Diets in China have changed significantly in the past 30 years and have changed more in urban areas than in rural areas. In 1987–88 the Chinese Government began conducting the Child Health and Nutrition Survey (CHNS), which established a baseline and continues to monitor child health and nutrition trends. Data from the CHNS suggest that over time diets have increased in fat, protein and sodium intake and decreased in the consumption of coarse grains, which have been replaced by refined grains. The consumption of animal-source foods has increased, as has the consumption of edible oils and the proportion of foods that include added sugars. Snacking and eating away from home have increased( Reference Zhai, Du and Wang 1 , Reference Wang, Zhai and Wang 2 ). These changes are most pronounced in major urban areas among wealthier and better-educated Chinese( Reference Wang, Zhai and Zhang 3 ). Changes in children’s diets reflect changes in adults’ diets( Reference Dong, Howard and Herring 4 ). Separate regional studies have confirmed increases in children eating more refined grains( Reference Bai, Wang and Liu 5 ), snacking more often and snacking on items containing more sugar( Reference An and Fang 6 ).
Education and public health leaders have noted these changes and begun experimenting with policies and programmes to try to increase beneficial behaviours in order to slow or reverse trends towards less healthy eating behaviours.
Changing eating behaviours is possible but difficult. Previous research suggests that for programmes to be effective in changing eating behaviours they need to address individual factors such as knowledge, attitudes, self-efficacy, norms, behavioural control and skills, as well as environmental factors such as interactions with important people like parents, teachers and community members, the availability of nutritious food and safe water, and a physical environment supportive of good eating practices( Reference Khambalia, Dickinson and Hardy 7 – Reference Feng, Xu and Huang 11 ). A recent systematic review of school-based behavioural interventions suggested that no single behavioural intervention could be as effective as a combination of interventions addressing both individual student needs and school environmental situations( Reference Khambalia, Dickinson and Hardy 7 ). Based on this principle, the US Centers for Disease Control and Prevention( 12 ) and the WHO( 13 ) have both proposed comprehensive programmes for improving the nutritional status of young people. The programme described in the present paper is based on WHO’s Health Promoting Schools model( 13 ) and is called a comprehensive nutrition education programme aimed at improving the eating behaviours of grade 4 primary-school students herein. Both the US Centers for Disease Control and Prevention’s comprehensive health education model and the WHO’s Health Promoting Schools concept operationalize Bandura’s social leaning theory that explains human behaviour in terms of a continuous interaction of cognitive, behavioural and environmental influences( Reference Bandura 14 – Reference Blitstein, Cates and Hersey 16 ). The healthy eating objectives that were the focus of this comprehensive programme were selected from The Guidelines for Nutrition and Diet for Chinese Residents ( 17 ). The present paper describes the evaluation of a comprehensive school-based nutrition education programme designed to improve the eating behaviours of grade 4 primary-school students.
Methods
Ethics approval
The China Center for Health Education (CCHE), the provincial bureau of health and the city bureaus of health and education all approved the project. Written parental consent was obtained prior to the start of children’s involvement in the primary-school-based nutrition education programme evaluation. The data analysis was conducted with a de-identified data set by a team of faculty and graduate students in the Department of Educational Psychology at the University of Nebraska–Lincoln (USA). The Institutional Review Board of the University of Nebraska–Lincoln reviewed and approved the analysis of the de-identified data (IRB approval number 20151215742EX).
Developing the comprehensive nutrition programme
This programme originated from discussions between health educators at the CCHE and health educators at the provincial and city level in Qinghai and Shandong. Qinghai is an interior province in China’s north-western high-altitude plateau and includes a number of ethnic minority groups. It has the second lowest provincial gross domestic product in China. Shandong is located on China’s east coast and has the third highest provincial gross domestic product. Developing and evaluating this new programme in two economically different areas was considered important to increase the generalizability, if the programme seemed to be effective.
The development of the proposed programme was led and coordinated by two health education specialists from the CCHE. The two specialists assembled an advisory panel consisting of professionals from the fields of health education, health promotion, behavioural sciences, education, physical education, nutrition, and statistics and epidemiology. This panel identified the project’s specific objectives and then produced the Handbook for Youth Nutrition and Exercise (handbook) that served as the project’s foundation. The handbook outlined the project’s nine behavioural objectives, the nutritional content to be shared, the education and communication strategies to be used, and the steps in project monitoring and evaluation. The first draft of the handbook was modified as planning proceeded to accommodate local conditions.
