Extensive evidence indicates that exposure to childhood trauma or other adversities is associated with increased risk of subsequent psychotic experiences. Reference Trotta, Murray and Fisher1 In a recent analysis of data from the World Health Organization (WHO) World Mental Health (WMH) surveys, McGrath et al Reference McGrath, McLaughlin, Saha, Aguilar-Gaxiola, Al-Hamzawi and Alonso2 found that childhood adversities, such as sexual or physical abuse, were associated with increased risks of subsequent psychotic experiences even after adjustment for lifetime comorbid mental disorders. Exposure to traumatic events later in life has also been linked to increased risk of subsequent psychotic experiences. Cross-sectional Reference Beards, Gayer-Anderson, Borges, Dewey, Fisher and Morgan3 and longitudinal Reference Kelleher, Harley, Lynch, Arseneault, Fitzpatrick and Cannon4,Reference Spauwen, Krabbendam, Lieb, Wittchen and van Os5 studies have found especially high psychotic experience risk associated with traumatic events involving interpersonal violence. Reference Saha, varghese, Slade, Degenhardt, Mills and McGrath6,Reference Jenkins, Mbatia, Singleton and White7 There is also evidence of a dose–response relationship between number of traumatic events and risk of subsequent psychotic experiences. Reference Saha, varghese, Slade, Degenhardt, Mills and McGrath6,Reference Scott, Chant, Andrews, Martin and McGrath8 However, many traumatic events are predicted by prior mental disorders and associated with an increased risk of subsequent mental disorders, most notably post-traumatic stress disorder (PTSD). Reference Kessler, McLaughlin, Koenen, Petukhova and Hill9–Reference Karam, Friedman, Hill, Kessler, McLaughlin and Petukhova11 We recently demonstrated that the associations of psychotic experiences with mental disorders (including PTSD) are often bidirectional. Reference McGrath, Saha, Al-Hamzawi, Andrade, Benjet and Bromet12 Thus, it seems reasonable to hypothesise that the associations of traumatic events with subsequent onset of psychotic experiences might be influenced by comorbid mental disorders. Reference Soosay, Silove, Bateman-Steel, Steel, Bebbington and Jones13 This could be true either because lifetime mental disorders with onsets prior to traumatic events are associated both with increased risk of subsequent traumatic event exposure (such as bipolar disorder associated with increased risk of interpersonal violence, attention-deficit hyperactivity disorder (ADHD) associated with increased risk of motor vehicle collisions) and because traumatic events are associated with increased risk of subsequent mental disorders (both PTSD and other disorders). The main aim of this study was to examine the associations of type and number of traumatic events with the subsequent onset of psychotic experiences across 16 WMH countries and to evaluate the extent to which these associations were explained statistically by PTSD and other mental disorders.
Method
Samples
The WMH surveys are a coordinated set of community epidemiological surveys administered in probability samples of the non-institutionalised civilian household population in countries throughout the world (www.hcp.med.harvard.edu/WMH). Reference Kessler and Ustun14 We examined data from 16 WMH surveys that included both a psychosis module and items related to trauma exposure. These 16 countries are distributed across North and South America (Colombia, Mexico, Peru, Brazil, USA); Africa (Nigeria); the Middle East (Lebanon); the South Pacific (New Zealand) and Europe (Belgium, France, Germany, Italy, The Netherlands, Portugal, Romania, Spain). The majority of these surveys were based on multistage, clustered area probability household sampling designs, the exceptions being Belgium, Germany and Italy, which used municipal resident registries to select respondents (online Table DS1). The weighted (by sample size) average response rate across all 16 surveys was 70.5%.
In keeping with previous studies of psychotic experiences, Reference McGrath, McLaughlin, Saha, Aguilar-Gaxiola, Al-Hamzawi and Alonso2,Reference Saha, varghese, Slade, Degenhardt, Mills and McGrath6,Reference McGrath, Saha, Al-Hamzawi, Andrade, Benjet and Bromet12 we made the a priori decision to exclude individuals reporting psychotic experiences who screened positive for possible schizophrenia/psychosis and manic depression/mania (i.e. respondents who were either told by a doctor that their psychotic experiences were caused by these conditions or who were treated with antipsychotic medications for these symptoms). This resulted in excluding 130 respondents (0.5% of all respondents), leaving 24 464 respondents for this study (online Table DS1).
Procedures
All WMH interviews were conducted face-to-face by trained lay interviewers in the homes of respondents. Informed consent was obtained before beginning the interview. Procedures for obtaining informed consent and data protection (ethical approvals) were reviewed and approved by the institutional review boards of the collaborating organisations in each country. Reference Kessler and Ustun15 Standardised interviewer training and quality control procedures were used consistently in the surveys. All WMH interviews had two parts. Part I, administered to all respondents, contained assessments related to core mental disorders (depression, mania, panic disorder, social phobia, specific phobia, agoraphobia, generalised anxiety disorder, substance use). Part II, which included other mental disorders, traumatic events and psychotic experiences, was administered to respondents who met lifetime criteria for any part I disorder and a random proportion of the rest. Respondents in the part II sample were weighted by the inverse of their probability of selection to restore representativeness. Additional weights were used to adjust for differential probabilities of selection within households, non-response and to match the samples to population sociodemographic distributions. Reference Kessler and Ustun15
Data collection and data items
The instrument used in the WMH surveys was the WHO Composite International Diagnostic Interview (CIDI), Reference Kessler and Ustun15 a validated fully structured diagnostic interview (https://www.hcp.med.harvard.edu/wmhcidi/download-the-who-wmh-cidi-instruments/) designed to assess the prevalence and correlates of a wide range of mental disorders according to the definitions and criteria of both the DSM-IV and ICD-10 diagnostic systems. 16,17 DSM-IV criteria are used in the current report. WHO translation, back-translation and harmonisation protocols were used to adapt the CIDI for use in each participating country.
