Community-based surveys have found that otherwise well individuals endorse items related to psychotic symptoms (Reference Eaton, Romanoski and AnthonyEaton et al, 1991; Reference Van Os, Hanssen and Bijlvan Os et al, 2000). An Australian study identified an increased likelihood of delusional experiences associated with certain demographic variables, including male gender, younger age, unemployment, migrant status (but only those from non-English-speaking backgrounds), urban residence, lower income, lower educational achievement and living alone (Reference Scott, Chant and AndrewsScott et al, 2006). Cannabis dependence and alcohol dependence were also found to be associated with delusional experiences (Reference Degenhardt and HallDegenhardt & Hall, 2001). A number of studies have now shown an association between traumatic events in childhood and psychotic symptoms (Reference Janssen, Krabbendam and BakJanssen et al, 2004; Reference Spauwen, Krabbendam and LiebSpauwen et al, 2006). We had the opportunity to further examine the association between exposure to trauma, post-traumatic stress disorder (PTSD) and delusional experiences in a large, representative community-based Australian sample.
METHOD
The 1997 National Survey of Mental Health and Wellbeing was conducted by the Australian Bureau of Statistics from May to August 1997 from a representative sample (random stratified, multistage area sampling) of persons living in private dwellings throughout Australia (Reference Andrews, Henderson and HallAndrews et al, 2001). The sample excluded special dwellings (e.g. hospitals, nursing homes and hostels), and dwellings in remote and sparsely populated areas of Australia. Approximately 13 600 private dwellings were initially selected in the survey sample. One person aged 18 years or over from each dwelling was subsequently invited to participate, with 10 641 individuals agreeing to do so, a response rate of 78%. Respondents were asked about symptoms in the previous 12 months. The presence of mental disorders was assessed by trained non-clinician interviewers using a modified version of the Composite International Diagnostic Interview (CIDI; World Health Organization, 1993).
As this particular survey was designed to identify common mental disorders, the full CIDI sections required to diagnose psychotic disorders were not included. However, the interview included items designed to identify individuals who might be psychotic. There were three ‘screen’ items, each with follow-up probes, as well as an item related to past diagnosis of schizophrenia (Appendix 1). The psychosis probe questions were only asked if the respondent had endorsed the related screen item. These items relate to delusional experiences such as delusions of control, thought interference and passivity; delusions of reference or persecution; and grandiose delusions. Responses were coded as ‘yes’, ‘no’ or (for probes only) ‘not applicable’. All participants were administered the three screen items; people who responded positively to any of the screen items were then asked the related follow-up probe question. Positive endorsement of a delusional experience was recorded in individuals who responded ‘yes’ to question G1A, ‘yes’ to G2A or ‘no’ to GA3 (see Appendix 1). For this analysis, delusional experience was dichotomised into none v. one or more, as there were relatively few respondents who endorsed two or three probe items (Reference Scott, Chant and AndrewsScott et al, 2006).
To examine the association between exposure to traumatic events and delusional experiences, trauma was assessed from the questions relating to the diagnostic section of the CIDI for eliciting PTSD. The CIDI asks ten questions about possible traumatic events that people might have experienced (see Appendix 2). If respondents had experienced one or more of these traumatic events, they were then asked further questions from the CIDI (World Health Organization, 1993) to either establish or exclude a diagnosis of PTSD.
Participants were then divided into three new groups:
-
(a) those denying any life-threatening or overwhelming traumatic events (no trauma);
-
(b) those who had experienced at least one traumatic event but who did not meet criteria for PTSD (trauma without PTSD);
-
(c) those who had experienced at least one traumatic event and who had PTSD (trauma with PTSD).
