Antipsychotic medication is fundamental to the effective management of schizophrenia, in terms of both acute treatment and relapse prevention. Long-acting depot antipsychotics, given every 1-6 weeks by intramuscular injection, were developed in the 1960s as an additional method of drug delivery aimed specifically to counter problems with treatment adherence in chronic sufferers (Reference SimpsonSimpson, 1984) and to simplify the medication process (Reference JohnsonJohnson, 1984; Reference Barnes and CursonBarnes & Curson, 1994; Reference Davis, Metalon and WatanabeDavis et al, 1994). A series of systematic reviews on the efficacy, effectiveness and safety of depot neuroleptic drugs in the treatment of schizophrenia has been published recently (Reference Adams and EisenbruchAdams & Eisenbruch, 2000; Reference Coutinho, Fenton and QuraishiCoutinho et al, 2000; Quraishi & David, Reference Quraishi and David2000a , Reference Quraishi and David b , Reference Quraishi and David c , Reference Quraishi and David d , Reference Quraishi and David e ; Reference Quraishi, David and AdamsQuraishi et al, 2000), summarised in the accompanying article (see Adams et al, this issue). Here we review the published evidence on patient and staff satisfaction with depots. It is ironic that the very reasons why clinicians favour depot medication in certain circumstances are those that make this method of administration unpopular with some users. For example, Anderson et al (Reference Anderson, Leadbetter and Williams1989) reported that the depot clinic is perceived as being “out of date, not geared to the needs of the patient, inaccessible and unable to provide personalised care”. Pereira & Pinto (Reference Pereira and Pinto1997) stated that “ Consumer advocates concentrate on the undeniable adverse effects of antipsychotic drugs and upon the accusation that depot treatments involve an element of coercion”. It is against this backdrop that the review was carried out.
Objective
The objective of the review was to explore patient and nurse satisfaction with depot antipsychotic medication. None of the studies included in the effectiveness reviews reported data that directly assessed patient satisfaction with the medication. Consequently, a wider review incorporating studies of mixed design and not restricted to randomised controlled trials (RCTs) was instituted. The specific aims were to investigate: patient satisfaction with depot antipsychotic medication; the patient preferred setting for the administration of depot antipsychotic medication; patient preference for depot antipsychotic medication or oral antipsychotic medication; and nurse satisfaction with depot antipsychotic medication.
METHOD
A systematic search strategy was implemented. This involved searching the following electronic databases: Medline, Embase, PsycINFO, CINAHL and The Cochrane Library from 1966 up to the end of May 1999. The review used a subject and textword search strategy with DEPOT, DELAYED-ACTION PREPARATIONS, (INTRAMUSCULAR) INJECTIONS and ANTIPSYCHOTIC (AGENTS) and/or NEUROLEPTIC (DRUGS) as the main search terms. The databases were also searched using specific depot drug names in order to be as comprehensive as possible. These were combined with ‘satisfaction’, ‘attitude’ and related terms. Reference and library source searching plus hand-searches also were carried out (see Appendix).
Inclusion/exclusion criteria
Studies were included if they contained original data describing nurse or patient satisfaction (i.e. any opinion or attitude) towards depot antipsychotic medication according to the title or abstract. A second independent reviewer selected studies from a random 10% of the references to ensure that selection of studies was reliable. Where differences of opinion occurred, these were resolved by discussion.
Analysis
The quality of the articles was assessed in two stages. The first stage used a ‘hierarchy of evidence’. This is a method of categorising studies via the attributes of their design. It is a hierarchy of bias, which increases progressively downwards. We used an amalgamation of two hierarchies (University of York NHS Centre for Reviews and Dissemination, 1996; Reference GreenhalghGreenhalgh, 1997) — essentially from RCTs, through non-randomised controlled trials, to cohort studies, to case-control studies, to case series, etc. The categorisation for each study was carried out by two of us (J. W., R. G.) independently and any disagreements were resolved by discussion.
The second stage comprised the assessment of the studies using a 13-item checklist constructed specifically for the review. The items for this checklist were derived from a number of sources (University of York NHS Centre for Reviews and Dissemination, 1996; Reference GreenhalghGreenhalgh, 1997) and finalised by discussion between us. The checklist focused upon those variables most often highlighted in critical appraisal, namely, justification of sample size, sampling, response/drop-out rates, validity of measures and the generalisability of the results (see Tables 1 and 2).
