1 Introduction
As in many other European countries, prenatal diagnosis (PND) was introduced in France in the 1970s, marking the transition from eugenics to genetic counselling.Footnote 1 It was on the initiative of a small number of reproductive scientists and geneticists familiar with international research practices. For many years they enjoyed substantial autonomy, self-regulating their practices as a professional organisation funded by the French national health system. In the 1980s, the international context surrounding medical research changed drastically with the rise of bioethics and of patient-led campaigning that led to the regulation of medical and scientific practices. As shown by French sociologist, Nicolas Dodier, this period saw a shift away from the ‘clinical tradition’ model of healthcare, that privileged the personal authority of practitioners in patient-related decision-making, towards the ‘therapeutic modernity’ model of standardised, evidence-based medicine and the institutionalisation of bioethics.Footnote 2 During genetic counselling consultations, ‘in contrast with traditional clinical encounters, emphasis was placed on the separation between the objective analysis of the situation and the choice between existing options regarding reproductive life and medical intervention’.Footnote 3 This shift went hand in hand with a number of transformations: the decline of medical paternalism and the rise of the patient as an active decision maker;Footnote 4 the introduction of a logic of ‘choice’ and reproductive autonomy into the clinical relationship;Footnote 5 and, not least, the rise of the disability rights movement, which reframed disability as socially constructed,Footnote 6 and which criticised PND for discriminating against disabled people.Footnote 7 As a result of all these changes, PND practices became increasingly regulated – through legislation and by recommendations from national and international organisations.
In 1994, France passed a law on bioethics, of which one of the aims was to regulate PND activities.Footnote 8 The government set up a nationwide network of multidisciplinary PND centres (CPDPNs), to provide expertise and to take responsible for implementation. In 2001, the French minister for health set up the Comité National Technique de l’Echographie (National Technical Ultrasound Committee) to define the brief for ultrasound screening and for diagnosis. In 2004, amendments to the law on bioethicsFootnote 9 created the Agence de la biomédecine (ABM) to govern and monitor the activities of CPDPNs and of diagnostic laboratories, and to come up with guidelines and recommendations, including some that were based on ethical considerations. Focusing on the decision-making autonomy of patients obliged practitioners to inform couples, while at the same time obeying a principle of non-directiveness that transfers responsibility for the decision to women and families, which is sometimes difficult to achieve. Other recommendations, from the biomedical domain, were based on the current state of scientific knowledge; for example, the points to be covered during an ultrasound scan or the calculation of risk associated with given ultrasound soft markers. Furthermore, the courts became involved in the regulation of PND from the 2000s.Footnote 10 Media coverage of high-profile malpractices proceedings considerably increased the concerns of practitioners regarding the threat of legal action.Footnote 11
Historians have examined the dissemination of techniques in different countries. Generally linked to abortion legislation, they mark the shift from laboratory to clinic and from eugenics to genetic counselling. Initially, the latter was essentially a question of vocabulary. In the 1960s, eugenics was no longer well received and the expression ‘human genetics’ was used to refer to the same ideas and practices, focused on the collective good and the prevention of disability. However, with the emergence of genetic counselling, responsibility for decisions relating to reproduction gradually shifted over to women and couples, following the principles of autonomy and non-directiveness.Footnote 12 It was not that geneticists had abandoned the eugenics programme, they had seen that the couples who used their services made ‘rational’ decisions, realising of their own accord that there was convergence between private interests and the interests of the population as a whole, without needing to be directed.Footnote 13
Social scientists have examined practices associated with PND and their effects, including the moral dilemmas faced by womenFootnote 14 and by practitioners.Footnote 15 Others have looked at counselling practices, at the way in which information on risks is provided and understood by women, and at whether or not medical practitioners comply with the principle of non-directiveness.Footnote 16 The autonomy of women and couples, as promoted in counselling practices, has been widely examined. These studies show that a neutral attitude can cause women to feel abandoned.Footnote 17 Several authors have found this liberal orientation, which places responsibility for decision-making on the private sphere, to be an instrument of governmentality,Footnote 18 of ‘biocitizenship’Footnote 19 or of a ‘new eugenics’ based on citizen demands.Footnote 20 But while couples’ decision-making autonomy has been the object of much research, few works have examined the autonomy of practitioners in current PND practices, or the way in which autonomy has been impacted by changes in clinical practices. This article will attempt to redress this gap by offering a detailed analysis of PND practices, rooted in the French local socio-political context that I briefly described above. By observing staff activities in CPDPNs, it examines comparatively how French PND practitioners have been coping with the rapid change that saw the shift from the total autonomy of genetic counselling practices to a legal and institutional framework designed to make them homogeneous. The first section of the article explores the historical context for the establishment of PND practices in France, from the unregulated early 1970s to the implantation of the national regulatory framework introduced by the government in the 1990s and 2000s. It is based on interviews and on a witness seminar organised in 2012 with France’s PND pioneers.Footnote 21 The second section analyses contemporary practices, focusing on decision-making in relation to authorisations by French PND centres for pregnancy termination due to foetal malformation. To do so, I combine two types of sources. To assess the homogeneity of practices targeted by the regulatory framework, I use administrative and quantitative data on the activity of each centre. I complemented these sources with an ethnography of work organisation and of the processes of deliberation found in two selected centres – one in Paris, the other in the provinces. The inductive analysis of the ethnographic data reveals differences in decision-making processes and attitudes towards PND, topics that are usually absent in archival sources. This analysis shows major differences in the way practitioners interpret official guidelines, define their missions and organise their work in such a way as to maintain relative autonomy.