The main analyses examined the relationship between exposure to traumatic events and endorsement of one or more delusional experience. Unadjusted relative risk for endorsement (and 95% confidence intervals) are presented for trauma without PTSD and trauma with PTSD, both with and without adjustment for age (18–29 years, 30–39 years, 40–49 years, 50–64 years, 65 years and over) and gender. Because delusional experiences are known to be associated with psychosis and substance misuse, the main analyses adjusted for, first, a past diagnosis of schizophrenia (self-report), and second, cannabis and alcohol dependence (Reference Degenhardt and HallDegenhardt & Hall, 2001). As a secondary analysis, we also adjusted for demographic variables previously associated with delusional experiences: marital status, country of birth, socio-economic status, urbanicity and employment status (Reference Scott, Chant and AndrewsScott et al, 2006).
We then explored if delusional experiences were associated with exposure to each particular type of traumatic event. For participants exposed to each trauma, the relative risk of endorsement of any delusional experience, adjusting for age and gender, was calculated (see Table 3). We also examined if there was a dose–response relationship between exposure to a greater number of different types of traumatic events and endorsement of delusional experiences. Respondents were divided into four groups:
-
(a) those who reported no exposure to trauma;
-
(b) those who reported exposure to one or two different types of traumatic events;
-
(c) those who reported exposure to three or four different types of trauma;
-
(d) those who reported exposure to five or more different types of traumatic events.
Finally, as a secondary analysis, we explored if those who had previously received a diagnosis of schizophrenia were more likely to endorse delusional experiences, and to report past exposure to trauma.
The survey data were analysed with the appropriate population weights (in order to generate appropriate standard errors) using SAS version 9.1 for Windows. Significant differences were identified by standardised two-tailed Z-scores adjusted for multiple pairwise comparisons by the Bonferroni procedure. Estimates with standard errors less than 25% of the estimate value are considered to be reliable.
RESULTS
Of the 10 641 persons surveyed, 478 (4.49%) endorsed one or more delusional experiences. Within the sample, 4537 (42.6%) reported that they had never been exposed to a traumatic event, whereas 5725 (53.8%) reported that they had been exposed to a traumatic event but did not meet criteria for PTSD. However, 379 (3.6%) participants met diagnostic criteria for PTSD.
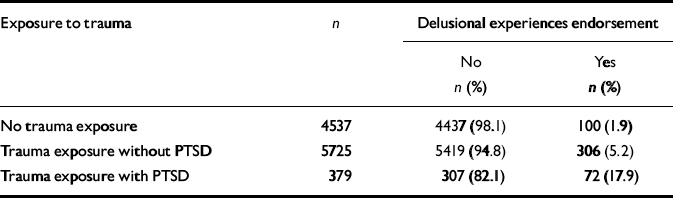
Table 1 shows the rate of endorsement of delusional experiences in participants from the three groups of trauma exposure. Table 2 shows the relative risk of endorsement where the reference group is those who have no history of exposure to trauma. Endorsement of any delusional experience was significantly more likely in individuals who had been exposed to a traumatic event in their lifetime. The relative risk increased significantly in participants who had PTSD (note that the confidence intervals for the relative risks do not overlap between those with or without PTSD). The association between trauma (with and without PTSD) remained significant after adjusting for age, gender, past diagnosis of schizophrenia, and alcohol and cannabis dependence. Further analysis was undertaken adjusting for the demographic factors previously associated with endorsement of delusional experience (i.e. marital status, country of birth, socio-economic status, urbanicity and employment status). The significance and direction of the associations between trauma (with and without PTSD) and delusional experience were essentially unaltered (data not shown).
