Suboptimal environmental conditions during critical periods of development, including inadequate nutrition, may programme physiological mechanisms and contribute to chronic disease risk( Reference Barker, Osmond and Kajantie 1 ). Epidemiological research linking prenatal nutrition to children's health has focused largely on maternal macronutrient intakes such as energy and protein or correlates of nutritional status such as birth size and other indicators of fetal growth assessed retrospectively( Reference Barker 2 ). More recent evidence suggests the importance of specific micronutrients in prenatal programming of long-term health( Reference Monk, Georgieff and Osterholm 3 ). Moreover, various dietary components and inadequacies may mitigate or enhance the impact of chemical environmental exposures during early development as underscored by the National Advisory Environmental Health Sciences Council( 4 ). While epidemiological data are sparse for prenatal studies, dietary intake of antioxidants and methyl nutrients have been shown to reduce air pollution effects in non-pregnant adult samples( Reference Baccarelli, Cassano and Litonjua 5 , Reference Romieu, Castro-Giner and Kunzli 6 ). Interactions have also been observed for other physical (e.g. tobacco smoke) and social (e.g. psychological stress) environmental exposures( Reference Gallo, Renzi and Loizzo 7 , Reference Jiang, Yan and West 8 ). The methyl nutrient choline has recently been associated with alterations in the methylation state of genes influencing development of the fetal hypothalamic–pituitary–adrenal axis( Reference Jiang, Yan and West 8 ), which, in turn, has been linked to birth outcomes( Reference Baibazarova, van de Beek and Cohen-Kettenis 9 ) and respiratory and neurodevelopment during childhood( Reference Wright, Fisher and Chiu 10 ). Thus, understanding the correlates of inadequate dietary intakes may help inform effective intervention and prevention strategies in children's environmental health.
Studies from developing countries document dietary deficiencies in pregnancy as well as effects of micronutrient status on pregnancy outcomes( Reference Tulchinsky 11 ). A recent systematic review and meta-analysis demonstrates that pregnant women in developed countries, including the USA, are also at risk of suboptimal micronutrient intakes( Reference Blumfield, Hure and Macdonald-Wicks 12 ). It is also unlikely that pregnant and childbearing-aged women in developed countries have adequate intake of micronutrients, such as Fe and Ca, through foods alone( Reference Turner, Langkamp-Henken and Littell 13 ). Existing US studies have notable limitations, as most pre-date mandatory folic acid fortification, lack data on emerging essential micronutrients (i.e. choline, betaine) and few consider ethnic minorities. Of the three US studies including both African American and Hispanic women( Reference Lenders, Hediger and Scholl 14 – Reference Swensen, Harnack and Ross 16 ), all examine a narrow range of micronutrients and lack assessments of choline and betaine intake, and only one considered both dietary and supplementation sources( Reference Blumfield, Hure and Macdonald-Wicks 12 ).
Moreover, while studies in non-pregnant samples link a number of sociodemographic characteristics and dietary inadequacies, these associations have not been well studied in pregnant women in the USA. Minority status( Reference Vaccaro and Huffman 17 ), lower education( Reference Aggarwal, Monsivais and Drewnowski 18 , Reference Kant and Graubard 19 ), food insecurity( Reference Kirkpatrick and Tarasuk 20 ) and lower income( Reference Aggarwal, Monsivais and Drewnowski 18 ) have all been linked to poorer nutrition in non-pregnant US adult samples. Other studies suggest nativity (US-born v. foreign-born)( Reference Harley, Eskenazi and Block 21 ) and acculturation status (e.g. years living in the USA)( Reference Perez-Escamilla 22 ) also contribute to dietary behaviours, although such data are even more limited. This is an important area of research because health inequalities may be attributed, in part, to disparities in micronutrient intakes across race/ethnicity and socio-economic status (SES)( Reference Vaccaro and Huffman 17 ).
In order to begin to address some of these gaps, the objectives of the present study were twofold: (i) to comprehensively assess a wide range of dietary micronutrient inadequacies (including choline and betaine) from food and dietary supplements, which post-dates the mandatory folic acid fortification; and (ii) to examine the sociodemographic correlates of micronutrient intakes in an urban US population comprised largely of African American and Hispanic pregnant women. Classes of micronutrients examined in these analyses were selected based on our current understanding of the mechanisms through which nutritional factors in pregnancy may impact fetal growth and development and exert more long-term effects( Reference Langley-Evans 23 ).
