Childhood obesity is an important public health concern across the world, with rates increasing dramatically over recent decades in many developed countries( Reference Lien, Henriksen and Nymoen 1 – Reference Ventura and Birch 4 ). A recent review has shown that in some European countries, these increasing trends have stabilized( Reference Lien, Henriksen and Nymoen 1 , Reference Sleddens, Kremers and Stafleu 3 , Reference Ventura and Birch 4 ). Childhood obesity can lead to insulin resistance and type 2 diabetes, hypertension and CVD later in life( Reference Singh, Mulder and Twisk 5 , Reference Roberts, Shields and de Groh 6 ).
Poor diet is widely acknowledged to be a key driver of childhood obesity. The most recent Canadian Community Health Survey reported that over 60 % of children aged 9–13 were not consuming current Canadian recommendations for servings of vegetables and fruit( Reference Shields and Rozin 7 ). Low daily consumption of vegetables and fruit is also common among children in other developed countries( Reference Ohly, Pealing and Hayter 8 , Reference Berge, Wall and Larson 9 ). Higher consumption of nutritious, lower-energy foods, such as vegetables and fruit, is assumed to displace highly energy-dense, non-nutritious foods in children, assisting in weight management, although there is little empirical evidence to confirm this( Reference Bayer, Nehring and Bolte 10 ). In adolescence, a period of rapid development, the consumption of vegetables and fruits is considered to be important( Reference Neumark-Sztainer, Wall and Perry 11 ). Vegetable and fruit consumption in adulthood has been shown to be protective against CVD, cancer and stroke( Reference Wright, Norris and Newman Giger 2 , Reference Neumark-Sztainer, Wall and Perry 11 ). Because dietary habits learned in childhood and adolescence often persist into adulthood, healthy eating patterns established in childhood may lead to continued healthy behaviour in adulthood and prevention of lifetime disease( Reference Roberts, Shields and de Groh 6 , Reference Ohly, Pealing and Hayter 8 , Reference Neumark-Sztainer, Wall and Perry 11 ).
There is an extensive literature base providing strong evidence that parents play an important role in shaping their children’s health behaviours and outcomes( Reference Ventura and Birch 4 , Reference Sleddens, SMPL and Thijs 12 – Reference McClain, Chappuis and Nguyen-Rodriguez 16 ). As such, parents are the focus of many public health strategies aiming to improve children’s diet and reduce the prevalence of childhood obesity( Reference Wright, Norris and Newman Giger 2 , Reference Andrews, Silk and Eneli 17 – Reference Neumark-Sztainer 20 ). Recent systematic reviews have shown that parenting style, rules, home environment and parental role modelling are associated with their children’s diet and body weight( Reference Ventura and Birch 4 , Reference Sleddens, SMPL and Thijs 12 , Reference Webber and Loescher 15 , Reference McClain, Chappuis and Nguyen-Rodriguez 16 ). Similar findings have been found for other children’s health behaviours such as television viewing and physical activity( Reference Andrews, Silk and Eneli 17 , Reference Vander Ploeg, Wu and McGavock 18 , Reference Fung, Kuhle and Lu 21 ). The dietary literature about parental practices and children’s outcomes predominantly focuses on specific dietary outcomes such as breakfast consumption, energy intake, soft drink consumption, and vegetable and fruit consumption( Reference Neumark-Sztainer, Wall and Perry 11 – Reference Van Lippevelde, Velde Te and Verloigne 14 ). Although these specific dietary behaviours can act as a proxy for overall adequacy of the diet, studies linking parental practices to complete dietary patterns are limited. The use of a diet quality index allows an assessment of the whole diet pattern rather than specific foods or nutrients, allowing the evaluation of how overall diet patterns align with recommendations( Reference Marshall, Burrows and Collins 22 , Reference Smithers, Golley and Brazionis 23 ). In children, higher scores on diet quality indices have been shown to be associated with better lean mass, improved school performance and reduced feelings of sadness and worry, although studies using diet quality indices in children are few( Reference Smithers, Golley and Brazionis 23 – Reference McMartin, Willows and Colman 25 ). In adults, diet quality indices have been used to determine chronic disease risk and risk of mortality from chronic disease( Reference Marshall, Burrows and Collins 22 ). Although there is much literature to demonstrate that parents exert a key influence on children’s specific nutrition behaviours, studies linking parental encouragement and caring about healthy eating and its influence on children’s diet quality are limited. As diet quality indices provide a more comprehensive overview of dietary patterns that better predict disease risk than individual nutrients, foods or habits, and studies using diet quality indices in children are limited, investigating determinants of overall diet quality for children can make an important contribution to the children’s health literature( Reference Marshall, Burrows and Collins 22 , Reference Smithers, Golley and Brazionis 23 , Reference Kim, Haines and Siega-Riz 26 ).