Psychotic experiences
The psychosis module included questions about six psychotic experience types – two related to hallucinatory experiences and four related to delusional experiences (online Tables DS2, DS3). The respondents were asked if they ever experienced each psychotic experience (for example ‘Have you ever seen something that wasn't there that other people could not see?’; ‘Have you ever heard any voices that other people said did not exist?’ etc.). Only psychotic experiences occurring when the person was ‘not dreaming, not half-asleep, or not under the influence of alcohol or drugs’ were included. For those with psychotic experiences, age at onset of psychotic experiences was also assessed.
Mental disorders
The WMH version of the CIDI assessed lifetime history of 21 mental disorders including mood disorders, anxiety disorders, behaviour disorders, eating disorder, and substance use disorders (online Table DS4). Clinical reappraisal studies indicate that lifetime diagnoses based on the CIDI have good concordance with diagnoses based on masked clinical interviews. Reference Haro, Arbabzadeh-Bouchez, Brugha, de Girolamo, Guyer and Jin18
Traumatic experiences
The CIDI assessed 29 traumatic events that have been broadly classified into six categories. Details of these categories have been published elsewhere. Reference Benjet, Bromet, Karam, Kessler, McLaughlin and Ruscio19 These categories are: (a) collective violence (civilian in a war zone, refugee, civilian in region of terror, kidnapped, and relief worker in war zone); (b) caused/witnessed bodily harm (purposely injured, tortured, or killed someone, combat experience, accidentally caused serious injury or death, saw atrocities, and witnessed death/dead body or saw someone seriously hurt); (c) interpersonal violence (beaten up by caregiver, witnessed physical fight at home, and beaten up by someone else); (d) intimate partner/sexual violence (raped, sexually assaulted, beaten up by spouse/romantic partner, stalked, traumatic event to loved one, private event, and some other event); (e) accidents/injuries (child with serious illness, natural disaster, life-threatening illness, toxic chemical exposure, other life-threatening accident, and automobile accident); and (f) other traumas (unexpected death of a loved one, mugged or threatened with a weapon, and man-made disaster). Information on age at first exposure associated with each traumatic event was also collected. Of note, this study extends our previous report on the subset of traumatic events that occurred in childhood Reference McGrath, McLaughlin, Saha, Aguilar-Gaxiola, Al-Hamzawi and Alonso2 by evaluating the impact of traumatic events occurring across the lifespan.
Statistical analysis
Lifetime prevalence of each traumatic event was calculated using cross-tabulation. Discrete-time survival analysis with person-year as the unit of analysis was used to investigate the associations of exposure to traumatic events with the subsequent first onset of psychotic experiences. A person-year data-set was created such that each year in the life of each respondent (up to and including the age at onset of psychotic experience or their age at interview, whichever came first) was treated as a separate observational record. In all analyses the year of psychotic experience onset was coded as 1 and earlier years coded as 0 on a dichotomous outcome variable. Traumatic events were coded as 1 only beginning the year after the onset of traumatic events to ensure that we were not including onsets of traumatic event and psychotic experience occurring in the same year or traumatic events occurring after psychotic experience onset. We estimated 29 bivariate models (i.e. considering only 1 traumatic event type out of 29 types at a time) in predicting psychotic experiences adjusting for age-cohort, gender, person-year dummy variables, and country. We then estimated a series of multivariate models: (a) model 1 included all traumatic events simultaneously as predictors without considering the number of traumatic events (type model); (b) model 2 included number of traumatic events coded as dummy variables (exactly 1, exactly 2, …, 5 or more traumatic events) without any information on type of traumatic events (number model); (c) model 3 included both type and number of traumatic events (simple interactive model); and (d) model 4 included type and number of traumatic events along with a separate interaction term between each type and each number of other co-occurring traumatic events (complex interactive model). The latter models showed the ‘marginal effects’ of each type of traumatic event, where a marginal effect is the ‘partial derivative effect’ (a unique contribution) of a specific traumatic event to psychotic experiences while the contribution from all other traumatic events remains constant. Owing to the co-occurring nature of traumatic events, it is difficult to fractionate the impact of individual traumatic events on psychotic experiences using models 1–3. While model 3 assumed simple interactions, model 4 allowed each type of traumatic event to vary in slope as a function of number of co-occurring traumatic events. The model with the best fit to the data according to the Akaike information criterion (AIC) was carried forward into subsequent examination of the extent to which associations of traumatic events with subsequent psychotic experiences changed when we adjusted for history of PTSD (model 5) and also other temporally prior (to the psychotic experience) mental disorders (model 6).
As the WMH data are both clustered and weighted, the design-based Taylor series linearisation implemented in SUDAAN software was used to estimate standard errors and evaluate the statistical significance of coefficients. Survival coefficients were exponentiated and reported as odds ratios. All significance tests were evaluated using 0.05-level two-sided tests.
