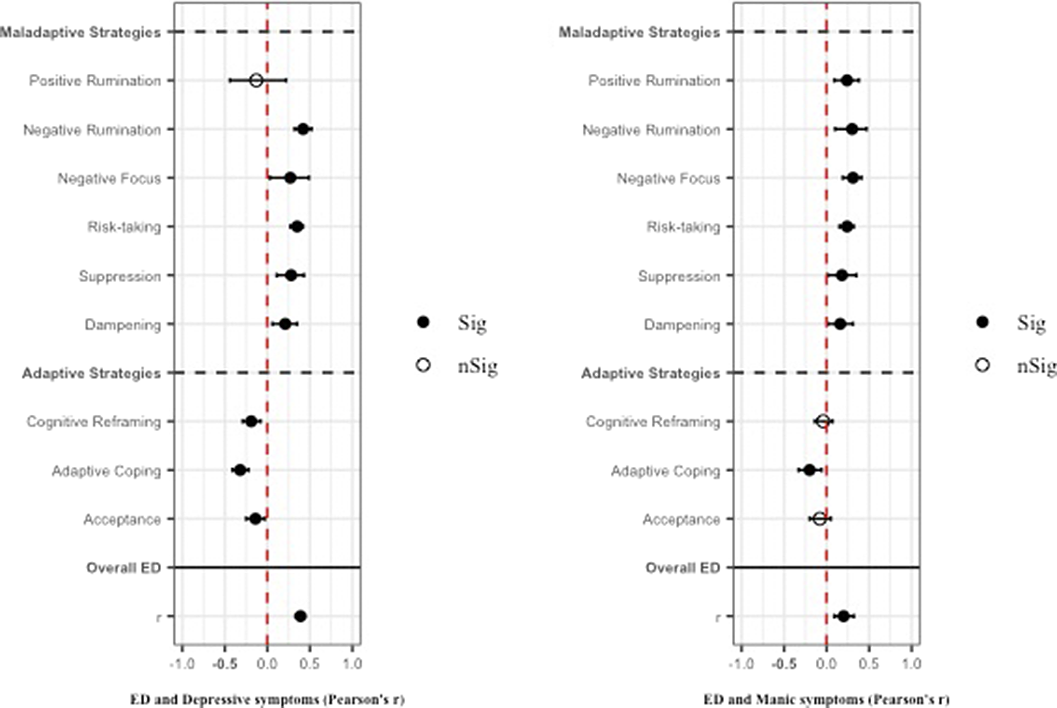
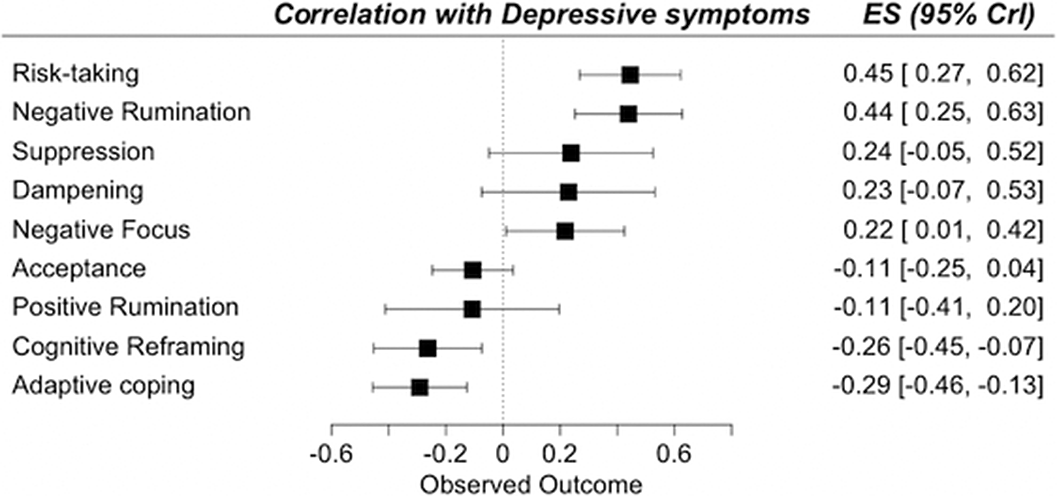
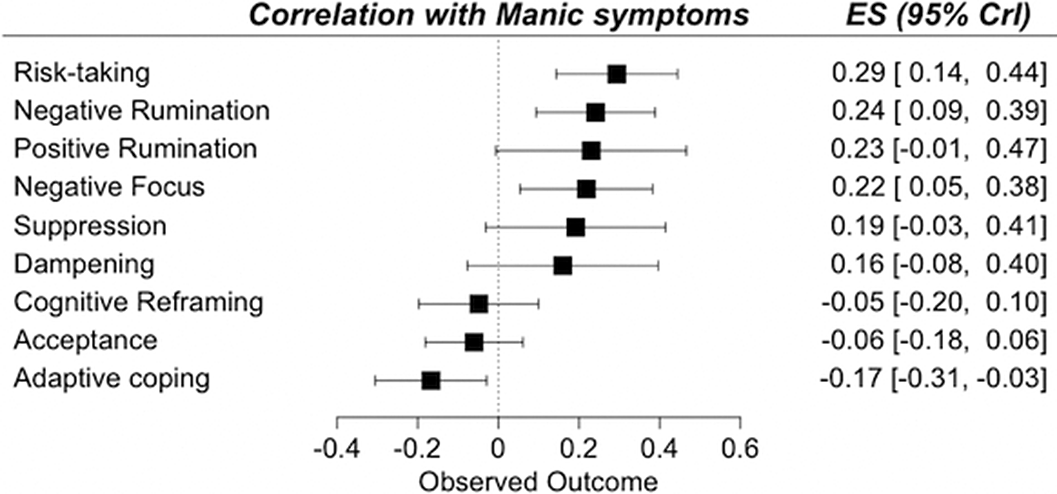
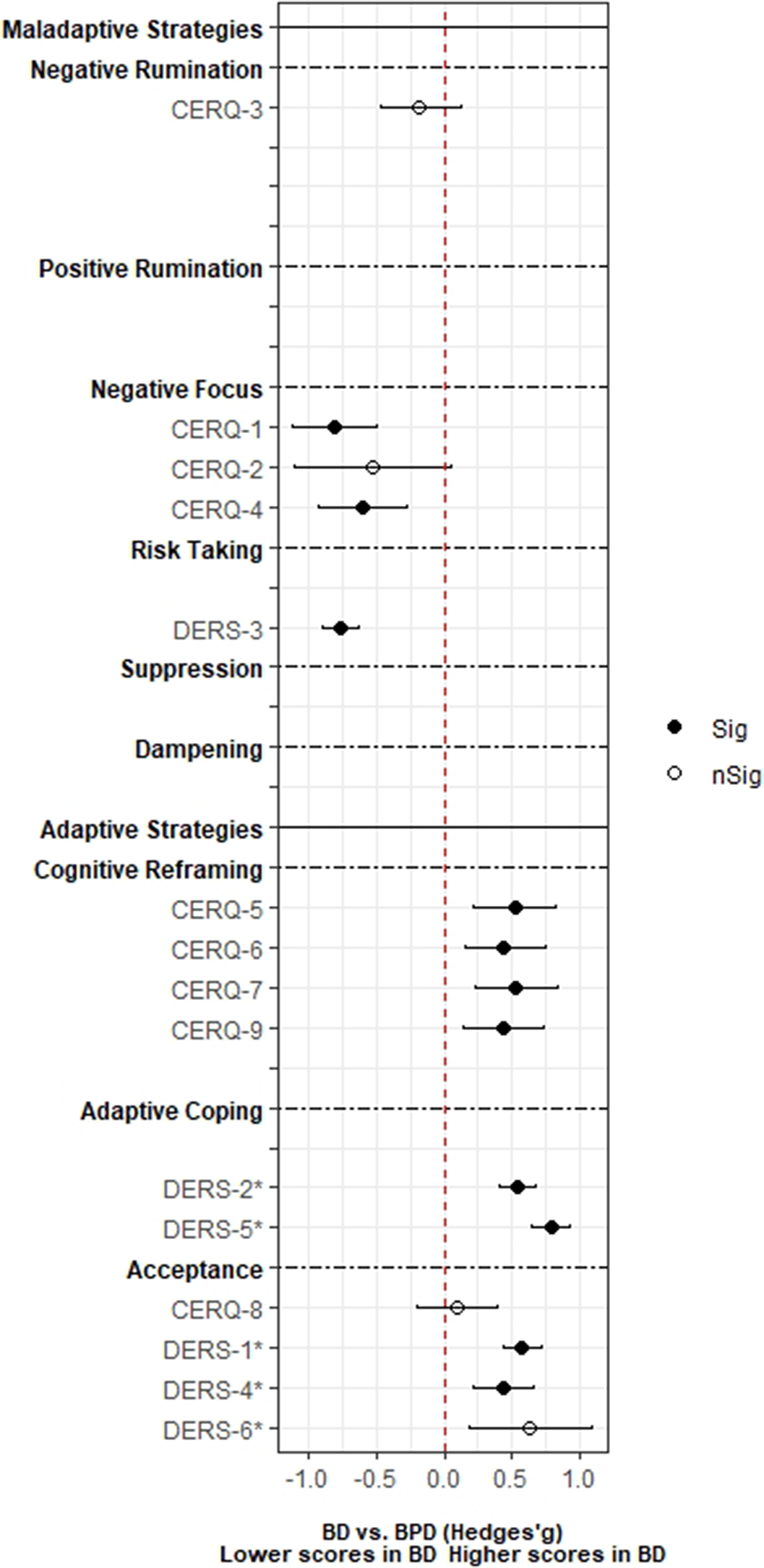
ResultsA total of 3,239 records was identified and, after duplicate removal and title/abstract evaluation, 112 were explored at the full text. Twenty-nine studies were finally included, and it was possible to perform a meta-analysis with twenty-two (145 comparisons) of them. Only studies comparing BD with MDD, and BPD provided sufficient data to perform a meta-analysis. People with BD did not differ from people with MDD in most of the comparisons considered. However, BD patients presented higher positive rumination (two comparisons: SMD=0.46; CI=0.27, 0.64; p=8.5e-07; I2=0%; and SMD=0.34; CI=0.15, 0.52; p=2.7e-04; I2=0%) and risk-taking behaviors (SMD=0.48; CI=0.27, 0.69; p=8.11e-06; I2=0%). In contrast, people with BPD displayed an overall higher degree of ED (SMD=-1.22; CI=-1.94, -0.5; p=9.1e-04; I2= 