Table 1 Characteristics of included studies (study denoted by first author and year of publication)

| Study | Design | Participants | n | Satisfaction outcome measures |
|---|---|---|---|---|
| Anderson 1989 | Cross-sectional survey | Diagnosis: not specified; patients attending 2 depot clinics over a 1-month period. | 168 | 16-item questionnaire investigating general attitudes towards the depot clinic |
| Setting: hospital-based depot clinics | ||||
| Bennett 1995 | Cross-sectional survey | Diagnosis: not specified | 55 | 20-item questionnaire investigating CPNs' practice in administration of depot medication and their attitudes towards it |
| Profession: CPN | ||||
| Setting: CPNs in 3 health districts | ||||
| Brooker 1996 | Cross-sectional survey | Diagnosis: not specified; attendees of depot clinics in north-west catchment area | 270 | 34-item questionnaire investigating clients' views about their depot medication and the arrangements of their depot clinic |
| Setting: depot clinics | ||||
| Reference BuisBuis 1992 | Cross-sectional survey | Diagnosis: not specified; “most had a diagnosis of schizophrenia” | 44 | Adapted UKU side-effect scale. Objective criteria replaced with subjective |
| Setting: out-patient clinic | ||||
| Burns 1998 | RCT | Diagnosis: schizophrenia | 149 | Exit interviews describing nurses' attitudes towards their ability to perform the structured assessments |
| Profession: practice nurses | ||||
| Setting: 140 general practices, south London | ||||
| Reference CantleCantle 1997 | Cross-sectional survey | Diagnosis: not applicable | 26 | 10-item questionnaire regarding management of schizophrenia in general practice |
| Profession: GPs and practice nurses | ||||
| Setting: study day | ||||
| Reference DesaiDesai 1999 | Quaisi-case—control | Diagnosis: DSM—IV schizophrenia | 143 | Patient acceptance of medication on 7-point scale |
| Setting: out-patients referred to the study | Comparison of depot/oral on 7-point scale | |||
| Eastwood 1997 | Cross-sectional survey | Diagnosis: not specified; patients receiving depot medication in a number of settings | 100 | Semi-structured depot neuroleptic interview investigating patients' knowledge about their medication and their attitudes towards it |
| Garavan 1998 | Cross-sectional survey | Diagnosis: DSM—III—R schizophrenia | 70 | Drug attitude inventory |
| Setting: out-patient clinic | ||||
| Goldbeck 1999 | Cross-sectional survey | Diagnosis: not specified; patients receiving depot medication at a community health centre in Clydebank | 59 | Semi-structured interview looking at depot medication issues |
| Setting: community health centre | ||||
| Hoencamp 1995 | Cross-sectional survey | Diagnosis: DSM—III schizophrenia | 174 | 17-item Modified Patient Request Scale (Dutch Version); 8-item Neuroleptic Evaluation and Attitude List (interview) |
| Setting: out-patient clinic, depot=81, oral=93 | ||||
| Jacobsson 1980 | Cross-sectional survey | Diagnosis: schizophrenia | 43 | Interview |
| Setting: hospital depot clinic | Questionnaire | |||
| Kendrick 1998 | Cross-sectional survey | Diagnosis: not applicable | 192 | Postal survey |
| Profession: practice nurse | Focus group | |||
| Setting: GP surgery | ||||