Table 1 Exposure to trauma and any delusional experience
| Exposure to trauma | n | Delusional experiences endorsement | |
|---|---|---|---|
| No n (%) | Yes n (%) | ||
| No trauma exposure | 4537 | 4437 (98.1) | 100 (1.9) |
| Trauma exposure without PTSD | 5725 | 5419 (94.8) | 306 (5.2) |
| Trauma exposure with PTSD | 379 | 307 (82.1) | 72 (17.9) |
Table 2 Relative risk of delusional experience endorsement with any exposure to trauma

| Exposure to trauma | Delusional experience endorsement | ||
|---|---|---|---|
| Unadjusted RR (95% CI) | Adjusted for gender and age RR (95% CI) | Adjusted for gender, age, cannabis or alcohol dependence and past diagnosis of schizophrenia RR (95% CI) | |
| No trauma exposure | Reference | Reference | Reference |
| Trauma exposure without PTSD | 2.68 (2.18-3.30)* | 2.45 (1.94-3.10)* | 2.03 (1.61-2.57)* |
| Trauma exposure with PTSD | 9.24 (6.95-12.27)* | 9.22 (6.73-12.62)* | 6.37 (4.54-8.94)* |
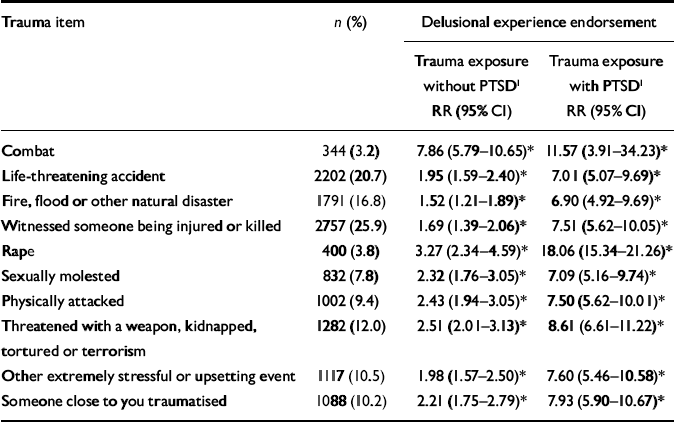
Table 3 shows the relative risk of endorsement of any delusional experience with each type of traumatic event after adjusting for age and gender. The relative risk varied but remained significant with exposure to all traumas. The relative risk of endorsement increased when the participants also met diagnostic criteria for PTSD. Table 4 shows that the relative risk of endorsement of delusional experience was significantly increased in the participants exposed to a greater number of different types of traumatic event (χ2=26.74, d.f.=2, P<0.001).
Table 3 Relative risk of delusional experience endorsement with exposure to different trauma
| Trauma item | n (%) | Delusional experience endorsement | |
|---|---|---|---|
| Trauma exposure without PTSD1 RR (95% CI) | Trauma exposure with PTSD1 RR (95% CI) | ||
| Combat | 344 (3.2) | 7.86 (5.79-10.65)* | 11.57 (3.91-34.23)* |
| Life-threatening accident | 2202 (20.7) | 1.95 (1.59-2.40)* | 7.01 (5.07-9.69)* |
| Fire, flood or other natural disaster | 1791 (16.8) | 1.52 (1.21-1.89)* | 6.90 (4.92-9.69)* |
| Witnessed someone being injured or killed | 2757 (25.9) | 1.69 (1.39-2.06)* | 7.51 (5.62-10.05)* |
| Rape | 400 (3.8) | 3.27 (2.34-4.59)* | 18.06 (15.34-21.26)* |
| Sexually molested | 832 (7.8) | 2.32 (1.76-3.05)* | 7.09 (5.16-9.74)* |
| Physically attacked | 1002 (9.4) | 2.43 (1.94-3.05)* | 7.50 (5.62-10.01)* |
| Threatened with a weapon, kidnapped, tortured or terrorism | 1282 (12.0) | 2.51 (2.01-3.13)* | 8.61 (6.61-11.22)* |
| Other extremely stressful or upsetting event | 1117 (10.5) | 1.98 (1.57-2.50)* | 7.60 (5.46-10.58)* |
| Someone close to you traumatised | 1088 (10.2) | 2.21 (1.75-2.79)* | 7.93 (5.90-10.67)* |
Table 4 Relative risk of delusional experience endorsement and exposure to the number of different types of traumatic events

| Number of different types of traumatic events | n (%) | Delusional experiences endorsement RR (95% CI) |
|---|---|---|
| No trauma | 4537 (42.6) | Reference |
| 1 or 2 | 4287 (40.3) | 2.51 (2.02-3.13)1 |
| 3 or 4 | 1392 (13.1) | 2.93 (2.22-3.86)1 |
| 5 or more | 425 (4) | 9.54 (7.26-12.53)1 |
In the entire sample, 87 persons (0.82%) reported that they had received a past diagnosis of schizophrenia. Compared with the remainder of the sample, this group were more likely to report a delusional experience (RR=8.30, 95% CI 5.82–11.83, adjusted for age and gender); however, they were not significantly more likely to report past exposure to trauma (RR=1.12, 95% CI 0.72–1.76).
