Recent prospective investigations have reported that measures of both impaired neurodevelopment in childhood (delayed speech and motor milestones) (Reference Jones, Rodgers and MurrayJones et al, 1994) and poor intellectual functioning in adulthood (Reference David, Malmberg and BrandtDavid et al, 1997) are associated with the risk of adult-onset psychosis. Causal pathways underlying these associations are unclear. Three explanations have been suggested for the associations with low IQ at 18 years of age (Reference David, Malmberg and BrandtDavid et al, 1997). First, they could reflect the direct effect of impaired intellectual functioning on social interaction and social understanding, leading to misunderstandings, paranoia and social withdrawal (Reference Malmberg, Lewis and DavidMalmberg et al, 1998). Second, in utero exposures, birth complications or genes may influence aspects of neurodevelopment concerned both with intellectual performance and with risk of schizophrenia. Significantly, low birth weight is associated with poorer cognitive function in childhood (Reference Seidman, Buka and GoldsteinSeidman et al, 2000) and adulthood (Reference Richards, Hardy and KuhRichards et al, 2001), and with an increased risk of schizophrenia (Reference Geddes, Verdoux and TakeiGeddes et al, 1999; Reference Kunugi, Nanko and MurrayKunugi et al, 2001). Lastly, it is possible that these associations are partly explained by reverse causality: early disease processes may impact adversely on cognitive function, as indicated by the decline in intellectual performance with age in those who went on to develop schizophrenia in the British 1946 birth cohort (Reference Jones, Rodgers and MurrayJones et al, 1994). To investigate these associations further we have used linked birth, military conscription, socio-economic and psychiatric admissions data on a cohort of Swedish males undergoing conscription medical examinations, including psychological assessment, between 1990 and 1994.
METHOD
Data-set examined
The original study sample was based on 334 577 males born in Sweden between 1973 and 1980 and resident in Sweden at the time they were conscripted into the military between 1990 and 1997. Study members underwent medical examinations at conscription. Revised and modified psychological test procedures were introduced from August 1994 and completed in all six conscription centres by the end of that year (J. Lothigius, personal communication, 2002). The results of the original tests of intellectual performance are consequently available for only a small proportion (<1%) of subjects conscripted after October 1994, compared with 84% before this date. Therefore, we have restricted the analyses to subjects conscripted up to and including October 1994. All individuals in this study were thus examined by the same tests of intellectual performance. We excluded from our analysis subjects with schizophrenia or other non-affective psychosis diagnosed at the time of their military medical examination or who had been admitted to hospital with either of these diagnoses before conscription. Thus, our initial data-set was based on 197 613 males who were conscripted before October 1994 and who had no pre-army or conscription diagnosis of psychosis. The cases of disease examined in our analyses were therefore incident cases in the period following military medical examination.
Record linkage
Information on the study sample was obtained from a linkage between the Swedish medical birth registry, the military service conscription registry, the population and housing censuses of 1970 and 1990 and the Swedish in-patient discharge register (up to 31 December 1997). Hospital admissions were coded using ICD-9 and, for more recent years, ICD-10.
Disease outcomes
We examined associations with all non-affective, non-drug-related psychoses (ICD-9 295, 297-299; ICD-10 F20-F29). We categorised the participants into two groups: those admitted with a diagnosis of schizophrenia (ICD-9 295; ICD-10 F20); and those admitted with a diagnosis of non-affective, non-schizophrenic psychosis (ICD-9 297-9; ICD-10 F21-F29). Although the latter category included those diagnosed using ICD-9 as having ‘psychoses with origin specific to childhood’ (ICD-9 code 299), only one subject fell into this category. As this person was found to be well at the conscription medical and had no record of previous psychiatric admissions, we included this subject among our adult-onset psychoses.
To minimise misclassification of diagnosis, if subjects were admitted on more than one occasion, we used the latest diagnosis, assuming this to be the most accurate. The non-schizophrenic, non-affective group comprised patients with non-schizophrenic psychotic disorders not thought to be due to substance misuse or to be affective in origin. This group of diagnoses therefore included people who received a diagnosis of paranoid states or other non-organic psychoses; we excluded affective psychoses seeing that in ICD-9 this grouping also includes subjects with ‘endogenous depression’ whose aetiology may be different. Although schizoaffective disorders are coded differently in ICD-10 (as F25) rather than within the schizophrenia (ICD-9 295) grouping in ICD-9, there were no cases of this disorder, coded using ICD-10, in our data-set.
Ethical approval for the study was obtained from the Karolinska Institute research ethics committee.