Experimental methods
Study population
Participants were from the PRogramming of Intergenerational Stress Mechanisms (PRISM) study, a prospective pregnancy cohort of 276 mother–child pairs originally designed to examine how perinatal stress influences respiratory health in children when controlling for other environmental exposures (chemical stressors, nutrition). Women were recruited from prenatal clinics at 26·9 (sd 8·1) weeks’ gestation from the Beth Israel Deaconess Medical Center and the East Boston Neighborhood Health Center from March 2011 to August 2012. Trained research staff approached women on selected clinic days. Recruitment sites were chosen given desired heterogeneity in sociodemographic and racial/ethnic characteristics. Eligibility criteria included: (i) English- or Spanish-speaking; (ii) age ≥18 years at enrolment; and (iii) singleton pregnancy. All women approached to participate completed a screener questionnaire including data on key variables including maternal age, race/ethnicity, education and nativity status. Procedures were approved by the human studies committee at the Brigham and Women's Hospital; written consent was obtained in the participant's primary language.
Nutrition assessment and processing
Maternal dietary intake was assessed at enrolment by trained interviewers using the modified Block98 (version 98·2; NutritionQuest, Berkeley, CA, USA) FFQ (Block 2006_Bodnar FFQ) consisting of approximately 120 food/beverage items( Reference Block, Hartman and Dresser 24 , Reference Snook Parrott, Bodnar and Simhan 25 ). The measure has been validated in multicultural populations( Reference Snook Parrott, Bodnar and Simhan 25 , Reference Volgyi, Carroll and Hare 26 ). Modifications were made to include a more extensive list of fish and seafood items( Reference Siega-Riz, Bodnar and Savitz 27 ). The FFQ asks about usual food and beverage intakes in the 3 months prior to pregnancy; women were not asked to differentiate their intake before v. during pregnancy. The food list was developed from National Health and Nutrition Examination Survey (NHANES) III dietary recall data; portion size pictures enhanced accuracy of quantification. For each item, women were asked how often (daily, weekly, monthly or rarely/never) and how much (small, medium or large serving sizes) they consumed. The FFQ also queried the type and frequency of dietary supplements, especially vitamins and minerals, used in the prenatal period.
FFQ were processed through the online Block Dietary Data Systems (Berkeley, CA, USA) using the US Department of Agriculture (USDA) Food and Nutrient Database for Dietary Surveys (FNDDS) utilizing software originally developed at the National Cancer Institute( Reference Block, Hartman and Dresser 24 ). Energy, macronutrient and micronutrient intakes were calculated per day by using nutrient values based on data from the third NHANES, the 1994–1996 Continuing Survey of Food Intakes by Individuals (CSFII) and the USDA Nutrient Database for Standard Reference( 28 ). Folate values were derived using the USDA 1998 nutrient database( 28 ). For foods with added folic acid, dietary folate equivalents (DFE) were calculated as: micrograms of naturally occurring food folate + (micrograms of added folic acid × 1·7)( 29 ). Nutrient calculations were provided by NutritionQuest using the USDA Nutrient Database for Standard Reference( 28 ) for the dietary variables and related nutrients of interest. Betaine and choline values were derived from the USDA Database for the Choline Content of Common Foods( 30 ) and the USDA Database for the Choline Content of Common Foods, Release 2( 31 ). Unlisted values were imputed using recipes or applying values from similar foods.
Nutrient intakes were compared with the recommended nutrient intakes of the Institute of Medicine (Estimated Average Requirement (EAR), Adequate Intake (AI), Upper Tolerable Limit (UL)) when available( 32 – 36 ). Pregnancy energy cut-off values recommended by Meltzer et al. ( Reference Meltzer, Brantsaeter and Ydersbond 37 ) and implemented by others( Reference Blumfield, Hure and Macdonald-Wicks 12 ) were used. Women were considered at risk for nutrient inadequacy if their total (food + supplement) nutrient intake was less than the EAR or AI for pregnant women as done previously( Reference Snook Parrott, Bodnar and Simhan 25 ). We calculated the likelihood of Fe inadequacy using the cut-point approach( 34 ).
Maternal characteristics
Information on race, maternal education, height and weight, smoking, nativity status and financial hardships was collected by interview-based questionnaire. Race/ethnicity was self-reported and categorized as Caucasian, Hispanic, African American, or other/mixed. Nativity status was defined as being US-born or foreign-born. Acculturation was considered based on age at immigration, length of time living in the USA and primary language spoken (Spanish, English or bilingual). Maternal education was categorized as high (some college or college degree) or low (high school/high-school diploma or less than high school). Perceived financial difficulties were assessed by the self-reported degree of difficulty (no difficulty v. at least some degree of difficulty) in living on the total household income and meeting monthly payments/bills( Reference Pearlin, Lieberman and Menaghan 38 ); these items were addressed independently in the analyses. Women reported smoking (yes/no) at baseline and in the third trimester; women were classified as smokers if they reported smoking at either visit. Maternal BMI was calculated from height and pre-pregnancy weight reported at enrolment and categorized as normal weight (BMI <25 kg/m2), overweight (BMI ≥25 to <30 kg/m2) or obese (BMI ≥30 kg/m2)( 39 ).
