Background
The global population is rapidly aging. According to the United Nations (2015), adults over the age of 60 accounted for 9.9 per cent (607 million) of the world’s population in 2000. This share increased substantially, to 12.3 per cent (901 million), in 2015, with projected increases to 16.5 per cent in 2030 and 21.5 per cent in 2050. The older population, whose age cut-off may vary in different contexts and regions, is growing faster in urban areas, and the aging process is most advanced in developed countries. In Canada, older persons are the fastest-growing age group. In 2016, 16.9 per cent of Canada’s population was aged 65 or older, compared to 7.6 per cent in 1961, and for the first time the number of older people surpassed the number of children (0–14 years). The older population is projected to make up a quarter of Canada’s population by 2036 (Statistics Canada, 2016).
International migration is another global trend that has shaped the demographic landscape worldwide, particularly in major immigrant-receiving countries such as Canada, the United States, the United Kingdom, and Australia. Canada has seen an increasing influx of newcomers, particularly from Asia and the Middle East (Statistics Canada, 2016). Although immigrants represent 21 per cent of Canada’s total population, they make up 30 per cent of the country’s older population (65 years and older) (Statistics Canada, 2011). In major urban centres, immigrants make up large proportions of the overall older adult population. In the Toronto Census Metropolitan Area, for example, immigrants account for 48 per cent of the total population but 70 per cent of the population over age 65 (Statistics Canada, 2011).
Immigrants living and aging in a foreign country face many settlement challenges, creating a demand for essential services such as health services (Dean & Wilson, Reference Dean and Wilson2010; Joo & Lee, Reference Joo and Lee2016; Tsoh et al., Reference Tsoh, Sentell, Gildengorin, Le, Chan, Fung and Nguyen2016; Zhou, Reference Zhou2012). They often underutilize health services and encounter multiple access barriers related to language, culture, health beliefs, cost, lack of health insurance, location (e.g., availability and distance), and socioeconomic status (Campbell, Klei, Hodges, Fisman, & Kitto, Reference Campbell, Klei, Hodges, Fisman and Kitto2014; Thomson, Chaze, George, & Guruge, Reference Thomson, Chaze, George and Guruge2015; Wang & Kwak, Reference Wang and Kwak2015). These barriers to health care access could have a great impact for aging immigrants because of their advanced years, decreasing mobility, and low socioeconomic status, which may further affect their health status (Dean & Wilson, Reference Dean and Wilson2010; Subedi & Rosenberg, Reference Subedi and Rosenberg2014).
Older immigrants with a longer length of residence in their host country than newcomers in general show a higher prevalence of self-reported health status and chronic diseases compared to non-immigrants and younger immigrants (Creatore, Moineddin, Booth, Glazier, & Manuel, Reference Creatore, Moineddin, Booth, Glazier and Manuel2012; Kennedy, Kidd, McDonald, & Biddle, Reference Kennedy, Kidd, McDonald and Biddle2015; McDonald & Kennedy, Reference McDonald and Kennedy2004). However, a healthy immigrant effect among newcomer older adults is somewhat evident (Gee, Kobayashi, & Prus, Reference Gee, Kobayashi and Prus2004). Recent immigrants including older immigrants usually arrive in the country healthier than the Canadian-born population and long-term older immigrants (Gee et al., Reference Gee, Kobayashi and Prus2004; Laroche, Reference Laroche2000; Wang & Palacios, Reference Wang and Palacios2017). In the first six months to two years after arriving, older immigrants begin to experience physical and mental health problems due to migration and settlement challenges and stress related to cultural differences, discrimination, environmental adaptation, dietary changes, or difficulties with the health care system (Ahmed et al., Reference Ahmed, Shommu, Rumana, Barron, Wicklum and Turin2016; Sanou et al., Reference Sanou, O’Reilly, Ngnie-Teta, Batal, Mondain, Andrew and Bourgeault2014; Thomson et al., Reference Thomson, Chaze, George and Guruge2015). After approximately 10 years living in Canada, they experience further health decline, and their health status becomes inferior to that of their Canadian-born counterparts (Ahmed et al., Reference Ahmed, Shommu, Rumana, Barron, Wicklum and Turin2016; Gee et al., Reference Gee, Kobayashi and Prus2004; Guruge et al., Reference Guruge, Birpreet and Samuels-Dennis2015a; Sanou et al., Reference Sanou, O’Reilly, Ngnie-Teta, Batal, Mondain, Andrew and Bourgeault2014).
As one of the five principles of the Canada Health Act (CHA), accessibility is meant to guarantee that provincial health insurance plans “provide for insured health services on uniform terms and conditions and on a basis that does not impede or preclude, either directly or indirectly whether by charges made to insured persons or otherwise, reasonable access to those services by insured persons” (Government of Canada, n.d.). The underlying sentiment of accessibility in the CHA is to ensure equal access to medically necessary services for all Canadians regardless of their age, immigration status, or socioeconomic status (Ahmed et al., Reference Ahmed, Shommu, Rumana, Barron, Wicklum and Turin2016; Wilson & Rosenberg, Reference Wilson and Rosenberg2004). However, a recent review by Kalich, Heinemann, and Ghahari (Reference Kalich, Heinemann and Ghahari2016) found many health care barriers facing immigrants in Canada, affecting both their ability to access care and the quality of care they receive. Other studies have identified both individual and structural barriers facing immigrants in accessing primary health care or mental health services (Ahmed et al., Reference Ahmed, Shommu, Rumana, Barron, Wicklum and Turin2016; Crawford, Ahmad, Beaton, & Bierman, Reference Crawford, Ahmad, Beaton and Bierman2016; Thomson et al., Reference Thomson, Chaze, George and Guruge2015). To date, no review has focused specifically on older immigrants, arguably the most vulnerable among the immigrant population.
