivariate statistical modelling of the factors that predict the work- and health-related outcomes of regulated nurses described in this article.
Methods
Our data are from the TREC program (ongoing since 2007). TREC is a multi-level (provinces, regions, facilities, units within facilities, care providers), longitudinal research program that examines (1) modifiable elements of organizational context in LTC facilities that are associated with knowledge translation (use of best practices) by care providers, and (2) the impact of context and knowledge translation on care providers’ quality of work life and on resident health outcomes (Estabrooks, Squires, Cummings, Teare, & Norton, Reference Estabrooks, Squires, Cummings, Teare and Norton2009). The TREC study is guided by the promoting action on research implementation in health services (PARiHS) framework (Kitson, Harvey, & McCormack, Reference Kitson, Harvey and McCormack1998), which postulates that successful implementation is a function of the interplay between evidence, context, and facilitation.
Sampling
TREC is currently situated in 91 urban nursing homes in three Western Canadian provinces: British Columbia, Alberta, and Manitoba. All LTC facilities that met TREC inclusion criteria were eligible to participate in the research program (see Supplementary File 1). We selected facilities by using stratified (by health care region within province, owner-operational model, and facility size) random sampling. There are five TREC health regions across the three western Canadian provinces: British Columbia (two regions), Alberta (two regional zones within the one Alberta health region), and Manitoba (one region). The TREC facilities in our study fell into three categories of owner-operator models: (a) public, not for profit – a facility supported primarily through public funds, owned and operated by the local government; (b) voluntary, not for profit – a facility run by a voluntary, cultural, or religious organization; and (c) private, for profit – a facility in which the individuals or agency in control receive compensation (other than wages, rent, or other expenses) for the services they provide. Finally, we categorized facilities by their size for sampling purposes: small (fewer than 80 beds), medium (80 to 120 beds), and large (greater than 120 beds).
Data Collection
TREC data reported in this article were collected from September 2014 to May 2015 using facility surveys, unit surveys, and care provider (staff) surveys. TREC facility and unit surveys collected structural data (e.g., number of beds, services offered) and were administered by TREC staff in short structured interviews with LTC facility administrators (facility surveys) and care managers (unit surveys). TREC provider surveys measured organizational context, best practice use, work life outcomes (e.g., empowerment), health outcomes (e.g., burnout, health status), and individual factors (e.g., attitude towards research) believed to influence best practice use and care provider quality of work life. The care provider surveys were completed by care aides (using a computer-assisted interview process) and by regulated nurses (RNs and LPNs), allied health providers, practice specialists, and managers (using an online survey). In this article, we report on data collected from regulated nurses – RNs and LPNs. All regulated nurses employed in the 91 TREC facilities who met the regulated nurse inclusion criteria (Table 1) and who could be contacted (through mail or personally) were invited to self-complete the TREC nurse survey online.
Table 1: Inclusion criteria (regulated nurses)

Measures
Definitions of the variables reported in this article, as well as their measurement and reliability, are given in Table 2. Our dependent variables were the demographic characteristics and work- and health-related outcomes of the nurses. Our six independent variables were nursing role (RN vs. LPN); province (British Columbia, Alberta, Manitoba); health region (five regions: two in British Columbia, two in Alberta, one in Manitoba); owner-operator model type (public, voluntary, private for profit); facility size (small, medium, large); and age of nurse (< 35 years, 35–54 years, > 55 years).