Sampling
The programme’s effectiveness was evaluated in two provinces, one economically developed province and one economically underdeveloped province. For evaluation purposes a convenience sample of schools was selected from each province. Provincial authorities selected three cities in each province and then, in consultation with local officials, selected two primary schools in each city. Inclusion criteria specified that eligible schools had not previously been involved in a major health education diet/nutrition-related project, had enrolments of at least 1000 students, and included school administrators and school leaders and local health department officials willing to work together to develop and implement the programme. Once the schools were identified, one school in each city was randomly designated a programme school and the other school became the control school. Control schools continued their standard educational practices. Grade 4 students were selected for the programme because they are considered old enough to master the cognitive/knowledge/skill aspects of the proposed programme and they and their parents were not yet preoccupied with preparation for the grade 5 national examinations for entry into middle school.
Implementation of the programme
Beginning in 2014, the principal in each programme school appointed a school health committee consisting of leading teachers, parents and community leaders. The committee included health educators from the city bureau of health and the city bureau of education. This committee began its work by holding discussion groups with teachers, school staff, parents and community leaders. Information, directions and suggestions from these discussion groups were then integrated into the handbook. When the handbook was completed, the principal in each programme school met with classroom teachers, physical education teachers, the school doctor, health teachers, and representatives from the cities health and education bureaus to plan the specific activities for their school. The project allowed some flexibility to accommodate local conditions, but the core programme activities were required: (i) integrate nutrition lessons and activities into all 4th-grade classes; (ii) provide programmes on nutrition and physical activity for all teachers twice per semester; (iii) provide a community programme about good nutrition for parents once per semester; (iv) distribute information pieces about nutrition and physical activity to all 4th-grade students; (v) develop social media messages on nutrition to be distributed twice per semester; (vi) develop and post blackboard and wall messages promoting good eating, to be posted twice per semester; and (vii) organize community programmes related to good nutrition once per semester.
The Health Promoting School model includes making tangible changes in the environment that enable and reinforce the healthy behaviour students are taught in class. The intervention taught 4th graders to eat more vegetables and fruits and to drink more water. On the environmental level, schools were expected to improve school food and access to safe drinking-water.
Each programme school principal was responsible for ensuring these activities were carried out during the year of implementation. The programme school principal planned and coordinated staff and teacher training activities to implement the new comprehensive nutrition education programme.
Programme outcome measures
Nine outcome measures were identified by the panel of experts convened by CCHE at the beginning of the project. The nine measures were based in the content of The Guidelines for Nutrition and Diet for Chinese Residents ( 17 ) and panel members’ experiences with nutrition education. Students self-reported the number of times they did each behaviour on a survey. A value of 1 was given if a student reported performing a behaviour at or exceeding the recommended level, a value of 0 was given if a student reported performing a behaviour lower than the recommended level; otherwise responses were coded as missing. The sum of scores indicated the number of eating behaviours for which a student met the recommended level, with a maximum score of 9. Specific behaviours and the recommended level for each behaviour are shown in Appendix 1.
The programme was conducted during the entire school year of the students’ 4th grade. Pre-programme measures were collected from students in the last month of their 3rd-grade year and post-programme measures were collected in the last month of their 4th-grade year. The student surveys were carried out by personnel from the local bureau of health in all classes during school hours.
Quality control
The principal and teachers maintained the daily records of programme activities for their school. Twice each semester, staff from the local-level Centers for Disease Control (CDC) met with the principal and teachers of each programme school to review the record of programme activities and discuss any modifications being made to the planned programme. Once each semester staff from the province-level CDC and the specialists from the CCHE visited the programme city to review programme activity records, encourage programme adherence and address problems arising during the programme implementation. Observations from these regular visits provided feedback on adherence and implementation issues.
Statistical analysis
Descriptive statistics described the average number of recommended eating behaviours reported by all groups, pre- and post-programme, in each province, as well as the proportion of students meeting the recommended level for each behaviour at post-assessment in each province. Descriptive summary was calculated using the statistical software package IBM SPSS Statistics version 25.
