Neuropsychological assessment, in the broader sense, is common clinical practice with older adults because of the widespread use of mental status examinations and dementia rating scales. In the more narrow sense, a neuropsychological assessment conducted by a clinical psychologist or clinical neuropsychologist is used less frequently and for more specific purposes. This paper outlines these uses and provides a brief overview of the different types of test that might be used, with a clinical example to illustrate the type of information gained. This review is designed not to be comprehensive, but to provide a pointer towards the latest trends in test development.
Uses of assessment
The purpose of neuropsychological assessment in clinical practice must be considered carefully if good use is to be made of available resources. The time taken, the specialist skills required and the effort of the patient all have to be balanced against the questions it will answer. A number of assessment goals should be considered and these fall into the following three main categories: detection of neuropsychological impairment, monitoring change and identification of specific disabilities.
Detection of neuropsychological impairment
At the early stages of neurodegenerative illnesses such as Alzheimer's disease, changes in cognitive function can be difficult to ascertain accurately using dementia rating scales alone. The greater sensitivity of a full assessment can sometimes detect areas of neuropsychological impairment or, conversely, determine that there is no clinically significant problem in patients who are unduly worried about perceived cognitive decline. Detection may prove to have a more important role in the future, with the increase in pharmacological treatment of dementia where early intervention may prove beneficial. Generally, neuropsychological tests tend to have high sensitivity, but low specificity in relation to differential psychiatric diagnosis. They detect neuropsychological dysfunction when it exists, but are less useful in distinguishing between different types of psychiatric or neurological disorder.
Monitoring change
In certain instances an initial assessment can form a baseline against which to monitor subsequent changes in functioning. For example, the rate of decline in Alzheimer's disease can be determined through multiple testing, particularly at the early stages where the diagnosis may be uncertain. The differential diagnosis between depression and dementia can be enhanced in this way, with improvements or decrements determining what is ‘driving’ the initial cognitive impairment. Assessing the benefits of psychological or pharmacological interventions is more likely to take place in the context of research rather than routine clinical practice. It should be recognised that a principle of neurorehabilitation is that changes in the activities of daily living or in the quality of life of the patient are the primary goal of intervention and these can be measured directly.
Identification of specific disabilities
In Alzheimer's disease the pattern of cognitive decline can vary widely between patients (Reference Morris and WoodsMorris, 1999), and this variability increases with stroke or vascular dementia. The person's strengths and weaknesses can be identified, and this information can be used in a wide range of issues, from assessing competence (e.g. driving ability) to finding compensatory strategies or helping the caregiver to understand the behaviour of the patient. Relatives and care staff can misunderstand a range of neuropsychological impairments in older people, including, for example, visuospatial disturbances, neglect syndromes and executive dysfunction. If not properly recognised, this can result in inappropriate approaches to management. There are many examples of this, but one observed by R.G.M was the placing of an older adult with mild unilateral visual neglect in a bed against a wall, with the ‘neglect’ side facing away from the wall.
Assessing the individual
The approach to neuropsychological assessment can vary widely, with each clinical psychologist tending to have a preferred ‘cocktail’ of measures and to tailor procedures to suit individual patients. The reader might refer to a number of reviews in this area for more information (e.g. Morris & McKiernan, 1994; Woods, 1999).
Assessment of older adults follows the pattern of neuropsychological assessment in general, but a number of aspects arise more frequently. A successful neuropsychological assessment often relies on a shared understanding of the overall purpose, with the establishment of confidence and trust. In older adults, more work is required to explain the purpose of the assessment and to establish rapport. Whether this is because of cohort differences in terms of understanding about psychological procedures or the longer time taken for comprehension is not fully understood. In some instances, such as in later Alzheimer's disease, the patient's lack of insight can limit understanding. In these cases, the patient will often accept the purpose of the assessment with less explanation, provided that care is taken to establish good rapport and an unhurried and relaxed approach is taken.
An additional factor is that sensory loss is more common in older adults. Both visual and hearing loss are known to correlate negatively with psychometric test performance, and failure to take this into account can result in a false impression of neuropsychological impairment. It is possible to compensate for uncorrected vision by using largely auditorily presented material or visual material that does not require fine vision. Some tests provide stimulus material tailored for people with poor vision, for example, the booklet version of the National Adult Reading Test - Revised (NART-R; Nelson & Willison, 1991). Problems with hearing should be corrected using hearing aids or communicator systems, but it is possible to assist by slowing the rate of delivery and increasing the volume, taking care not to increase the pitch. These factors may appear obvious, but are frequently overlooked by those engaged in clinical assessment.