Table 2: Descriptions, measurements, and reliability of dependent variables
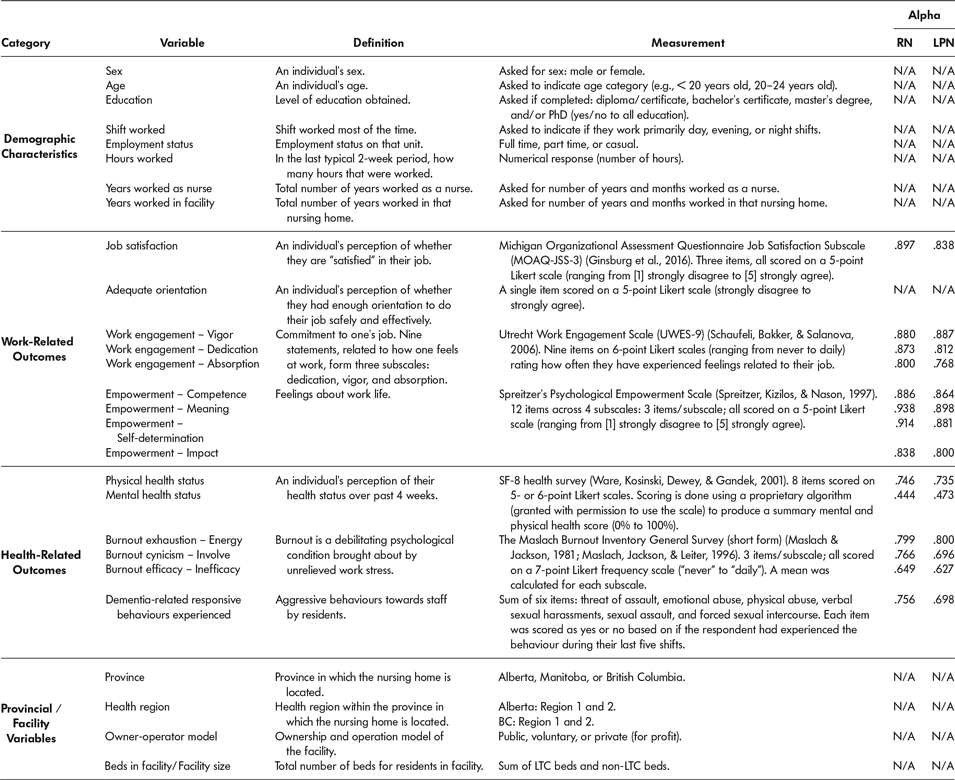
Note. Work Eng = Work Engagement, Emp = Empowerment. Items developed by the TREC team unless otherwise specified.
From the TREC facility survey, we obtained the following variables: province, region, owner-operator model, and facility size. From the care provider (RN and LPN) survey we obtained all of the nurse demographic characteristics as well as the work- and health-related outcomes. Eight demographic characteristics, which we measured with items created by the TREC team, included sex, age, education, shift worked most of the time, employment status, hours work in two weeks, years worked as a nurse, and years worked in facility. Work-related outcomes included job satisfaction, measured using the Michigan Organizational Assessment Questionnaire Job Satisfaction Subscale (MOAQ-JSS-3) (Ginsburg et al., Reference Ginsburg, Berta, Baumbusch, Rohit Dass, Laporte, Reid and Taylor2016); adequate orientation (single item from TREC survey); three facets of work engagement (vigor, dedication, absorption) measured using the Utrecht Work Engagement Scale (Schaufeli, Bakker, & Salanova, Reference Schaufeli, Bakker and Salanova2006); and four facets of psychological empowerment (competence, meaning, self-determination, impact) that we measured with Spreitzer’s Psychological Empowerment Scale (Spreitzer, Kizilos, & Nason, Reference Spreitzer, Kizilos and Nason1997). Health-related outcomes included physical and mental health status that we measured using the SF-8 Health Survey (Ware, Kosinski, Dewey, & Gandek, Reference Ware, Kosinski, Dewey and Gandek2001); three facets of burnout (exhaustion-energy, cynicism-involvement, efficacy-inefficacy) measured using the Maslach Burnout Inventory-Short Form (Maslach, Jackson, Leiter, Schaufeli, & Schwab, Reference Maslach, Jackson, Leiter, Schaufeli and Schwab1981; Maslach & Jackson, Reference Maslach and Jackson1981; Maslach & Jackson, Reference Maslach and Jackson1984); and, finally, dementia-related responsive behaviours experienced (i.e., aggression from residents towards staff), which we measured with a scale developed by the TREC team.