DISCUSSION
Based on the largest sample to date, we found that individuals who had been exposed to a traumatic event were more likely to report delusional experiences. There was a dose–response relationship between the variables of interest: those who reported exposure to a greater number of different types of traumatic events were more likely to report delusional experiences. Furthermore, those who had developed PTSD after exposure to traumatic events were also more likely to report delusional experiences. The association between trauma, PTSD and delusional experiences persisted after controlling for factors known to be associated with psychotic symptoms. The association remained significant for each type of trauma examined, including those more likely to occur in childhood (sexual molestation) and those of adult life (direct combat).
Trauma, PTSD and psychotic symptoms
A number of community-based studies from different countries have shown an association between exposure to trauma and psychotic symptoms. Previous community surveys have shown an association between child abuse and psychotic symptoms (Reference Ross, Anderson and ClarkRoss et al, 1994; Reference Janssen, Krabbendam and BakJanssen et al, 2004; Reference Whitfield, Dube and FelittiWhitfield et al, 2005; Reference Shevlin, Dorahy and AdamsonShevlin et al, 2007). Another study has shown an association between PTSD and positive psychotic symptoms (Reference Sareen, Cox and GoodwinSareen et al, 2005). Two further studies have reported psychotic symptoms associated with traumatic events other than child abuse (Reference Bebbington, Bhugra and BrughaBebbington et al, 2004; Reference Spauwen, Krabbendam and LiebSpauwen et al, 2006).
We found that delusional experiences were associated with all types of trauma. The association was especially strong in those who had reported rape. Bebbington et al (Reference Bebbington, Bhugra and Brugha2004) reported a strong association between childhood sexual abuse and psychotic disorder, whereas Spauwen et al (Reference Spauwen, Krabbendam and Lieb2006) found the association was most strong in people who had exposure to a natural catastrophe.
To the best of our knowledge, this is the first study to show that PTSD complicating exposure to trauma increases the likelihood of endorsement of delusional experience compared with trauma exposure without PTSD. We suggest that people with PTSD have had more adverse psychological adjustments to traumatic events. Our study also found a significant dose–response relationship between exposure to traumatic events (as assessed by the number of different types of traumatic events) and increased likelihood of endorsing delusional experiences. This is consistent with the study of Spauwen et al (Reference Spauwen, Krabbendam and Lieb2006), who found increased psychotic symptoms in people exposed to a greater number of traumatic events.
Pathways of causality
Although cross-sectional surveys such as this study do not allow us to untangle the web of causation underpinning this association, several potential pathways warrant consideration. Delusional experiences could reflect a final common pathway for a wide range of adverse exposures such as substance misuse, trauma or other general stressors (e.g. migrant status, lack of significant other, unemployment). In other words, delusional experiences may be diffuse, non-specific ‘surface markers’ that emerge from a wide variety of biological and/or environmental risk factors (Reference Degenhardt and HallDegenhardt & Hall, 2001; Reference Van Os and McGuffinvan Os & McGuffin, 2003; Reference Scott, Chant and AndrewsScott et al, 2006).