To inform and improve the effectiveness of policies and programmes for the improvement of children’s diets and prevention of childhood obesity and chronic disease, we investigated the association between parental encouragement and caring about healthy eating and their child’s diet quality and body weight status using a large, population-based sample of parents and children in Alberta, Canada.
Methods
Study design
The present research is an analysis of secondary data acquired from the Raising healthy Eating and Active Living (REAL) Kids Alberta Evaluation, a population-based survey of grade 5 children (aged 10–11 years) and their parents or guardians throughout the province of Alberta, Canada. The evaluation serves to assess the impact of programmes and policies for the prevention of childhood obesity administered by Alberta Health. The survey occurred in three waves in 2008, 2010 and 2012 using a one-stage stratified random sampling design( Reference Fung, Kuhle and Lu 21 ). All Albertan schools were included in the sampling frame with the exception of private, francophone, on-reserve federal, charter and colony schools( Reference Fung, Kuhle and Lu 21 ). This accounted for 90·2 % of eligible students in the province. Schools were stratified into three geographical areas – metropolitan, urban and rural – and schools were randomly selected within these strata to achieve a balance of students from each group( Reference Fung, Kuhle and Lu 21 ). Upon selection, the school principal was given the opportunity to agree or decline to his/her school’s participation. If the principal declined, another school within the stratum was randomly selected as a replacement until the target of approximately 150 schools in each year was reached. All three waves had the same protocol and reached a new group of parents and their grade 5 children. The evaluation consisted of three questionnaires: one directed at parents or guardians (home survey) and two directed at children (student survey and FFQ). Informed consent was provided by parents at the time of the home survey. Students provided assent before the completion of their surveys. Trained evaluation assistants administered the student survey and FFQ, as well as collected height and weight measurements, during classroom time at the participating schools. Additional information about the REAL Kids Alberta Evaluation can be accessed at the website (http://www.realkidsalberta.ca). All procedures involving human subjects were approved by the University of Alberta’s Health Research Ethics Board. Ethical approval was also obtained for the current secondary data analysis from the University of Alberta’s Health Research Ethics Board.
Assessment of exposure
The home survey directed at parents or guardians of students included two questions related to beliefs and support for healthy eating: (i) ‘How much do you personally care about eating healthy foods?’ and (ii) ‘To what extent do you encourage your child to eat healthy foods?’ Responses for each question corresponded to an ordinal scale from 1 to 4, where a response of 1=‘not at all’, 2=‘a little bit’, 3=‘quite a lot’ and 4=‘very much’. Few parents responded ‘not at all’ or ‘a little bit’ to either question (Table 1) and therefore these responses were combined into one category for the purposes of analysis. Surveys are available online (http://www.realkidsalberta.ca).
Table 1 Characteristics of grade 5 students and their parent(s) or guardian(s) participating in the REAL Kids Alberta Evaluation in Alberta, Canada in 2008, 2010 and 2012 (n 8388)
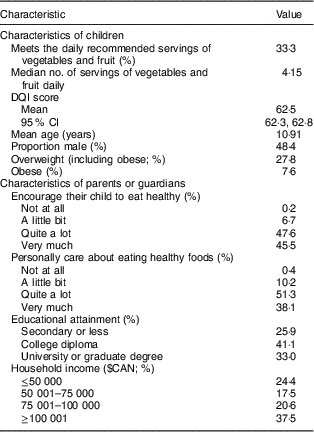
DQI, Diet Quality Index-International.