In Canada, the emphasis on “aging in place” is often coupled with inadequate and constraining funding and staffing challenges for long-term care (Brazil, Maitland, Ploeg, & Denton, Reference Brazil, Maitland, Ploeg and Denton2012; Heckman, Kelley, Stolee, & Strachan, Reference Heckman, Kelley, Stolee and Strachan2014; Williams et al., Reference Williams, Lum, Morton-Chang, Kuluski, Peckham, Warrick and Ying2016). This has led to an increased dependence on primary health care, delivered mainly by primary health care physicians (PHPs) or family physicians to older adults living in home or community settings. However, shortages of physicians – in particular, family physicians – have been a long-standing and pressing issue in Canada due to the country’s aging population, aging physicians, and physician maldistribution in different geographic areas (Dove, Reference Dove2009; Heckman et al., Reference Heckman, Kelley, Stolee and Strachan2014; McElroy, Reference McElroy2004; Pong, Reference Pong2008; Silver, Reference Silver2017). These factors collectively put older immigrants at a disadvantage with respect to accessibility of timely, quality, and culturally competent health care.
The purpose of this scoping review is to summarize the existing research and knowledge concerning older immigrants’ access to, and utilization of, health services in Canada. The focus is primary health care delivered mainly through PHPs, who also play an important role in managing mental health care and other specialized areas such as cardiovascular and diabetes care as well as monitoring, screening, and preventive care. Thus, relevant research on accessing mental health services, health promotion, and chronic disease prevention is also included in the review, to gain a comprehensive understanding of barriers, challenges, and facilitators in terms of older immigrants’ access to care in Canada. Services that are typically not covered by provincial (universal) health insurance plans – such as optometry, dentistry, and therapies that require extended health insurance – have been excluded from the review.
The review provides a thorough understanding of the status of access to health services among older immigrants in a publicly funded health care system. It yields implications for developing public health policies that address the unmet health needs of older immigrants. The findings will contribute to our knowledge of the adequacy of the Canadian health care system in providing needed care to older immigrants in the context of “aging in place”.
Methodology
The study used the five-stage framework for conducting a scoping review outlined by Arksey and O’Malley (Reference Arksey and O’Malley2005): (1) identifying the research question, (2) identifying relevant studies, (3) reviewing and selecting relevant studies for the final review, (4) charting the data or key information from the studies under review, and (5) summarizing and reporting the results. The broad research question used to guide the review was as follows: What are the experiences of older immigrants in Canada in accessing primary health care? We conducted the search using the library database of the authors’ institution, which collectively searches a large number of electronic databases, including Summon, MEDLINE, PubMed, Proquest, Scopus, Google Scholar, Web of Science, PsycInfo, ERIC, and Health Systems Evidence. In Canada and many other developed countries, “older adults” are those aged 65 years and older. The World Health Organization (WHO) and some developing countries where life expectancy is shorter than in Canada use various age cut-offs for defining older adults (e.g., 55 and older, 60 and older) (World Health Organization, n.d.). As many older immigrants in Canada come from developing nations, a 55-and-older cut-off is deemed appropriate, as it reflects the cultural differences in viewing aging and older populations (Turcotte & Schellenberg, Reference Turcotte and Schellenberg2006).
Our inclusion criteria for the search results were as follows: (a) articles written in English, (b) peer-reviewed, (c) focus on older immigrants’ access to care, and (d) Canadian context. We conducted four rounds of keyword search or until the relevance was saturated. The first search used a combination of keywords, including seniors OR older adults AND immigrant AND Canada AND primary health care OR primary physician. A total of 200 records were generated. After screening by title, we deemed 91 of these to be relevant. The keyword search was then updated to include “barrier” as a keyword. However, this yielded the same search results. The second keyword search included health services AND seniors OR older adult AND immigrant AND barrier. A total of 200 records were generated, 79 of which were related to the research question. Combining the relevant records from the first and second searches and removing duplicates yielded 161 relevant records. A third search used the following keywords: barrier OR access to health care AND older OR senior AND immigrants. It yielded 96 new and relevant records. A fourth search included the following keywords: barrier OR access to health care AND older AND spatial OR distance. It also yielded 200 results, although the relevance was saturated at 100 results, including three duplicates and 41 relevant new articles. In total, we chose 298 articles for in-depth review. Although no minimum year limit was put on the search results, all of the selected articles were published between 2002 and 2017.
The in-depth review process (see Figure 1) consisted of two steps: (a) screening of all 298 articles by abstract, and (b) reading of all remaining articles in full. Consultation with two experienced researchers in the field generated six more articles, resulting in 304 articles to be screened by abstract. After screening by abstract, 97 articles remained for full reading. The reference lists of the 25 most relevant articles (of the 97) were scanned, yielding an additional 67 relevant references. After screening by abstract, only 25 were deemed relevant. Therefore, we read 122 articles in full, 31 of which met the inclusion criteria and were included in the scoping review. In an effort to collate the articles in the scoping review, we charted all 31 selected articles based on author information, study population (ethnicity/origin, age, sample size, location), methodology (method, design, analysis), health topic, and barriers (see Table 1).