Statistical Analyses
We calculated means and standard deviations for all interval-level variables which included three of the eight demographic characteristics (hours worked in two weeks, years worked as a nurse, years worked in LTC facility) and all of the work- and health-related outcome variables. For categorical level variables which included the remaining five demographic characteristics (sex, age, education, shift worked most of the time, employment status), we calculated frequency counts and proportions. To assess for differences across all independent variables (demographic characteristics, work- and health-related outcomes) by nursing role (RN vs. LPN) and by health region within province, we used chi-squared tests for categorical dependent variables (e.g., shift worked most of the time), and we used independent groups t test for interval dependent variables (e.g., empowerment). To assess differences by province, owner-operator model, facility size, and nurse age, we used chi-squared tests for categorical dependent variables and one-way ANOVA for interval dependent variables.
Post-hoc tests that we used were logistic regression for categorical dependent variables and Bonferonni correction for interval level–dependent variables. All regulated nurses were first pooled to assess for differences by role (RN vs. LPN). Following this analysis, we treated RNs and LPNs as separate samples to assess each for differences by province, health region, owner-operator model type, facility size, and nurse age. Unlike unregulated staff (i.e., health care aides), the vast majority of regulated nurses in our sample were not able to identify a care unit that they worked on most of the time; therefore, a clustering correction for care unit was not possible nor necessary in our analyses. Our analyses are detailed in Tables 3–7 and Supplementary Files 2–3.
Table 3: Comparison of demographic characteristics among professional nurses by role (RN vs. LPN) (n = 757)

Note. a Chi-square test was used to test statistical differences in categorical variables (sex, age, education, shift, employment status) and t test was used for quantitative (interval and ratio level variables – hours worked, years worked as nurse, years worked in home). b Post-hoc test used was logistic regression. Significant differences were in the following age categories (reference was > 60 years): 20–29 years, 30–39 years, 40–49 years, and 50–59 years. c Post-hoc test used was logistic regression. Significant differences were in the following shift categories (reference was night): day shift and evening shift. d Post-hoc test used was logistic regression. Significant differences were in the following employment category (reference was casual): part-time. e Post-hoc test used was Bonferonni correction.
Table 4: Comparison of work- and health-related outcomes among professional nurses by role (RN vs. LPN) (n = 757)

Note. a Effect size to determine magnitude of any differences. We used eta squared which were interpreted using Cohen’s (1988) criteria: small effect = 0.01, medium effect = 0.06, and large effect = 0.14.
Table 5: Comparison of work- and health-related outcomes among RNs by age (n = 309)

Note. a Effect size to determine magnitude of any differences. We used eta squared which were interpreted using Cohen’s (1988) criteria: small effect = 0.01, medium effect = 0.06, and large effect = 0.14. b Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years and 55+ years. c Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years and 35–55 years, and < 35 years and 55+ years. d Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years and 35–55 years, and < 35 years and 55+ years. e Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years and 35–55 years, and < 35 years and 55+ years. f Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years and 35–55 years, and < 35 years and 55+ years. g Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years and 35–55 years, and < 35 years and 55+ years. h Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years old and 35–55 years old.
Table 6: Comparison of work- and health-related outcomes among LPNs by age (n = 448)

Note. a Effect size to determine magnitude of any differences. We used eta squared which were interpreted using Cohen’s (1988) criteria: small effect = 0.01, medium effect = 0.06, and large effect = 0.14. b Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years old and 35–55 years old. c Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years old and 35–55 years old, and < 35 years old and 55+ years old. d Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years old and 35–55 years old. e Post-hoc test used was Bonferroni correction. Significant difference was between < 35 years old and 35–55 years old.
