226 results
Low-cost tree crown dieback estimation using deep learning-based segmentation
-
- Journal:
- Environmental Data Science / Volume 3 / 2024
- Published online by Cambridge University Press:
- 18 September 2024, e18
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
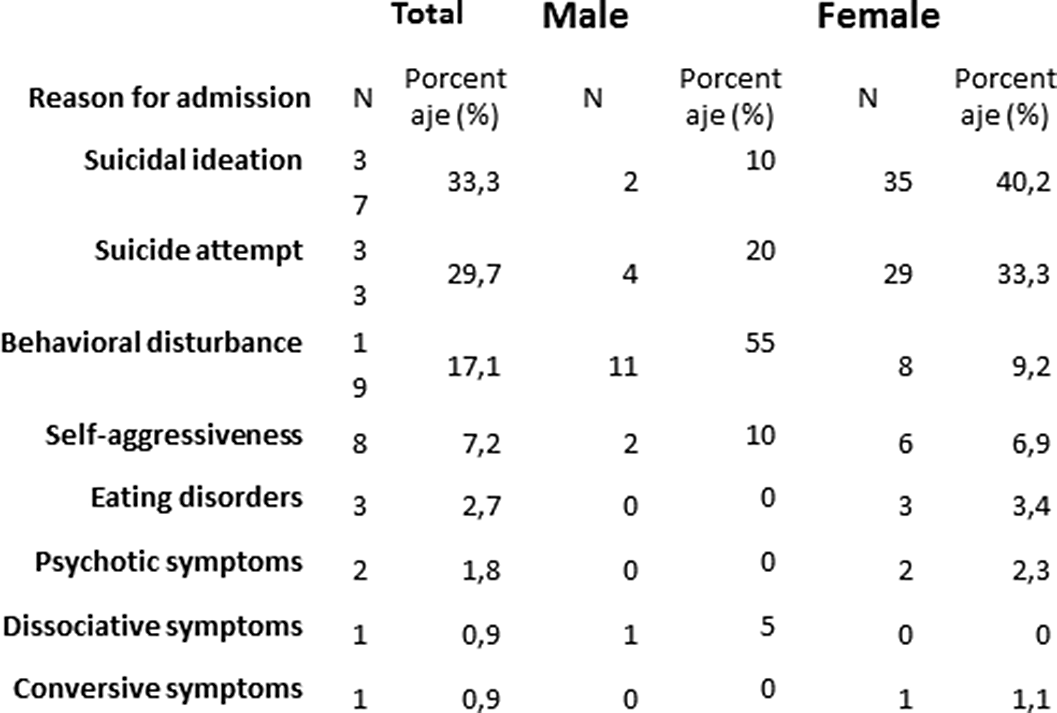
Descriptive study of suicidal behavior in adult population attended in an emergency department during a one-year period and comparative study with the following annual period
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S783-S784
-
- Article
-
- You have access
- Open access
- Export citation
Descriptive study of adolescents hospitalized in the Psychiatric Unit of a hospital in Madrid, Spain
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S102
-
- Article
-
- You have access
- Open access
- Export citation
Use of aripiprazole long-acting injectable release as a stabiliser. About a case
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S435-S436
-
- Article
-
- You have access
- Open access
- Export citation
Understanding the Occurrence of Psychiatric Disorders in Epilepsy in Brazil: An Epidemiological Investigation
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S98
-
- Article
-
- You have access
- Open access
- Export citation
Major depressive episode in the elderly. Use of maintenance ECT: a case report.
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S641
-
- Article
-
- You have access
- Open access
- Export citation
Mental and Behavioral Disorders Associated with the Use of Psychoactive Substances and Alcohol: An Epidemiological Analysis in Southern Brazil
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S831
-
- Article
-
- You have access
- Open access
- Export citation
Impulsivity as a predictor factor of health-related risk-taking
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S652
-
- Article
-
- You have access
- Open access
- Export citation
Vortioxetine as an effective drug in the treatment of depression in adolescents with long QT index. A case report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S454-S455
-
- Article
-
- You have access
- Open access
- Export citation
Pimozide as an effective treatment for obsessive symptoms related to physical discomfort in the context of somatoform symptomatology.
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S422-S423
-
- Article
-
- You have access
- Open access
- Export citation
Epidemiological analysis of hospitalizations for Schizophrenia, Schizotypal Disorders and Delirium in Rio Grande do Sul over the last 5 years
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S390-S391
-
- Article
-
- You have access
- Open access
- Export citation
Comparison of PTSD prevalence between immigrants and locals with psychotic disorders
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S97
-
- Article
-
- You have access
- Open access
- Export citation
Food intake restriction in patient with autism spectrum disorder and Moebius syndrome, a strong association. A case report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S454
-
- Article
-
- You have access
- Open access
- Export citation
Emotionally charged events as a trigger for the acute development of psychotic symptomatology. A case report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S689
-
- Article
-
- You have access
- Open access
- Export citation
Relationship between circadian rhythm and Malondialdehyde serum levels in acute and stabilized schizophrenic patients
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S759
-
- Article
-
- You have access
- Open access
- Export citation
Systematics and life cycles of four avian schistosomatids from Southern Cone of South America
-
- Journal:
- Journal of Helminthology / Volume 98 / 2024
- Published online by Cambridge University Press:
- 03 June 2024, e47
-
- Article
-
- You have access
- HTML
- Export citation
Gender Differences in the abuse of new technologies, and other addiction problems of patients from primary care
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S327-S328
-
- Article
-
- You have access
- Open access
- Export citation
Lisdexamfetamine in combination with guanfacine as an effective treatment in the management of behavioral disturbances in patients with Attention Deficit Hyperactivity Disorder (ADHD) and Autism Spectrum Disorder (ASD). Case report
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S739-S740
-
- Article
-
- You have access
- Open access
- Export citation
PANS Case Report. Assessment and management implications for a Liaison Child Psychiatry Program
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S730
-
- Article
-
- You have access
- Open access
- Export citation
Alcohol use in adult patients with autism spectrum disorder (ASD). Case report
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S762
-
- Article
-
- You have access
- Open access
- Export citation