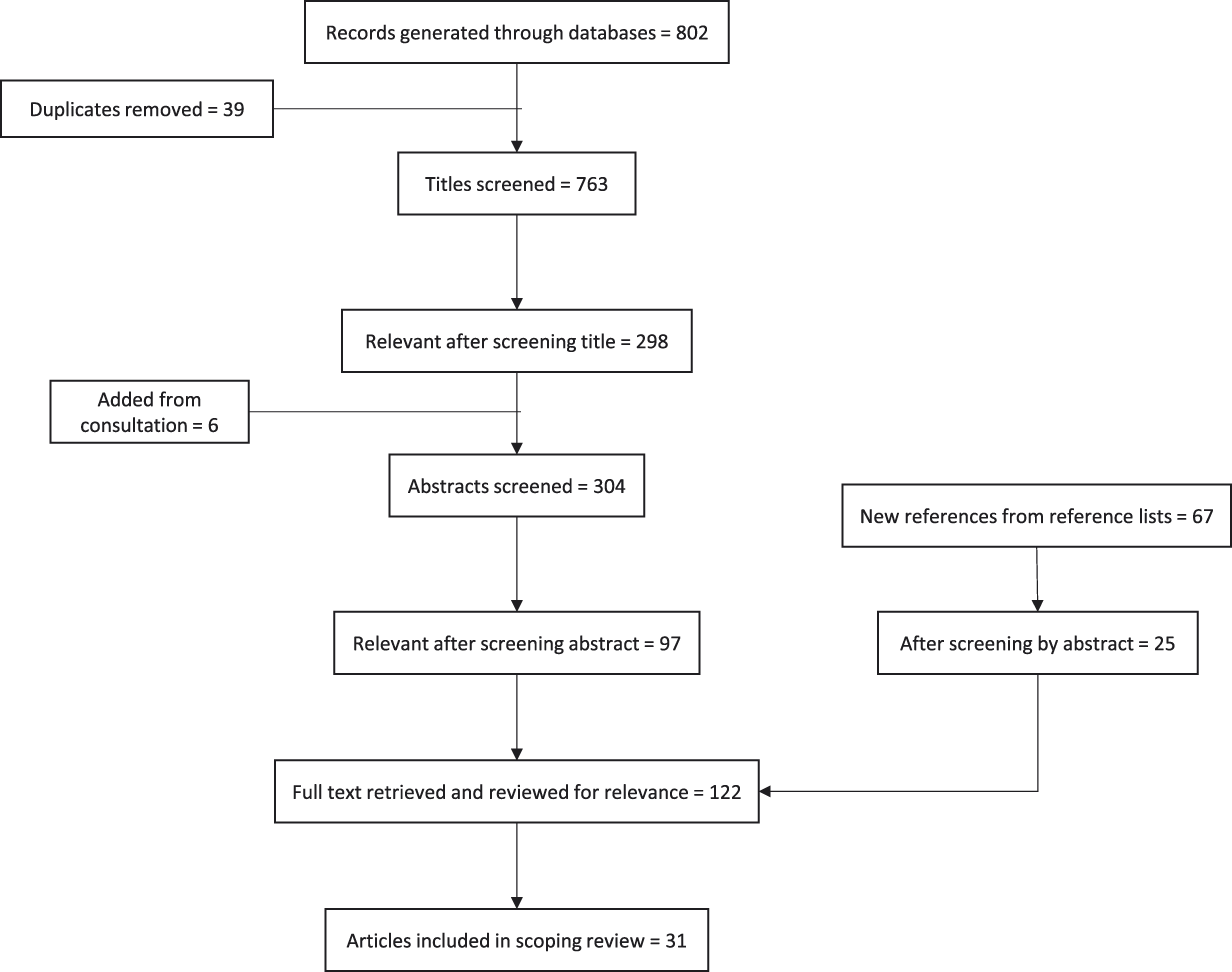
Figure 1: Research methods for scoping review
Table 1: Summary of articles included in the review
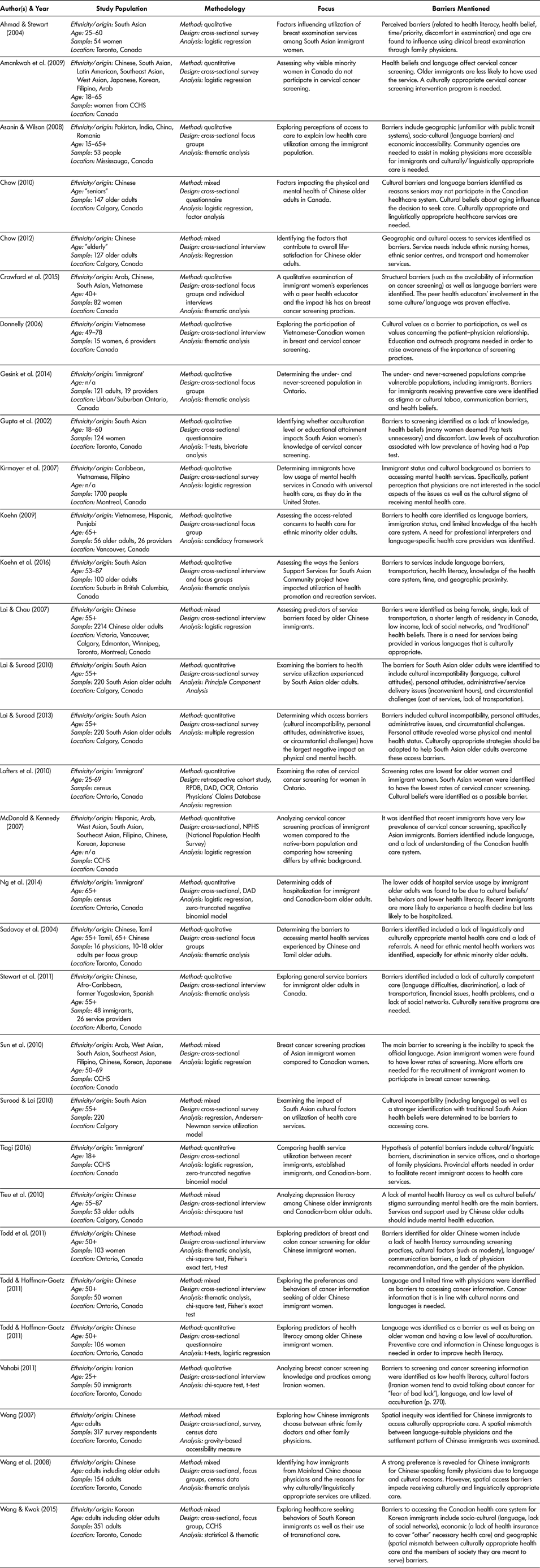
Note. CCHS = Canadian Community Health Survey; DAD = Discharge Abstract Database from Canadian Institute for Health Information (CIHI); OCR = Ontario Cancer Registry; RPDB = Registered Person’s Database.