Results
Prevalence of traumatic events in those with and without psychotic experiences
Of the 24 464 respondents, more than two-thirds (n = 18 535, 71.8%) reported exposure to at least one traumatic event in their lifetime (online Table DS5). The lifetime prevalence of traumatic event exposure among respondents with psychotic experiences was 90.4% compared with 70.5% in those with no psychotic experiences. Among respondents with psychotic experiences, there was a wide variation in the frequency of exposure to specific types of traumatic events, with the highest prevalence reported for unexpected death of a loved one (45.6%) followed by witnessed death or saw someone seriously hurt (41.8%), and mugged or threatened with weapon (29.9%). In this sample, more than three-quarters (75.8%) of the traumatic events occurred before the onset of psychotic experiences, whereas only 19.2% occurred after psychotic experience onset (χ2 1 = 337.3, P< 0.001) (online Table DS5).
The associations of type and number of traumatic events with psychotic experiences
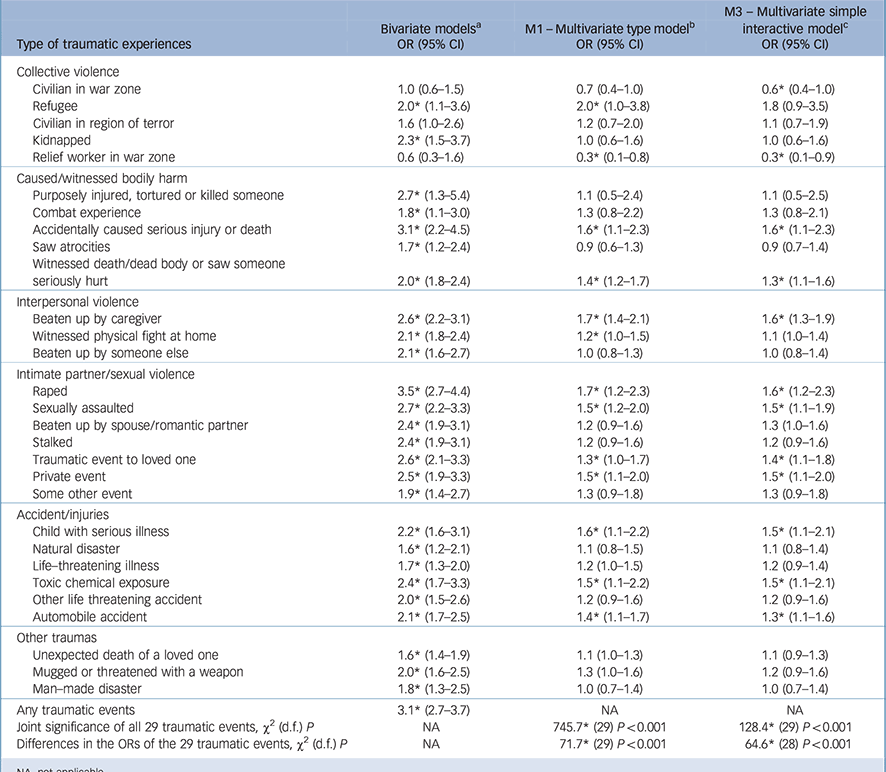
Tables 1 and 2 summarise the bivariate and multivariable associations of type and number of traumatic events with subsequent first onset of psychotic experiences. Overall, respondents with any traumatic event had threefold increased odds of subsequent onset of psychotic experiences (OR = 3.1, 95% CI 2.7–3.7) compared with respondents with no traumatic events. In the bivariate models, all but three traumatic event types (civilian in war zone or region of terror, and relief worker in war zone) were significantly associated with elevated odds of subsequent psychotic experiences. The significant odds ratios ranged between 1.6 and 3.5 with the highest being associated with rape (OR = 3.5, 95% CI 2.7–4.4), and the lowest with unexpected death of a loved one (OR = 1.6, 95% CI 1.4–1.9) and natural disaster (OR = 1.6, 95% CI 1.2–2.1).
Table 1 Bivariate and multivariate associations of temporally prior traumatic experiences with subsequent onset of psychotic experiences
| Type of traumatic experiences | Bivariate models
a
OR (95% CI) |
M1 – Multivariate type model
b
OR (95% CI) |
M3 – Multivariate simple interactive model c OR (95% CI) |
|---|---|---|---|
| Collective violence | |||
| Civilian in war zone | 1.0 (0.6–1.5) | 0.7 (0.4–1.0) | 0.6* (0.4–1.0) |
| Refugee | 2.0* (1.1–3.6) | 2.0* (1.0–3.8) | 1.8 (0.9–3.5) |
| Civilian in region of terror | 1.6 (1.0–2.6) | 1.2 (0.7–2.0) | 1.1 (0.7–1.9) |
| Kidnapped | 2.3* (1.5–3.7) | 1.0 (0.6–1.6) | 1.0 (0.6–1.6) |
| Relief worker in war zone | 0.6 (0.3–1.6) | 0.3* (0.1–0.8) | 0.3* (0.1–0.9) |
| Caused/witnessed bodily harm | |||
| Purposely injured, tortured or killed someone | 2.7* (1.3–5.4) | 1.1 (0.5–2.4) | 1.1 (0.5–2.5) |
| Combat experience | 1.8* (1.1–3.0) | 1.3 (0.8–2.2) | 1.3 (0.8–2.1) |
| Accidentally caused serious injury or death | 3.1* (2.2–4.5) | 1.6* (1.1–2.3) | 1.6* (1.1–2.3) |
| Saw atrocities | 1.7* (1.2–2.4) | 0.9 (0.6–1.3) | 0.9 (0.7–1.4) |
| Witnessed death/dead body or saw someone seriously hurt |
2.0* (1.8–2.4) | 1.4* (1.2–1.7) | 1.3* (1.1–1.6) |
| Interpersonal violence | |||
| Beaten up by caregiver | 2.6* (2.2–3.1) | 1.7* (1.4–2.1) | 1.6* (1.3–1.9) |
| Witnessed physical fight at home | 2.1* (1.8–2.4) | 1.2* (1.0–1.5) | 1.1 (1.0–1.4) |
| Beaten up by someone else | 2.1* (1.6–2.7) | 1.0 (0.8–1.3) | 1.0 (0.8–1.4) |