Risk factors investigated
As part of the conscription process each young man undergoes a standard examination of physical health, intellectual capacity and psychological function. The physical examination includes measures of height and weight. The tests of intellectual function have been described in detail else-where (Reference David, Malmberg and BrandtDavid et al, 1997; Reference Jiang, Rasmussen and WassermanJiang et al, 1999; Reference OttoOtto, 1976; Reference Nilsson, Nyberg and OstergrenNilsson et al, 2001) but complete information is unavailable as they are considered classified military material. The fullest description is given by David et al (Reference David, Malmberg and Brandt1997). In brief, there are four basic tests: technical/mechanical skills with mathematical/physics problems; logic/general intelligence test; a verbal test detecting synonyms; and a test of visuo-spatial/geometric perception. We included one further test in this analysis: a test for the potential suitability of the conscript to be an officer, the score for which was based on a loosely structured interview with a psychologist.
Testing is carried out in six regional conscription centres. Central training and instruction of the psychologists who carry out the tests, and the use of a standard manual, help to ensure consistency (Reference Nilsson, Nyberg and OstergrenNilsson et al, 2001). Results from the five tests are standardised against data from previous years to give each subject a score from 1 to 9 for each scale (Reference David, Malmberg and BrandtDavid et al, 1997). Low scores indicate poor intellectual functioning.
We investigated the association of each of these measures of intellectual performance with subsequent hospital admission with a diagnosis of psychosis. These associations were examined in age-adjusted statistical models, in models with additional adjustment for growth in utero and in models with further adjustment for markers of adverse events at or after birth (see below).
We hypothesised that intellectually impaired subjects with well-educated parents would be at higher risk of developing psychosis, because such discordance might act as a marker of either impaired neurodevelopment, resulting from complications in utero and early childhood, or of stress arising from conflict between parental aspirations and offspring's intellectual potential (Reference Eaton and HarrisonEaton & Harrison, 2001). We therefore tested for interactions between cognitive function and parental education with regard to the risk of developing psychosis.
Statistical methods
All analyses were carried out in Stata version 6 for PC (StataCorp, 1996). We used Cox's proportional hazards models to assess the influence of the factors listed above on the incidence of schizophrenic and non-affective non-schizophrenic psychosis. Because of the low number of incident cases of psychosis and our desire to assess whether associations with intellectual function were linear, we grouped scores on the nine-point scale for each measure into three categories (1-3, 4-6 and 7-9) and used those scoring 7-9 (highest ranking on each scale) as the reference category in our models. Tests for linear and non-linear trends in the association between the test scores and psychosis were, however, based on the nine-point scale.
In our initial models we examined associations with each intellectual function scale adjusting only for age. In our subsequent models we controlled for markers of in-utero and birth exposures. We first controlled for markers of foetal growth, birth weight (<2500g, 2501-3000g, 3001-3500g, 3501-4000g and >4000g); birth length (as a continuous term); and gestational age (≤36, 37-41 and ≥41 weeks). In our fully adjusted models we assessed the effect of controlling additionally for: season of birth (spring, summer, autumn, winter); Apgar score (Reference ApgarApgar, 1953) at 1 min (≤6 or 7+); maternal parity (1, 2 or 3+); Caesarean section birth; maternal age (≤20, 20-24, 25-29, 30-34, 35+ years); head circumference (20-31 cm, 32-34cm, 35-36cm, 37-55cm); uterine atony/prolonged labour; congenital malformation; and parental education (both parents educated for more than 10 years/only one parent educated for more than 10 years/neither parent educated for more than 10 years).
To test for non-linearity in the observed associations we added a term for the explanatory variable squared (quadratic term) to models including a linear term for this variable. Tests for interaction or non-linearity are based on likelihood ratio tests comparing models with and without the relevant explanatory variables. Subjects are censored at the time of first admission, death or emigration. To investigate whether the associations with intellectual functioning diminished with increasing duration of follow-up we divided the follow-up time into two periods (≤2.9 years and >2.9 years), each containing half the incident cases. Follow-up ended on 31 December 1997.
RESULTS
Subjects included in main analyses
Of the 197 613 males in our original dataset, we excluded 87 970 because of missing information relating to their birth, conscription examination or parental education. Our main analyses were therefore based on 109 643 subjects with complete data for all these factors. As many subjects had missing data for one or more of the tests of intellectual performance, we assessed possible selection bias by comparing the characteristics of those with and without full data on each of the scales. Subjects with missing data when compared with those with full data tended to be of smaller size at birth (4.0% v. 2.5% weighed <2.5kg); to have lower Apgar scores (4.9% v. 4.0% scored ≤6); and a greater proportion had congenital malformations (5.9% v. 5.0%). Their adult height and body mass index were similar to those with full data but their parents were more highly educated. These differences, although slight, were statistically significant (P<0.01) because of the large sample size.