2 The Establishment of Prenatal Diagnosis in France
The first positive prenatal diagnoses were made in France in 1970, following the development of a successful foetal cell culture technique by geneticist Joëlle Boué and bacteriologist André Boué, a Paris-based husband-and-wife team.Footnote 22
2.1 Infrastructure and Technologies Under Practitioner Control
Although abortion was still illegal at that time in France, so-called therapeutic abortion was allowed from 1939 under a change to the Code de la Famille in cases where the pregnancy endangered the mother’s life.Footnote 23 From the 1950s, the dispositif used by obstetricians who practiced such abortions was later expanded to include other indications, such as German measles and toxoplasmosis.Footnote 24 The chromosomal anomalies and metabolic diseases discovered through PND were added to the list of indications, without any change in procedure and without practitioners having to worry about the authorities.
This context enables the understanding of the reasons why the PND pioneers did not take part in public debates on abortion that raged in 1970s France; several of them confirmed this during the interviews:
I never wanted to be part of any of those movements (
![]() $\ldots$
) We certainly didn’t hide away, but we never went to any opposition or public meeting or anything like that. (
$\ldots$
) We certainly didn’t hide away, but we never went to any opposition or public meeting or anything like that. (
![]() $\ldots$
). We kept to our technical, scientific field. I think we made the right choice because that’s why people trusted us (André Boué, extract from an interview with Marianne Bach in 2001).Footnote
25
$\ldots$
). We kept to our technical, scientific field. I think we made the right choice because that’s why people trusted us (André Boué, extract from an interview with Marianne Bach in 2001).Footnote
25
The therapeutic abortion dispositif sufficed to meet their needs. Indeed, they were not all in favour of the deregulation of abortion, as can be seen in this extract from a speech given by Professor Hervet, a gynaecologist-obstetrician, during the Entretiens de Bichat sessions in 1970:Footnote 26
To give just one example, nowadays in many cases of German measles contracted at the beginning of a pregnancy (
![]() $\ldots$
) an expert can be found to sign the abortion protocol (
$\ldots$
) an expert can be found to sign the abortion protocol (
![]() $\ldots$
). Medical abortions are agreed with a liberalism that is increasing from one day to the next, a liberalism that it is neither necessary nor possible to enclose in new legislative devices.
$\ldots$
). Medical abortions are agreed with a liberalism that is increasing from one day to the next, a liberalism that it is neither necessary nor possible to enclose in new legislative devices.
The link between the history of genetic counselling and women’s mobilisation for the right to abortion, a major issue in many countries,Footnote 27 would not appear to be pertinent to the case in France, although the fact that the techniques were available would at some stage probably have led to a broader law on foetal indications. In 1970, draft legislation was put forward in this respect but was immediately rejected on the basis that it did not resolve the public health problem of illegal abortions.Footnote 28
However, the government’s delegation of the matter of reproduction to scientists and doctors is demonstrated by the specific nature of the French law.Footnote 29 While most countries that had legalised abortion had restricted the practice to the term of foetus viability, French legislation clearly distinguished between two reasons. On the one hand, it set the term beyond which a voluntary termination (IVG) could no longer be performed at ten weeks of pregnancy, which is very restrictive compared to other countries.Footnote 30 On the other hand, in accordance with the requests of PND pioneers, it imposed no limits on medical termination of pregnancy (MTP):Footnote 31
You know that our law does not provide for any term limit (for MTP) That was my doing. (
![]() $\ldots$
) When Simone Veil made her law, she asked for my advice on the medical aspects. (
$\ldots$
) When Simone Veil made her law, she asked for my advice on the medical aspects. (
![]() $\ldots$
) We worked very closely with our colleagues abroad. They had all set a term limit and this was creating all sorts of problems. If you were there the week before, you could terminate the pregnancy, but one week later you could not. I explained this to Simone Veil. I said that the ideal solution was to have no limit because otherwise there’d be terrible situations. She said ‘That’s what I’ll do’ (André Boué, extract from an interview with Marianne Bach in 2001).
$\ldots$
) We worked very closely with our colleagues abroad. They had all set a term limit and this was creating all sorts of problems. If you were there the week before, you could terminate the pregnancy, but one week later you could not. I explained this to Simone Veil. I said that the ideal solution was to have no limit because otherwise there’d be terrible situations. She said ‘That’s what I’ll do’ (André Boué, extract from an interview with Marianne Bach in 2001).
Once the technique had been perfected, the dissemination of PND practices was facilitated by recourse to another dispositif, one developed for the neonatal diagnosis of phenylketonuria (PKU), introduced in France in 1966.Footnote 32 Based on a nationwide network of maternity centres and diagnostic laboratories, this dispositif was managed by an association of geneticists (AFDPHE – Association Française pour le Dépistage et la Prévention des Handicaps de l’Enfant). An initial experiment, carried out between 1974 and 1977 in five university towns, gave pregnant women aged forty and older the opportunity to have an amniocentesis to examine the foetal karyotype; the detection of Down syndrome automatically led to an abortion.Footnote 33 In 1980, an agreement signed by the AFDPHE, the Association des centres de biologie prénatale and the Caisse nationale d’assurance maladie set the fee for the procedure and the age threshold at thirty-eight, with the French health service reimbursing the AFDPHE. Women therefore had nothing to pay up front.Footnote 34
Realising early on that targeting women aged thirty-eight and over led to only 20 per cent of Down syndrome foetuses being diagnosed, French researchers focused their efforts on ‘women at added risk’.Footnote 35 Screening then became possible through the use of maternal serum markers, a procedure tested by the AFDPHE in the 1990s and reimbursed by the French health service from 1997 onwards. Merging into existing dispositifs, French researchers, geneticists and biologists thus quietly set about introducing PND in France, using a model that some described as professional self-regulation.Footnote 36
While PND was becoming rooted in the clinic, practitioners organised collegial practices. At the end of the 1970s, most hospitals in which there were PND practitioners had created multidisciplinary teams that met regularly to discuss possible MTP cases. They had two functions: 1) emotional, they avoided the practitioner having to make a decision on his/her own, making it possible to defer what was often a difficult decision and sharing responsibility by calling upon complementary skills; 2) ethical, these teams constituted a space for reflection upon practices and made it possible to introduce local regulations. The oversight committee at Toulouse hospital is one such example among many.Footnote 37 The interactions developed between obstetricians, paediatric geneticists and foetal pathologists, along with improvements in technical performance, particularly in the field of ultrasound, led to the emergence of a new medical segment:Footnote 38 foetal medicine. A learned society – the Club de Médecine Fœtale – and a journal of the same name, were created in the mid-1980s. Training was then organised and an annual Foetal Medicine Congress came into being in the 1990s.