Table 7: Comparison of work- and health-related outcomes among professional nurses by region within BC (n = 324)

Ethics
Ethical approval was obtained from the research ethics boards of all investigator-affiliated universities, and operational approvals were obtained at all 91 participating LTC facilities.
Results
Demographic Characteristics
From September 2014 to May 2015, 757 regulated nurses (309 RNs and 448 LPNs) from 89 facilities completed the TREC nurse survey (Table 3); no nurses in the remaining two TREC facilities completed the survey. The majority of respondents, irrespective if an RN or LPN, were female (n = 661, 87.3%) and 40 years of age or older (n = 487, 64.3%). RNs were primarily from Alberta (n = 126, 40.8%), followed by British Columbia (n = 113, 36.6%) and Manitoba (n = 70, 22.7%) whereas the majority of LPNs were from British Columbia (n = 211, 47.1%), followed by Alberta (n = 146, 32.6%) and Manitoba (n = 91, 20.3%). All nurses (RNs and LPNs combined) primarily worked day shifts (n = 374, 49.4%), with 278 (36.7%) working mostly evening shifts, and 95 (12.6%) working night shifts. The majority of RNs were employed part time (n = 166, 53.7%), with 122 (n = 39.5%) employed full time, and 21 (6.8%) employed casually. Conversely, the majority of LPNs were employed full time (n = 228, 50.9%) with 177 (39.5%) employed part time, and 42 (9.4%) employed casually. Years’ experience in nursing, on average, was 11.6 years for RNs compared to 6.9 years for LPNs. Years working in the current LTC facility was substantially less for both groups at 5.5 years for RNs and 4.3 years for LPNs.
We found statistically significant differences by nursing role (RN vs. LPN) on all demographic characteristics with the exception of sex (Table 3). With respect to age, all age categories with the exception of fewer than 20 years, were significantly different between RNs and LPNs with higher proportions of RNs being older (> 40 years) compared to LPNs. For shift worked most of the time, significantly higher proportions of RNs worked the night shift compared to LPNs, while more LPNs worked day and evening shifts compared to RNs. For employment status, significantly higher proportions of RNs worked part-time while more LPNs worked full-time. RNs, on average, worked significantly fewer hours in a two-week period compared to LPNs (59 hours vs. 63 hours) and had significantly more years’ experience both as a nurse (11.6 years vs. 6.9 years) and in the current LTC facility (5.6 years vs. 4.3 years).
Select (but fewer) demographic characteristics differed by province, health region, owner-operator model, facility size, and age of the nurse. For RNs, significant differences were found by province (employment status), region (British Columbia: education and years worked as a nurse), owner-operator model (age, education, and years worked as a nurse), and age of the nurse (education, years worked as a nurse, and years worked in the LTC facility). Statistically significant differences were not found by facility size for RNs. More significant differences were found in the LPN sample which included province (age, employment status, and years worked as a nurse); region (British Columbia: education; Alberta: years worked as a nurse, years worked in LTC facility); owner-operator model (age, employment status, years worked as nurse, and years worked in LTC facility); facility size (education, employment status); and age of nurse (sex, employment status, years worked as a nurse, and years worked in LTC facility). Supplementary File 1 outlines the detailed results for these comparisons.
Work- and Health-Related Outcomes
Mean scores by nursing role (RN vs. LPN) for work- and health-related outcomes are presented in Table 4. Significant differences between RNs and LPNs were noted for two work-related outcomes (empowerment–self-determination, empowerment–impact) and one health-related outcome (dementia-related responsive behaviours experienced). RNs had significantly higher scores on both facets of empowerment compared to LPNs (self-determination: mean score 4.12 for RNs vs. 3.91 for LPNs; impact: mean score 3.89 for RNs vs. 3.67 for LPNs). However, LPNs experienced significantly more dementia-related responsive behaviours from residents compared to RNs (2.81 behaviours on average over the last 5 shifts for LPNs compared to 2.35 behaviours for RNs).