The mean age at the time of conscription was 18.2 (range 16.6-21.7) years. Subjects were followed-up for a mean 5.04 (range 0.03-7.83) years after their conscription medical examination. Over this time 60 (0.06%) subjects developed schizophrenia and 92 (0.08%) developed non-affective, non-schizophrenic psychosis. The annual incidence rate of non-affective psychosis was estimated as 0.27 per 1000 person-years and of schizophrenia as 0.11 per 1000 person-years. The mean length of time between conscription examination and hospital admission was 2.78 (range 0.33-6.00) years for schizophrenia and 2.96 (range 0.22-5.92) years for other non-affective psychoses. For all five intellectual function tests, a greater proportion of those who developed psychosis had low scores (1-3) than those who did not (Table 1).
Table 1 Distribution of intellectual function scores in subjects admitted to hospital with a diagnosis of schizophrenia or other non-affective psychosis and in subjects without such diagnoses

| Intellectual function test1 | Diagnosis | ||
|---|---|---|---|
| No diagnosis of any non-affective psychosis or schizophrenia (n=109 491) | Schizophrenia (n=60) | Non-schizophrenic, non-affective psychoses (n=92) | |
| Technical test score | |||
| 1-3 | 19294 (17.62%) | 32 (53.34%) | 34 (36.96%) |
| 4-6 | 62446 (57.03%) | 20 (33.33%) | 40 (43.48%) |
| 7-9 | 27751 (25.35%) | 8 (13.33%) | 18 (19.56%) |
| Logic test score | |||
| 1-3 | 18207 (16.63%) | 22 (36.67%) | 34 (36.96%) |
| 4-6 | 59285 (54.14%) | 29 (48.33%) | 40 (43.48%) |
| 7-9 | 31999 (29.23%) | 9 (15.00%) | 18 (19.56%) |
| Synonym test score | |||
| 1-3 | 21232 (19.39%) | 19 (31.67%) | 32 (34.78%) |
| 4-6 | 64577 (58.98%) | 32 (53.33%) | 42 (45.65%) |
| 7-9 | 23682 (21.63%) | 9 (15.00%) | 18 (19.57%) |
| Spatial test score | |||
| 1-3 | 21752 (19.87%) | 24 (40.00%) | 31 (33.70%) |
| 4-6 | 60257 (55.03%) | 25 (41.67%) | 42 (45.65%) |
| 7-9 | 27482 (25.10%) | 11 (18.33%) | 19 (20.65%) |
| Suitability for being an officer, test score | |||
| 1-3 | 19970 (18.24%) | 33 (55.00%) | 41 (44.56%) |
| 4-6 | 67512 (61.66%) | 24 (40.00%) | 40 (43.48%) |
| 7-9 | 22009 (20.10%) | 3 (5.00%) | 11 (11.96%) |
Age-adjusted and multivariable models
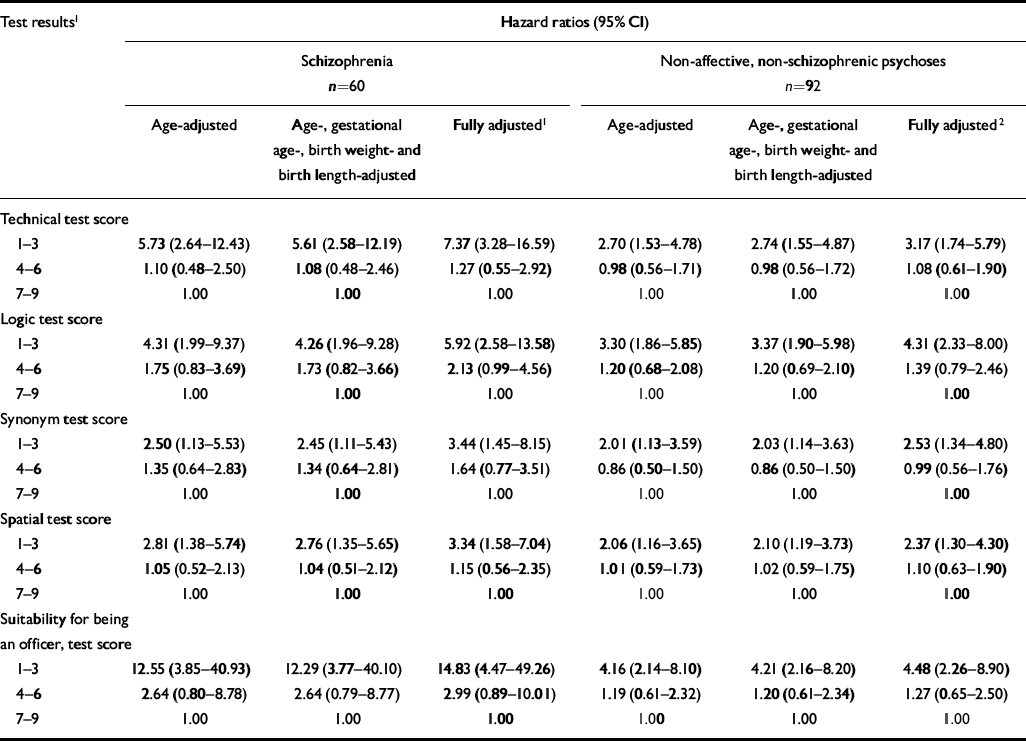
Table 2 presents the age-adjusted; birth weight-, birth length- and gestational age-adjusted; and fully adjusted analyses of disease risk in relation to test scores. For schizophrenia and non-affective non-schizophrenic psychosis, disease risk was greatly (2- to 14-fold) increased in those scoring 1-3 in each of the tests compared with those scoring 7-9. Risks were only marginally raised, or in some cases lower, among those scoring 4-6 compared with those scoring 7-9. Tests for non-linearity, using the continuous test scores, showed that for most intellectual test scores the trends were consistent with supralinear increases in risk with decreasing test results. There were two exceptions to this general pattern: the association between the schizophrenia and (a) the logic test, and (b) the test for the suitability for being an officer. Here the trends were consistent with a linear increase in risk with decreasing test scores.