Ethnic identity
Ethnic identity was ascertained using the fourteen-item subscale assessing positive ethnic attitudes and sense of belonging, ethnic identity achievement and ethnic behaviour, from the Multigroup Ethnic Identity Measure (MEIM)( Reference Phinney 40 ). The MEIM has been used in Caucasian, African American and Hispanic populations with good validity and reliability( Reference Nguyen, Subramanian and Sorensen 41 ). Item responses, ranging from 1 (strongly disagree) to 4 (strongly agree), were summed (reverse scoring negatively worded items) and averaged over all items; the median split was used to index high and low ethnic identity scores.
Economic-related food insecurity
Two items assessed economic-related food insecurity: (i) ‘How often do you not have enough money to afford the kind of food you and your family should have?’ (‘never’, ‘once in a while’, ‘often’ and ‘very often’; scores collapsed as never/ever), adapted from an economic strain measure( Reference Pearlin, Lieberman and Menaghan 38 ); and (ii) ‘In the past 6 months, did you go without food because you did not have the money to pay for it?’ (yes/no), from the Crisis in Family Systems-Revised measure( Reference Shalowitz, Berry and Rasinski 42 ). Women responding ‘ever’ and/or ‘yes’, respectively, were considered to be experiencing food insecurity from an economic perspective.
Statistical considerations
Nutrient intakes were energy adjusted using the residual method( Reference Willett, Howe and Kushi 43 ). Because residuals have a mean of zero and include negative values, they do not provide an intuitive sense of intakes. Therefore, the predicted nutrient intake for the mean energy intake of the sample (8354·6 kJ (1996·80 kcal)) was used as a constant. Supplemental intakes were then added to the energy-adjusted nutrients to provide the total energy-adjusted intakes of each micronutrient.
Logistic regression was performed for each micronutrient, with inadequate intake as the outcome. All models were adjusted for maternal age (years), pre-pregnancy BMI and prenatal smoking status( Reference Cuco, Fernandez-Ballart and Sala 44 – Reference Padrao, Silva-Matos and Damasceno 46 ). Micronutrient inadequacies resulting in low cell counts unable to generate reliable odds ratios were assessed by using the median of the micronutrient distribution as a cut-point to index high and low intakes. Due to the small number of bilingual women, analyses including primary language compare English- with Spanish-speaking women only. Results are presented as odds ratios and corresponding 95 % confidence intervals. The χ 2 test was conducted to investigate possible differences in micronutrient intakes (dietary + supplements) above the UL( 29 , 32 – 36 ) by race, ethnic identity, food insecurity and other sociodemographic factors. Analyses assumed a two-sided alternative hypothesis, a 0·05 significance level and were conducted using the SAS statistical software package version 9·2.
Results
Characteristics of respondents
Of 389 eligible women approached, 276 agreed to participate (70·95 %). There were no significant differences based on age, race/ethnicity, education and nativity status when comparing eligible women who participated and those who declined participation. Two women with implausible energy intake (<2092 kJ (<500 kcal) or >20 920 kJ (>5000 kcal)) were excluded from analyses( Reference Meltzer, Brantsaeter and Ydersbond 37 ), resulting in 274 women participating in the study. Table 1 summarizes sample characteristics. Women were predominantly minorities (42·3 % Hispanic, 17·5 % African American, 9·9 % other/mixed). More than half the sample reported a low ethnic identity (54·1 %). Nearly half were foreign-born (47·8 %), with the majority moving to the USA as adults (67·7 %) and residing in the USA for longer than 5 years (78·5 %). Most women identified as English-speaking (63·6 %), almost one-third identified as primarily Spanish-speaking (31·2 %) and the remaining women identified as bilingual (5·2 %). One-third reported a high school education or less. More than half identified difficulty living on total household income (59·6 %) or meeting monthly payments (52·8 %). Food insecurity was reported by over a quarter of women (27·8 %). Additionally, the majority of women were overweight or obese (64·0 %), and 16·8 % smoked during pregnancy. Age at time of immigration and duration in the USA were not associated with micronutrient inadequacies, and thus are not considered further.