| Intimate partner/sexual violence | |||
| Raped | 3.5* (2.7–4.4) | 1.7* (1.2–2.3) | 1.6* (1.2–2.3) |
| Sexually assaulted | 2.7* (2.2–3.3) | 1.5* (1.2–2.0) | 1.5* (1.1–1.9) |
| Beaten up by spouse/romantic partner | 2.4* (1.9–3.1) | 1.2 (0.9–1.6) | 1.3 (1.0–1.6) |
| Stalked | 2.4* (1.9–3.1) | 1.2 (0.9–1.6) | 1.2 (0.9–1.6) |
| Traumatic event to loved one | 2.6* (2.1–3.3) | 1.3* (1.0–1.7) | 1.4* (1.1–1.8) |
| Private event | 2.5* (1.9–3.3) | 1.5* (1.1–2.0) | 1.5* (1.1–2.0) |
| Some other event | 1.9* (1.4–2.7) | 1.3 (0.9–1.8) | 1.3 (0.9–1.8) |
| Accident/injuries | |||
| Child with serious illness | 2.2* (1.6–3.1) | 1.6* (1.1–2.2) | 1.5* (1.1–2.1) |
| Natural disaster | 1.6* (1.2–2.1) | 1.1 (0.8–1.5) | 1.1 (0.8–1.4) |
| Life–threatening illness | 1.7* (1.3–2.0) | 1.2 (1.0–1.5) | 1.2 (0.9–1.4) |
| Toxic chemical exposure | 2.4* (1.7–3.3) | 1.5* (1.1–2.2) | 1.5* (1.1–2.1) |
| Other life threatening accident | 2.0* (1.5–2.6) | 1.2 (0.9–1.6) | 1.2 (0.9–1.6) |
| Automobile accident | 2.1* (1.7–2.5) | 1.4* (1.1–1.7) | 1.3* (1.1–1.6) |
| Other traumas | |||
| Unexpected death of a loved one | 1.6* (1.4–1.9) | 1.1 (1.0–1.3) | 1.1 (0.9–1.3) |
| Mugged or threatened with a weapon | 2.0* (1.6–2.5) | 1.3 (1.0–1.6) | 1.2 (0.9–1.6) |
| Man–made disaster | 1.8* (1.3–2.5) | 1.0 (0.7–1.4) | 1.0 (0.7–1.4) |
| Any traumatic events | 3.1* (2.7–3.7) | NA | NA |
| Joint significance of all 29 traumatic events, χ2 (d.f.) P | NA | 745.7* (29) P<0.001 | 128.4* (29) P<0.001 |
| Differences in the ORs of the 29 traumatic events, χ2 (d.f.) P | NA | 71.7* (29) P< 0.001 | 64.6* (28) P< 0.001 |
NA, not applicable
a. Each lifetime traumatic event type was used as a predictor of psychotic experiences onset in separate discrete-time survival model controlling for age-cohorts, gender, person-year dummies, and country
b. Model was estimated with dummy variables for all temporally prior traumatic events entered simultaneously including the controls specifed above
c. Model was estimated with dummy variables for type and number of traumatic events (starting at 2 traumatic events, 3 traumatic events, …, 5 or more traumatic events) entered simultaneously as predictors of psychotic experiences onset including the controls specifed in (a)
* P<0.05, 2–sided test
Table 2 Associations between number of temporally prior traumatic experiences and the subsequent onset of psychotic experiences
| M2 – Multivariate number model
a
OR (95% CI) |
M3 – Multivariate simple interactive model
b
OR (95% CI) |
|
|---|---|---|
| 1 traumatic event | 2.3* (1.9–2.8) | – |
| 2 traumatic events | 3.5* (2.8–4.4) | 1.7* (1.4–2.1) |
| 3 traumatic events | 4.0* (3.1–5.1) | 1.5* (1.1–2.0) |
| 4 traumatic events | 5.0* (3.8–6.7) | 1.5* (1.1–2.2) |
| 5 or more traumatic events | 7.6* (6.1–9.5) | 1.3 (0.8–2.1) |
| Joint significance of number–of–traumatic event measures χ2 (d.f.) P |
355.9* (5) P< 0.001 | 34.0* (4) P<0.001 |
a Model was estimated with dummy variables for all number of traumatic events without any information about type of traumatic events entered simultaneously controlling for age–cohorts, gender, person–year dummies, and country
b Model was estimated with dummy variables for type and number of traumatic events (starting at 2 traumatic events, 3 traumatic events, …, 5 or more traumatic events) entered simultaneously as predictors of psychotic experiences onset including the controls specifed in (a).
* P<0.05, 2–sided test.