Similar to our assessment of demographic characteristics, fewer work-and health-related outcomes differed by province, health region, owner-operator model, facility size, and age of the nurse than by role (RN vs. LPN). The majority of significant differences for both RNs and LPNs were by nurse age, the details of which can be found in Tables 5 (RNs by age) and 6 (LPNs by age). Three outcomes – two work-related outcomes: (a) perception of having received adequate orientation and (b) work engagement–vigor, and one health-related outcome: (c) mental health status – were significantly different by nurse age in both RNs and LPNs. For all three outcomes, values were higher (better/positive) in older nurses compared to younger nurses. Three additional work-related outcomes, all facets of empowerment (competence, meaning, impact), and one additional health-related outcome (burnout–exhaustion) were significantly different by age in the RNs sample only. For empowerment, values were consistently higher (better/positive) among older compared to younger RNs. For burnout–exhaustion, however, values were higher (which is bad/negative) in younger compared to older RNs. For LPNs, only one additional outcome (work engagement–dedication) varied significantly by nurse age with older LPNs reporting higher dedication levels compared to younger LPNs. See Tables 5 and 6 for details.
With respect to differences in work- and health-related outcomes by province, only RNs displayed any significance, and it was for one health-related outcome: dementia-related responsive behaviours experienced. RNs in Manitoba experienced significantly more dementia-related responsive behaviours (average: 2.73 behaviours in last five shifts) compared to RNs in British Columbia (average: 1.98 behaviours in last five shifts). Differences in work and health-related outcomes by region were found only within British Columbia. RNs in British Columbia differed by region on two health-related outcomes: (a) mental health status and (b) burnout (efficacy–inefficacy). LPNs in British Columbia also differed by region with respect to one work-related outcome: their perception of having received adequate orientation. In the case of all three outcomes (mental health status, burnout efficacy–inefficacy, perception of having received adequate orientation), values were higher (better) in the same region. See Table 7.
Few differences in work- and health-related outcomes were found by an owner-operator model, and where differences did exist, there was no consistency as to which operator models led to better nurse outcomes. For instance, RNs differed by owner-operator model on two work-related outcomes: (a) work engagement–vigor (best with private-operator models), and (b) work engagement–dedication (best with public-operator models). LPNs differed by owner-operator model on one work-related variable: empowerment–impact (best with private-operator models). No significant differences in work- and health-related outcomes were found by facility size (small, medium, large). Details of these analyses can be found in Supplementary File 2.
Discussion
This study is the first, to our knowledge, to comprehensively describe regulated nurses (RNs and LPNs) working in Canadian LTC facilities. Using data from a large research program across Western Canada, we provided a summary of regulated nurses in Canadian LTC facilities with respect to their demographic characteristics, as well as several important work- and health-related outcomes. We also conducted and provided a detailed and robust comparison of these characteristics and nurses’ work- and health-related outcomes by nursing role, province, health region, owner-operator model type, facility size, and nurse age. As a result, this study offers several novel insights about the current group of regulated nurses working in Western Canadian LTC facilities.
Differences by Age
In terms of demographic characteristics, we found significant differences between RNs and LPNs. For example, LPNs were younger than RNs. In our sample, 42.4 per cent of LPNs were under 40 years of age, compared to only 25.9 per cent of RNs. This difference may be related to the shift in regulated nurse staffing that has taken place in some Western provinces over the past decade. Historically, most LTC facilities were staffed with RNs only; however, this has changed over time (Canadian Institute for Health Information, 2017), and so the younger LPNs may also be newer to the LTC workforce than their older RN counterparts. As well, in terms of job availability, RNs have always worked across the continuum of care (i.e., acute [hospital-based] care, community/home care, and long-term care) and have had a greater range of opportunities than LPNs, who, until recently, have been more limited in their scope of practice in acute care settings and were more likely to work in the community or long-term care (Canadian Institute for Health Information, 2017; Corazzini et al., Reference Corazzini, Anderson, Mueller, Thorpe and McConnell2013).