| Larsen 1996 | Cross-sectional survey | Diagnosis: ICD-10 schizophrenia | 53 | 14-item questionnaire specially designed to evaluate the patients' attitude to treatment; Psychological General Well-being Schedule |
| Setting: out-patient clinic | ||||
| Pan 1989 | Quasi-case—control | Diagnosis: schizophrenia; attenders and irregular attenders at depot clinic | 80 | 4-part Health Belief Questionnaire specifically designed for the study |
| Setting: hospital depot clinic | ||||
| Pereira 1997 | Cross-sectional survey | Diagnosis: chronic schizophrenia/paranoid psychosis | 173 | Semi-structured interview/questionnaire investigating patients' attitudes towards their medication |
| Setting: out-patient clinic | ||||
| Poole 1998 | Cross-sectional survey | Diagnosis: not specified; patients receiving depots in a number of settings within the locality | 47 | Questionnaire asking patients to choose where they would prefer to received their medication |
| Reference Sandford, Sandford and GournaySandford 1996 | Cross-sectional survey | Diagnosis: not specified; patients receiving depots in 5 clinics | 58 | Structured interview investigating patients' views of the care and service they received at the clinic |
| Setting: 5 depot clinics | ||||
| Singh 1995 | Cross-sectional survey | Diagnosis: schizophrenia (188), manic—depressive psychosis (15) and schizoaffective disorder (15) | 218 | 17-item interview questionnaire investigating |
| Setting: hospital-based depot clinic | patients' views of the care and service they received at the clinic | |||
| Smith 1999 | Quasi-case—control | Diagnosis: schizophrenia DSM—III—R | 40 | 4-item interview schedule derived from motivational interviewing, investigating attitudes towards medication and compliance |
| Setting: depot clinic and day hospital | ||||
| Reference WarrenWarren 1998 | Cross-sectional survey | Diagnosis: not specified; patients receiving depot antipsychotics | 76 | Structured interview schedules investigating the quality of care during the administration of depot medication |
| Profession: 68 nurses | ||||
| Setting: various | ||||
| Reference WistedtWistedt 1995 | Cross-sectional survey | Diagnosis: schizophrenia (68); other diagnoses (5) | 73 | Six questions investigating patient attitudes towards their depot medication, asked by mental health nurse |
| Setting: depot clinic |
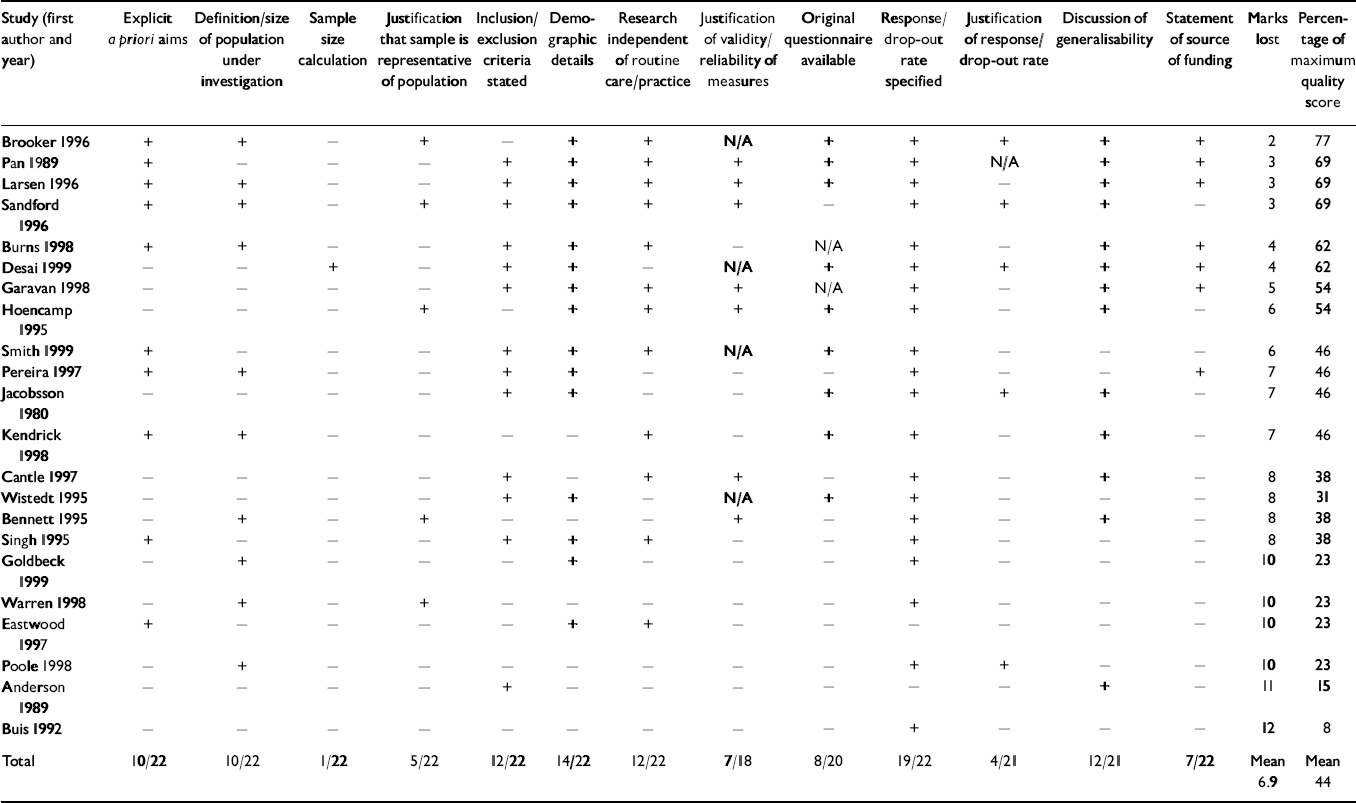
Table 2 Checklist results: quality of studies
| Study (first author and year) | Explicit a priori aims | Definition/size of population under investigation | Sample size calculation | Justification that sample is representative of population | Inclusion/exclusion criteria stated | Demographic details | Research independent of routine care/practice | Justification of validity/reliability of measures | Original questionnaire available | Response/drop-out rate specified | Justification of response/drop-out rate | Discussion of generalisability | Statement of source of funding | Marks lost | Percentage of maximum quality score |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Brooker 1996 | + | + | - | + | - | + | + | N/A | + | + | + | + | + | 2 | 77 |
| Pan 1989 | + | - | - | - | + | + | + | + | + | + | N/A | + | + | 3 | 69 |
| Larsen 1996 | + | + | - | - | + | + | + | + | + | + | - | + | + | 3 | 69 |