Table 2 Age-adjusted, birth anthropometry-adjusted and fully adjusted hazard ratios of schizophrenia and other non-affective psychoses in relation to intellectual function test results
| Test results1 | Hazard ratios (95% CI) | |||||
|---|---|---|---|---|---|---|
| Schizophrenia n=60 | Non-affective, non-schizophrenic psychoses n=92 | |||||
| Age-adjusted | Age-, gestational age-, birth weight- and birth length-adjusted | Fully adjusted1 | Age-adjusted | Age-, gestational age-, birth weight- and birth length-adjusted | Fully adjusted2 | |
| Technical test score | ||||||
| 1-3 | 5.73 (2.64-12.43) | 5.61 (2.58-12.19) | 7.37 (3.28-16.59) | 2.70 (1.53-4.78) | 2.74 (1.55-4.87) | 3.17 (1.74-5.79) |
| 4-6 | 1.10 (0.48-2.50) | 1.08 (0.48-2.46) | 1.27 (0.55-2.92) | 0.98 (0.56-1.71) | 0.98 (0.56-1.72) | 1.08 (0.61-1.90) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 |
| Logic test score | ||||||
| 1-3 | 4.31 (1.99-9.37) | 4.26 (1.96-9.28) | 5.92 (2.58-13.58) | 3.30 (1.86-5.85) | 3.37 (1.90-5.98) | 4.31 (2.33-8.00) |
| 4-6 | 1.75 (0.83-3.69) | 1.73 (0.82-3.66) | 2.13 (0.99-4.56) | 1.20 (0.68-2.08) | 1.20 (0.69-2.10) | 1.39 (0.79-2.46) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 |
| Synonym test score | ||||||
| 1-3 | 2.50 (1.13-5.53) | 2.45 (1.11-5.43) | 3.44 (1.45-8.15) | 2.01 (1.13-3.59) | 2.03 (1.14-3.63) | 2.53 (1.34-4.80) |
| 4-6 | 1.35 (0.64-2.83) | 1.34 (0.64-2.81) | 1.64 (0.77-3.51) | 0.86 (0.50-1.50) | 0.86 (0.50-1.50) | 0.99 (0.56-1.76) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 |
| Spatial test score | ||||||
| 1-3 | 2.81 (1.38-5.74) | 2.76 (1.35-5.65) | 3.34 (1.58-7.04) | 2.06 (1.16-3.65) | 2.10 (1.19-3.73) | 2.37 (1.30-4.30) |
| 4-6 | 1.05 (0.52-2.13) | 1.04 (0.51-2.12) | 1.15 (0.56-2.35) | 1.01 (0.59-1.73) | 1.02 (0.59-1.75) | 1.10 (0.63-1.90) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 |
| Suitability for being an officer, test score | ||||||
| 1-3 | 12.55 (3.85-40.93) | 12.29 (3.77-40.10) | 14.83 (4.47-49.26) | 4.16 (2.14-8.10) | 4.21 (2.16-8.20) | 4.48 (2.26-8.90) |
| 4-6 | 2.64 (0.80-8.78) | 2.64 (0.79-8.77) | 2.99 (0.89-10.01) | 1.19 (0.61-2.32) | 1.20 (0.61-2.34) | 1.27 (0.65-2.50) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 |
For all measures of intellectual functioning, associations were stronger in relation to schizophrenia. The strongest predictor of risk was the assessment of the subject's suitability for officer status, with a hazard ratio of 12.55 (95% CI 3.85-40.93) among those scoring 1-3 in age-adjusted models. Controlling for birth weight, birth length and gestational age had little effect on these associations.