A two-level model was used to evaluate the time × intervention interaction effect on students’ eating behaviour for all students. Many students who completed the questionnaire at both time points changed classrooms between 3rd and 4th grade, so random effects of students and classrooms were crossed. Time (pre-programme and post-programme) was the predictor at level 1; intervention (control and programme) and province (Qinghai and Shandong) were the predictors at level 2. The advantage of multilevel modelling over traditional methods for analysing behaviour change is that it does not require equal numbers of responses from each participant. Students with missing values were not excluded but their scores contributed less to the results( Reference Raudenbush and Bryk 18 ). The complete model is presented in Appendix 2. Data analysis was done with the MIXED procedure in the statistical software package SAS version 9.4.
Results
In the present analysis, there were 2847 (63·5 %) students from Shandong and 1635 (36·5 %) students from Qinghai; 2086 students (46·5 %) were in programme schools and 2396 students (53·5 %) were in control schools; 2398 (53·5 %) were male and 2069 (46·2 %) female, with fifteen (0·3 %) not reporting gender.
Pre/post scores
Table 1 shows the average number of eating behaviours that met the recommended levels at pre- and post-assessment for both the programme and control schools in each province. At pre-assessment, Shandong students in control and programme schools on average met recommended levels for four behaviours, and Qinghai students in control and programme schools met recommended levels for three behaviours. After post-assessment, Shandong students in programme schools on average met recommended levels on six behaviours, and Qinghai students in programme schools met recommended levels on four behaviours.
Table 1 Average number of grade 4 students’ eating behaviours meeting recommended level (of nine possible) by province and intervention group at pre- and post-assessment, China, May 2014–June 2015

Multilevel modelling
Table 2 indicates a significant interaction effect between intervention and time, indicating that score change from pre- to post-assessment was different between students in the programme and control schools. On average, students in Shandong met or surpassed recommended levels on significantly more eating behaviours than students in Qinghai, controlling for the other variables in the model.
Table 2 Fixed effects of predictor variables on grade 4 students’ eating behaviours, China, May 2014–June 2015
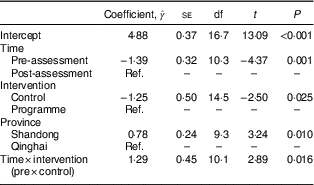
Ref., reference category.
Satterthwaite approximation was used for denominator df.
Because of the significant interaction effect, a follow-up test was done. At post-assessment, students in the programme schools had a significantly higher score than students in the control schools (meanpost,control – meanpost,programme = −1·25, se = 0·50, t (14·5) = −2·50, P = 0·025) and showed improvement in healthy eating behaviours after the comprehensive nutrition education programme (meanpre,programme – meanpost,programme = −1·39, se = 0·32, t (10·3) = −4·37, P = 0·001). The full result of the follow-up test is presented in the online supplementary material, Supplemental Table 1.
Proportion of achievement
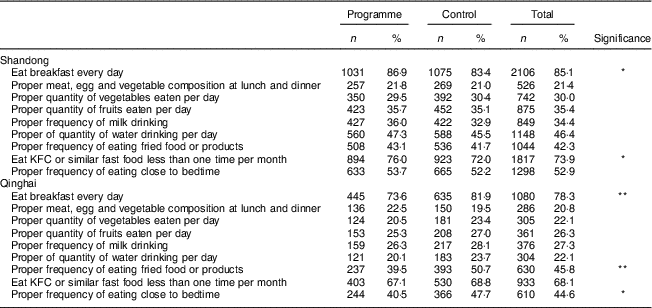
Table 3 shows small but inconsistent differences between the programme and control schools at pre-assessment. Table 4 shows that in Shandong a significantly larger proportion of the students in the programme schools than in the control schools met the recommended level for each of the nine eating behaviours. In Qinghai, a significantly larger proportion of the students in programme schools than in control schools met the recommended level for three of the nine behaviours. In general, eating breakfast every day and eating fast food less than once per month were the two behaviours reported by the most Shandong and Qinghai students. Having proper vegetable-to-meat/egg composition at lunch and dinner and drinking milk every day were the two behaviours reported the least among Shandong and Qinghai students.