| Reference Sandford, Sandford and GournaySandford 1996 | + | + | - | + | + | + | + | + | - | + | + | + | - | 3 | 69 |
| Burns 1998 | + | + | - | - | + | + | + | - | N/A | + | - | + | + | 4 | 62 |
| Reference DesaiDesai 1999 | - | - | + | - | + | + | - | N/A | + | + | + | + | + | 4 | 62 |
| Garavan 1998 | - | - | - | - | + | + | + | + | N/A | + | - | + | + | 5 | 54 |
| Hoencamp 1995 | - | - | - | + | - | + | + | + | + | + | - | + | - | 6 | 54 |
| Smith 1999 | + | - | - | - | + | + | + | N/A | + | + | - | - | - | 6 | 46 |
| Pereira 1997 | + | + | - | - | + | + | - | - | - | + | - | - | + | 7 | 46 |
| Jacobsson 1980 | - | - | - | - | + | + | - | - | + | + | + | + | - | 7 | 46 |
| Kendrick 1998 | + | + | - | - | - | - | + | - | + | + | - | + | - | 7 | 46 |
| Reference CantleCantle 1997 | - | - | - | - | + | - | + | + | - | + | - | + | - | 8 | 38 |
| Reference WistedtWistedt 1995 | - | - | - | - | + | + | - | N/A | + | + | - | - | - | 8 | 31 |
| Bennett 1995 | - | + | - | + | - | - | - | + | - | + | - | + | - | 8 | 38 |
| Singh 1995 | + | - | - | - | + | + | + | - | - | + | - | - | - | 8 | 38 |
| Goldbeck 1999 | - | + | - | - | - | + | - | - | - | + | - | - | - | 10 | 23 |
| Reference WarrenWarren 1998 | - | + | - | + | - | - | - | - | - | + | - | - | - | 10 | 23 |
| Eastwood 1997 | + | - | - | - | - | + | + | - | - | - | - | - | - | 10 | 23 |
| Poole 1998 | - | + | - | - | - | - | - | - | - | + | + | - | - | 10 | 23 |
| Anderson 1989 | - | - | - | - | + | - | - | - | - | - | - | + | - | 11 | 15 |
| Reference BuisBuis 1992 | - | - | - | - | - | - | - | - | - | + | - | - | - | 12 | 8 |
| Total | 10/22 | 10/22 | 1/22 | 5/22 | 12/22 | 14/22 | 12/22 | 7/18 | 8/20 | 19/22 | 4/21 | 12/21 | 7/22 | Mean | Mean |
| 6.9 | 44 |
RESULTS
The search strategy produced 1374 articles. Of these, 22 met the inclusion criteria for containing satisfaction data. Sixteen studies explored patient attitudes towards depot antipsychotic medication, four looked at the opinions of nurses and two investigated both. Eighteen studies were cross-sectional surveys, three were quasi-case-control studies and there was one RCT. The sample size of the studies ranged from 26 to 270 participants (median=73). The total number of patient participants was 2311. Various settings were used for the studies, including hospital-based depot clinics, outpatient clinics and general practitioner (GP) surgeries. Twenty studies used questionnaires or interviews specifically designed for the study, one adapted an existing measure and one applied an existing measure. The characteristics of the included studies and scales used are described in Table 1.
The quality of the studies was mixed. Their performance on the checklist (Table 2) and marks scored was in the range 1-10 out of a maximum of 13 (mean score=44%). Ten (48%) studies failed to score on eight of the items. The studies performed best for: ‘response rate specified’ (included by 90% of the studies) and ‘demographic details’ (67%). However, only one study included a sample size calculation, and, although 19 studies stated their response or drop-out rate, only four of these justified or explained these rates. Similarly, 16 studies did not attempt to show that their sample was in any way representative of the population they were aiming to investigate.
