CLINICAL SCENARIO
A 65-year-old male with known chronic obstructive pulmonary disease (COPD) presents to the emergency department (ED) with a 4-day history of progressive dyspnea, productive cough, and fever. His vital signs are p120; BP 98/50; RR 28; Temp 38°C; oxygen saturation 84% room air. He's looking tired, and you anticipate that he will need intubation. The patient is in a high acuity area, and you prepare your team and ask for additional help from a colleague.
How will you approach airway management, in this case?
KEY CLINICAL QUESTIONS
- 1.
What is the best position for the patient?
Patient positioning can aid laryngoscopic view during intubation, as well as maximize preoxygenation efforts. When considering view, Collins et al.Reference Collins, Lemmems and Brodsky1 compared the standard “sniffing” position to “ramped” position in obese patients (aligning the external auditory meatus to the sternal notch). They concluded that the “ramped” position obtained a better laryngeal view compared with the standard position, for this patient group.
The lung's functional residual capacity (FRC) is used as an oxygen reservoir during emergency preoxygenation. Supine patients have a reduced FRC. Ramkumar et al.Reference Ramkumar, Umesh and Philip2 studied the duration of non-hypoxic apnea in three groups that were preoxygenated differently (conventional v. head-up tilt v. 5cm H2O positive end expiratory pressure [PEEP]). They found that 20o of head-up tilt resulted in a longer duration of non-hypoxic apnea.
- 2.
How can I tell whether this will be an easy or difficult intubation, and does an assessment for airway difficulty inform my decision about rapid sequence intubation?
Abnormal anatomy and physiology can make airway management challenging. A bedside assessment for difficulty with laryngoscopy, bag and mask ventilation, use of an extraglottic device, and performance of a surgical airway should be done prior to intubation. Minor anatomic and physiologic challenges are common in ED patients. Most can be successfully overcome with good laryngoscopic and mask ventilation technique, use of video laryngoscopy (VL), and robust preoxygenation. In these cases, rapid sequence intubation (RSI, sedation and neuromuscular blockade) is the preferred and most effective approach.Reference Brown, Bair and Pallin3 However, if laryngoscopy and rescue gas exchange (i.e., bag and mask ventilation) are predicted to be especially difficult or impossible, then paralysis might be hazardous, and an “awake” attempt (topical anesthesia augmented by judicious use of ketamine) would be most prudent. Regardless of the degree of anticipated difficulty, rescue plans for gas exchange and intubation (placement of a laryngeal mask airway, surgical airway, etc.) should be defined prior to medication administration. Commonly used mnemonics for airway difficulty can be found in Table 1.Reference Brown, Sakles and Mick4
Table 1. Mnemonics for airway difficulty

Adapted with permission from Brown CA III, Sakles JC, Mick N, eds. Walls Manual of Emergency Airway Management. 5th ed. Philadelphia: Wolters Kluwer; 2018.
- 3.
What is the best way to preoxygenate this patient?
Preoxygenation increases the amount of safe apnea time, which in turn increases the time available for endotracheal intubation. Weingart and LevitanReference Weingart and Levitan5 reviewed the options for providing this optimally. They recommended using a standard non-rebreather mask with a high oxygen flow rate, aiming for 3 minutes of tidal volume breathing. Recent evidence suggests that flush-flow rate oxygen (40–70 lpm) should be used via a non-rebreather for preoxygenation.Reference Driver, Prekker and Kornas6 The head should be elevated if feasible. Transitioning to non-invasive positive pressure ventilation (NIPPV) may be required if oxygen saturations remain at 94% or less with ambient pressure oxygenation and suggests intrapulmonary shunting. Adding nasal cannula at 15 L/minute as a source of apneic oxygenation (ApOx) can extend the safe apnea time.
A recent meta-analysis showed a benefit to using ApOx in the ED. One ED-based randomized controlled trial showed no impact from ApOx, but this was likely due to the short duration of apnea (90% intubated in under 100 seconds). There was no opportunity to see a benefit from ApOx.Reference Caputo, Azan and Domingues7
- 4.
