503 results
Cognitive behavioral self-help interventions for individuals experiencing psychosis: a systematic review
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 09 September 2024, pp. 1-11
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Liquor for breakfast, fighting against alcohol consumption
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S408-S409
-
- Article
-
- You have access
- Open access
- Export citation
Emotional meanings reported by patients about their life experiences under the following in the Watch and Wait protocol: A qualitative study in a Brazilian surgery university specialized outpatient service
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S650
-
- Article
-
- You have access
- Open access
- Export citation
A man stitches his mouth in the context of a personality disorder
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S654-S655
-
- Article
-
- You have access
- Open access
- Export citation
Relation between biomarkers and suicide attempts in patients with schizophrenia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S125
-
- Article
-
- You have access
- Open access
- Export citation
From schizotypy to psychosis: is it a natural continuum?
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S658-S659
-
- Article
-
- You have access
- Open access
- Export citation
Conversive and Factitious disorders: Differential diagnosis based on a case report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S444
-
- Article
-
- You have access
- Open access
- Export citation
Short-chain fatty acids in schizophrenia: are they affected by a depressive state?
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S765-S766
-
- Article
-
- You have access
- Open access
- Export citation
Hydroxychloroquine in systemic lupus erythematosus and psychosis. A case report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S748-S749
-
- Article
-
- You have access
- Open access
- Export citation
Alexithymia in population with depressive disorders and suicidal ideation: results of an observational study
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S361
-
- Article
-
- You have access
- Open access
- Export citation
Persistent COVID an differential diagnosis with depression symptoms
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S502
-
- Article
-
- You have access
- Open access
- Export citation
Crisis resolution teams: are we doing things well?
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S609-S610
-
- Article
-
- You have access
- Open access
- Export citation
Bipolar Disorder in Pregnancy: A Challenging Case Managed with Maintenance Electroconvulsive Therapy
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S115-S116
-
- Article
-
- You have access
- Open access
- Export citation
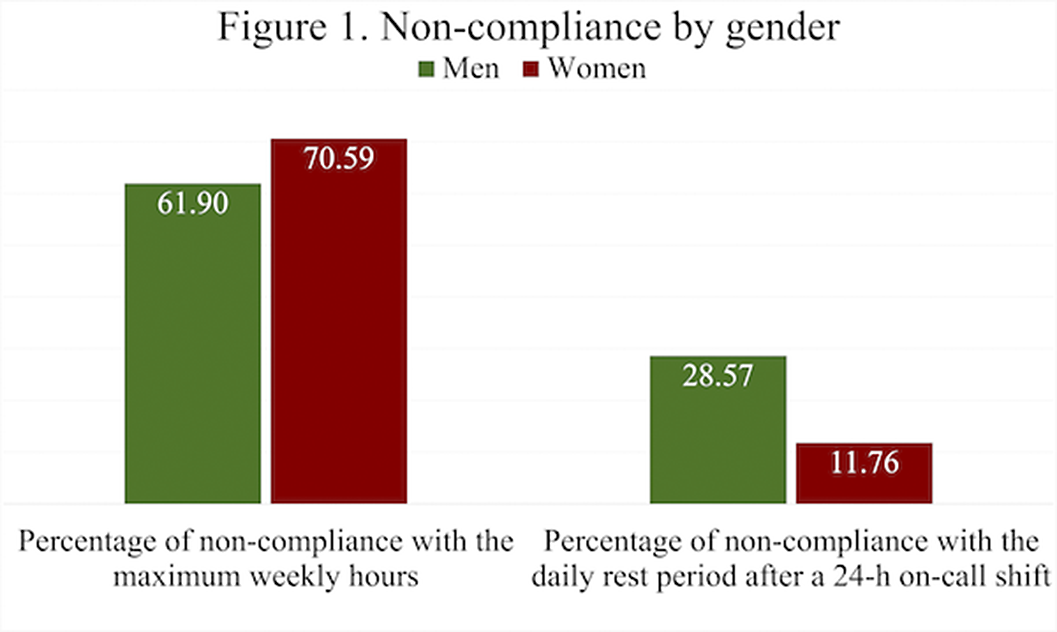
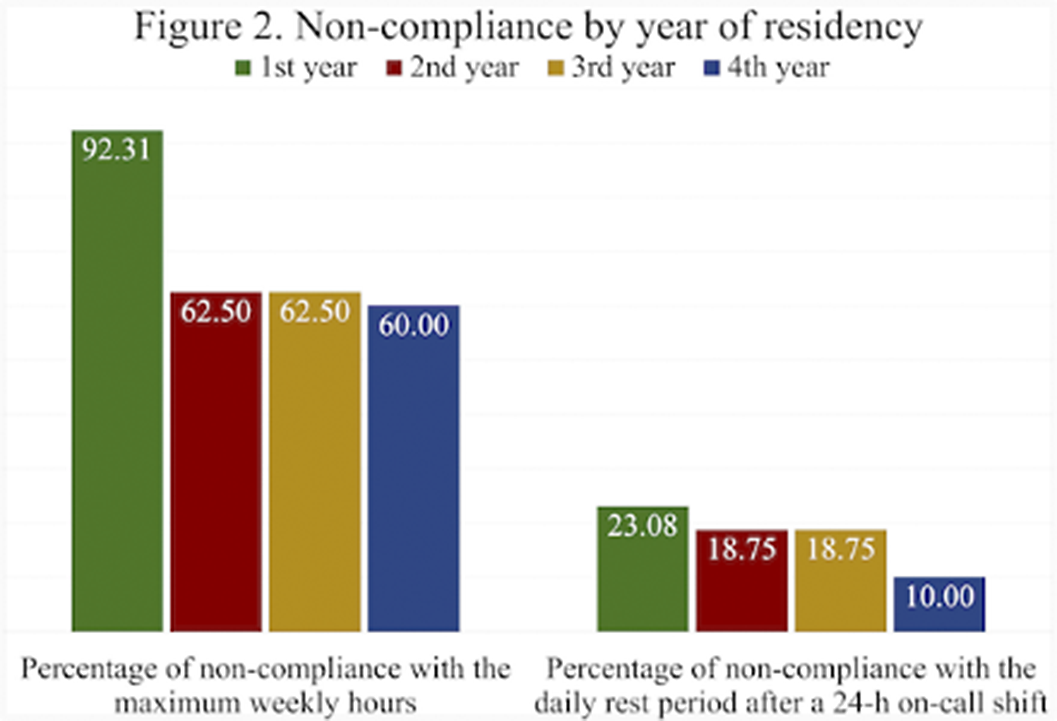
Psychiatry resident physician duty hours, resting times and European Working Time Directive compliance in Spain
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S393-S394
-
- Article
-
- You have access
- Open access
- Export citation
Prevalence of diabetes and insulin resistance in patients with diagnosis of schizophrenia or other psicotic disorders
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S741
-
- Article
-
- You have access
- Open access
- Export citation
Lithium withdrawal and relapse in bipolar disorder when kidney function deteriorates
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S427-S428
-
- Article
-
- You have access
- Open access
- Export citation
Delusional parasitosis: the importance of a multidisciplinary approach
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S750
-
- Article
-
- You have access
- Open access
- Export citation
The Recovery concept in Assertive Community Treatment: Truth or Fake?
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S715-S716
-
- Article
-
- You have access
- Open access
- Export citation
Intractable Singultus: Causes, diagnosis and treatment. A case report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S496
-
- Article
-
- You have access
- Open access
- Export citation
From adjustment disorder to schizotypal personality disorder
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S652-S653
-
- Article
-
- You have access
- Open access
- Export citation