Results
Overview of Selected Studies
Of the 31 studies we included in the scoping review, 10 per cent (n = 3) were based on data collected from one study (Lai & Surood, Reference Lai and Surood2010; Lai & Surood, Reference Lai and Surood2013; Surood & Lai Reference Surood and Lai2010). All three studies were included in the analysis because they were based on different aspects of health care access and service utilization. Approximately 29 per cent (n = 9) focused on women, 55 per cent focused on seniors only (n = 17), and 16 per cent involved service providers. In these studies, older immigrants were defined differently, as age 50 and older, 55 and older, or 65 and older, or using vague terms such as “elderly” or “older adults”.
All of the studies were Canadian-based. Sixteen were set in Ontario (n = 16; 44%), with nine (n = 9) focusing on the Greater Toronto Area and one (n = 1) comparing urban and suburban Ontario. Eight of the studies (n = 8; 22%) were set in Alberta, with seven (n = 7) focusing on Calgary. Other study settings included Montreal (n = 2); British Columbia (n = 2); and St. John’s, Newfoundland, and Labrador (n = 1). Seven studies used large data sets across Canada (n = 7). One study (n = 1) used data from seven Canadian cities: Victoria, Vancouver, Calgary, Edmonton, Winnipeg, Toronto, and Montreal. In terms of study population, several studies (n = 14; 39%) focused on broad, region-encapsulating groups such as South Asian (n = 10), Hispanic and Latin American (n = 3), West Asian (n = 3), and Arabic immigrants (n = 4; 11%). Other studies examined country-specific groups such as immigrants from China (n = 9; 25%), South Korea (n = 1), Vietnam (n = 1), France (n = 1), and Iran (n = 1). A few studies (n = 7; 19%) were comparative, examining the immigrant versus the non-immigrant population. Nine studies (n = 9; 25%) included more than one immigrant group; these covered a range of some 23 different groups (see Table 1).
Approximately 39 per cent (n = 14) of the studies employed qualitative methodology, 30 per cent (n = 11) used a quantitative approach, and 30 per cent (n = 11) used a mixed-methods approach. Sample sizes ranged from 8 to 1,700. In the researchers’ analyses, approximately 69 per cent of the studies (n = 25) used primary data collected from interviews or questionnaires, 25 per cent (n = 9) used secondary data, and 6 per cent (n = 2) used mixed primary and secondary data. The study researchers used a wide range of secondary data sources, such as the Canadian Community Health Survey (CCHS), the National Population Health Survey (NPHS), the Ontario Physicians’ Claims Database, and the Ontario Cancer Registry (see Table 1).
Summary of the Studies
We organized the 36 articles into three focus areas: primary health care access and service utilization, health promotion and cancer screening, and mental health service utilization.
Primary Health Care Access and Service Utilization
Family physicians play a pivotal role in providing primary care to older immigrants and helping them to manage chronic illnesses, which are generally most prevalent among older adults. Several studies focus on health care access among older immigrants from various ethno-racial communities, such as South Asian (Surood & Lai, Reference Surood and Lai2010); Afro-Caribbean, former Yugoslavian, and Spanish (Stewart et al., Reference Stewart, Shizha, Makwarimba, Spitzer, Khalema and Nsaliwa2011); and Chinese (Chow, Reference Chow2012; Lai & Chau, Reference Lai and Chau2007). Older immigrants face intertwining barriers associated with language and discrimination, lack of culturally appropriate programs, lack of awareness of health services that are available, cultural differences in service use, health beliefs, and transportation (Lai & Chappell, Reference Lai and Chappell2006; Lai & Surood, Reference Lai and Surood2013; Thomson et al., Reference Thomson, Chaze, George and Guruge2015). Poor access to health services often goes hand in hand with insufficient financial, human, and information resources, as well as a general “inadequate geographical coverage” of services, resulting in resettlement challenges for older immigrants (Guruge et al., Reference Guruge, Birpreet and Samuels-Dennis2015a, Reference Guruge, Thomson and Seifi2015b). Older immigrants with limited proficiency in the country’s official languages may use improvised sign language, use friends or family members as interpreters, or, occasionally, hire someone as an interpreter (Stewart et al., Reference Stewart, Shizha, Makwarimba, Spitzer, Khalema and Nsaliwa2011; Surood & Lai, Reference Surood and Lai2010). Some older Vietnamese and Hispanic immigrants have expressed an unwillingness to use family interpreters because they are reluctant to ask family members to take time off work (Koehn, Reference Koehn2009), whereas some French-speaking immigrants have shown a reluctance to use interpretation services during physical examinations for reasons of privacy and accuracy of interpretation (Ngwakongnwi, Hemmelgarn, Musto, Quan, & King-Shier, Reference Ngwakongnwi, Hemmelgarn, Musto, Quan and King-Shier2012).