In the UK a tailored approach to the choice of neuropsychological tests is usually adopted, with a basic set of tests, supplemented by those used to follow up a particular ‘lead’. This tailoring becomes more important for older people, whose response to failure can be more marked, compromising motivation. It is possible to adjust the complexity of the tests used to minimise the perception of failure. In addition, the tests selected must be sufficiently sensitive and discriminative to accommodate the overall level of impairment of the patient. For example, it may be appropriate to use the full range of adult tests for an otherwise intelligent patient who is at the very early stages of Alzheimer's disease, but a set of briefer screening tests would be more appropriate at a later stage (see below).
Brief assessment
In addition to the frequently used mental status examinations, such as the Abbreviated Mental Test (AMT; Qureshi & Hodkinson, 1974) and the Mini-Mental State Examination (MMSE; Folstein & Folstein, 1988), a number of screening procedures have been developed specifically for neuropsychological use with older people. These all have the advantage of being less threatening than some less specialised adult neuropsychological tests, partly because of the type of material used.
A recently developed battery is the Kendrick Assessment Scales of Cognitive Ageing (kasca; Kendrick & Watts, 1999), which are based on the older Kendrick Battery for the Detection of Dementia in the Elderly. It includes four main sub-tests that measure object recall, digit copying, reasoning and visuospatial ability. The kasca is also intended for testing cognition in people without neuropsychological or neuropsychiatric disturbance, and includes tests that have been used for this purpose in the past. These are the object recall test and digit copying, which have the advantage of parallel forms with normative data relating to a 6-week retest. Overall, the test can be used to screen for dementia.
A more comprehensive approach is the Middlesex Elderly Assessment of Mental State (MEAMS; Golding, 1989), which incorporates 12 brief tests of a core group of neuropsychological functions. It includes, for example, tests of orientation, name learning, verbal comprehension, arithmetic and perception, with two parallel forms incorporated. The idea of the test is that all items should be passed, regardless of intellectual ability (provided this is within the ‘normal’ range). This makes it less sensitive to mild impairments, but it is appropriate as a screening instrument for specific deficits. It has been validated on patients with Alzheimer's disease and vascular dementia, and data are available for older people with depression. An example showing the use of this test is given in the Appendix. An alternative to the MEAMS is the Cambridge Cognitive Examination (CAMCOG). This was developed as part of a larger assessment instrument for dementia, the Cambridge Mental Disorders of the Elderly Examination (CAMDEX; Roth et al, 1988), but is frequently used alone. Like the MEAMS, it consists of a number of brief tests, including those relating to orientation, language, memory, praxis, attention, abstract thinking and perception. This battery tends to be more sensitive to cognitive impairment at the early stages of dementia (Reference Huppert, Jorm and BrayneHuppert et al, 1996) and has been validated on patients with Alzheimer's disease, vascular dementia, depression and delirium. The CAMCOG has been found to be highly reliable, and a factor analysis of the sub-test data suggests two main factors, one relating to intelligence and the other to memory functioning (Reference Huppert, Jorm and BrayneHuppert et al, 1996). A screening instrument that has international use is the Consortium to Establish a Registry for Alzheimer's Disease (CERAD) neuropsychological battery, which includes tests of fluency, naming, constructional praxis, free recall and recognition (Reference Morris, Heyman and MohsMorris et al, 1989). The clinical utility of this test has been investigated in a number of different nationalities (see, e.g. Unverzagt et al, 1999), and it discriminates well between normal older people and those with dementia. Such screening instruments can be useful in cases where a more extensive neuropsychological assessment is not possible either because of time limitations or the severity of impairment of the patient. Owing to the brevity of the individual tests, care should be taken not to over-interpret individual results within the battery.
Intellectual assessment
Intelligence tests are frequently used by neuropsychologists to establish an approximate level of overall ability against which to compare deficits in individual functions. For example, memory performance in the average range would be regarded as normal in someone of average-range intelligence, but not necessarily normal in an individual of very superior intelligence. In neuropsychological assessment of older people, many of whom may have dementia, an alternative aim is to detect the level of overall deterioration. This has to be done against a marker of premorbid ability, estimated either from the patients' educational or socio-economic background or using specialist psychometric procedures such as the NART-R.