Assessment of outcome measures
Diet quality
Diet quality was assessed using the Diet Quality Index–International (DQI) score calculated based on student responses to the Harvard Youth/Adolescent FFQ. The DQI is a composite measure of diet that ranges from 0 to 100, with higher scores indicating better diet quality. It measures diet quality over four categories: adequacy, variety, moderation and overall balance( Reference Kim, Haines and Siega-Riz 26 ). A DQI score is based on a combination of consumption of whole foods and nutrients that can be derived from responses to the FFQ.
Meeting recommendations for vegetables and fruit
Each participant’s vegetable and fruit intake was calculated as number of servings from the ‘Vegetables and Fruit’ category outlined by Eating Well with Canada’s Food Guide ( 27 ) as also measured using the FFQ. A binary variable was generated for each participant to indicate if he/she met or did not meet the recommendation of six servings of vegetables and fruit daily( 27 ).
Weight status
Height was measured to the nearest 0·1 cm using a stadiometer (Seca-Stadiometers, Germany) and body weight to the nearest 0·1 kg using calibrated digital scales (Health-o-meter, USA). Children were asked to remove their shoes for both measurements. BMI was calculated as kg/m2 and overweight was defined using the BMI cut-off point for children and youth established by the International Obesity Task Force( Reference Cole, Bellizzi and Flegal 28 ). This cut-off point is based on the adult health-related definition of overweight (BMI≥25 kg/m2), but is adjusted for specific age and sex categories for children.
Confounding variables
Analyses were adjusted for child’s gender, school region, year of evaluation, parental education attained and household income. Tables show results for unadjusted, partially adjusted and fully adjusted models. Analyses were also adjusted for energy intake for improved validity as per recommendations for the analyses of FFQ data( Reference Willett 29 ). Energy intake was also derived from the FFQ.
Analysis
Sample characteristics
A total of 15 875 parents and students were invited to participate; 9784 parents completed and returned their home survey as well as provided consent for their child to participate, resulting in a 62 % consent rate. Following receipt of their parents’ consent, 9210 children participated in the evaluation resulting in a 58 % completion rate. Students or parents who had incomplete or missing responses for any of the variables of interest were excluded from the analysis, as were students reporting energy intakes lower than 2092 kJ (500 kcal) or higher than 20 920 kJ (5000 kcal), leaving 8388 parents and students to be included in the current analysis.
Statistical analysis
Random-effects models were applied due to the clustering of students within schools. Univariable linear and logistic regression models were first used to quantify associations between parental encouragement and caring variables and the outcomes of diet quality, meeting vegetable and fruit requirements and overweight. The response of ‘quite a lot’ was used as a reference category. Next, we applied multivariable linear and logistic regression models to adjust for potential confounders including child gender, energy intake, school region, year of evaluation, parental education and household income (model 1). Finally, we considered all exposures simultaneously to determine their independent associations with the outcomes of interest (model 2).
To determine if parental encouragement and personal caring about healthy eating had a synergistic effect on the outcomes of interest, an interaction model was built. Parents who responded ‘very much’ to both questions or ‘not at all/a little bit’ to both questions were compared with parents who responded ‘quite a lot’ to both questions.
All analyses were completed using the statistical software package Stata SE version 13.
Results
Descriptive statistics for children and parents are presented in Table 1. Because of infrequency of the response of ‘not at all’, these responses were combined with response of ‘a little bit’ for the purposes of subsequent analysis.
