The relationship between BMI and all-cause mortality has been extensively explored in several studies. Obesity has generally been shown to be associated with significantly increased all-cause mortality in many previous studies( Reference Flegal, Kit and Orpana 1 ). However, there is still substantial inconsistency regarding the risks of mortality among underweight persons. Indeed, several epidemiological studies have suggested no significant increase in all-cause mortality among individuals in the low BMI category( Reference Chen, Yang and Offer 2 – Reference Arndt, Rothenbacher and Zschenderlein 9 ), while many other studies do( Reference Jee, Sull and Park 10 – Reference Flegal, Kit and Graubard 20 ).
In Asia, where general populations tend to be leaner and being underweight is highly prevalent, understanding the health outcomes associated with being underweight has become particularly important. Nevertheless, large prospective studies have yet to confirm the relationship between underweight and all-cause mortality, especially in a modern context, where mortality from tuberculosis and other infectious diseases is low. Therefore we aimed to investigate the associations between being underweight and mortality in Korean men and women.
Methods
Study population
The Korea Medical Insurance Corporation (KMIC) provides health insurance to civil service workers, teachers and their dependants in Korea. Of the entire Korean population (approximately 43 million in 1990), 4 603 361 (11 %) were insured by KMIC, including 1 213 594 workers and 3 389 767 dependants. All insured workers are required to participate in biennial medical examinations performed by KMIC. In 1990 and 1992, respectively 95 % and 94 % of workers completed the biennial examinations. The KMIC study comprised a 25 % systematic random sample of male workers and all female workers, drawn from insured members ordered by national identification numbers. The study comprised 108 461 men and 64 119 women, aged 35–59 years, who underwent physical examinations twice in 1990 and 1992. Ethical approval was given by the Institutional Review Board of Severance Hospital at Yonsei University.
Measurements
The KMIC biennial examinations were conducted in a standardized fashion by medical staff at local hospitals. In 1990, examinations were conducted at 416 hospitals. A questionnaire was administered to each participant three to four days before physical examination, and completed questionnaires were reviewed and edited by trained staff. Smoking history, alcohol consumption, physical activity and health status were assessed in 1992. Age was documented in 1990. Height, weight, fasting glucose, total cholesterol, systolic blood pressure and diastolic blood pressure were measured in 1990 and 1992, and were averaged for analysis. BMI was calculated as weight in kilograms divided by the square of height in metres (kg/m2). BMI groups were divided according to the WHO recommendations for Asians: underweight, <18·5 kg/m2; normal range, 18·5–22·9 kg/m2; overweight at risk, 23·0–24·9 kg/m2; obese I, 25·0–29·9 kg/m2; and obese II, ≥30·0 kg/m2 ( 21 ). Participants were classified as current smokers if they were smoking, ex-smokers if they smoked at least one cigarette during their whole life but quit, and never smoker if they never smoked even one cigarette.
Mortality follow-up
The follow-up period, which lasted 14 years, was from 1 January 1993 to 31 December 2006. Death certificates from the National Statistical Office were issued according to identification numbers that were assigned to the participants at birth. The causes of death were coded according to the International Classification of Diseases, 10th revision (ICD-10): CVD were categorized by ICD-10 codes I00–I99; cancers were classified by ICD-10 codes C00–C97; and respiratory diseases were coded by ICD-10 codes J00–J99. Other causes of deaths were defined as deaths from other causes than cardiovascular, cancer and respiratory causes.
Statistical analysis
We excluded 8317 men and 4561 women who had known diseases at baseline, and further excluded 2041 men and 329 women who died during 1993–1997 to minimize the impact of reverse causality. We also excluded 3970 men and 10 733 women who had no information on smoking. Finally, we included 94 133 men and 48 496 women for analysis. All statistical analyses were performed separately for men and women. Baseline characteristics of the participants are listed according to BMI categories. Cox’s proportional hazards regression models were used to calculate hazard ratios (HR) and 95 % CI to investigate the association between BMI and all-cause mortality after adjusting for age and alcohol consumption. In order to investigate whether being underweight is associated with all-cause mortality independently from smoking status, we calculated HR and 95 % CI separately for never smokers, ex-smokers and current smokers. The Cox’s regression models were adjusted for age, alcohol consumption and cigarettes smoked per day (only for current smokers). As an exploratory analysis, we also calculated HR and 95 % CI for cause-specific mortality: CVD, cancer, respiratory disease and other causes. All statistical procedures were performed using the statistical software package SAS version 9·2 and all P values less than 0·05 were considered statistically significant.
Results
The general characteristics of the study participants are presented according to BMI category in Table 1. For men, the numbers of individuals in each BMI group (<18·5 kg/m2, 18·5–22·9 kg/m2, 23·0–24·9 kg/m2, 25·0–29·9 kg/m2, ≥30·0 kg/m2) were 974 (1·0 %), 40 254 (42·8 %), 29 369 (31·2 %), 22 946 (24·4 %) and 590 (0·6 %), respectively. For women, the numbers in those groups were 2199 (4·5 %), 29 209 (60·2 %), 11 028 (22·7 %), 5841 (12·0 %) and 219 (0·5 %), respectively. Male participants who were underweight had relatively lower mean values for blood pressure, fasting glucose and total cholesterol; they were also more likely to be current smokers, non-drinkers and physically inactive, compared with those in higher BMI categories. Female participants who were underweight had relatively lower mean age, blood pressure, fasting glucose and total cholesterol; they were also more likely to be non-drinkers and physically inactive, compared with women in higher BMI categories.