Premorbid intelligence
The ability to predict what intelligence would have been in the absence of brain damage relies on finding a test that reflects intellectual ability, but is least sensitive to the effect of brain damage. For dementia, at least, certain tests approximately fulfil these criteria: an example is the Wechsler Adult Intelligence Scale - Revised (WAIS-R) vocabulary sub-test. The most effective has been the NART-R, a reading test for irregularly spelt words. Here the reader has to ‘know’ the word, rather than relying on phonology to read it correctly (e.g. ‘cellist’, ‘gauche’ and ‘topiary’). The NART-R has proved remarkably resistant to the effects of early dementia, although performance does eventually reduce with moderate or severe dementia (Reference Patterson, Graham and HodgesPatterson et al, 1994). In people followed up into old age, it has also been shown to correlate better with measures of childhood intelligence than do the intellectual measures originally used. Crawford et al (1989) showed that the earlier NART score accounts for about two-thirds of the variance in performance on the Wechsler Adult Intelligence Scale (WAIS), which is significantly better than the combination of age, gender, years of education and social class. A short NART-R, with half the number of items, has now been developed for clinical use (Reference Beardsall and HuppertBeardsall & Huppert, 1997).
Despite the remarkable properties of the NART-R, it has a number of limitations. One is the low ceiling of the test, such that it fails to discriminate between levels in the very superior range of intelligence. It also does not stretch very far below the average range and has to be supplemented by the Schonnel Graded Word Reading Test, which violates a principle of the NART-R by including regular words. Inaccuracies in scoring the responses of patients can occur in practice, due in part to the difficulties in following the pronunciation guide, and the inability of the test to cope with regional accents. Alternatives to the NART-R exist, such as the Cambridge Contextual Reading Test (CCRT; Beardsall, 1998), which embeds items from the NART-R into sentences, so that words are not seen in isolation. Initial studies have shown that this test may yield a better prediction of premorbid intelligence than the NART-R for patients with mild or moderate dementia (Conway & O'Carroll, 1997). Another measure is the Spot-the-Word Test, which requires the patient to differentiate real words from non-words (Reference Baddeley, Emslie and Nimmo-SmithBaddeley et al, 1992). This test has the advantages that a verbal response is not required and that it is not susceptible to variation in regional accent. Drawbacks are that it has not proved a very successful predictor of verbal intelligence and it is susceptible to the effects of mild dementia, raising doubts about its validity in routine clinical use (Reference Beardsall and HuppertBeardsall & Huppert, 1997).
Intelligence
Determining the extent of global deterioration or establishing a marker for future deterioration are the main reasons for assessing intellectual function. The most widely used procedure has been the WAIS, superseded by the revised version (WAIS-R) and, very recently, by the WAIS-III (Reference WechslerWechsler, 1997). The main advantage of the WAIS series is the comprehensive nature of their material (the WAIS-III has 14 sub-tests), although a complete assessment can be beyond the scope of many older people with brain damage. Nevertheless, the WAIS-III has been designed with older people in mind, extending the range of the normative data from 74 years of age to a maximum of 89 years, in five age bands starting from 65 years. The stimuli have been modified to be more appropriate to older adults. For example, material has been enlarged, less emphasis is placed on speed and new sub-tests, such as Matrix Reasoning, which does not require manual manipulation, have been added. The battery has recently been validated in the UK by Wycherley et al (1999).
Short forms of the WAIS series have also been developed. A number of the short forms of the WAIS-R show that traditional short forms for older adults (such as Comprehension and Vocabulary, Block Design and Object Assembly) provide reasonably reliable estimates of verbal or performance intelligence. A short form of the WAIS-III has been developed, called the Wechsler Abbreviated Scale of IQ (WASI; Wechsler, 1999). This uses only the Similarities, Vocabulary, Block Design and Matrix sub-tests of the WAIS-III and incorporates parallel forms. It has normative data for older people and has also been validated on a UK population (Reference Mockler and CrawfordMockler & Crawford, 2000).
Owing to the desire to test people longitudinally (for example, to chart the decline associated with early dementia), the viability of repeat testing is an important issue. Practice effects are significant in the WAIS series and lead to an underestimate of the decline of a patient. This has been explored throughout the age range for the WAIS-III and it has been found to be less of a problem for older people. For example, for a group of 16-29 year olds, full-scale IQ increases by a mean of 6.3 points after a short test-retest period; for 75-89 year olds, the mean increase is only 3.2 points (Weschler, 1997).