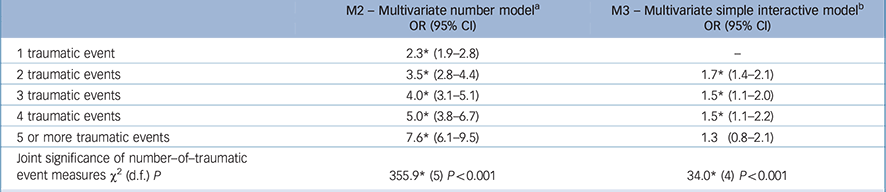
In model 1, which adjusted for all traumatic events types, 13 of the 29 traumatic event types were significantly associated with onset of psychotic experiences, with odds ratios ranging from 0.3 (95% CI = 0.1–0.8) for relief worker in a war zone to 2.0 (95% CI = 1.0–3.8) for being a refugee. As a set, traumatic events were significantly associated with psychotic experiences (χ2 29 = 745.7, P<0.001), and there was significant variation in the magnitude of associations across traumatic events (χ2 28 = 71.7, P< 0.001). With respect to the number of traumatic events (Table 2, model 2), a dose-response relationship between traumatic events and psychotic experiences, was evident with the odds ratios increasing monotonically as exposure to traumatic events increased (χ2 5 = 355.9, P<0.001).
In model 3, which adjusted for both type and number of traumatic events, 12 traumatic events were significantly associated with psychotic experiences: 10 with increased odds of subsequent psychotic experiences whereas two traumatic events (‘relief worker in war zone’, ‘civilian in war zone’) were protective with respect to subsequent psychotic experience onset. The odds ratio associated with number of traumatic events were consistently elevated and in the range 1.7–1.3 (Table 2, model 3), indicating that the relative odds of subsequently having psychotic experiences among respondents with more than one prior traumatic event were between 1.7 and 1.3 times the relative odds implied by multiplying together the marginal odds ratios. For example, a respondent who had been exposed to beaten by caregiver, raped, sexually assaulted, and an automobile accident would have an expected odds ratio of subsequent psychotic experiences of 5.0 compared with someone with no traumatic event exposure (i.e. 1.6 × 1.6 × 1.5 × 1.3). Given that the number of possible traumatic event interaction combinations (229–30 = 536 870 911) greatly exceeded the number of observations, model 3 makes the simplifying assumption that the odds ratios describing interactions are identical for all co-occurring traumatic events involving the same number of traumatic events. However, we found that the test for variation in odds ratios was significant (χ2 28 = 64.6, P<0.001), indicating variation across traumatic event types in the interaction of traumatic event type and number of other traumatic events in predicting psychotic experiences. Thus, we next evaluated a more complex interactive model (model 4) that considered distinct interactions for specific traumatic events together with number of other co-occurring traumatic events.
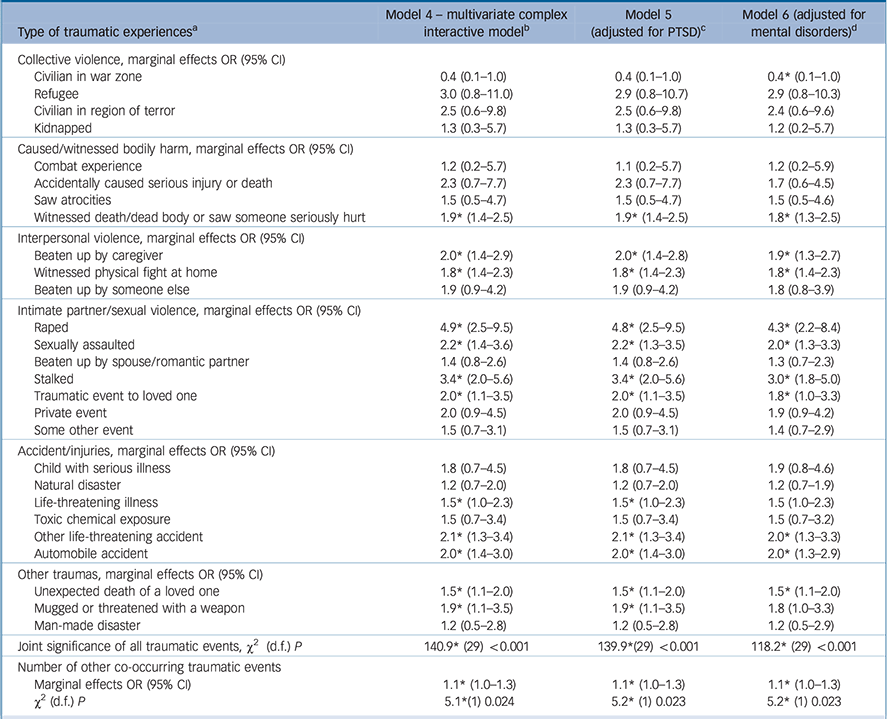
Table 3 presents a set of complex interactive models with both type and number of traumatic events (model 4) as well as models adjusted for mental disorders (models 5 and 6). Twelve traumatic events were significantly associated with psychotic experience onset in the ‘marginal effects’ models. Interestingly, several traumatic events showed stronger associations with psychotic experience in this model. For example, those who endorsed ‘raped’ had about fivefold increased odds of subsequent onset of psychotic experiences (OR = 4.9, 95% CI 2.5–9.5). The ‘marginal effect’ for number of traumatic events was significant (χ2 1 = 5.1, P = 0.024). The result shows that for every one-unit increment of number of traumatic events, we expect a 10% increase in the odds of subsequent onset of psychotic experiences regardless of the type of traumatic events (OR = 1.1, 95% CI 1.0–1.3).