In a separate analysis, we found a linear association between gestational age-adjusted birth weight and all five measures of intellectual functioning. For every 1000 g increase in birth weight, technical test scores increased by 0.21 (95% CI 0.19-0.23) units, logic scores by 0.22 (95% CI 0.20-0.25), synonym tests by 0.12 (95% CI 0.10-0.15), spatial scores by 0.24 (95% CI 0.22-0.27) and officer status scores by 0.14 (95% CI 0.12-0.16).
In the fully adjusted models, where we controlled for a range of markers for obstetric complications and parental education, disease risk was higher than in the simple age-adjusted models. Addition of the measure of parental education to these multivariable models led to this increased risk, whereas the other factors examined had little effect on the estimates of risk.
Effects of early disease on cognitive function
To assess whether intellectual function may have been affected by early, pre-diagnostic disease processes (reverse causality) we investigated whether the strength of the association with intellectual function varied in cases diagnosed soon after conscription, compared with those admitted to hospital several years later (Table 3). For most of the tests examined, associations were some-what weaker in later-onset than early-onset cases, although confidence intervals were wide.
Table 3 Age-adjusted hazard ratios of early1- and late2-onset schizophrenia and other non-affective psychoses in relation to intellectual function tests

| Test results3 | Hazard ratios (95% CI) | |||
|---|---|---|---|---|
| Schizophrenia n=60 | Non-schizophrenic, non-affective psychoses n=92 | |||
| Early onset n=30 | Late onset n=30 | Early onset n=46 | Late onset n=46 | |
| Technical test score | ||||
| 1-3 | 6.11 (2.05-18.14) | 5.35 (1.78-16.13) | 3.76 (1.67-8.50) | 1.85 (0.81-4.23) |
| 4-6 | 1.00 (0.31-3.24) | 1.20 (0.38-3.76) | 0.94 (0.41-2.19) | 1.00 (0.48-2.11) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 |
| Logic test score | ||||
| 1-3 | 9.67 (2.14-43.63) | 2.79 (1.08-7.20) | 5.54 (2.21-13.87) | 2.18 (1.02-4.67) |
| 4-6 | 4.59 (1.06-19.89) | 0.93 (0.37-2.38) | 1.88 (0.76-4.67) | 0.85 (0.41-1.76) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 |
| Synonym test score | ||||
| 1-3 | 2.93 (1.04-8.25) | 1.86 (0.52-6.61) | 2.46 (1.07-5.66) | 1.64 (0.73-3.70) |
| 4-6 | 0.89 (0.31-2.52) | 1.95 (0.67-5.71) | 0.91 (0.40-2.06) | 0.83 (0.39-1.75) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 |
| Spatial test score | ||||
| 1-3 | 3.55 (1.28-9.85) | 2.19 (0.79-6.02) | 3.04 (1.26-7.34) | 1.49 (0.69-3.22) |
| 4-6 | 1.01 (0.35-2.90) | 1.09 (0.42-2.83) | 1.43 (0.61-3.34) | 0.76 (0.37-1.57) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 |
| Suitability for being an officer, test score | ||||
| 1-3 | 8.86 (2.03-38.53) | 19.99 (2.66-150.23) | 7.08 (2.47-20.30) | 2.45 (1.00-6.02) |
| 4-6 | 1.96 (0.44-8.77) | 3.99 (0.52-30.68) | 1.30 (0.43-3.88) | 1.13 (0.49-2.63) |
| 7-9 | 1.00 | 1.00 | 1.00 | 1.00 |
Interactions with parental education
For only one of the test results (spatial perception) was there evidence that the association with schizophrenia differed depending on parental education (P for interaction=0.03) (Table 4). Risk was greatest among poorly functioning conscripts who had well-educated parents. The hazard ratio for schizophrenia, based on only 16 cases, was 6.48 (2.53-16.53) in the low-scoring (1-3) group with the best-educated parents, compared with those with high intellectual test scores and well-educated parents. Although there was a significant interaction for only one of the test results, inspection of Table 4 shows that for all five tests of intellectual functioning risk of schizophrenia was consistently greater in the group of poorly functioning conscripts with well-educated parents.