Memory
One of the most common neuropsychological disturbances in older adults is in memory functioning, mainly owing to its ubiquitous presence in Alzheimer's disease and other major forms of dementia. Memory function can decrease quite significantly in normal ageing, and a neuropsychological assessment is sometimes used to determine whether complaints of memory disturbance are clinically significant.
A summary of current appropriate memory tests is given in Table 1. A number of tests have been developed specifically for older adults or for people with dementia. For a brief test of memory function, the Kendrick Object Learning Test, now part of the kasca (see above), is recommended. This has pictorial objects for remembering and the material is very acceptable for general use. An alternative specialised test is the Anomalous Sentence Test (AST; Weeks, 1988), which requires the repetition of sentences that are grammatically nonsensical (e.g. ‘Not in walls to the hunters rain in poetry’). This is designed to exceed the capacity of memory span and so test for short-term memory function. An alternative, for more able patients, is to use one of the range of individual memory tests developed more generally for adults, an example being the Rey Auditory Verbal Learning Test (Reference Mitrushina, Satz and DrebingMitrushina et al, 1994), which can be used to help to differentiate between processes concerned with encoding and retrieval.
Memory test batteries have the advantage of being far more comprehensive and reliable, provided that they are not too taxing. In the past, many tests did not have good normative data for older adults, but this tends not to be the case for newer versions of the main test batteries. The Warrington Recognition Memory tests have been updated to form a more comprehensive Camden Memory Test Battery (Reference WarringtonWarrington, 1996). It contains shorter verbal recognition and face recognition tests, and new tests of paired associate learning and pictorial recognition memory. The new battery has adequate normative data for older adults, but the patient still has to process each item with an orienting question within 3 seconds, which may be too fast for some people.
Other test batteries have also been revised, including the 1995 Rivermead Behavioural Memory Test (extended version: Wilson et al, 1999). The revised test is more sensitive, but the normative data relate to average or above average control subjects. The Wechsler Memory Scale has undergone a second transformation (WMS-III), and, although the test is very long for an older adult population, it has excellent USA older adult normative data, with a direct comparison with half the USA standardisation sample for the WAIS-III. The latter feature is particularly advantageous when trying to establish whether the memory dysfunction in a patient is differentially greater than the level of cognitive decline. It has been validated on a UK population (Reference Wycherley, Benjamin and CrawfordWycherley et al, 1999).
Language
Language dysfunction is a frequent neuropsychological disability in older people, not least because it is associated with both Alzheimer's disease and stroke. In Alzheimer's disease, for example, the breakdown of language function follows a clear pattern (Table 2) and is readily observable when assessing patients both informally and formally. Despite this fact no test batteries have yet been developed specifically for older people.
However, many general tests of language functioning are embedded in the brief neuropsychological batteries reviewed above, and information can be extrapolated from the WAIS-III verbal sub-tests. Additionally, brief language batteries have been developed that are appropriate for use with older adults. The short form of the Schuell Minnesota Aphasia Test (Reference Powell, Bailey and ClarkPowell et al, 1980) and the Frenchay Aphasia Screening Test (Reference Enderby, Woods and WadeEnderby et al, 1986) are still recommended for this purpose. In addition, specialised areas of language function, such as naming, can be assessed using the McKenna and Warrington Graded Naming Test, which has normative data available on 710 subjects aged between 18 and 77 years (Reference WarringtonWarrington, 1997). Fluency is assessed using variations of the Controlled Oral Word Association Test, which requires the patient to retrieve as many words as possible beginning with a particular letter in a short period. Crawford et al (1992) have used NART scores to calculate a predicted fluency score on the basis of the premorbid function of the patient.
Executive functioning
Problems in the sequencing and organisation of cognition present one of the most challenging aspects of neuropsychological rehabilitation. In older adults, this type of problem is seen in a variety of patients, including those with neurodegenerative disorder or stroke. It can be more difficult to assess because the greater complexity of executive tasks tends to make them more sensitive to the effects of normal ageing. For the same reason, tests of executive functioning tend to be sensitive to generalised brain damage such as that seen, for example, in Alzheimer's disease.