From a different perspective, delusional experiences associated with trauma could be viewed as dissociative phenomena (Reference Vander Kolk, Pelcovitz and Rothvan der Kolk et al, 1996). Other researchers have noted the close links between trauma, dissociation and psychotic symptoms (Reference StartupStartup, 1999). Although conceptually distinct, in the absence of a detailed clinical interview, delusional experience as an expression of dissociation may be phenomenologically indistinguishable from delusions reported in the prodrome of psychosis. The symptomatic overlap of these syndromes and the growing body of evidence linking trauma and psychotic symptoms suggests that the taxonomy of these symptoms warrants closer scrutiny.
It is also feasible that exposure to trauma in susceptible individuals might be a risk-modifying factor (a component cause) for psychosis, through as yet unidentified mechanisms. For example, a number of authors postulate that dysregulation of the hypothalamic–pituitary–adrenal axis with elevated cortisol levels could contribute to the hippocampal changes that are associated with the onset of psychosis (Reference Read, Perry and MoskowitzRead et al, 2001; Reference Corcoran, Walker and HuotCorcoran et al, 2003). Exposure to chronic stress and elevated cortisol levels are associated with hippocampal changes (Reference SapolskySapolsky, 1996) and reduced hippocampal volume is a relatively consistent finding in imaging studies of schizophrenia (Reference Wright, Rabe-Hesketh and WoodruffWright et al, 2000). Thus, trauma might lead to altered stress hormones, which might then ‘catalyse’ the neurobiological mechanisms contributing to the onset of psychosis. Other mechanisms linking stress (e.g. ‘social defeat’) to risk of psychosis through dysregulation of dopaminergic pathways have also been proposed (Reference Selten and Cantor-GraaeSelten & Cantor-Graae, 2005)
Empirical support for trauma as a causal factor for psychosis is inconsistent. One prospective study showed no increase in rates of schizophrenia in adults who had been ascertained by child protection services as sexually abused in childhood (Reference Spataro, Mullen and BurgessSpataro et al, 2004). However, there were significant limitations in this study, identified by both the authors and others (Read & Hammersley, 2005). In contrast, two studies have prospectively found an increased incidence of psychotic symptoms in those who reported exposure to traumatic events (Reference Janssen, Krabbendam and BakJanssen et al, 2004; Reference Spauwen, Krabbendam and LiebSpauwen et al, 2006). The notion that traumatic events cause delusions is lent some weight by the dose–response relationship identified in this study and in a previous study (Reference Spauwen, Krabbendam and LiebSpauwen et al, 2006). Although there is now clear evidence of an association between traumatic events, PTSD and psychotic symptoms (Reference Bebbington, Bhugra and BrughaBebbington et al, 2004; Reference Janssen, Krabbendam and BakJanssen et al, 2004; Reference Sareen, Cox and GoodwinSareen et al, 2005; Reference Spauwen, Krabbendam and LiebSpauwen et al, 2006), the explanation for this association requires further investigation.
Study limitations
Our study has a number of limitations. Only three probe items were used to measure delusional experiences, and the study was not able to address other psychotic symptoms such as hallucinations. The version of the CIDI used in this study was not able to generate diagnoses of psychotic disorders. Although 87 participants reported a past diagnosis of schizophrenia, the validity of this diagnosis could not be formally tested. Furthermore, although the CIDI allows counts of up to ten different types of trauma, it does not provide information on the frequency of exposure to these events (i.e. an individual might be repeatedly exposed to one particular type of event). The interpretation of endorsement of delusional experience also requires a degree of caution, as the CIDI interviews were conducted by trained laypeople rather than by clinicians.
We have no definitive information about the timing of the exposure to the traumatic event, and therefore cannot differentiate between trauma experienced in childhood and adolescence and that happening later in life. Thus, we cannot determine if the trauma exposure preceded the development of delusional experience. However, other studies of childhood trauma and psychotic symptoms showed that the traumatic events preceded the onset of psychotic symptoms (Reference Janssen, Krabbendam and BakJanssen et al, 2004; Reference Spauwen, Krabbendam and LiebSpauwen et al, 2006).