90.7) and used fewer adaptive ER strategies. Additionally, higher levels of self-blaming (SMD=-0.80; CI=-1.11, -0.50; p=2.68e-07; I2=0) and impulsive behavior (SMD=-0.76; CI=-0.89, -0.63; p=5.4e-29; I2=0) were observed.
Image:
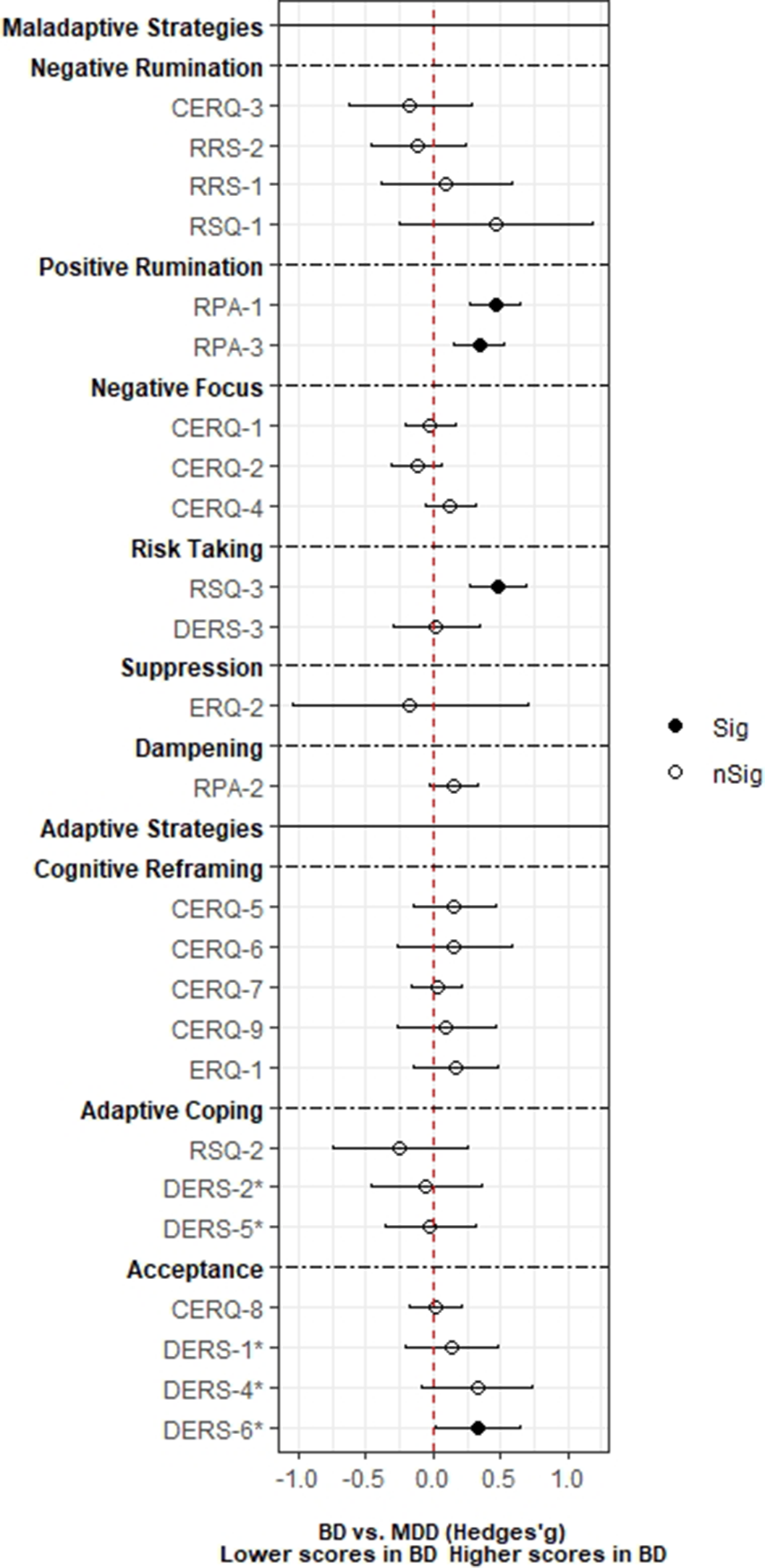
Image 2:
Disclosure of InterestM. De Prisco: None Declared, V. Oliva: None Declared, G. Fico Grant / Research support from: “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), Consultant of: Angelini, Janssen-Cilag and Lundbeck, J. Radua Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00394, CPII19/00009) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER) and the Instituto de Salud Carlos III, I. Grande Grant / Research support from: Spanish Ministry of Science and Innovation (MCIN) (PI19/00954) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIII-Subdirección General de Evaluación y el Fondos Europeos de la Unión Europea (FEDER, FSE, Next