Many standardised tests of executive functioning now have good normative tests. These include, for example, the Wisconsin Card Sorting Test (Reference Grant and BergGrant & Berg, 1993), which has normative data for people up to 89 years of age. This test, which requires the patient to sort cards to a number of changing undisclosed rules, may be more appropriate in its shorter version, for which normative data for older people are also available (Reference Axelrod and HenryAxelrod & Henry, 1992). Other appropriate tests in this area are the Stroop Test (Reference Trenerry, Crossen and DeBoeTrenerry et al, 1989), which has USA normative data in a sample ranging up to 79 years, and the Trail Making Test (Reference Spreen and StraussSpreen & Strauss, 1988).
A criticism of conventional tests of executive functioning is that some lack ‘ecological validity’, in that they are unable to predict organisational problems in everyday life. An example of a newer test developed to address this issue is the Behavioural Assessment of Dysexecutive Syndrome (BADS; Wilson et al, 1996). This test, which has been standardised in control subjects aged between 16 and 87 years, includes a number of novel sub-tests. For example, the Zoo Map Test, which measures planning, resembles a board game and requires the patient to plan a route to visit six of twelve locations in a zoo. In one scenario a planned route to follow is provided, while in another the patient has to plan a route. A further test, which has proved sensitive to problems with organisation, is the modified Six Elements Test, which requires the patient to schedule their time and prioritise their effort on six tasks over a 10-minute period. Ecologically valid tests of this sort may prove more useful in predicting outcome and functional capacity in older adults with neuropsychological disorder.
Computerised procedures
Despite the ubiquity of low-cost personal computers, their use has had a relatively small impact on routine clinical assessment. This may be because rapid technological developments have discouraged the standardisation of a range of procedures. Additionally, for older adults, the computer poses more of a ‘threat’ as an unfamiliar technology, although this may change as more of the current cohort of older people become computer literate. None the less, a number of computerised procedures have been developed and a sample of these are reviewed below.
A range of early procedures, suitable for older adults, tried to exploit the advantages of computer testing. For example, the Cognitive Neuromotor Testing Battery (Reference Allen, Ellinwood and LogueAllen et al, 1993) uses computer technology to measure simple reaction time, visuomotor skill, complex processing and memory. Correlations were found with more traditional tests of mental status. An alternative battery is the Computerised Neuropsychological Examination (Reference Ritchie, Allard and HuppertRitchie et al, 1993), developed to measure attention, memory, visuospatial and language functioning, with the use of touch-sensitive screens. This takes 40 minutes to administer and has been standardised on 335 older adults.
The Cambridge Automated Neuropsychological Test Battery has been available for a number of years. It has been continuously updated and is now available for use with Windows-based operating systems. It consists of a range of tests of memory, attention and planning and has been validated extensively on different patient populations, including a large sample of older people (Reference Robbins, Merle and OwenRobbins et al, 1998). This battery also makes use of touch-sensitive screens, which older adults frequently find more acceptable than other input devices. The main clinical use, however, has been as a research tool for evaluating drug trials. The reliability of this test has been investigated by Lowe & Rabbitt (1998), who found marked variability in test-retest correlations, with some of the measures falling below levels Òconsidered methodologically acceptable”. This may not be a fair criticism of the test, since some tests in the battery assess strategy formation, which by definition is subject to practice effects and is therefore unlikely to yield reliable findings in repeated tests. Nevertheless, Lowe and Rabbitt provide useful information about the pitfalls of using this particular battery for longitudinal testing.
Conclusions
Owing to the common occurrence of brain disorder in older people, neuropsychological assessment forms a large part of the work of clinical psychologists working with them. New approaches and techniques are resulting in significantly improved tests, but the principles on which they rest remain the same. They must be tailored to take into account what the individual can achieve; ensure that the assessment procedures are well standardised for the particular population; and allow for the fact that sensory loss may be a major factor affecting cognitive performance. Neuropsychological assessment can be useful in the diagnosis of neurological or psychiatric disorder in older people, but only if used in context: it is not appropriate as the main diagnostic instrument. Finally, a neuropsychological approach should always form part of the overall strategy of care for the patients. As suggested recently by Woods (1999), Òa mechanistic approach to assessment is not appropriate”. Not only must we determine the important questions to ask and clarify the purpose of asking them, but we must also apply the right approach to obtaining information, both from assessments and from other sources.
Appendix - A case study example
Referral
A 76-year-old woman was referred for a neuropsychological assessment of her suitability for cognitive therapy for treatment of anxiety and mild depression.