Unlike other countries, such as Germany for example,Footnote 39 PND practices were introduced in France in a slow and quiet fashion. The main driving forces were the government’s total delegation to geneticists and biologists and the French health system’s funding of PND programmes before abortion legislation had even been passed. The shift from laboratory to clinic took place just as smoothly due to medical eugenics being traditionally present in France.Footnote 40 Most of the pioneering PND geneticists were indeed both researchers and physicians. There was no public debate on the matter.Footnote 41 Public debate did not cover medical abortion, as feminists defended free abortion with support from doctors other than those promoting PND. Disabled persons groups were slow to react and adopted a liberal and nuanced stance. The economic argument that had caused public controversy in countries such as Sweden,Footnote 42 although probably mobilised by the government to decide on how to fund the programmes, remained implicit. In such a context, practitioners and researchers remained perfectly autonomous when it came to regulating their own practices.
2.2 The Era of Regulations
The situation changed in the 1990s and to an even greater extent in the 2000s. The cognitive and moral context surrounding clinical practice in general was transformed. In France, as in most Western countries, a liberal vision of genetic counselling replaced the previous prevention of disability.Footnote 43 PND would be framed no longer as a means ‘to prevent children with serious diseases from being born, but rather ‘to assist pregnant women in making their own choices’.Footnote 44 An ethical split in fœtal diagnosis arise ‘during which the providers of the technology assume the responsibility for only the reliability of the technologies while the ethical and existential choices about the selective termination of pregnancies to pregnant women personal choice and autonomy of women and family are in the fore’.Footnote 45
The logic of rational choice increasingly dictated both official discourse and medical consultations; decisions on whether or not to opt for prenatal screening and diagnosis were increasingly left to the private sphere and private individuals.Footnote 46
This transformation was particularly reflected in a new determination to regulate and control practices in France. In the wake of the 1994 law on bioethics, policymakers introduced one regulatory text after another to govern practices and to officially certify professional bodies. Regarding the decision to perform a MTP, the law made it obligatory for the woman to seek authorisation from a CPDPN. Each centre comprised a coordinator, obstetricians, sonographers, geneticists and neonatologist-paediatricians, often with other specialists such as surgeons, paediatric cardiologists, foetal pathologists, psychologists, and so on. Every request for an MTP was required to be discussed by a multidisciplinary staff, who gave a consultative opinion; two doctors working in the chosen centre were required to sign the attestation authorising an MTP. CPDPNs were and still are located in public or not-for-profit care centres, with the aim of offering equal access to healthcare.Footnote 47 Centres vary in size, history and organisation. The Agence de la biomédecine (ABM), a state agency essentially made up of doctors, was tasked with monitoring PND equity and homogenising practices throughout the country.Footnote 48 Since the ABM was set up in 2004, CPDPNs have each year provided the Agence with an activity report detailing the number of MTPs performed per type of foetal pathology and the term of pregnancy at which they took place. The Agence is tasked with gathering, analysing and disseminating the annual reports issued by the centres. It has made recommendations that regulate the practice and obligations of doctors and that place women’s decision-making autonomy at the heart of the prenatal consultation.
Over a period of ten years, a whole range of regulatory texts were passed to ensure that practices remained equitable and homogeneous, removing medical decision-making (particularly that of pregnancy termination) from the doctor–patient relationship and placing it under peer control, within the framework of collegial practice, supervised by a government agency and regulated by legislative texts. After several decades of total delegation to doctors, the State would appear to be wanting to take back control of PND practices. One might wonder about the effectiveness of this new regulatory framework, about the manner in which practitioners have appropriated it and about how it has affected PND practices at population-level.
3 Prenatal Diagnosis Practices in CPDPNs: A Comparative Analysis
In this second part of the article, I draw on two types of data to shed light, comparatively, on the transformations of practices induced by the regulatory framework that had been imposed on practitioners. The first section compares the activity records of each centre, in particular the number of MTP certificates signed each year according to the type of foetal indications. This analysis makes it possible to objectify differences in attitudes between centres and to question therefore the alleged homogeneity of practices that dominated professional discourse. The second section presents a comparative ethnographic analysis of two centres. Indeed, it is only through the direct observation of these practices, located in singular local contexts, that the researcher can identify processes and mechanisms that accounted for the differences observed quantitatively. As a result, this section covers three themes that emerged inductively from the data. The first theme concerns the organisation of the teams’ work, while the other themes derive from deliberations and decision-making processes, namely the way MTPs were discussed and uncertainty and disability tolerance.
3.1 CPDPNs Activity: Apparent Homogeneity
Today, official discourse typically declares that the objective of PND practice regulation has been met. Practitioners and experts unanimously point out the considerable homogeneity in the indications that are the object of MTP authorisations.Footnote 49 The argument is based on the analysis of centres’ refusals to accept couples’ requests for an MTP. Such refusals are in fact rare (less than 2 per cent of requests), which, as far as the ABM is concerned, is evidence of a high level of consensus between couples and professionals with regard to what constitute ‘acceptable’ indications:
We find few differences between the opinions of CPDPNs and those of couples, as in 2007 CPDPNs refused only 112 attestations for 6,645 issued (1.7%) (ABM internal note, November 2009).