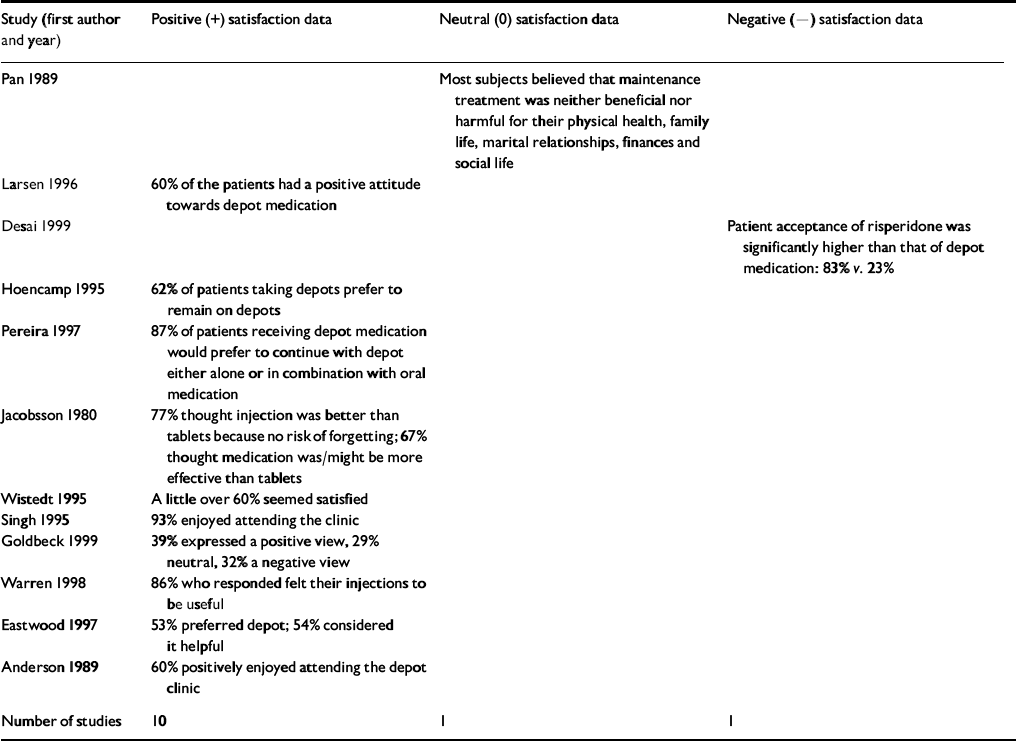
Ten of the twelve studies that included specific attitudinal or preferential data found that their patients held some positive views towards depot antipsychotic medication. One reported a neutral view and one a negative attitude (Table 3).
Table 3 Patient satisfaction with depot antipsychotics
| Study (first author and year) | Positive (+) satisfaction data | Neutral (0) satisfaction data | Negative (-) satisfaction data |
|---|---|---|---|
| Pan 1989 | Most subjects believed that maintenance treatment was neither beneficial nor harmful for their physical health, family life, marital relationships, finances and social life | ||
| Larsen 1996 | 60% of the patients had a positive attitude towards depot medication | ||
| Reference DesaiDesai 1999 | Patient acceptance of risperidone was significantly higher than that of depot medication: 83% v. 23% | ||
| Hoencamp 1995 | 62% of patients taking depots prefer to remain on depots | ||
| Pereira 1997 | 87% of patients receiving depot medication would prefer to continue with depot either alone or in combination with oral medication | ||
| Jacobsson 1980 | 77% thought injection was better than tablets because no risk of forgetting; 67% thought medication was/might be more effective than tablets | ||
| Reference WistedtWistedt 1995 | A little over 60% seemed satisfied | ||
| Singh 1995 | 93% enjoyed attending the clinic | ||
| Goldbeck 1999 | 39% expressed a positive view, 29% neutral, 32% a negative view | ||
| Reference WarrenWarren 1998 | 86% who responded felt their injections to be useful | ||
| Eastwood 1997 | 53% preferred depot; 54% considered it helpful | ||
| Anderson 1989 | 60% positively enjoyed attending the depot clinic | ||
| Number of studies | 10 | 1 | 1 |
Four of the five studies investigating patient preference regarding treatment setting reported that the majority preferred to receive their medication at the depot clinic (a regular forum attached to a hospital or community centre where depots are administered), whereas Poole & Grimes (Reference Poole and Grimes1998) found the preferred setting to be at home (Table 4). None of the studies found a majority of patients in favour of GP-based treatment. Indeed, this was the third least preferable option for all of the studies.