Interview
She was oriented in person, but not for time, believing the year to be 1988 (not 1998). She was cooperative and well motivated. Her manner and affect were appropriate and there was no evidence of word-finding difficulties or problems with communication.
Brief neuropsychological screening
The Middlesex Elderly Assessment of Mental State (Reference GoldingGolding, 1989) was used to screen for neuropsychological dysfunction in different areas. She failed on 6 sub-tests (orientation, spatial construction, fragmented letters, easy and hard unusual views, and verbal fluency), suggesting the need for a more extensive neuropsychological assessment.
Premorbid estimate
The National Adult Reading Test - Revised gave her an estimated full-scale IQ of 123 (in the superior range).
Current intellectual functioning
A short form of the Wechsler Adult Intelligence Scale - Revised, (Reference Crawford, Moore and CameronCrawford et al, 1992) gave the following sub-test age-scaled scores (mean=10; s.d.=3). Verbal skills: comprehension=7, similarities=9, prorated IQ=84; performance skills: block design=3, object assembly=3, prorated IQ=67; prorated full-scale IQ=77. Overall her intellectual function had decreased very significantly from the premorbid level, particularly in relation to performance IQ. The latter was characterised by the presence of constructional apraxia.
Memory
In the Rey Auditory Verbal Learning Test she recalled four of the 15 words presented, relying largely on recalling the most recent words in the list. After five attempts, this increased to seven words. After a delay of 20 minutes, three words were recalled. This suggested overall a moderate impairment.
Executive functioning
She scored 21 words on the Controlled Oral Word Association Test, approximately consistent with her verbal IQ. She was also tested on the Hayling (inhibition) and Brixton (spatial anticipation) tests. Her scores on both tests were in the impaired range.
Conclusions
There was widespread intellectual decline affecting performance IQ more than verbal IQ, with specific constructional apraxia. She had a moderate memory impairment and executive dysfunction. This pattern was consistent with early dementia, with established impairment in three or more areas of neuropsychological function. A reassessment of her functioning would have been undertaken in 6 months and a behavioural, rather than strictly cognitive-behavioural, approach to managing her anxiety and depression.
Multiple choice questions
-
1. Neuropsychological assessment of older adults:
-
a is highly specific in terms of differential psychiatric diagnosis
-
b can provide a baseline from which to monitor cognitive deterioration
-
c can aid the differential diagnosis between dementia and depression
-
d is the primary outcome measure for all forms of neurorehabilitation
-
e can be used to determine the persons' strengths and weaknesses.
-
-
2. When assessing older adults:
-
a explaining the purpose of the assessment and establishing rapport take longer
-
b a fixed battery of tests is recommended
-
c performance on psychometric tests developed for this group is usually unaffected by visual or hearing loss
-
d the format is generally the same as for younger adults if a more extensive assessment is used
-
e more extensive procedures can be used with an intelligent person with early dementia.
-
-
3. Brief neuropsychological batteries:
-
a have not been developed specifically for older adults
-
b can be used as screening instruments if more extensive assessment is not possible
-
c are not particularly useful for use with older adults
-
d have shown poor reliability
-
e should be interpreted with caution with respect to individual items.
-
-
4. Intellectual assessment in older adults:
-
a is not particularly useful
-
b can establish a level of overall ability against which to compare specific functional deficits
-
c is unreliable if shortened by selecting specific sub-tests of an intelligence battery
-
d with dementia can be enhanced using tests to determine premorbid intellectual ability
-
e is catered for in the new Wechsler Adult Intelligence Scale-III.
-
-
5. Memory dysfunction in older adults:
-
a is too common in normal people to be used to detect neuropsychological dysfunction
-
b can be assessed using tests for younger adults, if normative data are available
-
c can be comprehensively assessed, but some batteries are too taxing for this client group
-
d is one of the most common neuro- psychological disturbances
-
e is an area lacking specialist tests specifically for this client group.