We also found that younger (< 35 years) RNs report feeling less competent and that they had inadequate orientation compared to older RNs. As described earlier, RNs in LTC facilities tend to hold positions of greater leadership and are often accountable for resident care provided by others on the care team (Chu et al., Reference Chu, Ploeg, Wong, Blain and McGilton2016; McGilton et al., Reference McGilton, Bowers, Heath, Shannon, Dellefield, Prentice and Mueller2016). However, there is no structured pathway for RNs to learn how to take on such leadership roles in the care of older adults (Dwyer, Reference Dwyer2011). This relatively quick shift into managerial and leadership roles immediately upon entering the LTC facility workforce without concurrent training or mentorship has been reported by others (Bennett, Ward, Scarinci, & Waite, Reference Bennett, Ward, Scarinci and Waite2015) and could contribute to younger RNs’ feelings of lower competency and inadequate orientation. Furthermore, younger RNs (< 35 years) in our sample also experienced less meaning and impact in their job compared to older RNs. Because younger RNs may not have as extensive experience at the point-of-care as their older counterparts, they may not appreciate the impact of their role on care provision.
Both younger LPNs and RNs report significantly worse burnout–emotional exhaustion and poorer mental health compared to older age groups (corroborating findings from Woodhead et al.; Woodhead, Northrop, & Edelstein, Reference Woodhead, Northrop and Edelstein2016). One possible explanation for this may relate to seniority, which comes with age and time spent in a workplace. Seniority is important in health care environments, and can provide greater choice around holidays and shift scheduling. Previous research has found that more restricted holiday and shift choice, typically experienced by younger nurses with less seniority, can contribute to higher burnout and lower reported levels of good mental health (McGilton, Boscart, Brown, & Bowers, Reference McGilton, Boscart, Brown and Bowers2014). Overall, our results relating to the role of nurse age in residential LTC settings is an important consideration for employer-initiated programs and supports to ensure that this group is retained in the LTC facility-based sector over the course of their careers.
Differences by Role (RN vs. LPN)
In terms of type of roles, about half of the RNs in our sample (53.7%) worked part time. Again, this may reflect changing job patterns and a decline in full-time positions (Pyper, Reference Pyper2004). McGilton et al. (Reference McGilton, Boscart, Brown and Bowers2014) reported a trend towards limiting the number of full-time RNs in favor of LPNs and care aides (Berta et al., Reference Berta, Laporte, Deber, Baumann and Gamble2013; Canadian Institute for Health Information, 2017) as a common cost saving measure in the LTC sector. Yet at the same time, this shift to part-time may provide a buffering effect and also help explain differences in burnout–emotional exhaustion and mental health between LPNs and RNs.
Our results also illustrated differences between the amounts of dementia-related responsive behaviours that regulated nurses’ experience at work. Consistent with findings from Shields and Wilkins (Reference Shields and Wilkins2009) and from Estabrooks et al. (Reference Estabrooks, Squires, Carleton, Cummings and Norton2015), our results indicated that nurses closest to the point of care (LPNs) experience more dementia-related responsive behaviours from residents than do RNs. As LPNs tend to spend more of their time providing direct (i.e., medication provision) care than RNs, who spend the majority of their time providing indirect (i.e., charting, documenting) care (McCloskey et al., Reference McCloskey, Donovan, Stewart and Donovan2015), this finding is not surprising. However, it is concerning given the potential influence on other work-related outcomes (e.g., burnout) and risk for work-related injury. Recent research from the United States has demonstrated that in facilities where regulated nurses have clearly differentiated roles and there is greater RN presence closer to the point-of-care, there are lower rates of undesirable nurse and resident outcomes (Corazzini et al., Reference Corazzini, Anderson, Mueller, Thorpe and McConnell2013).