Parental encouragement and personal caring about healthy eating were both associated with diet quality. Children whose parents encouraged them ‘very much’ to eat healthy foods compared with those whose parents encouraged them ‘quite a lot’ scored 1·44 (95 % CI 0·96, 1·91) DQI units higher, adjusting for relevant confounders (model 1, Table 2). This association remained statistically significant when parental caring about healthy foods was included in the model (model 2, Table 2). Children whose parents encouraged their child ‘not at all’ or ‘a little bit’ to eat healthy foods scored 1·52 (95 % CI −2·37, −0·67) DQI units lower compared with those whose parents encouraged them ‘quite a lot’ (model 1, Table 2). These associations were very similar for responses about parental caring about healthy eating (Table 2). Children whose parents personally cared ‘very much’ about healthy eating scored 1·66 (95 % CI 1·09, 2·22) DQI units higher than those whose parents cared ‘quite a lot’, while those who cared ‘not at all’ or ‘a little bit’ scored 1·44 (95 % CI −2·26, −0·63) DQI units less (Table 2). These associations remained significant when including parental encouragement in the model.
Table 2 Association of parental encouragement and personal caring about healthy eating with their grade-5 child’s diet quality and likelihood of meeting vegetable and fruit recommendations; REAL Kids Alberta Evaluation in Alberta, Canada in 2008, 2010 and 2012 (n 8388)
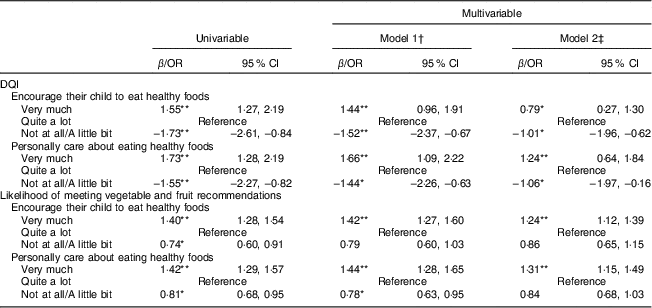
DQI, Diet Quality Index-International.
*P<0·05, **P≤0·01.
† Model 1 adjusted for child gender, energy intake, parental education, household income, school region and year of participation.
‡ Model 2 adjusted for child gender, energy intake, parental education, household income, school region, year of participation, parental encouragement of healthy eating and parent personally caring about healthy eating.
Increased parental encouragement and caring about healthy eating were associated with increased likelihood of their child meeting recommendations for vegetables and fruit (Table 2). Children whose parents encouraged them ‘very much’ to eat healthy foods were 1·42 (95 % CI 1·27, 1·60) times more likely to meet vegetable and fruit recommendations than those whose parents encouraged them ‘quite a lot’, when considering relevant confounders (Table 2). Children whose parents cared about healthy eating ‘very much’ compared with those who cared ‘quite a lot’ were 1·44 (95 % CI 1·28, 1·65) times more likely to meet vegetable and fruit recommendations than those who cared ‘quite a lot’. The association between parents who encouraged and cared about healthy eating ‘not at all’ or ‘a little bit’ and likelihood of meeting vegetable and fruit recommendations was weak, but the trend did show a gradient that less encouragement and caring led to lower likelihood of meeting recommendations (Table 2).
Children whose parents encouraged them ‘very much’ to eat healthy foods were 0·83 (95 % CI 0·71, 0·96) times more likely to be overweight (model 1, Table 3). When parental caring about healthy eating was included in the model, this association remained significant (model 2, Table 3). No statistically significant association was observed between parental caring about healthy eating and child likelihood of overweight when relevant confounders were considered.
Table 3 Association of parental encouragement and personal caring about healthy eating with their grade-5 child’s likelihood of overweight (including obese); REAL Kids Alberta Evaluation in Alberta, Canada in 2008, 2010 and 2012 (n 8388)

*P<0·05, **P≤0·01.
† Model 1 adjusted for child gender, parental education, household income, school region and year of participation.
‡ Model 2 adjusted for child gender, parental education, household income, school region, year of participation, parental encouragement of healthy eating and parent personally caring about healthy eating.