Furthermore, these refusals related to a limited number of indications that were identical in all centres (cleft lip, unilateral and partial agenesis of a limb, Klinefelter syndrome, and so on), which professionals in this field believe to illustrate the homogeneity of their practices:
The experiences of French multidisciplinary centres that submit annual reports on their activities to the Agence de la Biomédecine show that overall, throughout France, there is a high level of consensus on pathologies that are accepted without discussion (for MTPs). But there are also the same hesitations and ambiguities concerning pathologies that are seen as controversial and contestable and that are more or less the same for all teams (Fernand Daffos, foetal medicine specialist).Footnote 50
Yet is the homogeneity of indications for refusing MTP requests sufficient to assert the homogeneity of practices relating to MTP decisions? Upstream of a refusal, it is important to look at the space allowed for making a request. Are the conditions created for the expression of the possibility of having a MTP the same for all of the various CPDPNs, even when women come from different cultural backgrounds? Or will practitioners decide whether or not to open the door to discussions depending on their perception of the pathology, its consequences and their incorporate assumptions about women?Footnote 51 The following extract from a consultation with a migrant couple, following a foetal karyotyping, shows how the way in which the detected foetal pathology is presented to the couple cuts short any possibility of requesting a MTP:
Geneticist: we were worried that your baby had Down syndrome (
![]() $\ldots$
). He doesn’t have that at all, but he does have a small anomaly that is far less serious. We weren’t looking for it, but we found it. So I’m going to give you some information about it (
$\ldots$
). He doesn’t have that at all, but he does have a small anomaly that is far less serious. We weren’t looking for it, but we found it. So I’m going to give you some information about it (
![]() $\ldots$
). No malformation showed up on the ultrasound scan. Everything is fine. But we discovered something else that is a little unusual. Your baby has an extra chromosome. This causes problems, but they are not very serious. (
$\ldots$
). No malformation showed up on the ultrasound scan. Everything is fine. But we discovered something else that is a little unusual. Your baby has an extra chromosome. This causes problems, but they are not very serious. (
![]() $\ldots$
) It’s called Klinefelter syndrome. He’s a perfectly normal boy with normal genital organs, and as he grows everything will remain perfectly normal. A problem which may occur is that around the age of ten to twelve
$\ldots$
) It’s called Klinefelter syndrome. He’s a perfectly normal boy with normal genital organs, and as he grows everything will remain perfectly normal. A problem which may occur is that around the age of ten to twelve
![]() $\ldots$
(explanation about puberty). We’ll monitor him and he’ll become a man. He will be a man with a normal sex life, he will have sperm, but he won’t be able to have children normally (
$\ldots$
(explanation about puberty). We’ll monitor him and he’ll become a man. He will be a man with a normal sex life, he will have sperm, but he won’t be able to have children normally (
![]() $\ldots$
). Nowadays we can help (people with this condition) have children using laboratory techniques. Twenty years from now it will be even easier. So your son, he has problems, we’re not going to pretend everything is fine. He’ll need to be monitored and he’ll have problems having children. We know many people in this situation. It’s not particularly serious. Have I made the situation clear?
$\ldots$
). Nowadays we can help (people with this condition) have children using laboratory techniques. Twenty years from now it will be even easier. So your son, he has problems, we’re not going to pretend everything is fine. He’ll need to be monitored and he’ll have problems having children. We know many people in this situation. It’s not particularly serious. Have I made the situation clear?
Once the couple had left, the geneticist explained that there were ‘certain things’ she had not said, particularly the fact that statistically speaking Klinefelter boys have an IQ ten points lower than that of their siblings
![]() $.$
She added that in the CPDPN where she works, they no longer offer MTPs for Klinefelter syndrome, though they do sometimes accept requests, particularly where a couple has been given negative information by another practitioner.Footnote
52
The positive way in which the pathology is described is one of the elements likely to inhibit a request for an MTP. We might think that the geneticist is acting in a collective way. In trying to prevent any such request which would be embarrassing for the medical team, she is helping to strengthen the norms established in the centre. Whatever the case may be, while we might hypothesise that there are differences between CPDPNs regarding the space allowed to women to make MTP requests, their annual activity report does not allow us to verify this. These reports nevertheless provide interesting information.
$.$
She added that in the CPDPN where she works, they no longer offer MTPs for Klinefelter syndrome, though they do sometimes accept requests, particularly where a couple has been given negative information by another practitioner.Footnote
52
The positive way in which the pathology is described is one of the elements likely to inhibit a request for an MTP. We might think that the geneticist is acting in a collective way. In trying to prevent any such request which would be embarrassing for the medical team, she is helping to strengthen the norms established in the centre. Whatever the case may be, while we might hypothesise that there are differences between CPDPNs regarding the space allowed to women to make MTP requests, their annual activity report does not allow us to verify this. These reports nevertheless provide interesting information.
A comparative analysis of CPDPN activity is difficult to achieve as there is no common denominator that allows a comparison of the centres in terms of the number and indications of the MTPs that they annually perform. The volume of activity varies considerably from one centre to another and we cannot know the zones that each centre covers, as couples are free to contact the CPDPN of their choice. As I will come back to later, the number of case files discussed during multidisciplinary meetings also varies in accordance with different internal traditions.