Many older immigrants have developed a reliance on hospital emergency rooms and walk-in clinics as alternatives to using PHPs, not by choice but because of constraints related to the aforementioned barriers. Tiagi (Reference Tiagi2016) found that recent immigrants were less likely to visit a family practitioner and more likely to visit an emergency room, while the opposite was observed for established immigrants. Therefore, recent older immigrants are at a disadvantage in managing health during the resettlement period. Compared to both recent and established immigrants, Canadian-born populations were found to be more likely to use general practitioner services intensively. Older immigrants in Mississauga, Ontario – specifically, those from China, India, Pakistan, and Romania – were found to rely on walk-in clinics or emergency rooms for health care because general practitioners in their neighbourhood were not accepting new patients (Asanin & Wilson, Reference Asanin and Wilson2008). As a result, older immigrants with limited mobility are particularly challenged, as they are less likely to travel to other neighborhoods for health care. Although older immigrants may turn to hospital emergency rooms due to a lack of access to PHPs, it should be noted that recently arrived older immigrants in Ontario had lower rates of hospitalization than long-term immigrant and Canadian-born seniors (Ng, Sanmartin, Tu, & Manuel, Reference Ng, Sanmartin, Tu and Manuel2014). This likely reflects the superior health status of older recent arrivals, as well as their unmet health needs and poor health literacy (Ng et al., Reference Ng, Sanmartin, Tu and Manuel2014).
Health Promotion and Cancer Screening
A number of studies explored the barriers to health promotion and preventive care, such as cancer screening, which for older immigrants is primarily delivered or monitored by PHPs. Health illiteracy, language barriers, cultural differences, unavailability of services locally, declining mobility, and lack of transportation act collectively to prevent older immigrants from accessing health promotion programs, seeking cancer information, and participating in cancer screening (Gesink et al., Reference Gesink, Mihic, Antal, Filsinger, Racey, Perez and Ritvo2014; Koehn, Habib, & Bukhari, Reference Koehn, Habib and Bukhari2016; Todd, Harvey, & Hoffman-Goetz, Reference Todd, Harvey and Hoffman-Goetz2011; Todd & Hoffman-Goetz, Reference Todd and Hoffman-Goetz2011). Screening for breast and cervical cancers has been studied for different immigrant groups in various Canadian cities and regions. Iranian immigrant women in Toronto specifically and South Asian immigrant women generally were found to be challenged by a lack of knowledge about service location, screening procedures, and where to obtain relevant information (Ahmad & Stewart, Reference Ahmad and Stewart2004; Vahabi, Reference Vahabi2011). Sun et al. (Reference Sun, Xiong, Kearney, Zhang, Liu, Huang and Wang2010) found that Asian immigrants used mammogram services much less than non-immigrants and that language was one of the main factors: an Asian immigrant woman who spoke English or French was three times more likely to have ever had a mammogram. A preference for a female physician was an important factor in the use of breast cancer screening for Arab, Chinese, South Asian, and Vietnamese immigrants (Crawford, Frisina, Hack, & Parascandalo, Reference Crawford, Frisina, Hack and Parascandalo2015).
In Ontario, cervical cancer screening rates have been especially low for older women in low-income areas and for those who have immigrated recently as older adults (Lofters, Moineddin, Hwang, & Glazier, Reference Lofters, Moineddin, Hwang and Glazier2010). Similarly, racialized women have shown low rates of participation in cervical cancer screening compared to white women (Amankwah, Ngwakongnwi, & Quan, Reference Amankwah, Ngwakongnwi and Quan2009). Low screening rates have been seen in various groups, including Vietnamese and South Asian women in Toronto (Donnelly, Reference Donnelly2006; Gupta, Kumar, & Stewart, Reference Gupta, Kumar and Stewart2002). The barriers and challenges to cervical cancer screening include lack of knowledge about screening practices and the benefits of having a Pap test; cultural differences; language issues; and not having a family physician. McDonald and Kennedy (Reference McDonald and Kennedy2007) compared Canadian-born and immigrant populations (Hispanic, Arab, West Asian, South Asian, Southeast Asian, Filipino, Chinese, Korean, and Japanese) with regard to participation in cervical cancer screening. Although immigrant women have lower rates of Pap testing than Canadian-born women, the rates for immigrant women have increased with the number of years spent in Canada. Although screening rates differ by ethnic background, most immigrant women approach the same rates as Canadian-born women after 15 to 20 years in Canada. However, screening has remained low for Asian women who have been living in Canada for 15 to 20 years.
Mental Health Service Utilization
Immigrants in Canada have typically underutilized mental health services (Kirmayer et al., Reference Kirmayer, Weinfeld, Burgos, du Fort, Lasry and Young2007; Thomson et al., Reference Thomson, Chaze, George and Guruge2015). Recent immigrants in Ontario have had lower rates of using mental health services compared to long-term immigrants and native-born Canadians, whereas immigrants from Asia and the Pacific have used mental health services the least (Durbin, Moineddin, Lin, Steele, & Glazier, Reference Durbin, Moineddin, Lin, Steele and Glazier2015).