Further analysis revealed a clear synergistic and statistically significant interaction between parental encouragement for healthy eating and parental caring about healthy eating for children’s dietary outcomes. Compared with children whose parents responded ‘quite a lot’ for both questions, children whose parents who responded ‘very much’ to both questions scored an average of 2·06 (95 % CI 1·45, 2·66) DQI units higher. Comparatively, those whose parents responded ‘not at all’ or ‘a little bit’ to both questions scored an average of 1·77 (95 % CI −2·93, −0·61) fewer DQI units. Children whose parents responded ‘very much’ to both questions compared with the reference of ‘quite a lot’ for both had 1·65 (95 % CI 1·41, 1·93) times the odds of meeting vegetable and fruit requirements. There was a decreased, although not statistically significant, likelihood of child overweight for responses of ‘very much’ for both questions (OR=0·85; 95 % CI 0·72, 1·01).
Discussion
In the present study we assessed the association of parental encouragement and caring about healthy eating with children’s diet and body weight status. Using a large, population-based sample of Canadian children, we showed that increased parental encouragement and caring were both independently associated with increases in diet quality and likelihood of meeting recommendations for vegetable and fruit consumption. The existing literature has revealed positive impacts of parental involvement on children’s consumption of vegetables and fruit( Reference Ohly, Pealing and Hayter 8 ). However, to our knowledge, the present study is the first to reveal a correlation of parent caring and encouragement with healthy eating and diet quality of children. We also found that increased parental encouragement for their child to eat healthy foods was associated with a decreased likelihood of child overweight. Moreover, we showed that parental encouragement and caring about healthy eating work synergistically on the diet quality of children.
The majority of parents in this Canadian sample reported encouraging and personally caring about healthy eating at least ‘quite a lot’. This is similar to a Dutch study in which parents completed eight questions related to encouragement of their child’s eating habits (e.g. ‘I encourage my child to enjoy his/her food’)( Reference Sleddens, Kremers and Stafleu 3 , Reference McClain, Pentz and Nguyen-Rodriguez 30 ). On a 5-point Likert scale, the mean score for encouragement of positive eating behaviours was 3·88, indicating that the parents in this sample encouraged their children to exhibit positive eating habits often( Reference Sleddens, Kremers and Stafleu 3 , Reference Devine, Jastran and Jabs 31 – Reference Daniels, Jacobson and McCrindle 33 ). Ohly et al. measured parental caring about food and eating in British parents using a Food Involvement Score and found a mean score of 47 out of a possible 60 in their sample, again similar to the high level of caring observed in our sample( Reference Ohly, Pealing and Hayter 8 , Reference Neumark-Sztainer, Wall and Perry 11 ). Parents in the 2008 and 2010 REAL Kids Alberta Evaluation sample reported higher encouragement and personal caring about healthy eating than about physical activity, with 23·1 % of parents reporting that they personally cared about physical activity ‘not at all’ or ‘a little bit’( Reference Sleddens, Kremers and Stafleu 3 , Reference Ventura and Birch 4 , Reference Vander Ploeg, Maximova and Kuhle 34 ). This may indicate that parents may be more open to health promotion programmes that target improvement in eating behaviours compared with programmes that target other health behaviours. Alternatively, parents may be more aware of the relationship between diet and health than they are about physical activity.