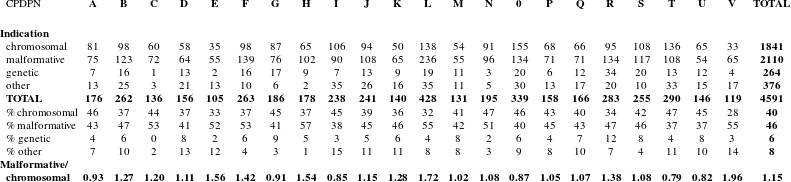
This said, the way in which the data are gathered makes it possible to get around this difficulty. Attestations authorising MTPs are recorded by type of original indication: chromosomal, genetic and malformative. The malformative indication category excludes those whose origin is known to be caused by a chromosome or gene. Table 1 shows the spread of indications for which MTP attestations were signed in 2009.Footnote 53 We can see that chromosomal and malformative anomalies account for 86 per cent of all attestations, yet each category has its own specificities. Chromosomal anomalies constitute the main core of routinised PND activity: they are stable within the population, homogeneous throughout the country, have been identifiable for a long time and in the vast majority of cases are the object of MTP authorisation. On the other hand, as I have observed, malformation is a blurred category, associated with suspicious images that are sometimes difficult to interpret and, even when there is no doubt, such as with an agenesis of the corpus callosum,Footnote 54 their functional consequences remain uncertain. We can assume that while there are indeed disparities between practices, they relate to uncertain situations, those located in the ‘grey area’ (to use the practitioners’ own term). For all of these reasons I felt it was reasonable to consider the number of diagnosed chromosomal anomalies as a common denominator that enabled comparison of the activity of the different centres.
Table 1 shows that, overall, there are slightly more MTPs for the malformation indication than for chromosomal anomaly: 46 per cent compared to 40 per cent; in other words, a ratio of 1.15. Yet if we compare centre indications, we find ratios that vary up to 100 per cent,Footnote 55 which suggests that PND practices are far from homogeneous. This suggests that differences in attitude between the centres in relation to the ‘malformation’ category might therefore reveal different practices regarding the way in which MTPs are approached and, more specifically, the space allowed to women to make a request. Different logics of action appear to continue despite the national regulatory framework designed to ensure homogeneity. To understand the reasons behind these different logics of action, the next section turns to the ethnographic observations of these practices through a case study of two centres.
Table 1: Number of attestations for medical termination of pregnancy issued in 2009, per type of medical indication. For reasons of comparability and robustness we only retained for analysis the prenatal diagnosis centres (CPDPNs) that issued one hundred or more medical terminations in 2009. In addition, with the exception of Paris, we combined the two centres of Lyon and Marseille into one.
3.2 Playing with the Regulatory Framework: Between Preservation and Commitment
My observations were made between 2010 and 2012 in a Paris centre and in a provincial centre. In each centre, I attended a large number of consultations with obstetricians, geneticists, sonographers, neonatologists and midwives, as well as the weekly meetings of the multidisciplinary teams. I also carried out interviews and was present during more informal moments of the practitioners’ work. All of the ethnographic material was transcribed and analysed using Grounded Theory and NVivo software.Footnote 56 Far from focusing solely on professional attitudes towards MTPs, the comparative analysis looked more broadly at how each centre organised its practices so as to conform to the new regulatory requirements.
The two CPDPNs present certain similarities. Both were located in university hospitals, which places them at the cutting edge of new technologies and research in PND. They both had a high volume of activity, with over 200 MTP attestations issued in 2009. Both centres had experience with collegial work well before the law on bioethics came into effect.Footnote 57 At the time of the fieldwork, the multidisciplinary team met every week to discuss a certain number of cases of suspected or diagnosed foetal pathologies, to make a decision concerning additional tests to be done or to envisage the possibility of an MTP. Both teams were coordinated by men who were heads of department within the hospital hierarchy – an obstetrician for the Paris centre and a geneticist for the provincial centre.Footnote 58 Their populations differed, however, with the Paris centre dealing with a larger number of women from poorer backgrounds, most of whom were immigrants. This is an important point. As with Rayna Rapp in New York,Footnote 59 I observed that practitioners’ attitudes differ in line with their presuppositions concerning women’s language skills, level of education, religious beliefs and understanding of the law on abortion. The Paris centre issued more authorisations for malformative pathologies and refused fewer MTPs than the provincial centre.Footnote 60
My comparative analysis reveals differences between the centres that illustrate the attitudes of the practitioners towards the recommendations and regulations that they were required to follow, and sheds light on the heterogeneity of practices. The differences relate to the way the teams organised their everyday work, how they discussed the cases put before them during staff meetings and approached the MTP issue.
3.3 Organisation of the Teams’ Work
In the Paris centre, conformity to the regulatory framework was achieved in such a way as to modify as little as possible the centre’s historical practices by exercising complete control of the format of meetings and by containing discussions in space and time. The desire for efficiency predominated, aided by strict hierarchical relations. Staff activity was centralised and formalised. Two midwives were dedicated full-time to preparing the multidisciplinary meetings. They collected the files, asked for any missing information, prepared a slide show of all the cases to be presented, in accordance with a standard model, and sent all of this by email to all participants prior to the meeting.
While regulations govern the composition of the teams and have increased the number of participants, including participants from outside the hospital, staff meetings were organised in such a way as to maintain a certain level of intimacy. The room in which they took place was isolated. The participants – practitioners from the multidisciplinary team, along with others from maternity units associated with the CPDPN if one of their patients is to be discussed – gathered in a small amphitheatre which may only be accessed by personnel with a badge. At the bottom of the amphitheatre, in the middle of the platform, sat the coordinator, surrounded by the department secretary, who took notes, one of the CPDPN’s two midwives, who had stacked in front of her the pile of files to be discussed, and finally the clinical assistant, who presented all of the cases out loud. On the opposite side of the boss was the consultant sonographer in front of an overhead projector and, next to her, the MRI specialist. They each commented on all of the imaging that was projected onto the large screen behind the platform. Aside from a few key personnel who felt that they could legitimately interject with spontaneous comments, the majority of participants in the room only spoke when the coordinator invited them to do so. Prior to each team meeting, the files were organised by medical specialty and presented in order of specialty, thus allowing the relevant specialists to leave the room and others to come in later. Once again for reasons of efficiency, before the weekly meeting there was a ‘pre-staff meeting’ during which the case files were selected so that only those that were subject to a regulatory obligation, sometimes interpreted relatively loosely, were presented at the weekly meeting.