Table 3 Pre-assessment: proportion of grade 4 students meeting the recommended level for each eating behaviour in control and programme schools by province, China, May 2014–June 2015
Missing data were excluded from calculation.
Difference between programme and control schools: *P <0·05, **P <0·001.
Table 4 Post-assessment: proportion of grade 4 students meeting the recommended level for each eating behaviour in control and programme schools by province, China, May 2014–June 2015

Missing data were excluded from calculation.
Difference between programme and control schools: *P <0·05, **P <0·001.
Quality control observations
Observations of programme implementation by the CCHE and CDC technical assistance teams made at the quality-control visits and reviews of the programme activity records maintained by the school principals indicated that Shandong schools were more successful in implementing the various programme activities and making upgrades to the school facilities and food services than the Qinghai schools. Principals reported difficulty in getting teachers to integrate nutrition topics into their classes throughout the curriculum. Considerable effort was needed to help teachers, staff and parents accept involvement in the novel aspects of the programme, such as parent–child joint activities. A great deal of effort, especially in Qinghai, was needed to find ways to improve the quality of food served at school and improve access to safe drinking-water.
The CCHE and CDC technical assistance teams who visited the programme schools observed that not all principals were equally supportive of the programme, especially at the beginning. The project created extra time demands on programme school principals and teachers. Qinghai principals were especially reluctant to commit resources and time to a programme with an unknown outcome.
Teachers and principals had opportunities to talk with parents and community members during the nutrition education activities arranged for them. They reported that parents and community members were reluctant to participate in the activities planned for them, largely because they had never attended something like this in the past, and they did not read the nutrition information pieces distributed to them as part of the parent and community activities. Some schools attempted to communicate information to parents by popular social media, but the effectiveness of this approach was not measured.
Discussion
This comprehensive school-based nutrition programme was more effective in improving students’ self-reported eating behaviours in Shandong than Qinghai. In Shandong, students’ self-reported behaviour improved on nine eating behaviours compared with Qinghai where students’ scores improved for only three of the eating behaviours. For each of the three improved behaviours in Qinghai the difference at post-assessment compared with pre-assessment was smaller than the pre–post differences of the Shandong students. While the magnitude of change in the two provinces was significantly different, the general positive results were similar to other Chinese studies( Reference Zhang, Cai and Tan 19 – Reference Mie, Sun and Wang 21 ).
Eating breakfast every day and eating fast food less than once per month were the two behaviour recommendations met by the most students in both provinces at pre-assessment and post-assessment. Even though the proportion of students in both provinces eating breakfast every day was high, the scores increased significantly in the programme schools in both provinces leading us to believe the change was likely the result of the nutrition education programme. Eating breakfast is largely under the control of parents, so it is possible the programme had an effect on parent behaviour either indirectly through students talking to their parents or directly through the educational and communication activities designed for the parents.
The one behaviour achieved by the fewest students at post-programme, even in the programme schools, was eating the proper vegetable-to-meat/egg composition at lunch and dinner. This was perhaps the most complex behaviour for students to carry out. Luncheon foods are largely under the control of the schools, so it is possible that the Shandong schools were able to revise their lunch menus in a positive manner and may also have been better at communicating this complex expectation to parents. The absence of change among Qinghai students suggests schools were unable to change this very specific aspect of food services in a noticeable manner and were unable to communicate this expectation to parents in an effective way.
In Shandong there was a significant increase in the proportion of students drinking milk, although this remains one of the eating behaviours reported by fewest students. In Qinghai there was no difference between programme and control schools in milk drinking. Increasing milk consumption is a challenge. Widespread availability of dairy products is relatively recent in China and many Chinese, including children, are lactase deficient. Lactose malabsorption prevalence is high( Reference Yang, He and Cui 22 ).
Even with the positive effects of this comprehensive nutrition education programme on eating behaviours of 4th graders, especially in Shandong, the 4th graders still showed low levels of several key healthy behaviours. Only 40·3 % of Shandong students and 19·6 % of Qinghai students reported eating a proper combination of vegetables/meat/eggs, only 54·7 % of students in Shandong and 33·9 % in Qinghai ate fruit every day, and only 61·3 % of the students in Shandong and 27·6 % of students in Qinghai ate vegetables every day. Unfortunately, this is the only known study conducted in China that used this set of behavioural measures, so it is not possible to suggest how representative these rates may be.