Finally, it is possible that individuals who experience delusions might be biased to overreport past exposure to trauma. However, it seems less feasible that such individuals would be likely to selectively endorse the symptoms of PTSD. Moreover, others have argued that it is more likely that traumatic events are underreported by people with mental disorders (Reference Read, Hammersley and MullenRead et al, 2005, Reference Read, van Os and MorrisonRead et al, 2005).
Clinical implications
With the growing evidence of an association between trauma and psychotic symptoms, clinicians and researchers need to ask people with psychotic symptoms about past exposure to traumatic events. In the light of findings that psychotic symptoms such as delusional experiences can predict later frank psychosis (Reference Yung, Phillips and YuenYung et al, 2003), the results of our study highlight the role of trauma exposure and PTSD as potential risk-modifying factors for psychosis. If PTSD is a component cause in only a small group of individuals with psychosis, then prompt treatment to reduce the risk of developing PTSD might also be able to avert some cases of delusional experiences – and possibly later psychosis (Reference DavidsonDavidson, 2004). From a different perspective, psychotic symptoms as part of the phenomenology of PTSD may give rise to diagnostic uncertainty. There is potential for patients with PTSD to be incorrectly diagnosed with a psychotic illness and receive inappropriate management (Reference Seedat, Stein and OosthuizenSeedat et al, 2003).
Finally, the association between PTSD and psychosis is broadly consistent with the renewed interest in social stress as a factor contributing to the high rates of schizophrenia in urban sites and in certain migrant groups (Reference Van Os, Krabbendam and Myin-Germeysvan Os et al, 2005). Regardless of the mechanisms of action and the exact nature of the causal pathways between PTSD, delusional experiences and psychosis, a more detailed understanding of the full spectrum of psychotic-like experiences in the general population might provide important new clues to help us understand the aetiopathogenesis of a range of psychiatric conditions.
APPENDIX 1
Screen items and probes for psychosis
Items selected from the Composite International Diagnostic Interview (World Health Organization, 1993) to identify possible cases of psychosis.
Screen G1
‘In the past 12 months, have you felt that your thoughts were being directly interfered with or controlled by another person?’
If yes, Probe G1A. ‘Did it come about in a way that many people would find hard to believe, for instance, through telepathy?’
Screen G2
‘In the past 12 months, have you had a feeling that people were too interested in you?’
If yes, Probe G2A. ‘In the past 12 months, have you had a feeling that things were arranged so as to have a special meaning for you, or even that harm might come to you?’
Screen G3
‘Do you have any special powers that most people lack?’
If yes, Probe G3A. ‘Do you belong to a group of people who also have these powers?’
Screen G4
‘Has a doctor ever told you that you may have schizophrenia?’
APPENDIX 2
Questions assessing lifetime exposure to trauma
Questions concerning possible exposure to traumatic events were derived from the diagnostic section of the Composite International Diagnostic Interview (World Health Organization, 1993):
-
(a) Did you ever have direct combat experience in a war?
-
(b) Were you ever involved in a life-threatening accident?
-
(c) Were you ever involved in a fire, flood or other natural disaster?
-
(d) Did you ever witness someone being badly injured or killed?
-
(e) Were you ever raped, that is someone had sexual intercourse with you when you did not want to, by threatening you, or using some degree of force?
-
(f) Were you ever sexually molested, that is someone touched or felt your genitals when you did not want them to?
-
(g) Were you ever seriously physically attacked or assaulted?
-
(h) Have you ever been threatened with a weapon, held captive or kidnapped or have you ever been tortured or the victim of terrorists?
-
(i) Have you ever experienced any other extremely stressful or upsetting event?
-
(j) Have you ever suffered a great shock because one of the events happened to someone close to you?







eLetters
No eLetters have been published for this article.