Table 1 Baseline characteristics of participants by sex: men (n 94 133) and women (n 48 496) aged 35–59 years in 1990, Korea Medical Insurance Corporation study

SBP, systolic blood pressure; DBP, diastolic blood pressure; FG, fasting glucose; TC, total cholesterol.
In Table 2, analyses adjusted for age and alcohol consumption revealed a significantly higher HR for total mortality in underweight men (HR=1·48; 95 % CI 1·21, 1·82) compared with individuals with normal BMI. Men in the obese II category were also associated with higher all-cause mortality (HR=1·28; 95 % CI 0·96, 1·70) compared with those with normal BMI, although the association was not statistically significant. Underweight (HR=1·20; 95 % CI 0·83, 1·74) and obese II (HR=1·55; 95 % CI 0·73, 3·29) women showed higher mortality than women with normal BMI, although these associations were not statistically significant.
Table 2 Hazard ratios for mortality according to BMI category by sex: men (n 94 133) and women (n 48 496) aged 35–59 years in 1990, follow-up period 1 January 1993 to 31 December 2006, Korea Medical Insurance Corporation study
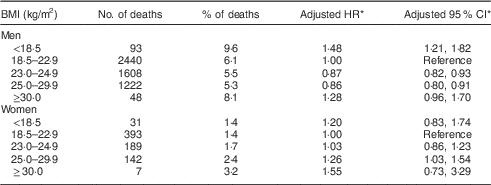
HR, hazard ratio.
* Adjusted for age and alcohol consumption.
In Table 3 we present the HR for all-cause mortality among the BMI groups stratified according to smoking status, with adjustment for age and alcohol consumption. The reference group comprised participants with normal BMI within the same stratum of smoking status. Among male never smokers, being underweight was not associated with all-cause mortality (HR=0·87; 95 % CI 0·41, 1·84); obese I (HR=1·15; 95 % CI 0·96, 1·36) and obese II (HR=1·98; 95 % CI 1·11, 3·53) men showed a higher risk of mortality, with the association for obese I men being nearly significant. Among male ex-smokers, none of the BMI groups showed significantly increased mortality risk. Among male current smokers, being underweight was associated with a significantly higher risk of mortality (HR=1·60; 95 % CI 1·28, 2·01). Among female never smokers, being underweight was not significantly associated with mortality (HR=1·12; 95 % CI 0·76, 1·65); obese I (HR=1·30; 95 % CI 1·07, 1·60) women showed a significantly higher risk of mortality. Among female ex-smokers and current smokers, the number of deaths in each BMI category was too small to properly assess the relationship between BMI and mortality.
Table 3 Hazard ratios for mortality according to BMI category and smoking status by sex: men (n 94 133) and women (n 48 496) aged 35–59 years in 1990, follow-up period 1 January 1993 to 31 December 2006, Korea Medical Insurance Corporation study

HR, hazard ratio.
* Adjusted for age and alcohol consumption.
† Adjusted for age, alcohol consumption and cigarettes per day.
We additionally assessed cause-specific mortalities to investigate causes contributing to the increased mortality risk observed in underweight male participants who smoke cigarettes. Among male current smokers, being underweight was associated with an increased risk of death from cancer, respiratory disease and other causes, but not from CVD, compared with males with normal BMI (data presented in online supplementary material, Supplemental Table 1).
Discussion
In the present large-scale and long-term prospective study of middle-aged Korean men and women, no significant associations between being underweight and all-cause mortality were observed among never smokers.
Previous studies have reported that underweight people with disease or poor health exhibit different patterns of mortality than healthy underweight people. Moreover, underweight individuals with one of several prevalent diseases also show marked increases in mortality, compared with their normal-weight counterparts( Reference Sharma, Vallakati and Einstein 22 – Reference Li, Liu and An 24 ). Thus, the inclusion of participants with underlying disease or poor health may limit analyses( Reference Manson, Willett and Stampfer 8 , Reference Jee, Sull and Park 10 , Reference Zheng, McLerran and Rolland 11 , Reference Zhang, Shu and Chow 25 , Reference Hu, Willett and Li 26 ). Accordingly, we excluded participants with underlying disease and those who died within the first 5 years of follow-up to reduce bias associated with reverse causality.