At both pre-assessment and post-assessment, in both control schools and programme schools, more students in Shandong reported the recommended eating behaviours than students in Qinghai, suggesting an overriding difference between the two provinces. Indeed, these two provinces were chosen because they are economically different and we wondered if the economic differences would influence the effectiveness of a comprehensive nutrition education programme, and clearly they did. Others have noted economic effects on children’s diet. Wang and colleagues( Reference Wang, Bentley and Zhai 23 ) reported that children in China in high-income families were more likely to maintain a high-meat diet over several years, and children living in the coastal regions were more likely to maintain a low-vegetable-and-fruit diet. Several studies have found milk consumption is associated with economic status( Reference Wei, Yang and Yan 24 , Reference Zhou, Tian and Wang 25 ). Other studies have found parent education level is associated with both economic status and healthier nutrition behaviours of their children( Reference Qian, Zhang and Newman 26 , Reference Feng, Liang and Zhu 27 ).
The difference in students’ scores in the two provinces may also have been affected by the geography of the two provinces. Shandong is on the east coast, on China’s main transportation networks and adjacent to major food-producing regions, meaning residents of Shandong may have easier access to a wider variety and to less expensive foods. Shandong enjoys a moderate climate compared with Qinghai, which is located on a semi-arid high-altitude plateau and has low-density livestock-based agriculture. The lower student scores in Qinghai for eating vegetables every day, eating fruits every day and frequently drinking milk all suggest the possibility that geographical factors, such as climate and transportation, affected the outcomes of this programme. There is little information to confirm a geographic explanation for the differences. Chinese literature on child nutrition has noted rural–urban differences but with little explanation about the reasons for these differences( Reference Zhai, Du and Wang 1 , Reference An and Fang 6 , Reference Zhang, Cai and Tan 19 ).
The observations made by the local and province-level technical assistance teams during the quality-control visits suggested that introducing the programme presented significant challenges and created low-level resistance for school personnel in both provinces. Involvement of school principals, staff, parents and local officials from the earliest planning stage through the entire school year was helpful to overcome the initial resistance. By the end of the programme year, the nutrition education programme appeared to have wider general support. Perhaps the greatest resource challenge faced by all schools, but especially the schools in Qinghai, was finding ways to improve the quality of food served at school and expand access to safe drinking-water.
Several of this programme’s activities deviated from traditional school practices. Even in elementary schools the pressure on teachers is significant. All Chinese 5th-grade students take a test that determines the schools they go to at the next level, and teachers feel the pressure to prepare students to do well on the test. Teachers are reluctant to teach lessons on nutrition, which is not a subject covered in the academic test. However, China is revising many of its teacher education programmes and modernizing school organization, so resistance to teaching innovations and new topic areas may be less significant in the future. The effect of generalized teacher resistance to aspects of this programme on the students’ scores is unknown. Support for the comprehensive nutrition education programme varied in degree among the programme schools and was perhaps less enthusiastic in Qinghai than in Shandong. No attempt was made to quantify support among teachers, staff or parents by individual school, and no attempt was made to judge programme effect by school. Increasing programme support among all school personnel could significantly increase learning and behaviour change among the elementary-age students. Any future iterations of this programme should consider assessing these variables in the evaluations.
The sensitivity of the programme evaluation was limited to the achievement of nine key eating behaviours. These were based on Chinese nutrition guidelines developed in response to rapid diet change in the last 30 years and, in at least one instance, on a prevailing cultural belief that it is unhealthy to eat close to bedtime. Future evaluations could benefit from measures of knowledge, expectancies about improving eating behaviours, specific behavioural intentions, and should consider measuring parent behaviours as well as student behaviours. Now that the basic programme model has been tried, programme effectiveness could possibly be improved by adding more preparation of teachers and staff, assessments of programme fidelity to the planned implementation and assessments of teacher enthusiasm for the programme.
This programme benefited from teachers and school staff being involved in developing activity plans from the very first stage. The effort and input from the technical support team from the CCHE and the provincial bureaus of health and education was a significant factor in this programme and is not sustainable. How long and with what degree of integrity the innovations that have been introduced will be maintained is not known.