Table 1 Participants’ demographic and SES characteristics: pregnant women (n 274), PRISM study, Boston, MA, USA, March 2011–August 2012
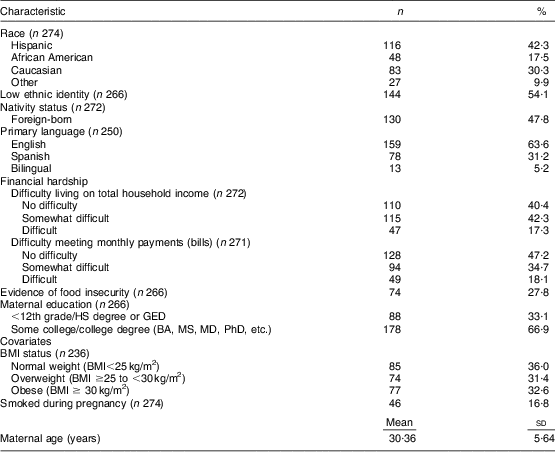
PRISM, PRogramming of Intergenerational Stress Mechanisms; SES, socio-economic status; HS, high school; GED, General Educational Development; BA, Bachelor of Arts; MS, Masters; MD, Doctor of Medicine; PhD, Doctor of Philosophy.
Intake of antioxidants
Vitamin E and Mg were the most common inadequacies identified, with 51·5 % and 38·3 % of women consuming less than the EAR, respectively (Table 2). The prevalence of inadequacies of other antioxidants in descending order was Zn (15·3 %), vitamin A (10·2 %), vitamin C (7·3 %) and Se (1·1 %). When compared with Caucasians, African Americans and Hispanics had greater odds of inadequate intakes across all antioxidants except Mg and Zn (Table 3). Low ethnic identity was associated with inadequate intakes of Mg (OR = 2·19; 95 % CI 1·20, 3·99). Being foreign-born was a significant predictor of vitamin E (OR = 3·73; 95 % CI 2·04, 6·82) and Zn (OR = 2·51; 95 % CI 1·05, 6·00) inadequacies and β-carotene intakes below the median (OR = 2·15; 95 % CI 1·22, 3·80). Spanish-speaking women were also more likely to report suboptimal intakes of β-carotene, vitamin E, Se and Zn compared with those women whose primary language was English (Table 3).
Table 2 Frequencies of micronutrient inadequacies in the study participants: pregnant women (n 274), PRISM study, Boston, MA, USA, March 2011–August 2012

PRISM, PRogramming of Intergenerational Stress Mechanisms.
†Based on dietary intake only.
‡These nutrient intakes were compared with Adequate Intake (AI) levels; all other micronutrients were compared with the Estimated Average Requirement (EAR).
Table 3 Associations between race, ethnic identity and nativity and total (dietary + supplement) micronutrient inadequacy in the study participants: pregnant women (n 274), PRISM study, Boston, MA, USA, March 2011–August 2012
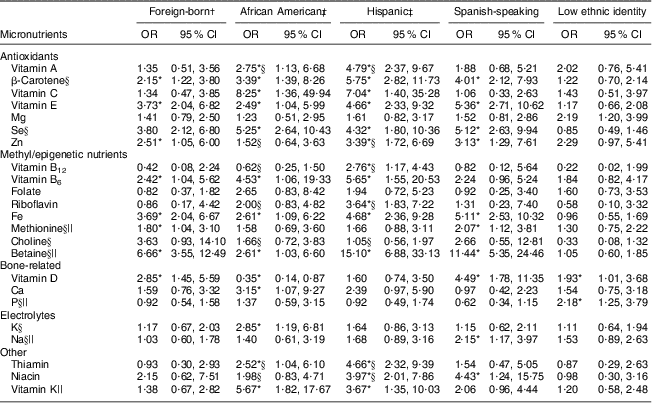
PRISM, PRogramming of Intergenerational Stress Mechanisms.
All analyses were adjusted for maternal age, BMI and smoking during pregnancy.
*Represents significance (P < 0·05).
†Women born in the USA are the reference group.
‡Caucasian women are the reference group. There were no significant findings among the other/mixed race category (data not shown).
§The median cut-point was used to define high and low total intake (vitamin A: 1133·62 μg; β-carotene: 4172·63 μg; Se: 111·36 μg; Zn: 13·58 mg; vitamin B12: 6·79 μg; riboflavin: 2·62 mg; methionine: 1·49 mg; choline: 311·47 mg; betaine: 159·89 mg; P: 1352·36 mg; K: 2·78 g; Na: 3·15 g; thiamin: 1·95 mg; niacin: 26·33 mg).
||Based on dietary intake only.