Table 4 Patient preference for treatment setting

| Study1 | n | Depot clinic (%) | Home (%) | GP (%) |
|---|---|---|---|---|
| Brooker 1996 | 270 | 742 | - | |
| Reference Sandford, Sandford and GournaySandford 1996 | 58 | 52 | 29 | 19 |
| Singh 1995 | 218 | 63/883 | 37 | 14 |
| Poole 1998 | 47 | 212 | 64 | 9 |
| Anderson 1989 | 168 | 562 | 39 | 17 |
| Number of studies | 4 | 1 | 0 |
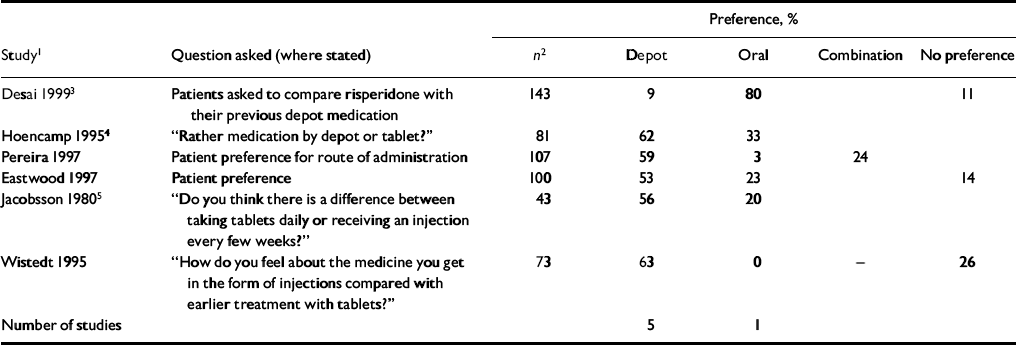
There were six studies that reported on a direct comparison of oral v. depot from the point of view of patient preference (Table 5). Five studies found that the majority of participants preferred to receive their medication via depot administration rather than in tablet form. Desai (Reference Desai1999), in an open non-randomised study comparing patients switched from depot to risperidone, found that 80% of their sample preferred oral medication.
Table 5 Patient preference for depot v. oral antipsychotic (unless otherwise stated, patients are on depot antipsychotics)
| Preference, % | ||||||
|---|---|---|---|---|---|---|
| Study1 | Question asked (where stated) | n 2 | Depot | Oral | Combination | No preference |
| Reference DesaiDesai 19993 | Patients asked to compare risperidone with their previous depot medication | 143 | 9 | 80 | 11 | |
| Hoencamp 19954 | “ Rather medication by depot or tablet?” | 81 | 62 | 33 | ||
| Pareira 1997 | Patient preference for route of administration | 107 | 59 | 3 | 24 | |
| Eastwood 1997 | Patient preference | 100 | 53 | 23 | 14 | |
| Jacobsson 19805 | “ Do you think there is a difference between taking tablets daily or receiving an injection every few weeks?” | 43 | 56 | 20 | ||
| Reference WistedtWistedt 1995 | “ How do you feel about the medicine you get in the form of injections compared with earlier treatment with tablets?” | 73 | 63 | 0 | - | 26 |
| Number of studies | 5 | 1 | ||||
Two studies investigated the importance given to particular side-effects. Buis (Reference Buis1992) asked patients to complete an amended version of the UKU side-effect rating scale (Reference Lingjaerde, Ahlfors and BechLingjaerde et al, 1987), where objective criteria had been replaced by subjective criteria. They then formed a hierarchy of the side-effects that were most important or troublesome. The top five were: sleepiness, increased fatigability, weight gain, tension or inner unrest and concentration difficulties. Side-effects associated with movement were among the least important. Larsen & Gerlach (Reference Larsen and Gerlach1996) reported that extrapyramidal symptoms (EPS) (apart from akathisia) were least reported by patients. However, 88% of patients who reported no side-effects had at least one EPS. Larsen & Gerlach (Reference Larsen and Gerlach1996) also found that non-physical or ‘psychic’ side-effects (dullness/tiredness) were the most frequently reported. This is in contrast to the perception of the patients' physician, who focused mainly on EPS.