-
Table 1 Summary of main memory test batteries for use with older people
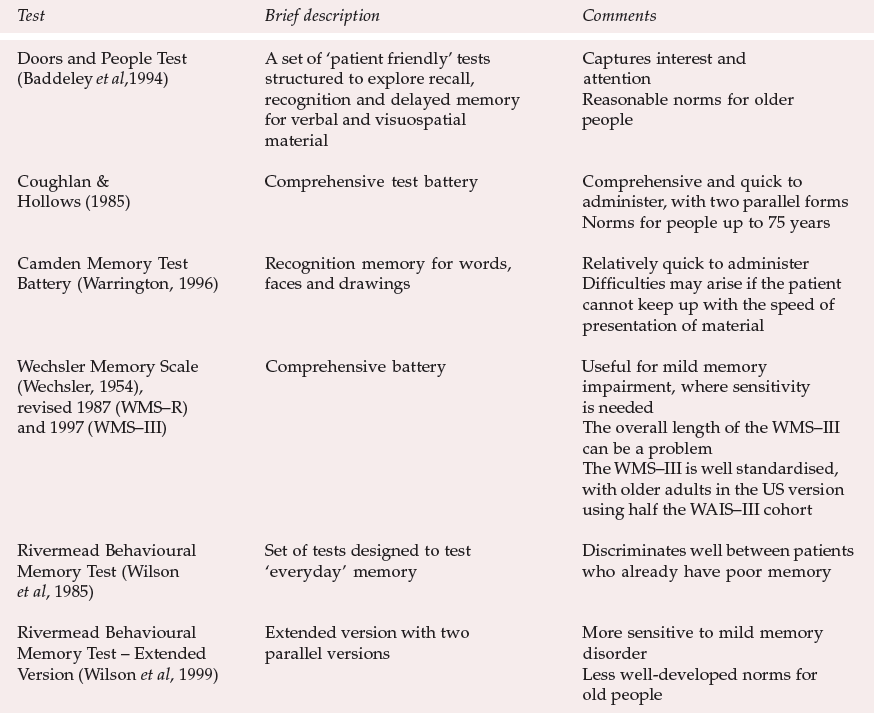
| Test | Brief description | Comments |
|---|---|---|
| Doors and People Test (Baddeley et al,1994) | A set of ‘patient friendly’ tests structured to explore recall, recognition and delayed memory for verbal and visuospatial material | Captures interest and attention |
| Reasonable norms for older people | ||
| Coughlan & Hollows (1985) | Comprehensive test battery | Comprehensive and quick to administer, with two parallel forms |
| Norms for people up to 75 years | ||
| Camden Memory Test Battery (Warrington, 1996) | Recognition memory for words, faces and drawings | Relatively quick to administer |
| Difficulties may arise if the patient cannot keep up with the speed of presentation of material | ||
| Wechsler Memory Scale (Wechsler, 1954), revised 1987 (WMS-R)and 1997 (WMS-III) | Comprehensive battery | Useful for mild memory impairment, where sensitivity is needed |
| The overall length of the WMS-IIIcan be a problem | ||
| The WMS-III is well standardised, with older adults in the US version using half the WAIS-III cohort | ||
| Rivermead Behavioural Memory Test (Wilson et al, 1985) | Set of tests designed to test ‘everyday’ memory | Discriminates well between patients who already have poor memory |
| Rivermead Behavioural Memory Test - Extended Version (Wilson et al, 1999) | Extended version with two parallel versions | More sensitive to mild memory disorder |
| Less well-developed norms for old people |
Table 2 Breakdown of language functioning as Alzheimer's disease progresses

| Early phase | Impaired word retrieval manifests as word-finding and confrontation-naming difficulties |
| In conversation the pattern of language is circumlocutionary | |
| Comprehension of complex verbal material is impaired | |
| Middle phase | Word-finding difficulties are more pronounced |
| The content of language can become vague and meaningless | |
| The syntax of language output is simplified | |
| Impaired language comprehension is exacerbated by the breakdown of reasoning ability | |
| ‘Positive’ signs of language disorder arise, such as paraphasia and verbal perseveration. | |
| Late phase | Mutism can occur |
| Any language produced may be limited to the meaningless repetition of words or nonsense sounds |
MCQ answers
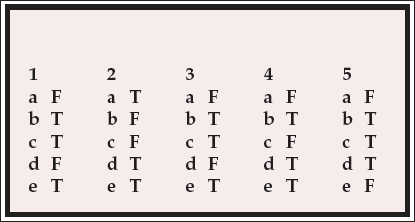
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | T | a | F | a | F | a | F |
| b | T | b | F | b | T | b | T | b | T |
| c | T | c | F | c | T | c | F | c | T |
| d | F | d | T | d | F | d | T | d | T |
| e | T | e | T | e | T | e | T | e | F |







eLetters
No eLetters have been published for this article.