Generation EU/Plan de Recuperación Transformación y Resiliencia_PRTR ); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); and the the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), CERCA Programme / Generalitat de Catalunya as well as the Fundació Clínic per la Recerca Biomèdica (Pons Bartran 2022-FRCB_PB1_2022), Consultant of: ADAMED, Angelini, Casen Recordati, Ferrer, Janssen Cilag, and Lundbeck, Lundbeck-Otsuka, Luye, SEI Healthcare, N. Roberto: None Declared, G. Anmella Grant / Research support from: Rio Hortega 2021 grant (CM21/00017) from the Spanish Ministry of Health financed by the Instituto de Salud Carlos III (ISCIII) and co-financed by the Fondo Social Europeo Plus (FSE+), Consultant of: Janssen-Cilag, Lundbeck, Lundbeck/Otsuka, and Angelini, D. Hidalgo-Mazzei Grant / Research support from: Juan Rodés JR18/00021 granted by the Instituto de Salud Carlos III (ISCIII), M. Fornaro: None Declared, A. de Bartolomeis Consultant of: Janssen, Lundbeck, and Otsuka and lecture fees for educational meeting from Chiesi, Lundbeck, Roche, Sunovion, Vitria, Recordati, Angelini and Takeda; he has served on advisory boards for Eli Lilly, Jansen, Lundbeck, Otsuka, Roche, and Takeda, Chiesi, Recordati, Angelini, Vitria, A. Serretti Consultant of: Abbott, Abbvie, Angelini, AstraZeneca, Clinical Data, Boehringer, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Innovapharma, Italfarmaco, Janssen, Lundbeck, Naurex, Pfizer, Polifarma, Sanofi, Servier, and Taliaz, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/00805, PI21/00787) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357. Thanks the support of the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), Consultant of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Medincell, Novartis, Orion Corporation, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), Consultant of: Angelini, Idorsia, Lundbeck, Pfizer, Takeda