We also observed differences in mental health, burnout–efficacy, work engagement–vigor and work engagement–dedication among LPNs across regions and owner-operator models. Previous research indicates that there is wide variation in the understanding of LPN scope of practice in LTC facilities (McCloskey et al., Reference McCloskey, Donovan, Stewart and Donovan2015), and there is great variation in how the role can be enacted in different facilities. Research previously demonstrated that when there are fewer RNs in an LTC facility, LPNs may engage in nursing activities that are beyond their scope of practice and for which they are ill-prepared (Mueller, Anderson, McConnell, & Corazzini, Reference Mueller, Anderson, McConnell and Corazzini2012) which may further contribute to negative work-related outcomes. Further research is needed to examine how the work context (i.e., regional staffing models, owner-operator differences) influences the enactment of the LPN role and the consequences for work-related outcomes.
Strengths and Limitations
Although our sample was large and representative of urban nursing homes in the western Canadian provinces of British Columbia, Alberta, and Manitoba, we have no assurance that our findings are representative of urban nursing homes in Canada in general. We saw several differences, especially by role (RN vs. LPN), region, and nurse age, suggesting that important variations may exist across the country with respect to a number of demographic characteristics and important work- and health-related outcomes for regulated nurses employed in LTC facilities. It is important to note that our findings do not reflect the situation in rural Canada; our sample was limited to urban LTC facilities. Although the nurse surveys were completed online allowing for anonymity and were subject to a rigorous quality assurance process, the data are self-reported and, therefore, may be subject to self-report measurement biases (i.e., recall and social desirability).
Next Steps
Our next steps involve conducting a series of multivariate statistical models using the TREC-regulated nurse data reported in this study to determine what factors – demographic, individual, and contextual – influence work- and health-related outcomes. This will allow us to offer concrete recommendations on how to improve quality of work life for regulated nurses in Canadian residential LTC settings which, in turn, will improve resident health outcomes. Importantly, this next phase of our work will be guided by a variety of theoretical perspectives relevant to nurses’ quality of work life. The use of theory in multivariate analyses is critical not only to the selection of appropriate variables to include in the models but also to give the final models a meaningful context. In addition, because many researchers try to test theories, findings from theory-based research are not only relevant to the theory’s explanation of events, but also to the findings of other researchers. Hence, greater progress in understanding nurses’ quality of work life will come when we build on each other’s work, which is often coordinated through the use of common theories. Unfortunately, there is no one all-encompassing theory or conceptual framework suitable to guide all of our future models on work- and health-related outcomes in nurses. Therefore, we will utilize the most appropriate theories for each planned model. For example, we are currently completing models of job satisfaction of regulated nurses, which are guided by Kanter’s theory of structural empowerment (Kanter, Reference Kanter1993) and Spreitzer’s theory of psychological empowerment (Spreitzer, Reference Spreitzer1995a, Reference Spreitzer1995b; Spreitzer et al., Reference Spreitzer, Kizilos and Nason1997).
Conclusion
This is the first study to describe the regulated nurse workforce and their work outcomes in Western Canada. We discovered several important differences both between and within regulated nurse groups (RNs and LPNs) working in LTC facilities which can be used to inform important and needed policy related to staffing decisions in Canadian LTC facilities. Our findings also point to places where additional system supports are needed, such as for younger RNs in the LTC workforce and LPNs working closer to the point of care. These findings, when combined with the earlier report on the unregulated (care aide) workforce (Estabrooks et al., Reference Estabrooks, Squires, Carleton, Cummings and Norton2015), provide a comprehensive examination of the nursing workforce in LTC facilities in Western Canada. This examination of the nursing workforce can be used to develop national and provincial strategies to improve the quality of work life for nurses in Western Canadian LTC facilities, which will lead to a higher quality of resident care for the older persons to reside in these residences.
Supplementary Material
To view supplementary material for this article, please visit https://doi.org/10.1017/S0714980818000478