Attempting to replicate this comprehensive elementary-school nutrition education at other schools, where teachers and staff were not involved in the programme development, will need to prepare teachers to use its modern (non-traditional) education techniques. School administrators at other schools will face the same hurdles of scheduling time, keeping records, and finding the money to improve school drinking-water and food services.
Given that this programme, despite its novelty, was carried out in six schools and produced modest but beneficial changes, the next stage is to implement the programme in a larger sample of schools without the national and provincial technical support, with schools relying on the local bureaus of health and education for cooperation and assistance.
Limitations
The number of schools (twelve) was too few to accommodate a nested design to assess school differences. This research looked at short-term programme effects, which were encouraging, but only long-term evaluation will truly confirm the programme effects and the possibility of contributing to improvements in child health. The evaluation base was narrow. A broader array of outcome measures would have been more informative. We do not know how much the special assistance given to this new programme from the outside technical support team or how much the programme’s novelty affected the results. We could not control for any effects from the many possible extraneous events occurring during the year of the programme. We did not evaluate the subjective observations made by visiting experts during quality-control visits against any a priori criteria. Nevertheless, there is much to learn by examining these short-term results that can guide the development of future programmes. While there have been few truly comprehensive school-based nutrition education programmes like this reported in the literature in China, it is encouraging that these positive results are similar to those reported by similar programmes( Reference Zhang, Cai and Tan 19 – Reference Mie, Sun and Wang 21 , Reference Qian, Newman and Shell 28 ).
Conclusion
This 4th-grade comprehensive school nutrition education programme increased healthy eating behaviours and suggested ways that a scaled-up initiative might have a more significant effect. Through maximum use of existing resources, changing eating practices in large populations over time may be done within existing school and public health resources. The findings from this project provide practice-based evidence to guide future school-based nutrition programme development. The present study highlights the need and the difficulty of evaluating school programmes of this type; an essential step in improving the eating behaviours of Chinese primary-school students.
Acknowledgements
Acknowledgements: The authors are grateful to Lanyan Ding (University of Nebraska–Lincoln Department of Educational Psychology) and Natalie Koziol (Nebraska Center for Research on Children, Youth, Families and Schools) for statistical advice. Michelle Maas (University of Nebraska–Lincoln Department of Educational Psychology) assisted with English editing. Financial support: This work was supported by a grant from Ferrero Trading (Shanghai) Co. Ltd to the China Center for Health Education, Beijing. The funder had no role in the design, analysis or writing of this article. Conflict of interest: None. Authorship: L.Q. and W.D. designed the project, recruited schools, provided technical assistance to the local school health committees and to the programme school administrators at all stages of the programme, supervised data collection by staff from the local bureaus of health, and were responsible for the overall quality of the project. L.Q., L.-W.Y. and D.F.S. analysed the data and interpreted results. L.Q. and W.D. wrote the first draft of the manuscript. L.Q., D.F.S. and I.M.N. provided critical edits for the final version. Ethics of human subject participation: Written parental consent was obtained prior to the start of their child’s involvement in the primary-school-based nutrition education programme evaluation. The data analysis was conducted with a de-identified data set by a team of faculty and graduate students in the Department of Educational Psychology at the University of Nebraska–Lincoln (USA). The Institutional Review Board of the University of Nebraska–Lincoln reviewed and approved the analysis of the de-identified data (IRB approval number 20151215742EX).