The provincial centre had seized upon the regulatory obligation as an opportunity to create cohesion in practices that were dispersed not only between the public and private sectors, but also geographically. In contrast to the Paris centre, many of the team members divided their time between sessions at the hospital and freelance activity. Multidisciplinary meetings thus included specialists from both the public and private sectors. The stronger heterogeneity of the participants went some way towards explaining why, regulatory mission aside, the staff meetings had a combined function of socialisation and training student midwives (in particular). This is also why the discussions were not limited to cases subject to a legal obligation, but could also include any other situation that a practitioner might wish to discuss with his/her peers.
Another important particularity of the provincial centre was the geographical dispersion of its associated maternity units, some of which were as far as 150 km away. This problem was solved through a videoconferencing system that may be simultaneously used by up to five peripheral entities, in which one, two or three practitioners could join for all or part of a staff meeting. Speaking time was thus divided between the centre and the peripheral entities. The result was that unlike the ‘between ourselves’ situation that prevailed in the Paris centre, the contours of the multidisciplinary meetings held by the provincial centre were variable and uncertain.
The way staff meetings were organised was friendlier and less formal than in the Paris centre. They took place in a room that was barely large enough to hold all of the participants. The latter came together around a large table (for the first to arrive) and in a second circle for the remainder. The coordinator always sat in the same position with, on his left, the secretary who notified the decisions and, on his right, a geneticist who replaced him should the need arise. The number and nature of the case files to be presented were not known in advance, with each practitioner bringing his/her file(s) on the day of the meeting; some of them showed slides, but this was not systematic. There was no particular order of presentation. Practitioners entered and left the room in a haphazard fashion, in accordance with their availability, so it was not unusual for a given patient’s case to be brought up at different moments during the meeting, by specialists who were not all present at the same time.
So, while the regulatory framework introduced in the 1990s and 2000s affected the number of members and composition of the teams, as well as the nature of the case to be presented – in particular by requiring that all indications that might give rise to an MTP be the object of collective discussionFootnote 61 – these formal changes had little impact on the work organisation of the teams created beforehand, with full autonomy and wish to maintain their traditions. Yet this practical configuration of staff meetings was not without consequence for the form and content of the discussions that took place therein.
3.4 Deliberations and the Decision-making Process
The substance of the discussions that took place during the weekly multidisciplinary meetings also reveals marked differences in the way in which the practitioners at the two centres adjusted their practices to comply with the regulatory framework. I will focus on two aspects that emerge from the comparative analysis: ways of talking about MTPs and perception of the risk of anomaly, both of which illustrate how the actors accommodate the rules and thus sustain the heterogeneity of their practices.
4 MTPs: How Were They Discussed?
In the Paris centre, the practitioners openly and very directly discussed the possibility of a MTP. This attitude was based on a strongly held historical position, deemed by the centre’s practitioners to be a specificity of their practices, even though it was in tension with the principle of non-directiveness recommended in the guidelines:Footnote 62
Coordinator: When we meet the parents, and it’s a serious case, (
![]() $\ldots$
) we suggest, we tell them it’s serious and that they can terminate the pregnancy. Under normal circumstances it is up to them to ask, but in this case we suggest it. We follow the line laid down by my predecessor, who I knew well and with whom I had a good relationship. We tell them ‘it’s your decision’. If they wish to keep the baby, we tell them we will look after it and we advise them. But we make the suggestion. I have colleagues who say that’s not good, that it should be left to the parents to ask. We’re the only ones who do that. It’s specific to us.
$\ldots$
) we suggest, we tell them it’s serious and that they can terminate the pregnancy. Under normal circumstances it is up to them to ask, but in this case we suggest it. We follow the line laid down by my predecessor, who I knew well and with whom I had a good relationship. We tell them ‘it’s your decision’. If they wish to keep the baby, we tell them we will look after it and we advise them. But we make the suggestion. I have colleagues who say that’s not good, that it should be left to the parents to ask. We’re the only ones who do that. It’s specific to us.
This tradition was established by the previous head of department, who had introduced collegial meetings in the early 1980s and who ‘believed that it was not down to the parents to bear the guilt of killing their child’, according to the current department’s supervisor. This point of view dominated the field of perinatal care, particularly regarding decisions to cease care for very premature infants.Footnote 63
It governed the Paris centre’s multidisciplinary discussions, adding an additional degree of freedom to the decision-making process. Whenever a serious pathology was diagnosed, or when a risk was deemed to be serious, the issue was whether or not a MTP should be suggested. A sort of implicit three-point scale had been established: there were some indications for which the practitioners suggested to the woman/couple that a MTP be performed; other indications for which they accepted if the woman made the request; and still others for which they refused.
In the following extract, consensus was sought to qualify the case of a foetus at thirty weeks of amenorrhea that presented several malformations that were not life-threatening and did not affect the brain. A chromosomal anomaly (inversion of the third chromosome) was discovered. Should a MTP be suggested, or not?
Coordinator: What do we suggest to parents with a Fallot, an intrauterine growth retardation, a single kidney?
Geneticist 1: I wouldn’t be shocked if we suggested termination.
Coordinator: If it is a de novo (there is no other case of the chromosomal anomaly in the family), then we must suggest a termination. Is the risk high enough to suggest a MTP?