Table 4 Risk of developing schizophrenia in relation to intellectual function tests at 18 years of age and parents' education1

| Test results stratified by parental education | Schizophrenia hazard ratios (95% CI) | ||
|---|---|---|---|
| Low score (1-3)2 | Medium score (4-6) | High score (7-9) | |
| Technical test | |||
| Both ≤ 10 years | 3.07 (1.03-9.13) (n=7) | 0.59 (0.15-2.36) (n=3) | 0.78 (0.09-6.49) (n=1) |
| Either ≤ 10 years | 2.57 (0.86-7.64) (n=7) | 0.85 (0.28-2.52) (n=7) | 0.34 (0.04-2.85) (n=1) |
| Both > 10 years | 8.53 (3.39-21.50) (n=18) | 1.02 (0.37-2.80) (n=10) | 1.00 (n=6) |
| Likelihood test for interaction: LR χ2 (d.f. 4)=2.73, P=0.60 | |||
| Logic test | |||
| Both ≤ 10 years | 3.57 (1.09-11.70) (n=6) | 0.87 (0.21-3.65) (n=3) | 1.95 (0.38-10.04) (n=2) |
| Either ≤ 10 years | 2.68 (0.78-9.27) (n=5) | 1.43 (0.47-4.37) (n=8) | 0.83 (0.16-4.28) (n=2) |
| Both > 10 years | 8.91 (3.10-25.65) (n=11) | 2.77 (1.03-7.45) (n=18) | 1.00 (n=5) |
| Likelihood test for interaction: LR χ2 (d.f. 4)=3.73, P=0.44 | |||
| Synonym test | |||
| Both ≤ 10 years | 2.47 (0.83-7.34) (n=7) | 0.57 (0.14-2.30) (n=3) | 0.96 (0.12-8.01) (n=1) |
| Either ≤ 10 years | 0.95 (0.24-3.81) (n=3) | 1.11 (0.40-3.07) (n=10) | 0.81 (0.16-4.02) (n=2) |
| Both > 10 years | 4.44 (1.58-12.49) (n=9) | 1.76 (0.70-4.41) (n=19) | 1.00 (n=6) |
| Likelihood test for interaction: LR χ2 (d.f. 4)=4.14, P=0.39 | |||
| Spatial test | |||
| Both ≤ 10 years | 0.78 (0.16-3.86) (n=2) | 1.23 (0.40-3.81) (n=6) | 2.10 (0.52-8.40) (n=3) |
| Either ≤ 10 years | 1.91 (0.62-5.92) (n=6) | 0.87 (0.29-2.60) (n=7) | 0.64 (0.13-3.18) (n=2) |
| Both > 10 years | 6.48 (2.53-16.56) (n=16) | 1.21 (0.45-3.22) (n=12) | 1.00 (n=6) |
| Likelihood test for interaction: LR χ2 (d.f. 4)=10.69, P=0.030 | |||
| Suitability for being an officer test | |||
| Both ≤ 10 years | 8.09 (1.68-38.94) (n=7) | 1.78 (0.33-9.73) (n=4) | (n=0) |
| Either ≤ 10 years | 6.43 (1.33-30.94) (n=7) | 1.93 (0.40-9.28) (n=7) | 1.06 (0.10-11.64) (n=1) |
| Both > 10 years | 19.09 (4.45-82.00) (n=19) | 3.01 (0.68-13.35) (n=13) | 1.00 (n=2) |
| Likelihood test for interaction: LR χ2 (d.f. 4)=1.93, P=0.59 | |||
There were no significant interactions between intellectual function and parental education with respect to other psychoses. Furthermore, inspection of the hazard ratios in relation to test results and parental education did not show any evidence that low-scoring offspring of well-educated parents were at greater risk than those of less-educated parents (data not shown).