There is a dearth of knowledge regarding older immigrants’ use of mental health services, with limited scholarship focusing on large ethnic groups such as South Asians and Chinese. Chinese and Tamil older adults in Toronto have faced difficulties in accessing mental health services as reported by Sadavoy, Meier, and Ong (Reference Sadavoy, Meier and Ong2004). The challenges include too few mental health workers, limited awareness of mental disorders, reliance on ethnic-specific agencies that do not address mental health, and reluctance of families to acknowledge mental illness due to the cultural stigma associated with it. Health illiteracy, language issues, and health beliefs are considered the main barriers. In a study examining mental health literacy among older Chinese in Calgary, Tieu, Konnert, and Wang (2010) found that only 11.4 per cent of those surveyed were able to correctly identify depression, compared to 74 per cent for the general population. According to Lai and Surood (Reference Lai and Surood2013), a number of factors can explain and predict the use of both physical and mental health services among older South Asian immigrants. These are cultural incompatibility, traditional South Asian health beliefs, personal attitudes, administrative problems, and circumstantial challenges. Researchers have recommended strategies for providing culturally competent health promotion, prevention, and intervention as a means to improve the delivery of mental health services to this group.
Intersecting Factors of Access to Health Services
The review identifies a number of intersecting factors that shape older immigrants’ access to and use of health services. These factors include health literacy, language and cultural barriers, health beliefs, spatial access, and structural barriers. They influence access to needed health services and are the key areas where recommendations and practical implications can be drawn to enhance delivery of care to older immigrants with unmet health needs. These factors have been summarized in the context of population aging and unequal distribution of health services, while highlighting major trends and difficulties with health care access among older immigrants.
Health Literacy
One of the main barriers to cancer screening for older immigrants, especially women, has been health illiteracy related to the nature of screening, service availability, and service location (Ahmad & Stewart, Reference Ahmad and Stewart2004; Amankwah et al., Reference Amankwah, Ngwakongnwi and Quan2009; Crawford et al., Reference Crawford, Frisina, Hack and Parascandalo2015; Donnelly, Reference Donnelly2006; Gesink et al., Reference Gesink, Mihic, Antal, Filsinger, Racey, Perez and Ritvo2014; Gupta et al., Reference Gupta, Kumar and Stewart2002; Koehn et al., Reference Koehn, Habib and Bukhari2016; Lofters et al., Reference Lofters, Moineddin, Hwang and Glazier2010; Todd & Hoffman-Goetz, Reference Todd and Hoffman-Goetz2011; Vahabi, Reference Vahabi2011). Also, some older immigrants have found the Canadian health care system confusing and hard to navigate when seeking primary health care (Chow, Reference Chow2012; Lai & Chau, Reference Lai and Chau2007; Ngwakongnwi et al., Reference Ngwakongnwi, Hemmelgarn, Musto, Quan and King-Shier2012; Ng et al., Reference Ng, Sanmartin, Tu and Manuel2014; Tiagi, Reference Tiagi2016). Lee, Choi, and Park (Reference Lee, Choi and Park2014) found older age to be a significant predictor of poor health literacy (2014). They reported that mental health literacy is particularly limited among older immigrants. In addition, any health-service information that is available may not be available in the desired language or may not be compatible with older immigrants’ cultural values and traditions.
Cultural and Language Barriers
The growing number of older immigrants in Canada suggests an increasing demand for culturally appropriate health services (McDonald, Reference McDonald2011). This scoping review has identified a common set of barriers related to culture and health beliefs, communication, knowledge about health care resources, and settlement experiences. Increased length of residence in Canada has usually led to increased acculturation and health literacy, which in turn should improve screening for breast and cervical cancer among older immigrant women (Ahmed & Stewart, 2004; Vahabi Reference Vahabi2011). However, screening rates have remained low for Asian immigrants who have been in Canada for 15 to 20 years, which suggests that cultural values or traditions may be the main barrier to cancer screening (McDonald & Kennedy, Reference McDonald and Kennedy2007).
Proficiency in the receiving country’s official language(s) is regarded as a key measurement of acculturation (the process of change in immigrants’ culture and value systems that occurs when they are exposed to the host country’s mainstream culture). Older immigrants generally have had few opportunities to learn and become proficient in English. Limited proficiency has been a persistent barrier to older immigrants obtaining health information, using screening services, and accessing primary health care and mental health care (Asanin & Wilson, Reference Asanin and Wilson2008; Crawford et al., Reference Crawford, Frisina, Hack and Parascandalo2015; Gesink et al., Reference Gesink, Mihic, Antal, Filsinger, Racey, Perez and Ritvo2014; Jang, Yoon, Park, & Chiriboga, Reference Jang, Yoon, Park and Chiriboga2016; Koehn, Reference Koehn2009; Lai & Chau, Reference Lai and Chau2007; Lai & Surood, Reference Lai and Surood2010; Ngwakongnwi et al., Reference Ngwakongnwi, Hemmelgarn, Musto, Quan and King-Shier2012; Páez, Mercado, Farber, Morency, & Roorda, Reference Páez, Mercado, Farber, Morency and Roorda2010; Stewart et al., Reference Stewart, Shizha, Makwarimba, Spitzer, Khalema and Nsaliwa2011; Sun et al., Reference Sun, Xiong, Kearney, Zhang, Liu, Huang and Wang2010; Tiagi, Reference Tiagi2016; Todd & Hoffman-Goetz, Reference Todd and Hoffman-Goetz2011; Todd et al., Reference Todd, Harvey and Hoffman-Goetz2011; Wang, Rosenberg, & Lo, Reference Wang, Rosenberg and Lo2008). Language barriers are related to poor health outcomes among older immigrants. Professional interpreters, family members, and even technologies (e.g., Google Translate) can serve to facilitate communication. However, researchers have found that very often both physician and patient experience discomfort when confidential health information is being discussed with an interpreter, whose translations may be inaccurate or even biased, with potential medical and ethical implications (Ginde, Clark, & Camargo, Reference Ginde, Clark and Camargo2009; Koehn, Reference Koehn2009; Ngo-Metzger et al., Reference Ngo-Metzger, Sorkin, Phillips, Greenfield, Massagli, Clarridge and Kaplan2007; Ngwakongnwi et al., Reference Ngwakongnwi, Hemmelgarn, Musto, Quan and King-Shier2012; Sears, Khan, Ardern, & Tamim, Reference Sears, Khan, Ardern and Tamim2013).