Geneticist 2: There are VACTERLs [acronym for this type of syndrome] who are fine.
Coordinator: So we need to complete the diagnosis.
Geneticist 2: Give us a week.
Coordinator: If the parents want a MTP, we’ll accept and we’ll do the tests after.
In the provincial centre, the question of pregnancy termination was far less frequently discussed during team meetings. They made decisions on the gravity of the pathology, as required by the recommendations, and when there was no doubt that the foetus was suffering from a serious pathology, this was notified in the report using standard wording that reflected the terms of the law authorising MTPs. In such situations, if the couple so requested, termination was accepted.
When the possibility of an abortion was expressed, it was done so with some restraint, usually in a euphemistic form which was in contrast with the head-on approach of the Paris centre. The practitioners used roundabout phrasing such as: ‘What are the parents’ thoughts at this time?’ or ‘What is the woman tending towards?’ Once it had been accepted that the pathology fell within the parameters defined by the law, the practitioners might consider the wishes of the woman or couple:
Coordinator: This is such a worrying intrauterine growth retardation that we must ask whether it is a situation with a high risk of a seriously debilitating anomaly that justifies a MTP, with the additional anomaly of the genital organs.
Sonographer: The (growth) curve is far below the third percentile. The cranial perimeter is more or less protected. It is difficult to estimate foetal weight under these conditions.
Coordinator: Is she asking for a termination?
Sonographer: She’s worried, she hasn’t asked, but she is aware that the question may arise. We need to give her the information.
One of the meetings I observed was especially useful in clarifying the attitudes adopted in the provincial centre, due to the presence of a new head of department. After discussing the case, and faced with a severe pathology, the coordinator announced the verdict, which was noted by the secretary:
Coordinator: Affection with a high risk of being seriously debilitating and incurable. Indication of karyotyping in the etiological report.
New participant: At what point do you talk about termination of pregnancy? Are you envisaging a MTP?
Coordinator: We put ‘high-risk affection’ in the report. The obstetrician has the arguments.
The reply was cryptic and demonstrates the coordinator’s wish to go no further than his responsibility to state the seriousness of the anomaly and its incurability. In the intimacy of the doctor–patient encounter, the obstetrician was free to act as he/she saw fit. My observations nevertheless show that at the provincial centre the practitioners tended to adopt a wait-and-see attitude, to observe the couple’s thought process, and tried to respect the principle of non-directiveness. Yet the way staff meetings were configured, not allowing people to know who was present when they were speaking, tended to cause discussions to be ‘smoothed over’, something that was very different from the direct and sometimes even crude exchanges observed in the intimacy of the Paris centre.
5 Uncertainty and Disability Tolerance
French PND practitioners had made the most of the wiggle room available in their interpretation of the law authorising MTPs, to define the boundaries of the new professional specialism of foetal medicine.Footnote 64 Legislators, in turn, had left them free to decide upon the ‘strong probability’, ‘particular gravity’ and ‘incurability’ of the foetal pathologies they encountered. While these criteria were at the heart of the deliberations, generally speaking doctors agreed on the acceptability of certain risks. ‘Curability’ in particular was often assessed in terms of the surgical techniques available. If early surgery could repair an anomaly, it must be attempted. This was the case for isolated diaphragmatic hernias, which could be operated on in the days following birth with, according to practitioners I observed, a 50 per cent chance of survival. Unless there were complications, termination of pregnancy was not envisaged in such cases. Taking this risk helped to improve surgical techniques. This was particularly the case for the transposition of the great heart vessels. Nowadays 95 per cent of new-born babies survive the operation.Footnote 65 Twenty years ago, 20 per cent died and 20 per cent suffered from complications due to a lack of oxygen.Footnote 66 If they were not too major, morphological malformations (such as an agenesis of the hand, for example) were deemed acceptable by practitioners. There was of course disability, but children (in their own opinion) successfully overcame this.Footnote 67 On the other hand, failure to identify a ‘polymalformative syndrome’, generally associated with mental retardation, remain a common fear, illustrating a form of historical continuity between PND practices and eugenics.Footnote 68 While medical imaging was able to detect an increasing number of anomalies, its ever-improving performances also generated more uncertainty.Footnote 69 As I frequently observed during the ultrasound consultations and staff meeting discussions, every suspicious image led to fear that there was a malformative pathology. Discussing whether it was an artefact, a ‘variant of the normal’, an irrelevant particularity or a sign that fit the description of a known syndrome, practitioners tried to bridge the gap between pre-screening and post-screening knowledge.Footnote 70 The latter hypothesis was generally prioritised and practitioners then strove to find other related signs that would allow them to reject or confirm.
Even when a diagnosis had been made, the consequences in terms of disability sometimes remained very uncertain, because for some anomalies the spectrum of clinical manifestations could be very broad.Footnote 71 A typical case for the study of an ‘acceptable’ and ultimately frequent risk was the agenesis of the corpus callosum, the part of the brain that links the two cerebral hemispheres.Footnote 72 Whether partial or total, in 50 per cent of cases it is linked to other signs and belongs to a potentially severe clinical table. In the remaining 50 per cent of cases it is isolated and may have no consequences.Footnote 73 Diagnosis was difficult; it was achieved through imaging from eighteen weeks of amenorrhea, but could only be definitively established by an MRI at thirty-two weeks of amenorrhea. Practices had for a long time been based on studies showing that a significant proportion of children without corpus callosum had moderate to severe mental retardation. Yet a most recent study conducted by Marie-Laure Moutard, a French paediatric neurologist who monitored a cohort of children with an agenesis of the corpus callosum, shows that in one-fifth to one-quarter of cases the children presented a moderate to severe intellectual deficit and that in three-quarters of cases their IQ was normal or very slightly below average.Footnote 74 The discovery of an agenesis of the corpus callosum plunged those involved into considerable uncertainty, which was a source of anxiety for couples who might then be tempted to ask for a MTP without waiting for the definitive diagnosis. In this case, the indication was recorded in the ‘malformation’ category. In both centres, I was able to observe several discussions on the conduct to follow when facing such a situation.