DISCUSSION
Main findings
Our results suggest that cerebral damage arising as a result of prenatal and obstetric adversity, as indicated by the measures available to us, does not underlie the association between poor intellectual performance and psychosis. In keeping with other studies (Reference David, Malmberg and BrandtDavid et al, 1997; Reference Davidson, Reichenberg and RabinowitzDavidson et al, 1999) we found that low scores on a range of tests of intellectual functioning performed around the age of 18 years were strongly associated with an increased risk of developing non-affective psychosis. There is some evidence that this association is strongest for cases arising in the years soon after measurement. The test most strongly associated with increased risk was the general assessment of suitability for officer status, but risk was increased across a range of test scores indicating global underperformance. Risks were somewhat stronger in relation to schizophrenia than other non-affective psychoses and were largely confined to the subjects with lowest scores on these tests. Controlling for parental educational status did not attenuate the observed associations.
Study strengths
We used routinely recorded data on birth-related, parental and adult exposures, collected before disease onset from a large group of young men from Sweden. The availability of birth as well as adult measures allowed us to investigate further the possible causal pathways suggested by David et al in their analysis of an earlier-born conscript cohort (Reference David, Malmberg and BrandtDavid et al, 1997). The range of test results available for analysis enabled us to determine whether poor performance is restricted to a particular domain of cognitive function. As case ascertainment was from a national inpatient register, the possibility of selection bias was reduced, although it is feasible that intellectual performance may influence the likelihood of admission.
Study limitations
Our case ascertainment was based on hospital-admitted cases only and used diagnoses recorded on an administrative database. Studies in the UK, however, indicate that even in areas with relatively community-oriented services, over 80% of cases are admitted within 3 years of presentation (Reference Sipos, Harrison and GunnellSipos et al, 2001). Furthermore, analyses of diagnoses recorded on the Swedish in-patient discharge register indicate that schizophrenia is diagnosed with reasonable accuracy (Reference David, Malmberg and BrandtDavid et al, 1997).
Second, our analysis was based on men with illness onset in early adulthood. It is possible that associations seen in males with early-onset schizophrenia may differ from those seen in females and in people with late-onset schizophrenia.
Third, as family history of psychotic disorder was not available we were unable to control for its potential confounding effects in this analysis. It is possible, for example, that the intellectual development of children brought up in a household where one or both parents suffer from psychosis may be impaired. However, only 5-10% of cases are likely to have had an affected parent (Reference Dalman, Allebeck and CullbergDalman et al, 1999; Reference Mortensen, Pedersen and WestergaardMortensen et al, 1999), whereas 30-50% of cases had low scores on the tests of intellectual functioning, making this possible effect unlikely to fully explain the observed associations.
Comparison with other studies
In an earlier analysis of Swedish conscripts examined in 1969-70, linear associations with IQ were reported which were equally strong in cases of psychosis occurring soon after conscription and in those occurring 10 or more years later (Reference David, Malmberg and BrandtDavid et al, 1997). In our analysis, the associations were generally weaker in later-onset cases. Similarly, in a cohort of Israeli conscripts followed-up for 8 years there was some evidence that the strength of association of measures of cognitive function and behaviour with schizophrenia diminished over follow-up (Reference Rabinowitz, Reichenberg and WeiserRabinowitz et al, 2000). However, in this Israeli cohort declines were seen for only one of four measures of cognitive function (Raven's Progressive Matrices) and one of four measures of behaviour (social functioning) (Reference Rabinowitz, Reichenberg and WeiserRabinowitz et al, 2000).
In keeping with the possibility that declines in cognitive function before disease onset explain the associations seen in the conscript cohorts described above, the British 1946 birth cohort and the National Collaborative Perinatal Project reported that associations with schizophrenia (Reference Jones, Rodgers and MurrayJones et al, 1994) and psychotic symptoms (Reference Kremen, Buka and SeidmanKremen et al, 1998) were stronger for cognitive function measures recorded nearer the time of diagnosis. Other studies, however, have reported no deterioration in intellectual function in subjects before development of schizophrenia (Reference Cannon, Bearden and HollisterCannon et al, 2000) and have found that non-affected siblings of children who go on to develop schizophrenia have similar deficits in cognitive function (Reference Cannon, Bearden and HollisterCannon et al, 2000), indicating a genetic or shared environmental influence on risk. David et al (Reference David, Malmberg and Brandt1997) reported that the single test result most strongly related to risk of schizophrenia was mechanical knowledge (equivalent to the technical test in our analysis). Likewise, of the four specific tests we examined, the strongest associations were seen in relation to the technical test.