Table 3 Multivariate associations of traumatic experiences with the subsequent first onset of psychotic experiences, with and without adjustment for prior and intervening mental disorders
| Type of traumatic experiences a | Model 4 – multivariate complex interactive model b |
Model 5 (adjusted for PTSD) c |
Model 6 (adjusted for mental disorders) d |
|---|---|---|---|
| Collective violence, marginal effects OR (95% CI) | |||
| Civilian in war zone | 0.4 (0.1–1.0) | 0.4 (0.1–1.0) | 0.4* (0.1–1.0) |
| Refugee | 3.0 (0.8–11.0) | 2.9 (0.8–10.7) | 2.9 (0.8–10.3) |
| Civilian in region of terror | 2.5 (0.6–9.8) | 2.5 (0.6–9.8) | 2.4 (0.6–9.6) |
| Kidnapped | 1.3 (0.3–5.7) | 1.3 (0.3–5.7) | 1.2 (0.2–5.7) |
| Caused/witnessed bodily harm, marginal effects OR (95% CI) | |||
| Combat experience | 1.2 (0.2–5.7) | 1.1 (0.2–5.7) | 1.2 (0.2–5.9) |
| Accidentally caused serious injury or death | 2.3 (0.7–7.7) | 2.3 (0.7–7.7) | 1.7 (0.6–4.5) |
| Saw atrocities | 1.5 (0.5–4.7) | 1.5 (0.5–4.7) | 1.5 (0.5–4.6) |
| Witnessed death/dead body or saw someone seriously hurt | 1.9* (1.4–2.5) | 1.9* (1.4–2.5) | 1.8* (1.3–2.5) |
| Interpersonal violence, marginal effects OR (95% CI) | |||
| Beaten up by caregiver | 2.0* (1.4–2.9) | 2.0* (1.4–2.8) | 1.9* (1.3–2.7) |
| witnessed physical fight at home | 1.8* (1.4–2.3) | 1.8* (1.4–2.3) | 1.8* (1.4–2.3) |
| Beaten up by someone else | 1.9 (0.9–4.2) | 1.9 (0.9–4.2) | 1.8 (0.8–3.9) |
| Intimate partner/sexual violence, marginal effects OR (95% CI) | |||
| Raped | 4.9* (2.5–9.5) | 4.8* (2.5–9.5) | 4.3* (2.2–8.4) |
| Sexually assaulted | 2.2* (1.4–3.6) | 2.2* (1.3–3.5) | 2.0* (1.3–3.3) |
| Beaten up by spouse/romantic partner | 1.4 (0.8–2.6) | 1.4 (0.8–2.6) | 1.3 (0.7–2.3) |
| Stalked | 3.4* (2.0–5.6) | 3.4* (2.0–5.6) | 3.0* (1.8–5.0) |
| Traumatic event to loved one | 2.0* (1.1–3.5) | 2.0* (1.1–3.5) | 1.8* (1.0–3.3) |
| Private event | 2.0 (0.9–4.5) | 2.0 (0.9–4.5) | 1.9 (0.9–4.2) |
| Some other event | 1.5 (0.7–3.1) | 1.5 (0.7–3.1) | 1.4 (0.7–2.9) |
| Accident/injuries, marginal effects OR (95% CI) | |||
| Child with serious illness | 1.8 (0.7–4.5) | 1.8 (0.7–4.5) | 1.9 (0.8–4.6) |
| Natural disaster | 1.2 (0.7–2.0) | 1.2 (0.7–2.0) | 1.2 (0.7–1.9) |
| Life-threatening illness | 1.5* (1.0–2.3) | 1.5* (1.0–2.3) | 1.5 (1.0–2.3) |
| Toxic chemical exposure | 1.5 (0.7–3.4) | 1.5 (0.7–3.4) | 1.5 (0.7–3.2) |
| Other life-threatening accident | 2.1* (1.3–3.4) | 2.1* (1.3–3.4) | 2.0* (1.3–3.3) |
| Automobile accident | 2.0* (1.4–3.0) | 2.0* (1.4–3.0) | 2.0* (1.3–2.9) |
| Other traumas, marginal effects OR (95% CI) | |||
| Unexpected death of a loved one | 1.5* (1.1–2.0) | 1.5* (1.1–2.0) | 1.5* (1.1–2.0) |
| Mugged or threatened with a weapon | 1.9* (1.1–3.5) | 1.9* (1.1–3.5) | 1.8 (1.0–3.3) |
| Man-made disaster | 1.2 (0.5–2.8) | 1.2 (0.5–2.8) | 1.2 (0.5–2.9) |
| Joint significance of all traumatic events, χ2 (d.f.) P | 140.9* (29) <0.001 | 139.9* (29) <0.001 | 118.2* (29) <0.001 |
| Number of other co-occurring traumatic events | |||
| Marginal effects OR (95% CI) | 1.1* (1.0–1.3) | 1.1* (1.0–1.3) | 1.1* (1.0–1.3) |
| χ2 (d.f.) P | 5.1*(1) 0.024 | 5.2* (1) 0.023 | 5.2* (1) 0.023 |
a. The traumatic events: ‘Relief worker in war zone’ and ‘Purposely injured, tortured, or killed someone’ are not included in the table as the results are not applicable because of unstable estimates. Total person-years used for this multivariate model is 1 041 109.
b. Complex interactive model was estimated with dummy variables for type and number of temporally prior traumatic events and interaction terms for each type of traumatic events and number of other traumatic events including the controls: age-cohorts, gender, person-year dummies, and country.
c. Model specifcation in (b) and additionally control for temporally prior post-traumatic stress disorder (PTSD) only.
d. Model specifcation in (b) and additionally control for 21 temporally prior and intervening mental disorders (PTSD inclusive).
* P<0.05, 2–sided test.