What tool should I use for intubation?
Multiple observational ED studies have shown improved glottic view, first attempt success and fewer adverse events when VL is used compared with direct laryngoscopy (DL).Reference Sakles, Patanwala, Mosier and Dicken8 VL, if available, should be part of routine emergency airway management practice. If DL is used, success can be optimized through use of a bougie and laryngeal manipulation.Reference Driver, Prekker and Klein9 DL, in rare circumstances, might be preferred if the intubator has never used VL but has extensive DL experience.
Box 1. Essentials for emergency airway management
• Preoxygenate for a minimum of 3 minutes in a head up or reverse Trendelenburg position using flush flow rate oxygen. Leave nasal cannula in place at 15 lpm for apneic oxygenation.
• Ramping may improve glottic view, especially in obese patients.
• If time allows, address hemodynamic instability prior to RSI.
• Assess for airway difficulty, and have rescue plans for gas exchange.
• Use VL if available. If DL is used, success can be maximized through use of a bougie and laryngeal manipulation.
- 5.
Do the patient's abnormal vitals make a difference in what I do?
Vasoplegia from induction agents and decreased venous return, as a result to positive pressure ventilation, can collude to induce circulatory collapse during RSI in patients with shock or poor cardiovascular reserve.Reference Heffner, Swords, Neale and Jones10 When time allows, a brief period of resuscitation with fluid or blood, as well as initiation of vasopressor agents (i.e., norepinephrine), should be started prior to RSI in patients with hemodynamic instability. Patients with a shock index (HR/SBP) > 0.8 are at greatest risk. A half-dose induction should be considered in patients with instability.
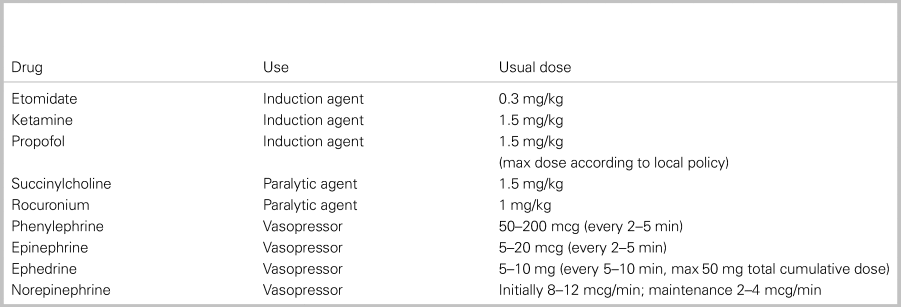
Box 2. Commonly used drugs in emergency airway management
CASE RESOLUTION
The patient requires intubation for hypoxic respiratory failure, likely due to a pneumonia and COPD. He is tried on face mask oxygenation at flush rate with upright positioning, but saturations remained at 93%. He was transitioned to Bi-PAP and saturations increased to 98%. The patient's shock index is 1.2; therefore, a 500-cc NS bolus was rapidly infused. Repeat vitals showed an HR of 108 and a systolic BP of 118 mmHg. His airway assessment for anatomic difficulty suggests minor concern about mask ventilation (presumed pneumonia and history of COPD), but he is not obese and does not have facial hair; therefore, with good bagging technique, gas exchange is predicted to be successful. You elect to intubate him with RSI using VL with a laryngeal mask airway as a back-up device. Intubation is successful and the patient is transitioned to the intensive care unit in serious but stable condition.
KEY POINTS
• Appropriate patient positioning will aid laryngoscopy as well as oxygenation
• A thorough airway assessment can help predict the difficult airway
• Obsessively preoxygenate and use ApOx. This will increase the safe apneic time to allow for intubation
• Correcting abnormal physiology prior to attempting intubation can reduce the risk of secondary compromise and insult.
Competing interests
None declared.