As shown in Table 4, low maternal education was most consistently associated with antioxidant inadequacies (vitamins A, C and E, β-carotene, Mg, Zn and Se). Food insecurity was significantly associated with antioxidant inadequacies with the exception of β-carotene and Zn. The odds of vitamin E inadequacy was increased more than twofold among those experiencing difficulty living on their total household income or difficulty in meeting monthly payments/bills. While overall 7·3 % of participants had vitamin C inadequacy, it was significantly more prevalent among those experiencing difficulty with living on their total household income (OR = 4·20; 95 % CI 1·14, 15·56) and meeting monthly payments/bills (OR = 4·37; 95 % CI 1·31, 15·50). This was also the case for suboptimal β-carotene intakes. Difficulty meeting monthly payments/bills was also a predictor of lower Se intakes. Women with intakes above the UL for Mg (35 %) were more likely to be Caucasian or Hispanic (χ 2 = 7·96, P = 0·05), more highly educated (χ 2 = 14·77, P < 0·01) and less likely to report food insecurity (χ 2 = 10·19, P < 0·01) or difficulty living on their total household income (χ 2 = 3·86, P = 0·05) or meeting payments/bills (χ 2 = 6·02, P = 0·01). Women with vitamin A (4·7 %), vitamin C (0·36 %), vitamin E (0 %), Se (0 %) and Zn (1·8 %) intakes above the UL were infrequent.
Table 4 Associations between food insecurity and sociodemographic factors and total (dietary + supplement) micronutrient inadequacy in the study participants: pregnant women (n 274), PRISM study, Boston, MA, USA, March 2011–August 2012
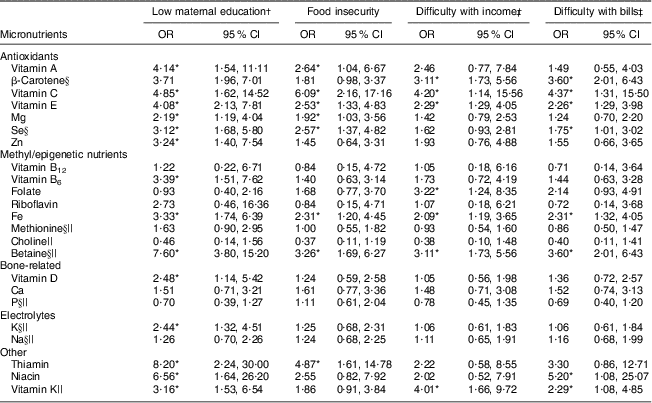
PRISM, PRogramming of Intergenerational Stress Mechanisms.
All analyses were adjusted for maternal age, BMI and smoking during pregnancy.
*Represents significance (P < 0·05).
†Women with some college education or college degree are the reference group.
‡Women with no difficulty are the reference group.
§The median cut-point was used to define high and low intake (β-carotene: 4172·63 μg; Se: 111·36 μg; methionine: 1·49 mg; betaine: 159·89 mg; P: 1352·36 mg; K: 2·78 g; Na: 3·15 g);
||Based on dietary intake only.
Methyl/epigenetic-nutrient intake
The prevalence of Fe intakes below the EAR of 22–23 mg/d was 56·6 % (Table 2). Approximately 15 % of women had folate and vitamin B6 inadequacies below the EAR. Inadequate choline intake was documented in almost all participants, with over 95 % consuming less than the AI level. With respect to sociodemographic predictors of methyl-nutrient intakes, Hispanics had significantly lower intakes of vitamin B12 (OR = 2·76; 95 % CI 1·17, 4·43) and riboflavin (OR = 3·64; 95 % CI 1·83, 7·22) compared with Caucasians; both African Americans and Hispanics had increased odds for inadequacies in vitamin B6 and Fe and suboptimal intakes of betaine compared with Caucasians (Table 3). Foreign-born women had greater odds of suboptimal intakes of vitamin B6, Fe, methionine and betaine compared with those born in the USA. Spanish-speaking women also had greater odds of Fe, methionine and betaine suboptimal intakes compared with English-speaking women. Low ethnic identity was not associated with the intake of methyl/epigenetic nutrients.
Inadequacies in vitamin B6 (OR = 3·39; 95 % CI 1·51, 7·62), Fe (OR = 3·33; 95 % CI 1·74, 6·39) and betaine (OR = 7·60; 95 % CI 3·80, 15·20) were significantly associated with lower education (Table 4). Fe inadequacy and low intake of betaine were significantly more common among women experiencing food insecurity or difficulty living on total household income or meeting monthly bills. Folate inadequacy was also significantly associated with difficulty living on the family's total income (OR = 3·22; 95 % CI 1·24, 8·35).