When we adjusted for PTSD (model 5), the pattern of findings (effect size, direction, and significance) remained remarkably similar. When we adjusted for all mental disorders assessed in the surveys (model 6, including PTSD), 11 of the 29 traumatic events were significantly associated with psychotic experiences. The patterns were generally consistent although for a handful of traumatic events, the odds ratios were slightly attenuated. Overall, these results indicate that the significant associations of specific traumatic events with onset of psychotic experiences were not explained by prior (to the psychotic experiences) mental disorders.
Discussion
Main findings
Based on a large data-set from 16 countries, we confirmed that traumatic events are associated with a threefold increased odds of subsequent first onset of psychotic experiences. There was a dose-response relationship between higher numbers of traumatic event types and odds of psychotic experiences. The findings are consistent with recent literature that traumatic events are associated with psychotic experiences in a dose-dependent fashion. Reference Beards, Gayer-Anderson, Borges, Dewey, Fisher and Morgan3–Reference Saha, varghese, Slade, Degenhardt, Mills and McGrath6,Reference Scott, Chant, Andrews, Martin and McGrath8 In addition, the study contributed two important findings: first, traumatic events were not equipotent with respect to the subsequent first onset of psychotic experiences. Second, comorbid mental disorders (including PTSD) did not account for the associations of traumatic events with psychotic experiences.
Variation in the strength of association
With respect to the variation in the strength of association across traumatic event types, prior research has often foiled to use statistical models that adequately address the intercorrelated nature of traumatic events. We constructed multivariable models that included a comprehensive list of 29 traumatic event types, and incorporated number of traumatic events per person, as well as interactive models. Similar to our earlier analysis of childhood adversities and psychotic experience onsets, Reference McGrath, McLaughlin, Saha, Aguilar-Gaxiola, Al-Hamzawi and Alonso2 we found that not all traumatic events had equivalent associations with subsequent first onset of psychotic experiences. For example, in the marginal effect model (model 4), we found that only 12 of the 29 traumatic event types were associated with an increased risk of subsequent psychotic experiences. Six of the ten traumatic events related to interpersonal violence, intimate partner, and sexual violence were associated with psychotic experiences (effect sizes ranged from 1.8 to 4.9 for ‘witnessed physical fight at home’ and ‘raped’, respectively). Those who endorsed ‘raped’ had fivefold increased odds of subsequent onset of psychotic experiences (OR = 4.9, 95% CI 2.5–9.5). The general pattern of findings indicates a complex interactive association between traumatic event types and number of traumatic events. In the complex interactive model (model 4), we also found that those who were exposed to more traumatic events were more likely to develop a first-onset psychotic experience regardless of type of traumatic events. This is consistent with the hypothesis that traumatic event exposure is a risk factor for psychosis, Reference Freedman20 and also lends additional support for the important role of stress in aetiological pathways underpinning risk of psychotic experiences. Interestingly, in some models, ‘civilian or relief worker in war zone’ showed protective effects with respect to subsequent psychotic experiences onset. This is consistent with previous WMH survey studies with traumatic events, which suggest that respondents who had war experience may have a reduced risk of mental or physical disorders compared with the general population. Reference Liu, Petukhova, Sampson, Aguilar-Gaxiola, Alonso and Andrade21 This may partly be because of a selection effect and/or to prior exposure promoting resilience. Reference Liu, Petukhova, Sampson, Aguilar-Gaxiola, Alonso and Andrade21 In summary, the nature of the relationship between exposure to traumatic events and subsequent psychotic experiences is more nuanced than previously thought.
Role of comorbid disorders
With respect to the explanatory effects of comorbid disorders, we found that the associations of traumatic events with psychotic experiences were mostly unchanged after adjustment for mental disorders that began prior to the onset of psychotic experiences. This adjustment included both confounding effects (i.e. mental disorders that both predicted subsequent occurrence of traumatic events and later onset of psychotic experiences) and mediating effects (i.e. traumatic events predicting subsequent onset of mental disorders that, in turn, are predictors of later psychotic experiences). No attempt was made to distinguish between the two types of effects. The finding that comorbid mental disorders do not account for the associations of traumatic events with subsequent psychotic experiences is consistent with our earlier findings that there was little or no influence of mental disorders on the associations of childhood adversities with psychotic experiences. Reference McGrath, McLaughlin, Saha, Aguilar-Gaxiola, Al-Hamzawi and Alonso2 In particular, we found that PTSD did not appear to play a substantial role in accounting for the associations of traumatic events with psychotic experiences. This was in contrast to an earlier finding, where those with both exposure to traumatic events and associated PTSD were at greater risk of lifetime psychotic experiences. Reference Scott, Chant, Andrews, Martin and McGrath8 However, our finding is consistent with the hypothesis that some (but not all) traumatic events may be ‘sufficient’ causes of subsequent psychotic experience onset (i.e. an intervening mental disorder is not required to trigger psychotic experiences). Of course, genetic factors and other unmeasured confounders could influence this association.