Cultural competency has been recognized as an important factor in addressing culturally specific health needs, improving quality of care, and reducing ethnic disparities in health status and health care access (Eshleman & Davidhizar, Reference Eshleman and Davidhizar2006). It is particularly important in the delivery of care to older immigrants who face language barriers and have strong traditional values and health beliefs. Our review indicates that older immigrants in Chinese and South Asian communities find that their traditional health beliefs are not honored in Western health care systems. It also indicates that cultural differences between care providers and patients can affect communication and treatment due to misinterpretation of patients’ symptoms and difficulty transmitting mainstream Western medical knowledge to patients from traditional ethnic communities (Lai & Chau, Reference Lai and Chau2007; Wang et al., Reference Wang, Rosenberg and Lo2008; Surood & Lai, Reference Surood and Lai2010; Chow, Reference Chow2012). In this regard, cultural competency has come to mean more than just providing care in ethnic languages through the use of multilingual health practitioners or interpretation services. It also has meant being open to different health beliefs and practices, and actively promoting health, including mental health, to minority groups. Cultural competency is especially pertinent in the delivery of mental health services to communities whose older members may not necessarily acknowledge mental health issues due to the stigma of mental illness.
Geographical Barriers and Spatial Access
Since the frequency of trip-making decreases with age, and since travel is needed in most cases of health care utilization, older immigrants face increasing geographical barriers in accessing health services. Geographical barriers result from spatial discordance (or spatial mismatch) between where culturally appropriate health services (such as those provided by PHPs) are located and where older immigrants reside. They have limited access to care for older immigrants with restricted mobility, no means of transportation, poor health status, and low socioeconomic status (Koehn et al., Reference Koehn, Habib and Bukhari2016; Lai and Surood, Reference Lai and Surood2010; Páez et al., Reference Páez, Mercado, Farber, Morency and Roorda2010; Stewart et al., Reference Stewart, Shizha, Makwarimba, Spitzer, Khalema and Nsaliwa2011). Clustering of physicians and health services in high density urban neighbourhoods in proximity to large hospitals results in underserved neighbourhoods in terms of access to culturally appropriate care for older immigrants. For example, older Korean immigrants in Toronto have traveled a greater distance, often by bus, to access Korean-speaking family physicians compared to those who communicate with PHPs in English (Wang & Kwak, Reference Wang and Kwak2015). Research conducted from a geographical perspective has found a general spatial discordance between the distribution of PHPs and access to linguistically appropriate PHPs for different immigrant groups in various cities in Ontario (Bissonnette, Wilson, Bell, & Shah., Reference Bissonnette, Wilson, Bell and Shah2012; Wang, Reference Wang2007). This means that immigrants often must travel out of their neighbourhood to access the small number of culturally appropriate PHPs who accept new patients. Koehn et al. (Reference Koehn, Habib and Bukhari2016) has found that in low density suburban areas in British Columbia, older South Asian immigrants, particularly women, with limited spatial access to health services and transportation are isolated and must rely on family members for transportation and translation.
Socioeconomic and Structural Barriers
The challenges that older immigrants face in accessing primary health care reflect the general shortage of physicians in Canada as well as a shortage of physicians and other health care providers who speak non-official languages. For example, although an important predictor of breast and colon cancer screening is having a doctor’s recommendation, immigrants face a structural barrier when seeking a culturally appropriate PHP in close proximity who accepts new patients (Amankwah et al., Reference Amankwah, Ngwakongnwi and Quan2009; Tiagi, Reference Tiagi2016; Todd et al., Reference Todd, Harvey and Hoffman-Goetz2011). Even though Canada has a publicly financed health care system, older immigrants still face economic barriers in accessing care. Provincial insurance plans cover only “medically necessary hospital and physician services,” and provinces may charge their residents a health care premium to help pay for publicly funded services. Without extended health insurance, which is normally obtained through employment or purchased privately, low-income older immigrants cannot access eye care, dental care, or other essential services, including mental health services.
Financial barriers are reported to be a significant factor for older Korean immigrants in Toronto requiring care not covered by provincial health insurance plans, such as eye care and dentistry, which have been in high demand among older members of the Korean community (Wang & Kwak, Reference Wang and Kwak2015). Older Chinese immigrants who are financially disadvantaged have been further disadvantaged by the barriers they encounter when attempting to obtain needed services or resources (Lai & Chau, Reference Lai and Chau2007). Older immigrants of low socioeconomic status or those who have recently arrived are particularly disadvantaged, as they are often excluded from the Canadian pension system because of their limited work years in Canada.