The present study’s findings are consistent with existing research indicating that parental encouragement and caring about healthy eating are associated with improved dietary outcomes for children( Reference Ohly, Pealing and Hayter 8 , Reference Neumark-Sztainer, Wall and Perry 11 , Reference Verloigne, Van Lippevelde and Maes 13 , Reference Van Lippevelde, Velde Te and Verloigne 14 , Reference Wrotniak, Epstein and Paluch 35 ). In a longitudinal study following Dutch parents and their children from age 6 to 8 years, parental encouragement about eating was found to be positively related to fruit intake( Reference Wright, Norris and Newman Giger 2 ). Data collected from parents and children ranging from 18 months to 5 years of age in the UK also demonstrated a link between parental food involvement and vegetable and fruit intake in their children( Reference Ohly, Pealing and Hayter 8 ). The same study demonstrated that increased parental involvement, or personal caring, about food improved their own diet( Reference Ohly, Pealing and Hayter 8 , Reference Lindsay, Sussner and Kim 19 ). Improvements in parental diet resulted in improved parental behaviour modelling, which reviews have found to be an important predictor of vegetable and fruit intake in children and adolescents( Reference Webber and Loescher 15 , Reference Lindsay, Sussner and Kim 19 , Reference McClain, Pentz and Nguyen-Rodriguez 30 ). Additionally, parents have frequently cited in qualitative studies that a healthy child is the primary motivator for household food practices( Reference Andrews, Silk and Eneli 17 , Reference Devine, Jastran and Jabs 31 – Reference Daniels, Jacobson and McCrindle 33 ). Findings from Project EAT (Eating Among Teens), a cross-sectional study using a large sample of American adolescents, showed that availability of foods in the home is among the most important determinants of children’s diets( Reference Ventura and Birch 4 , Reference Neumark-Sztainer, Wall and Perry 11 , Reference Azjen 36 ). The quantitative findings from the present study complement the above findings and add an association with overall diet quality beyond single nutrients, foods or behavioural indices.
It is important to note that we observed significant improvements in all observed health outcomes with an incremental change in response from ‘quite a lot’ to ‘very much’. This may indicate that consistent caring and encouragement by parents has a pronounced benefit to children’s health over moderate expression of these behaviours. We also saw that the incremental changes worked synergistically for encouragement and parental caring: when combined, the positive impact on children’s health outcomes was larger. These findings seem consistent with the existing literature about parenting style. Reviews about the association between parenting style and child overweight indicate that permissive parenting styles (i.e. parents who are not demanding of their child but highly responsive to their needs) and authoritarian parenting styles (i.e. parents who are highly demanding and less responsive to their children) are both associated with childhood overweight( Reference Sleddens, Kremers and Stafleu 3 , Reference Ventura and Birch 4 , Reference Verloigne, Van Lippevelde and Maes 13 , Reference Van Lippevelde, Velde Te and Verloigne 14 ). Meanwhile, authoritative parents who are both moderately responsive and demanding have children with the least likelihood of overweight( Reference Sleddens, Kremers and Stafleu 3 , Reference Ventura and Birch 4 ). This suggests that parents’ personal beliefs about food and the action of those beliefs through encouragement, rather than dictation, for their children work together in influencing children’s eating practices.
The present study has implications for health promotion strategies and interventions. The study reinforces previous evidence-based recommendations that parents are important health promotion targets for the prevention of childhood obesity and improvement of children’s diets. Findings from Project EAT lead to the recommendation that parents both model and encourage healthful eating behaviours without focusing on weight to obtain a healthy weight as well as a positive body image( Reference Neumark-Sztainer, Wall and Perry 11 , Reference Verloigne, Van Lippevelde and Maes 13 , Reference Neumark-Sztainer 20 , Reference Baranowski, O’Connor and Hughes 37 ). When reviewing the literature about parenting and childhood obesity, Lindsay et al. found that parents play a key role in the prevention of childhood obesity not only in terms of their influence on dietary habits but also in their influence on physical activity and sedentary activities( Reference Lindsay, Sussner and Kim 19 ). The authors further stated that existing data on interventions that include parents show promising results in the prevention of childhood obesity, although further research in this area is recommended( Reference Lindsay, Sussner and Kim 19 ). Our work answers this call for research. Our findings inform interventions to prioritize healthy eating and prevent childhood obesity. We showed that parental caring about healthy eating plays a role in children’s dietary habits and body weight, which may be reflected through improved home availability of healthy foods. Parental encouragement of healthy eating may add to this improvement in health behaviours and outcomes by influencing what children choose. Although we recommend parents as important targets for health promotion strategies, we acknowledge that the improvement of children’s diets and preventing childhood obesity require an integrated, broad approach.