Even though the exact mechanisms linking traumatic events to psychotic experiences remain poorly understood, there is considerable recent interest in how socially mediated factors and traumatic events may influence the aetiology of psychotic experiences. Traumatic events may create a constitutional disposition for psychotic experiences that may include heightened vulnerability to stress, Reference McLaughlin, Kubzansky, Dunn, Waldinger, Vaillant and Koenen22 elevated emotional reactivity and dysregulation Reference Liu, Petukhova, Sampson, Aguilar-Gaxiola, Alonso and Andrade21,Reference McCrory, De Brito, Sebastian, Mechelli, Bird and Kelly23 and deficits in cognitive control. Reference DePrince, Weinzierl and Combs24 For example, it is feasible that psychopathology emerges as the end product of distress and anxiety because of maladaptive stress and emotional reactions of traumatic events, which in turn may lead to dopamine sensitisation. These pathways may influence psychosis vulnerability. Reference Kapur25 Stress-related changes in the hypopituitary axis could also have an impact on brain circuitry via epigenetic mechanisms, leading to vulnerability to subsequent psychotic experiences. Reference Barker, Gumley, Schwannauer and Lawrie26
Limitations
Although the current study has many strengths (for example range of traumatic event types, large sample size, range of countries, uniform methodology for data collection), it also has several limitations that deserve comment. We excluded those who screened positive for possible psychotic disorders based on self-reporting having received a psychosis diagnosis or having used antipsychotic medications to treat the reported psychotic experiences. However, it is possible that some respondents who reported psychotic experiences had an untreated psychotic disorder. We also relied on retrospective reports about age at onset, which might have led to a recall bias. However, we note that several prospective studies have confirmed the association between traumatic events and subsequent psychotic experiences. Reference Kelleher, Harley, Lynch, Arseneault, Fitzpatrick and Cannon4,Reference Spauwen, Krabbendam, Lieb, Wittchen and van Os5 Although we had age at exposure for each type of traumatic event, we could not define the pattern of exposure across the life course (for example we could not identify those who only had childhood exposure v. those that had both childhood and adult exposure). We failed to control for all plausible correlates of both traumatic event exposure and psychotic experiences, as we wanted to focus on comorbid mental disorders and we were concerned that other plausible correlates (such as socioeconomic status and education) could be either causes or consequences of both traumatic event exposure and psychotic experiences. Finally, while our findings are consistent with the hypothesis that particular types of traumatic event exposure may contribute to the development of subsequent psychotic experiences, the surveys are cross-sectional and thus unable to determine causal pathways.
Implications
Despite these limitations, our study found that many of the traumatic events (11 out of 29) were independently associated with subsequent psychotic experiences in a large, community-based transnational study that were not mediated by mental disorders. The robust literature now linking traumatic events and subsequent psychotic experiences may enrich the epidemiological landscape of psychotic experiences, and can provide important clues to the aetiology and pathogenesis of psychotic experiences.
Funding
The World Health Organization World Mental Health (WMH) Survey Initiative is supported by the National Institute of Mental Health (NIMH; ), the John D. and Catherine T. MacArthur Foundation, the Pfizer Foundation, the US Public Health Service (, , and ), the Fogarty International Center (), the Pan American Health Organization, Eli Lilly and Company, Ortho-McNeil Pharmaceutical, GlaxoSmithKline, and Bristol-Myers Squibb. None of the funders had any role in the design, analysis, interpretation of results, or preparation of this paper. The views and opinions expressed in this report are those of the authors and should not be construed to represent the views of the World Health Organization, other sponsoring organisations, agencies, or governments.
Acknowledgements
A complete list of all within-country and cross-national WMH publications can be found at http://www.hcp.med.harvard.edu/wmh/. We thank the staff of the WMH Data Collection and Data Analysis Coordination Centres for assistance with instrumentation, feldwork, and consultation on data analysis.
Appendix
The WHO World Mental Health Survey collaborators are: Sergio Aguilar-Gaxiola, MD, PhD, Ali Al-Hamzawi, MD, Mohammed Salih Al-Kaisy, MD, Jordi Alonso, MD, PhD, Laura Helena Andrade, MD, PhD, Corina Benjet, PhD, Guilherme Borges, ScD, Evelyn J. Bromet, PhD, Ronny Bruffaerts, PhD, Brendan Bunting, PhD, Jose Miguel Caldas de Almeida, MD, PhD, Graca Cardoso, MD, PhD, Somnath Chatterji, MD, Alfredo H. Cia, MD, Louisa Degenhardt, PhD, Koen Demyttenaere, MD, PhD, John Fayyad, MD, Silvia Florescu, MD, PhD, Giovanni de Girolamo, MD, Oye Gureje, MD, DSc, FRCPsych, Josep Maria Haro, MD, PhD, Yanling He, MD, Hristo Hinkov, MD, PhD, Chi-yi Hu, MD, PhD, Yueqin Huang, MD, MPH, PhD, Peter de Jonge, PhD, Aimee Nasser Karam, PhD, Elie G. Karam, MD, Norito Kawakami, MD, DMSc, Ronald C. Kessler, PhD, Andrzej Kiejna, MD, PhD, Viviane Kovess-Masfety, MD, PhD, Sing Lee, MB, BS, Jean-Pierre Lepine, MD, Daphna Levinson, PhD, John McGrath, MD, PhD, Maria Elena Medina-Mora, PhD, Jacek Moskalewicz, PhD, Fernando Navarro-Mateu, MD, PhD, Beth-Ellen Pennell, MA, Marina Piazza, MPH, ScD, Jose Posada-Villa, MD, Kate M. Scott, PhD, Tim Slade, PhD, Juan Carlos Stagnaro, MD, PhD, Dan J. stein, FRCPC, PhD, Margreet ten Have, PhD, Yolanda Torres, MPH, Dra.HC, Maria Carmen viana, MD, PhD, Harvey Whiteford, MBBS, PhD, David R. Williams, MPH, PhD, Bogdan Wojtyniak, ScD.






eLetters
No eLetters have been published for this article.