Several pathways potentially link the gut microbiome with common mental disorder(Reference Rieder, Wisniewski, Alderman and Campbell1). Dietary fibre intake is essential in maintaining and shaping the composition of gut microbiome(Reference Simpson and Campbell2). Existing evidence from prospective cohort studies of dietary fibre intake and mood disorders is mixed(Reference Gangwisch, Hale, Garcia, Malaspina, Opler, Payne, Rossom and Lane3, Reference Sanchez-Villegas, Zazpe, Santiago, Perez-Cornago, Martinez-Gonzalez and Lahortiga-Ramos4). We studied associations between dietary fibre intake and common mental disorder (CMD) in the Whitehall II cohort study. We hypothesised an inverse association of fibre intake and incident common mental disorder 5 years later.
Analysis included 15,487 person-observations collected over 22 years of repeated data-collection. Dietary fibre intake was assessed using food frequency questionnaires, and energy adjusted(Reference Brunner, Stallone, Juneja, Bingham and Marmot5). CMD was measured with the 30-item General Health Questionnaire. Random-effects models were used to model the association between dietary fibre intake and CMD over 5-year cycles. CMD cases (⩾5 symptoms) were excluded at the start of each cycle. Analyses were adjusted for potential confounders (shown in Table 1), BMI, central obesity, cardiovascular disease (CVD), diabetes and cancer.
Table 1. Adjusted associations between dietary fibre intake and common mental disorders 5 years later.
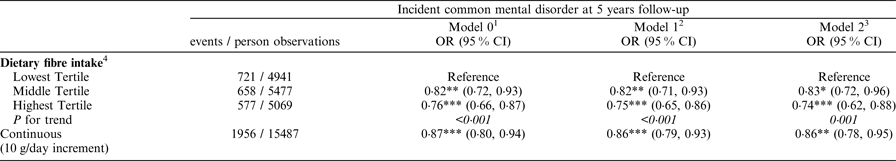
1 Model 0: age, sex, their interaction and ethnicity.
2 Model 1: Model 0 additionally adjusted for marital status, last grade level in civil service, smoking, alcohol intake, physical activity, sleep duration.
3 Model 2: Model 1 additionally adjusted fish intake, modified dash score, coffee and tea intake, sugar intake from sweet food/beverages, sugar intake from sweet food/beverages * sex and total calories.
4 Dietary fibre intake was energy adjusted.
There was a significant inverse association between dietary fibre intake and CMD (Table 1; *P < 0·05, **P < 0·01, ***P < 0·001). This association was slightly attenuated by adjustment for socio-economic factors, health behaviours, other dietary intakes such as sugar intake from sweet food/beverages. Further adjustment for BMI, central adiposity, cardio-vascular disease, diabetes and cancer did not change the results (not shown).
The study findings indicate a protective role of a diet high in fibre in long-term psychological health. In conclusion two of three prospective studies support the hypothesis(Reference Gangwisch, Hale, Garcia, Malaspina, Opler, Payne, Rossom and Lane3, Reference Sanchez-Villegas, Zazpe, Santiago, Perez-Cornago, Martinez-Gonzalez and Lahortiga-Ramos4).