Parental education
Our results showed that the risk of schizophrenia was greatest among poorly functioning conscripts who had well-educated parents. Eaton & Harrison (Reference Eaton and Harrison2001) have proposed that the early adult task of formulating a life plan is one of the most complex cognitive activities a person will ever engage in (Reference Eaton and HarrisonEaton & Harrison, 2001). Formulating a life plan involves psychological processes of aspiration, interest and estimation of probability of success, in addition to selecting, prioritising and balancing complex and subtly different future actions. The complexity of these cognitive tasks, and the associated psychological strain, are likely to be accentuated in low-performing children and low-performing young adults whose parents have higher educational backgrounds and expectations. Our findings were consistent with this speculation, and merit replication in other studies.
There are three other possible explanations, however. First, the difference may reflect environmentally induced neuro-developmental insults, with the parents' educational levels indicating the individual's potential rather than actual performance. Second, highly educated parents may be more vigilant and more reactive to the early manifestations of disorder, leading to biased early-case detection. If this is so, the strength of our finding should diminish with longer follow-up of the cohort. Lastly, it is possible that children of more highly educated parents are likely to have higher cognitive function scores and so, in the prodromal stages of schizophrenia, more may move further down the scale of intellectual functioning. In contrast, children of less well-educated parents are more likely to have lower intellectual test scores, and to be in the lowest category for these tests already, and so may not change category to the same degree.
Possible mechanisms underlying observed associations
Our study suggests that pre- and perinatal exposures do not underlie the association between poor intellectual performance and psychosis. This provides some evidence against Weinberger's model of fixed lesions acquired in early life interacting with later brain maturational processes to cause disease (Reference WeinbergerWeinberger, 1987). Other factors, such as genetic predisposition or later environmental exposures, may therefore be independently important. Such factors form part of recently proposed two- and three-hit models of schizophrenia pathogenesis (Reference PearlsonPearlson, 2000; Reference Velakoulis, Wood and McGorryVelakoulis et al, 2000) which suggest the importance of additive and interactive effects of environmental risk factors against a background of genetic predisposition. It has been suggested, for example, that insufficient synaptic elimination, synaptic expansion and axonal sprouting in adolescence may be important in schizophrenia aetiology (Reference Feinberg, Keshavan and MurrayFeinberg 1997); these processes may be influenced by environmental as well as genetic factors.
The associations we found with intellectual function were not specific to any single test domain, indicating that they reflect global impairment. The strongest impairments previously seen in relation to schizophrenia are for interpersonal skills, speed of thought and executive planning skills (Reference Jones, Rodgers and MurrayJones et al, 1994; Reference Diforio, Walker and KestlerDiforio et al, 2000; Reference Rabinowitz, Reichenberg and WeiserRabinowitz et al, 2000); these are likely to have been aggregated under the global assessment of suitability to be an officer.
The lack of consistent evidence of a dose—response effect, together with the observation that associations were generally stronger among cases arising soon after examination, provide some evidence that pre-diagnostic pathophysiological processes may have led to the observed associations. This is consistent with the possibility that rather than being a risk factor for psychosis in its own right, poor test performance may arise as a result of early disease processes (reverse causality). Alternatively, more impaired individuals may succumb sooner to the challenges of independent adult life, so that the risk associated with impairment appears greatest for early-onset cases. Against such an argument is the consistent observation in the literature that the mean age of disease onset is later in females than in males, whereas females reach sexual maturity and independence at an earlier age than males (Reference EatonEaton, 1988).
Long-term follow-up of this cohort will enable us to investigate some of the issues raised here. In particular, we will be able to determine the extent to which the observed associations with respect to subgroups are maintained in analyses with larger numbers of cases and later-onset cases. In this study poor intellectual functioning strongly predicted future risk of schizophrenia. For some tests over 50% of affected individuals but less than 20% of unaffected individuals scored 1-3, indicating the importance of gaining a greater understanding of the processes lying behind these associations.
CLINICAL IMPLICATIONS
-
▪ Poor intellectual performance at 18 years of age is strongly associated with the risk of developing schizophrenia and other non-affective psychoses in early adulthood.
-
▪ Cerebral damage resulting from obstetric complications or in-utero growth impairment does not appear to explain the associations between intellectual impairment and psychosis, but the adverse effects of prodromal disease on cognition may in part contribute to its associations with psychosis.
-
▪ Risk of schizophrenia in relation to poor intellectual performance appears to be greatest among subjects with well-educated parents.
LIMITATIONS
-
▪ Only hospital-admitted cases were studied and we used diagnoses as recorded on an administrative database.
-
▪ The analysis was restricted to young males with early-onset psychosis.
-
▪ We were unable to assess the influence on observed associations of a family history of psychotic disorder.







eLetters
No eLetters have been published for this article.