The REAL Kids Alberta Evaluation provides a large, representative sample of children, generalizability of results, directly measured heights and weights and a relatively high response rate, which should be considered as strengths. The usage of an FFQ allowed us to calculate a diet quality index which is reflective of overall disease risk due to diet. The findings from the present study are also underpinned by a robust, widely used theory regarding decision making and behaviours. The Theory of Planned Behavior( Reference Azjen 36 ) states that beliefs and actions founded on those beliefs predict behavioural intention, the most important predictor of a behaviour( Reference Andrews, Silk and Eneli 17 ). In the present study, we can deduce that positive parental support towards healthy eating is predictive of parents’ behaviour; that is, provision of healthy food opportunities for children. The cross-sectional design of the research is a limitation to interpretations of causality. Additionally, self-reported survey data are subject to error and the health behaviours in question are prone to social desirability bias. The high prevalence of parental encouragement and caring about healthy eating may be indicative of volunteer bias and not be representative of subgroups that may not be able to prioritize or access healthy eating opportunities such as socio-economically disadvantaged populations. It has also been documented that parenting practices and styles are defined inconsistently in the literature and measured using a wide variety of tools( Reference Ventura and Birch 4 , Reference Baranowski, O’Connor and Hughes 37 ). As such, comparisons of our findings to existing parenting literature may be challenging. Future study on this topic should include home availability of vegetables and fruit, which may be an intermediate variable in the relationship between parental encouragement and caring with their child’s diet and body weight( Reference Neumark-Sztainer, Wall and Perry 11 , Reference Verloigne, Van Lippevelde and Maes 13 , Reference Rosenkranz and Dzewaltowski 38 ). Future studies should also include more components of parental practices in regard to eating. The present study was limited to the two components included.
Conclusions
The present research showed that parental encouragement and caring about healthy eating have important implications for body weight status and children’s diet, most notably an improvement in overall diet quality. Further, the present research demonstrates that even when parents report a high prevalence of moderate to high caring and encouragement, the highest reported practices are associated with the most benefit to children. Health promotion initiatives that engage parents to consistently and effectively encourage and care about healthy eating may result in improvement of dietary outcomes of children and reduction of the prevalence of childhood obesity.
Acknowledgements
Acknowledgements: The authors thank all students, parents and schools for participating in the study. They also thank all evaluation assistants and health promotion coordinators for collecting and processing data; and Connie Lu, Pamela Bailey, Megan Purcell, Shelby Corley and Wendy Davis for leading the data collection, management and validation. Financial support: The REAL Kids Alberta Evaluation was funded through a contract with Alberta Health. The contract with Alberta Health supported data collection but had no role in the design, analysis or writing of this article. The present research was further funded through a Canada Research Chair in Population Health, an Alberta Research Chair in Nutrition and Disease Prevention, and an Alberta Innovates Health Solutions Scholarship to P.J.V. These sources of funding did not have a role in the design, analysis or writing of this article. All interpretations and opinions in the present study are those of the authors. Conflict of interest: None. Authorship: E.F., lead author of the paper, conducted all analyses and led all literature search, writing and interpretations. K.V.P. provided key support in conducting analyses and structuring the writing of the paper. Y.L.C. provided key support in conducting analyses, assisting in interpretation and provided extensive feedback for writing. K.S. assisted in the development of the research question, design of the study, in interpretation and providing feedback; and serves on the supervisory committee for E.F.’s studentship. P.J.V., Principal Investigator for the REAL Kids Alberta Evaluation which provided the data for this secondary analysis, played a key role in the development of the research question, design of the study, interpretation of results, structuring and writing of the manuscript; and serves as supervisor for E.F.’s studentship. Ethics of human subject participation: All procedures involving human subjects were approved by the University of Alberta’s Health Research Ethics Board. Informed, written consent for both parental and child participants was obtained from participating parents, written assent was obtained from all participating children.