Conclusion and Discussion
As a core issue in research on migration and health, access to health care plays a critical role for older immigrants, who are more vulnerable than both younger immigrants and the non-immigrant population, in health management during the resettlement period. Canada’s publicly funded health care system is aimed at ensuring equal access to health care for all, regardless of age and immigration status. Yet older immigrants encounter more barriers to health-service access and have higher rates of self-reported chronic diseases than both younger immigrants and their Canadian-born counterparts (Creatore et al., Reference Creatore, Moineddin, Booth, Glazier and Manuel2012; Kennedy et al., Reference Kennedy, Kidd, McDonald and Biddle2015; McDonald & Kennedy, Reference McDonald and Kennedy2004). This scoping review offers an in-depth analysis of the current literature on the experiences of older immigrants in accessing health services, particularly primary health care, in Canada. The findings of this scoping review reveal that the main barriers to accessing care – including primary health care, preventive services, and mental health care – are related to health literacy, linguistic and cultural differences, spatial access, and structural circumstances. Many older immigrants are socioeconomically disadvantaged and have limited access to Canadian pension plans. Low socioeconomic status not only influences service access, but is a key social determinant of health. The review makes an important contribution to the literature on health-service delivery and immigrant health, as it informs our understanding of the health care experiences of older immigrants, the fastest growing age group in Canada.
The scoping review has several limitations. Only studies published in English were considered. Most of the studies reviewed used primary data sources and were qualitative in their design and analysis. In the literature search process, the reference lists of only 25 studies were searched for additional sources. Most of the studies reviewed focused on men and women collectively, whereas the gender-specific studies focused only on women and their challenges as older immigrants. There were no studies focusing on men. The global gender ratios (as of 2013) are 85 men for every 100 women aged 60 to 79 and 61 men for every 100 women aged 80 and over. The majority of immigrants to Canada tend to be men, rendering the absence of male-based studies a limitation (Guruge et al., Reference Guruge, Thomson and Seifi2015b). Only four studies in the scoping review involved service providers, and these studies did not focus solely on the perspectives of service providers but included them with the perspectives of older immigrants.
In terms of region, most of the studies were based in Ontario or Alberta, with some based in British Columbia, Quebec, and Newfoundland and Labrador. No research surrounding older immigrants’ health care access was identified for other Canadian provinces or territories. Another limitation concerns the broad scope of the study populations, such as South Asian, with little emphasis on the heterogeneity of various populations and ethnicities within the group (Crawford et al., Reference Crawford, Ahmad, Beaton and Bierman2016). Several studies focused on South Asian or Chinese communities, which are Canada’s two largest immigrant groups (Koehn, Neysmith, Kobayashi, & Khamisa, Reference Koehn, Neysmith, Kobayashi and Khamisa2013). Recent immigrants from other “non-traditional” source countries or regions in East Asia, Southeast Asia, and Africa are underrepresented in the literature (Thomson et al., Reference Thomson, Chaze, George and Guruge2015). However, since Asian immigrants account for 50 per cent of immigrants in most English-speaking countries, this review can be helpful in other political and geographical contexts (Guruge et al., Reference Guruge, Thomson and Seifi2015b).
Several future research directions are identified. These include research on geographical access to health care and service distribution; qualitative research from the perspective of service providers; research that focuses on older immigrant men; comparative research on older immigrants living in urban versus rural areas; and research on older recent immigrants from a diverse range of global regions (e.g., Africa, the Middle East, Eastern Europe, South America) who are underrepresented in the extant literature. We also need research that acknowledges the heterogeneity of certain ethnic groups (such as South Asian) and how this impacts health care access and health outcomes among older members of these groups.
This scoping review focused on immigrants with legal status in Canada and with provincial health care coverage. Future research could examine the experiences of older migrants with refugee, undocumented, or other precarious status. Longitudinal research will be useful in tracking the progression, or lack thereof, of health care access over time among older immigrants. Wang and Kwak (Reference Wang and Kwak2015) reported that older Korean immigrants engage in transnational health practices, including travel to South Korea for care, importing medications, and consulting service providers in their homeland by phone or email, due to challenges experienced in meeting their health needs in Canada. Future research could investigate the prevalence of transnational health practices among other older immigrant groups and the possible relationship between these practices and barriers to health care access.
The findings of this review will serve to inform policies on and the delivery of health services and programs for older immigrants. Some of the policy implications of the findings include establishment of ethnic nursing homes, full insurance coverage for medical translators under provincial health care programs, and improvements to health literacy education for older recent immigrants, so that they receive adequate and timely information about the Canadian health care system and available resources. Health literacy education will inform older immigrants about the importance and availability of primary health care, mental health services and screening services, and where to go and who to talk to regarding questions related to health services. Efforts to enhance the delivery of culturally competent health care to older immigrants should go hand in hand with services to promote the social inclusion of older immigrants, enhance social support, and reduce exposure to discrimination. Community-based initiatives should consider all older immigrants, especially those in materially deprived neighbourhoods, thereby contributing to the overall well-being of the older immigrant community. The findings of the review also suggest the need to build age-friendly communities where policies, services – including health services – transportation, settings, and structures support and enable the healthy aging of immigrants in both urban and rural environments (Keating, Swindle, & Fletcher, Reference Keating, Swindle and Fletcher2011; Neville, Napier, Adams, Wham, & Jackson, Reference Neville, Napier, Adams, Wham and Jackson2016).