Nurse satisfaction
There were minimal data for nurse satisfaction with depot antipsychotics. No one paper focused specifically on the issue of nurse satisfaction with depot antipsychotics and all data included were embedded within articles looking at other topics. There were differences between the attitude of community psychiatric nurses (CPNs) and practice nurses. Bennett et al (Reference Bennett, Done and Hunt1995) reported that, overall, the CPNs' attitude was favourable towards administering and monitoring medication, although 29% felt that it did not utilise their skills. However, Burns et al (Reference Burns, Millar and Garland1998) reported that two-thirds of practice nurses administered depots but most lacked confidence and training. Kendrick et al (Reference Kendrick, Millar and Burns1998) surveyed practice nurses by post and held a focus group to find that they felt unsupervised and that CPNs should be administering depots. Cantle (Reference Cantle1997) surveyed 26 delegates (GPs and primary care nurses) at a training day for depot neuroleptics: 88% of the group stated that they would like more training. Warren (Reference Warren1998) carried out an audit of depot administration and reported that nurses wanted more training in medication and treating psychoses in general. Finally, only one of the five studies looking at patient preference for treatment setting investigated nurse opinion. Brooker et al (Reference Brooker, Faugier and Gray1996) asked clinic nurse managers of 135 depot clinics to rate their overall satisfaction (0=totally unsatisfactory, 8=excellent) with their clinic arrangements. The mean rating was 4.8, with 40% scoring below this figure.
DISCUSSION
There were few data in the literature concerned with patient satisfaction with depot antipsychotic medication, and even fewer investigating the attitudes of nurses. All were from the lower levels of the hierarchy of evidence. Although the cross-sectional survey is appropriate for investigating satisfaction, more complex longitudinal designs could be used to assess, for example, how attitudes may change over time.
Data quality
The favourable findings regarding depots in the majority of studies are in contrast to the negative popular perception of depot antipsychotic medication and the view put forward in the introduction (Reference Anderson, Leadbetter and WilliamsAnderson et al, 1989; Reference Pereira and PintoPereira & Pinto, 1997). However, the scarcity and mixed quality of the studies make generalisations problematic. First, no studies asked the same question to guage overall satisfaction, so amalgamating the responses may be inappropriate. Similarly, comparison between studies was difficult. Second, the higher quality studies tended to show less positive results, indicating a possible relationship between study quality and outcome, but because there are only two dissenters this cannot be concluded with confidence. Another more persuasive explanation for the findings is sample selection bias. The patients involved in the studies were, by definition, ‘attenders’ and ‘compliers’. People who attend depot clinics would be expected to be reasonably positive about depots, otherwise they would not attend. Data on non-attenders and non-compliance are, ipso facto, hard to obtain. The key factor is that the studies did not formally seek a sample that was representative of all those who were prescribed depot antipsychotic medication but took a convenience sample with all its associated pitfalls. Similarly, a non-selected group of patients on maintenance oral medication would include many who had been either on depots in the past or at least offered them and declined. The views of such patients on depots (presumably rather negative) would complete the picture, as well as perhaps offering insights into why such patients dislike depots (see Reference Hoencamp, Knegtering and KooyHoencamp et al, 1995). The most informative study would compare a population-based survey of all patients on maintenance treatment — depot and oral. Depot recipients are bound to have been given oral medication previously and many patients on oral medication also will have experience of depots. Hence, each could express a preference. Reasons for accepting/declining depots could be gathered systematically.
Preference for depots
Hoencamp et al (Reference Hoencamp, Knegtering and Kooy1995) did compare patients on oral and depot medication but could not obtain data regarding preference from those currently on oral medication. It was reported that 26 of the 93 patients on oral medication had been on depot medication previously but only two preferred depot medication. Nevertheless, the conclusion that can be drawn from this and similar studies is that the majority of patients on depot antipsychotic medication accept their medication, with approximately a quarter of patients in three of the studies not satisfied. Desai (Reference Desai1999) was the only study reporting that patients preferred oral medication to their current depot medication. However, this can be attributed to bias because the sample was composed of patients whose psychiatrists had considered that they would benefit from a switch from depot antipsychotic medication to risperidone, an oral atypical antipsychotic drug.
The results show that the majority of patients prefer to have their medication administered at a clinic organised for this purpose. This may be because of the social contact afforded by attending the clinic and ready access to health care professionals. These benefits would not follow from attendance at the GP surgery, where there would be few other relevant facilities on site. However, the bias described previously may also explain the preference for treatment setting. All five studies took their sample from patients receiving their medication at a depot clinic. None of the studies took a representative sample from patients of clinics, at home and at their GP surgery.
Reasons for preference
The evidence reviewed showed clear patient preference for depot antipsychotic medication over oral antipsychotic medication. Therefore, although evidence of clinical superiority may be elusive, we have found support for a ‘subjective superiority’ for depots. One possible explanation is convenience. Wistedt (Reference Wistedt1995) found that 67% of their sample thought it easier to have an injection than taking tablets once or twice daily. Hoencamp et al (Reference Hoencamp, Knegtering and Kooy1995) also found convenience to be an important factor, because 42% of those who preferred depots cited this as a reason why. In contradiction to the concerns regarding the loss of personal freedom, Jacobsson & Odling (Reference Jacobsson and Odling1980) reported that 67% of their sample receiving antipsychotics via a depot did so because of the control they had over the timing and dosage of treatment.