The physiological characteristics of smokers are not the same as those of the general population. In particular, smokers tend to have lower BMI( Reference Yanbaeva, Dentener and Creutzberg 27 ). Smoking is also one of the major leading risk factors for all-cause mortality worldwide( Reference Lopez, Mathers and Ezzati 28 , Reference Ezzati, Lopez and Rodgers 29 ). Associations between BMI and mortality should therefore be separately analysed according to smoking status. Some prospective studies undertaken in Western and Chinese populations have suggested that mortality is not increased in never smokers of the lowest BMI category( Reference Chen, Yang and Offer 2 – Reference Arndt, Rothenbacher and Zschenderlein 9 ). In contrast, other studies have found an increased risk of mortality in the leanest of participants who did not smoke( Reference Jee, Sull and Park 10 , Reference Song, Pitkaniemi and Gao 12 – Reference Flegal, Kit and Graubard 20 ). There could be several explanations for this difference. First, participants with underlying diseases were not adequately excluded. In fact, some of the studies did not exclude participants with underlying disease( Reference Song, Pitkaniemi and Gao 12 – Reference Hu, Tuomilehto and Silventoinen 19 ). Second, the validity of information on BMI may have been compromised. While repeated measurements can reduce measurement error, few of these previous studies measured height and weight twice. Third, the associations between being underweight and mortality could differ according to the age distribution of participants. Many studies included participants of ages 60 years or more( Reference Jee, Sull and Park 10 , Reference Song, Pitkaniemi and Gao 12 – Reference Flegal, Kit and Graubard 20 ). These older participants may more likely carry co-morbidities, leading to low BMI and introducing bias to the results.
One previous study performed in Korea suggested that male never smokers (HR=1·3; 95 % CI 1·2, 1·4) and ever smokers (HR=1·4; 95 % CI 1·3, 1·4) with low BMI (<18·5 kg/m2) exhibit higher mortality than reference males (BMI=23·0–24·9 kg/m2). Among female never smokers, those with low BMI showed higher mortality (HR=1·2; 95 % CI 1·1, 1·3) than the reference category( Reference Jee, Sull and Park 10 ). We were unable to clearly determine what made our study findings different from those of the previous Korean study. The two studies are, nevertheless, distinct in a few aspects. First, the previous study enrolled insured workers and their family members of a wider age range (35–95 years)( Reference Jee, Sull and Park 10 ), while our study enrolled only insured workers of ages 35 to 59 years. Second, the previous study enrolled participants who had undergone at least one health screening examination between 1992 and 1995, while our study enrolled participants who had undergone two health screening examinations in both 1990 and 1992, allowing us to use the means of two measurements for analysis to reduce measurement errors. Lastly, the reference categories were different: BMI=23·0–24·9 kg/m2 in the previous study and BMI=18·5–22·9 kg/m2 in our analysis.
Concerning current smokers, most previous studies have reported that underweight individuals are at a significantly increased risk of mortality( Reference Chen, Yang and Offer 2 , Reference Arndt, Rothenbacher and Zschenderlein 9 , Reference Jee, Sull and Park 10 , Reference Song, Pitkaniemi and Gao 12 , Reference Sasazuki, Inoue and Tsuji 13 , Reference Klenk, Nagel and Ulmer 16 – Reference Hayashi, Iwasaki and Otani 18 ). This was also reflected in our results. We speculate that being thin may indicate a greater susceptibility to the adverse effects of smoking and particular smoking behaviours, such as deep inhalation.
The strengths of our study include the use of data from a large prospective study in Korea, which is, in general, a lean population. Second, we excluded participants with underlying disease or who died within the first 5 years of follow-up. Third, our study used average BMI, which was measured twice at baseline years (1990 and 1992); thus, our data on BMI might be more reliable and less subject to measurement error. Information on deaths was also accurate, since deaths were confirmed from the National Statistical Office via use of identification numbers assigned to participants at birth.
Our study has several limitations that warrant consideration. First, we performed the study in only middle-aged Korean men and women, which may limit the generalizability of our results to other populations. Nevertheless, our data from a population with a much lower average BMI than most Western populations enabled us to robustly explore associations that may not be prevalent in other cohorts. Second, a considerable number of women were excluded from the analysis, because they did not report their smoking status. If smoking women with poor health status were less likely to report their smoking status than healthy smoking women, selection bias might occur and distort our study findings. Notwithstanding, we did perform sensitivity analyses classifying participants with unknown smoking status into never smokers and the results were very close to our initial results. Third, we did not assess the effect of weight changes after baseline evaluation. If an underweight participant was to gain weight and a normal-weight participant was to lose weight, the difference in BMI between the two groups might become smaller. Thus, we could not completely exclude the possibility of a bias towards the null.
In conclusion, the present study does not support that being underweight per se is associated with higher mortality than being of normal weight.
Acknowledgements
Acknowledgements: The authors thank the National Health Insurance Corporation (formerly the KMIC) for providing the data. Financial support: This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. Conflict of interest: None. Authorship: J.Y.L. designed the study concepts, analysed the data and prepared the manuscript. H.C.K., C.K., S.V.A., K.P. and D.R.K. contributed to data analysis and interpretation. K.-T.K. and W.C.W. contributed to data analysis, data interpretation and revisions of the manuscript. I.S. collected the data, designed the study concepts, interpreted the data and edited the manuscript. All investigators contributed to the final version of the report. Ethics of human subject participation: This study was approved by the Institutional Review Board of the Severance Hospital at Yonsei University.
Supplementary Material
To view supplementary material for this article, please visit http://dx.doi.org/10.1017/S136898001500302X