Supplementary material
To view supplementary material for this article, please visit https://doi.org/10.1017/S1368980018003713
Appendix 1 Specific eating behaviours and recommended levels

Appendix 2 Multilevel statistical model
The model is specified in the equation
 $$\eqalignno { Y_{{ijkl}} {\equals} \gamma _{{0000}} {\plus}\gamma _{{1000}} {\rm Time}_{{ijkl}} {\plus}\gamma _{{0001}} {\rm Intervention}_{l} \cr {\plus}\gamma _{{0002}} {\rm Province}_{l} {\plus}\gamma _{{1001}} {\rm Time}_{{ijkl}} {\times}{\rm Intervention}_{l} {\rm } \cr {\plus}{\rm }e_{{ijkl}} {\plus}u_{{0jkl}} {\plus}u_{{1jkl}} {\rm Time}_{{ijkl}} {\plus}u_{{00kl}}^{{Pre}} d_{{ijkl}}^{{Pre}} {\plus}u_{{00kl}}^{{Post}} d_{{ijkl}}^{{Post}} \cr {\plus}u_{{000l}} {\plus}{\rm }u_{{100l}} {\rm Time}_{{ijkl}} $$
$$\eqalignno { Y_{{ijkl}} {\equals} \gamma _{{0000}} {\plus}\gamma _{{1000}} {\rm Time}_{{ijkl}} {\plus}\gamma _{{0001}} {\rm Intervention}_{l} \cr {\plus}\gamma _{{0002}} {\rm Province}_{l} {\plus}\gamma _{{1001}} {\rm Time}_{{ijkl}} {\times}{\rm Intervention}_{l} {\rm } \cr {\plus}{\rm }e_{{ijkl}} {\plus}u_{{0jkl}} {\plus}u_{{1jkl}} {\rm Time}_{{ijkl}} {\plus}u_{{00kl}}^{{Pre}} d_{{ijkl}}^{{Pre}} {\plus}u_{{00kl}}^{{Post}} d_{{ijkl}}^{{Post}} \cr {\plus}u_{{000l}} {\plus}{\rm }u_{{100l}} {\rm Time}_{{ijkl}} $$
where: Y ijkl is the nutrition behaviour score at the ith time point for the jth student in the kth classroom and lth school;
Time ijkl is a dummy variable distinguishing the pre- and post-test measurements with the post-test as the reference group;
Intervention l is a dummy variable distinguishing the control and programme schools with the programme schools as the reference;
Province l is a dummy variable distinguishing Shandong and Qinghai province with Shandong as the reference;
γ
1000, γ
0001, γ
0002 and γ
1001 are the corresponding main and interaction effects;
![]() $e_{{ijkl}} \,\sim\,N\left( {0,\sigma ^{2} } \right)$
is the level 1 residual effect;
$e_{{ijkl}} \,\sim\,N\left( {0,\sigma ^{2} } \right)$
is the level 1 residual effect;
![]() $u_{{0jkl}} \,\sim\,N\left( {0,\tau _{0}^{j} } \right)$
and
$u_{{0jkl}} \,\sim\,N\left( {0,\tau _{0}^{j} } \right)$
and
![]() $u_{{1jkl}} \,\sim\,N\left( {0,\tau _{1}^{j} } \right)$
are the level 2 student random-intercept and slope effects, respectively;
$u_{{1jkl}} \,\sim\,N\left( {0,\tau _{1}^{j} } \right)$
are the level 2 student random-intercept and slope effects, respectively;
![]() $u_{{00kl}}^{{Pre}} \,\sim\,N\left( {0,\tau _{0}^{{Pre,k}} } \right)$
and
$u_{{00kl}}^{{Pre}} \,\sim\,N\left( {0,\tau _{0}^{{Pre,k}} } \right)$
and
![]() $u_{{00kl}}^{{Post}} \,\sim\,N\left( {0,\tau _{0}^{{Post,k}} } \right)$
are the time-specific (acute) level 2 classroom random-intercept effects activated at the respective time points by the dummy variables
$u_{{00kl}}^{{Post}} \,\sim\,N\left( {0,\tau _{0}^{{Post,k}} } \right)$
are the time-specific (acute) level 2 classroom random-intercept effects activated at the respective time points by the dummy variables
![]() $d_{{ijkl}}^{{Pre}} $
and
$d_{{ijkl}}^{{Pre}} $
and
![]() $d_{{ijkl}}^{{Post}} $
; and
$d_{{ijkl}}^{{Post}} $
; and
![]() $u_{{000l}} \,\sim\,N\left( {0,\tau _{0}^{l} } \right)$
and
$u_{{000l}} \,\sim\,N\left( {0,\tau _{0}^{l} } \right)$
and
![]() $u_{{100l}} \,\sim\,N\left( {0,\tau _{1}^{l} } \right)$
are the level 3 school random-intercept and slope effects, respectively.
$u_{{100l}} \,\sim\,N\left( {0,\tau _{1}^{l} } \right)$
are the level 3 school random-intercept and slope effects, respectively.