Women having intakes above the UL for folate (n 102) were more likely to be Caucasian or Hispanic (χ 2 = 38·65, P<0·01), US-born (χ 2 = 7·27, P = 0·01), have a higher education (χ 2 = 24·45, P<0·01), and no report of food insecurity (χ 2 = 4·88, P = 0·03) or difficulty living on their total family income (χ 2 = 10·59, P<0·01) or meeting payments/bills (χ 2 = 10·36, P<0·01). Women with vitamin B6 (0 %) and Fe (5·8 %) intakes above the UL were infrequent.
Intake of bone-related micronutrients
More than 75 % of women had inadequate intakes of vitamin D (Table 2). Ca inadequacies were also prevalent (19·3 %). Only three women had P intake levels below the EAR. Being African American had a protective effect on vitamin D inadequacy (OR = 0·35; 95 % CI 0·14, 0·87) and a negative effect on Ca inadequacy (OR = 3·15; 95 % CI 1·07, 9·27) compared with being Caucasian. Foreign-born (OR = 2·85; 95 % CI 1·45, 5·59) and Spanish-speaking women (OR = 4·49; 95 % CI 1·78, 11·35) as well as those reporting low ethnic identity (OR = 1·93; 95 % CI 1·01, 3·68) had higher odds of vitamin D inadequacies (Table 3). Women with a low education level also had higher odds of vitamin D inadequacy (Table 4). Bone-related micronutrient intakes higher than the UL were not prevalent in this cohort (vitamin D (0 %), Ca (0·73 %), P (0 %)).
Intake status of electrolytes
With the exception of one participant, all women had K intakes below the AI level of 4·7 g/d (mean intake of 2·80 g/d). Thus, associations with race/ethnicity and SES factors were examined using the median to define high and low intakes. African American race (OR = 2·85; 95 % CI 1·19, 6·81) and low educational status (OR = 2·44; 95 % CI 1·32, 4·51) were the only correlates of low K intakes (Tables 3 and 4, respectively). Conversely, the amount of Na consumed by this cohort was much higher than the AI level of 1·5 g/d (mean intake of 3·19 g/d) with 98·9 % consuming more than the AI and 98·2 % having Na intakes above the UL of 2·3 g/d. Spanish-speaking women consumed less Na than those women whose primary language was English (OR = 2·15; 95 % CI 1·17, 3·97).
Intake of other nutrients
The frequency of thiamin (6·9 %) and niacin (5·8 %) inadequacies was relatively low and did not vary by nativity or ethnic identity (Table 3). However, African Americans and Hispanics and low maternal education were significantly associated with lower intakes of thiamin and niacin (Tables 3 and 4, respectively). Thiamin and niacin inadequacies were also associated with food insecurity (OR = 4·87; 95 % CI 1·61, 14·78) and speaking Spanish (OR = 4·43; 95 % CI 1·24, 15·75), respectively.
Vitamin K intakes below the AI level were prevalent in over 20 % of the study population (Table 2). Hispanics (OR = 3·67; 95 % CI 1·35, 10·03) and African Americans (OR = 5·67; 95 % CI 1·82, 17·67) were more likely to have lower vitamin K intake than Caucasians. Low vitamin K intake was significantly more common among women with a lower level of education or more difficulty living on their total family income or meeting monthly payments/bills (Table 4).
Discussion
These analyses, considering both dietary and supplemental intakes, identify a range of micronutrient intake inadequacies in a multi-ethnic, primarily urban US population of pregnant women that may have implications for perinatal and more long-term child health. These analyses expand prior research involving pregnant US samples that pre-dated changes in folic acid awareness and its widespread fortification or more narrowly considered multivitamin use. We also identified vulnerable groups of women with distinct differences in dietary micronutrient composition related to sociodemographic factors that may inform tailored intervention strategies going forward.
Of the antioxidant inadequacies identified, vitamin E and Mg were most striking. Notably, the EAR for vitamin E is the same (12 mg/d) in pregnant and non-pregnant women; Mg requirements increase slightly during pregnancy (255 mg/d preconception to 290 mg/d in pregnancy). Although Mg intake exceeded the UL in some women, the prevalence of intake below the EAR was over 30 %. Hispanics and African Americans were more likely to report antioxidant inadequacies compared with Caucasians, with the exception of Mg. African Americans were most likely to have inadequate vitamin E intake. As other studies suggest that African Americans are less likely to select from food groups rich in α-tocopherol and Mg, such as nuts, seeds, whole grains, green leafy vegetables and vegetable oils( Reference Kant, Graubard and Kumanyika 47 ), this may represent a unique target for dietary intervention among this group. A recent pilot study demonstrated the feasibility and acceptability of a food-exchange-based intervention to optimize prenatal dietary vitamin E intake( Reference Clark, Craig and McNeill 48 ). Such studies should be expanded to include ethnic minority, urban populations.