The emphasis of patients on the ‘psychological’ side-effects described by Buis (Reference Buis1992) and Larsen & Gerlach (Reference Larsen and Gerlach1996) and its discordance with the emphasis of health professionals (Reference Larsen and GerlachLarsen & Gerlach, 1996) highlights the need for a patient focus. Although the physical side-effects must be addressed for the patient's safety and satisfaction, the psychological aspects also need to be addressed to improve quality of life. The neglect of this dimension may lead to non-compliance.
Nurse satisfaction
There are few studies looking at the perception of nurses administering depot antipsychotic medication. We may conclude, nevertheless, that there is ambiguity as to the type of nurse who should administer depot antipsychotic medication and that more and better training should be given (see Reference Burns, Millar and GarlandBurns et al, 1998; Reference Kendrick, Millar and BurnsKendrick et al, 1998).
APPENDIX: SEARCH STRATEGY
Database searching
-
(a) Medline, 1966—May 1999 (updated weekly): [(DEPOT$.mp/or exp Delayed-action preparations)/and (ANTIPSYCHOTIC$.mp/or exp antipsychotic agents or “NEUROLEPTIc$. MP)]
-
(b) PsycINFO, 1887—May 1999 (updated monthly): [(DEPOT$.mp/and (ANTIPSYCHOTIC$.mp/or “NEUROLEPTIC$.mp/or exp neuroleptic drugs)]
-
(c) CINAHL, 1993—April 1999 (updated monthly): [DEPOT$.mp/or exp injections, intramuscular)/and (ANTIPSYCHOTIC$.mp/or exp antipsychotic agents or “NEUROLEPTIC$.mp)]
-
(d) Embase, 1980—May 1999 (updated weekly): [DEPOT$.mp/and (ANTIPSYCHOTIC$.mp/or exp atypical antipsychotic agent/or NEUROLEPTIC$.mp/or exp neuroleptic agent)]
-
(e) The Cochrane Library (issue 4, 1999)
The above databases were also searched using specific depot drug names in order to make the search as comprehensive as possible (see text). These were combined with ‘satisfaction’ and related terms, as follows:
-
(a) Medline [(exp consumer satisfaction/or exp job satisfaction/or exp patient satisfaction/or exp personal satisfaction/or satisfaction.mp) or (exp attitude/or exp attitude of health personnel/or exp attitude to health/or attitude.mp)]
-
(b) PsycINFO [(exp satisfaction/or satisfaction.tw) or (exp adult attitudes/or exp attitudes/or exp drug use attitudes/or exp attitudes towards mental illness/or attitude$.tw)]
-
(c) CINAHL [(exp consumer satisfaction/or exp job satisfaction/or exp patient satisfaction/or exp personal satisfaction/or satisfaction.mp) or (exp attitude/or exp attitude of health personnel/or attitude to mental illness/or attitude$.mp)]
-
(d) Embase [(exp job satisfaction/or exp life satisfaction/or exp patient satisfaction/or exp satisfaction/or satisfaction.mp) or (exp patient attitude/exp nurse attitude/exp physician attitude/or attitude$.mp)]
Reference searching
The references of the included studies were inspected for further studies. Each of the included studies was sought as a citation on the SCISEARCH database. Reports of articles that had cited these studies were inspected in order to identify further trials.
Library source searching
The catalogues at the Institute of Psychiatry and the Royal College of Nursing were searched to obtain secondary sources:
-
(a) Depot and [antipsychotic or neuroleptic]
-
(b) Psychiatric Nursing and Depot
Hand-searching
The following journals were hand-searched for June, July and August 1999 to identify publications that may not have been entered on the databases yet:
-
(a) Acta Psychiatrica Scandinavica
-
(b) Journal of Mental Health
-
(c) British Journal of Psychiatry
-
(d) Schizophrenia Bulletin
-
(e) Psychiatric Bulletin
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
• Patients currently on depot medication are generally happy with that mode of delivery.
-
• Most patients on depots prefer them to oral drugs.
-
• Convenience seems to be the main reason for patient preference of depot.
LIMITATIONS
-
• There are no data from randomised controlled trials on the issue of patient satisfaction.
-
• The quality of data is not high.
-
• Surveys from representative samples of patients on maintenance antipsychotic medication have not been carried out.
Acknowledgements
The authors thank Dr Clive Adams for his expert assistance in carrying out the review.








eLetters
No eLetters have been published for this article.