Nearly all women reported choline intakes lower than the recommended AI. This is concerning since choline plays an important role in placental function and fetal development (birth defects, brain development), possibly by influencing DNA methylation status( Reference Jiang, Yan and West 8 , Reference Boeke, Baccarelli and Kleinman 49 ). As prenatal vitamins do not contain an adequate source of choline, some have proposed that women with low intakes of milk, meat, eggs or other choline-rich foods should consider a prenatal dietary supplement containing this micronutrient. Similar to findings in a number of developed countries (e.g. Japan, Australia, Europe, UK)( Reference Blumfield, Hure and Macdonald-Wicks 12 ), Fe inadequacy, which may also influence epigenetic modifications( Reference Cyr and Domann 50 – Reference Zhang, Zhang and Clark 52 ), was common in these women. Pregnant women are particularly vulnerable to Fe deficiency given that the EAR for Fe increases by approximately 15 mg/d in pregnancy( 34 ). However, even after considering supplementation in our sample, 57 % of women had inadequate Fe intakes and reported insufficient intakes of relevant food sources, which include red meats, fish, poultry, beans, lentils and fortified foods( 53 ). African American, Hispanic and foreign-born women consumed less Fe and other methyl nutrients, including vitamin B6 and betaine, compared with Caucasians and US-born women, respectively. While disparities in Fe intake among pregnant African Americans and Hispanics have been reported( Reference Mei, Cogswell and Looker 54 ), nativity status has been less well studied. One study found that pregnant Hispanic immigrants consumed more folate, vitamin C, Fe and Zn than US-born Hispanics( Reference Schaffer, Velie and Shaw 55 ). Longer duration of US residence has been attributed to lower energy intake( Reference Harley, Eskenazi and Block 21 ). Our study showed decreases in antioxidant and methyl-nutrient intakes among Hispanics and foreign-born women. Dissimilarities in micronutrient intakes by race and nativity could partly be explained by differences in the use of supplements, as previously shown with Fe( Reference Cogswell, Parvanta and Ickes 56 ). The complex relationships among race, nativity status and prenatal micronutrient intakes warrant further investigation.
Inadequate vitamin D intake was present in over 75 % of these women from the north-eastern USA, where vitamin D status is also likely influenced by season given the importance of sun exposure and consequent conversion to 25-hydroxyvitamin D( Reference Wuertz, Gilbert and Baier 57 ). Even moderately decreased levels of 25-hydroxyvitamin D have been associated with poor fetal and infant skeletal growth and tooth mineralization( Reference Marshall, Mehta and Petrova 58 ). Therefore, inadequate dietary intake of vitamin D may be more relevant in populations, such as this cohort, affected by seasonal climates where sun exposure, as a source of vitamin D, is limited. In our study, foreign-born women and those with low ethnic identity were most likely to have bone-related micronutrient inadequacies. Immigrant groups perceiving that their American identity is being challenged( Reference Cheryan and Monin 59 ) may abandon their ethnic identity and conform to an American identity, in part, by embracing poor dietary behaviours( Reference Guendelman, Cheryan and Monin 60 ). Thus, ethnic identity may be another important factor to consider when identifying vulnerable populations at risk for suboptimal nutrient status.
Low maternal education consistently predicted inadequate antioxidant and suboptimal or inadequate methyl-nutrient intakes. Data from non-pregnant US samples similarly report that education is an important predictor of diet quality( Reference Kant and Graubard 19 ). When micronutrient intakes, including vitamins A, C, D, E and B12, β-carotene, folate, Fe, Ca and Mg, were examined in relation to diet cost and SES (indexed by education and income), researchers found that lower-cost/quality diets were also consumed more frequently by lower-SES groups in the USA( Reference Aggarwal, Monsivais and Drewnowski 18 ). Taken together, these findings suggest that both maternal education and SES play a role in dietary intake.
Food insecurity was also significantly associated with antioxidant inadequacies (except Zn and β-carotene) and the methyl nutrients Fe and betaine. Food insecurity, characterized by limited and/or uncertain availability or access to nutritionally adequate foods( Reference Kendall and Kennedy 61 ), affected nearly 30 % of this population. Some have proposed that food insecurity could impact fetal development through physiological and psychological changes due to micronutrient deficiencies or the stress experienced as a result of limited access to nutritionally adequate food, respectively( Reference Ramsey, Giskes and Turrell 62 ). US and Canadian studies suggest that individuals experiencing food insecurity have lower intakes of fruits and vegetables( Reference Kirkpatrick and Tarasuk 20 , Reference Kaiser, Melgar-Quinonez and Townsend 63 , Reference Tingay, Tan and Tan 64 ), in part due to the perception that nutrient-dense food groups are expensive( Reference Tanumihardjo, Anderson and Kaufer-Horwitz 65 ). Our findings highlight the need for an enhanced elucidation of the impact of food insecurity on micronutrient intakes in multi-ethnic US pregnant women.
It is well established that not only nutrient deficiencies but also excesses can have adverse effects on perinatal outcomes and fetal development( Reference Mao, Liu and Li 66 ). As the majority of pregnant women in the USA take a dietary supplement, most frequently a multivitamin/mineral product, they may be more likely to exceed the UL. When considering food intakes combined with supplements, more than 35 % of the women in the present study reported Mg, folate and niacin intakes higher than the UL. In addition, nearly the entire study population (98 %) had Na intakes above the UL. Women reporting excessive intakes of Mg, folate and niacin were more likely to be Caucasian or Hispanic, of higher SES, US-born and not reporting food insecurity. These findings highlight the importance of including supplement use when examining dietary intakes during pregnancy and identifying excessive intakes as well as inadequacies.
Interpretation of our findings should be considered in light of our study's limitations. Food and supplemental intakes were based on participant recall and therefore subjected to under- or overestimation. For example, the multiple food items and choices in an FFQ may result in overestimation for some nutrients, and the retrospective nature of the questionnaire may influence recall. However, FFQ are useful for obtaining estimates of usual intake over time (e.g. months), including during pregnancy( Reference Blumfield, Hure and Macdonald-Wicks 12 ). Misclassification of nutrient intake is likely random and therefore would be expected to result in an underestimation of associations. Nevertheless, future research would be enhanced through the incorporation of food records and 24 h dietary recalls. Second, the median was used as the cut-point to define high and low micronutrient intakes when an EAR or AI was not available. This may not represent a true inadequacy. Thus, the results are best viewed as estimates rather than absolute levels of intake because FFQ may contain measurement error. We acknowledge that the assessment of food insecurity was not comprehensive. Nevertheless, our findings concerning economically related food insecurity are interesting and warrant further investigation. The approximately 70 % rate of participation at enrolment may reduce generalizability; however, women who were eligible and agreed to participate did not differ on key covariates when compared with those who declined.
Conclusions
The present study provides a thorough examination of the influence of race/ethnicity, SES and other sociodemographic factors, including nativity status and ethnic identity, on micronutrient intakes in a sociodemographically diverse sample of pregnant women in the USA. These data highlight the high prevalence of inadequate intakes of specific micronutrients (e.g. antioxidants, methyl nutrients, electrolytes, bone-related micronutrients) that have been implicated in the prenatal programming of developmental diseases, including allergies and asthma( Reference Erkkola, Nwaru and Kaila 67 ), obesity( Reference Yang and Huffman 68 ) and neurodevelopment( Reference Monk, Georgieff and Osterholm 3 ). Moreover, in utero micronutrient inadequacies may enhance fetal vulnerability to other environmental exposures (e.g. air pollution, stress)( Reference Monk, Georgieff and Osterholm 3 , Reference Kannan, Misra and Dvonch 69 ). Prenatal nutritional interventions may be enhanced in urban ethnic-minority populations if tailored to account for the specific sociodemographic determinants of prenatal dietary patterns.
Acknowledgements
Sources of funding: This work was supported by the National Institute of Environmental Health Sciences (NIEHS; grant number R21ES021318-01). NIEHS had no role in the design, analysis or writing of this article. Conflicts of interest: The authors report no conflict of interest. Authors’ contributions: R.J.W. and S.K. are co-senior authors. K.J.B. drafted the manuscript, contributed to the concept and design of the analyses, and led the analyses, interpretation of data and writing of the manuscript; R.O.W. contributed significantly to analyses and interpretation of data and provided critical review and revisions of the manuscript; K.D. contributed to the interpretation of data analyses and provided critical review and revisions of the manuscript; M.B.E. contributed to the interpretation of data analyses and provided critical review and revisions of the manuscript; H.F. contributed to the interpretation of data analyses and provided critical review and revisions of the manuscript; R.J.W. contributed to conception and design of the cohort, data acquisition, analyses and interpretation of data, and provided critical review and revisions of the manuscript; S.K. contributed to dietary data acquisition, analyses and interpretation of data, and provided critical review and revisions of the manuscript.