Once again, the two extracts from these observations illustrate different ways of managing uncertainty and apprehending the risk relating to the consequences of the anomaly. In the Paris centre, a partial agenesis of the corpus callosum was discovered at twenty-four weeks of amenorrhea:
Coordinator: X [sonographer] is wondering if there’s an agenesis of the posterior corpus callosum. We must nevertheless offer a karyotype and virus test (it is a question of eliminating an anomaly linked to a syndrome).
Geneticist: I don’t know, but we felt that as a prognosis a partial agenesis was no better than a complete agenesis! We need the neurologist’s opinion (absent that day). We are pretty much convinced that he’ll suggest a termination. That’s what he’s proposed more than once in this type of case, so we need him to give his opinion, to meet her before we reach twenty-two weeks.
The exchange shows that practitioners did not wish to take the risk of mental retardation, whatever the extent might be. In Paris, the risk of mental retardation frequently cropped up in discussions as a decisive argument for the action to be taken: to ‘suggest’ a MTP or to wait for the woman to request one. The provincial centre, in comparison, used more neutral terms:
Coordinator: It’s an isolated complete agenesis of the corpus callosum. We need to provide full information. Many of these children are fine. If the parents ask for a medical termination, we accept. That’s the attitude of Marie-Laure Moutard who monitors these children over the long term. The results are reassuring but don’t give us enough information to be able to refuse (an MTP) for these indications.
So if the woman asked for it, her wish would be granted. Returning to her case a little later, he added: ‘In 60 per cent of cases we don’t know what to do with a corpus callosum that is short and thick. We perform MTPs, which are associated with uncertainty. I suggest a midway recommendation: a diagnostic ultrasound.’
The provincial centre’s coordinator based himself on the existing state of medical and scientific knowledge to assess the uncertainty. According to established tradition, he transmitted this information to young trainee practitioners. He argued for a careful wait-and-see attitude, but would respect the woman’s autonomy, following the recommendations on good practice.
6 Discussion
My observations in the two CPDPNs show that despite the government’s determination to control practices, French PND practitioners at the centres conserved a level of relative autonomy. The Paris centre did its best to limit the impact of the new regulations on its practices. Its firm control of its PND-related activities allowed it to restrain the time spent, and the fact that meetings took place behind closed doors allowed people to speak more freely during discussions. Without taking too much risk, the practitioners continued to adhere to their locally specific culture by suggesting an abortion when a foetal pathology was deemed to be severe, even if this might appear debatable under the new standards of non-directiveness. Conversely, the provincial centre was engaged in the reform movement and clearly demonstrated its adherence to the new regulatory framework; using it to encourage and strengthen the links between professionals across divides of status and geography. On the other hand, the fact that meetings were more accessible meant that care must have been taken during discussions and probably limited their scope.
These differences shed light on the attitudes towards MTP authorisations observed at the macrosocial level. The directive attitude taken in the Paris centre (considered a hallmark), which was to explicitly propose an MTP, demonstrates their resistance to the movement – clearly described by historians of human geneticsFootnote 75 – that involved transferring responsibility for decisions relating to reproduction to women and families, while respecting their autonomy. This does not mean that practitioners at the Paris centre explicitly took collective responsibility for the prevention of disability, as was the case in the USA in the 1950s.Footnote 76 Here the motive was individual. Some were to see this as the persistence of a form of paternalism designed to unburden women from the guilt of having to decide on the death of the child they were carrying. In any event, this attitude necessarily worked in favour of an MTP being performed. The mechanism – whether this avoided any inhibition that couples may have had about raising the issue themselves, or whether the latter perceived this, from a normative standpoint, as being the correct thing to do – nevertheless remains unclear.
The attitude at the provincial centre, on the other hand, was to provide couples with detailed information on the situation without ever bringing their subjectivity into play, and then to wait for the couples to make their request before discussing with them the possibility of terminating the pregnancy. Here, responsibility for decision-making falls to the women and couples. Such an attitude tends to reduce the number of MTPs performed, as a couple may have envisaged such a possibility without daring to put it into words.
Moreover, my ethnographic observations show a persistent aversion on the part of practitioners regarding the risk of mental deficiency. This is embedded in a historical continuity with eugenics, the ideas and practices of which related more to intelligence than to physical health.Footnote 77 Although it varies in extent from one centre to another, the fear of ‘missing’ a malformation that might be the cause of a mental deficiency continues to have a strong impact on how practices are oriented.Footnote 78
This trend could be reinforced by rapid developments in comparative genomic techniques such as CGH Array (Comparative Genomic Hybridisation). These techniques are more efficient than karyotyping, since they allow the automated detection of chromosomal micro-deletions and micro-duplications potentially responsible for learning disability and dysmorphic features.Footnote 79 First used in genetic counselling, following an in utero death or MTP, this technique, by obtaining faster and faster results, represented a new resource for prenatal diagnosis. This tool was beginning to be used, in the Parisian centre where I carried out my fieldwork, for cases of foetal malformations identified through ultrasound and of unknown origin.
As we have seen, French regulation of practices, to which practitioners had themselves made a considerable contribution, leaves sufficient latitude for each centre to be able to forge its own identity, in a collegial manner. This latitude could be seen first and foremost in their assessments of the ‘strong probability’, ‘particular gravity’ or ‘incurability’ of the foetal pathologies encountered. The decision on what constituted an acceptable risk varied from one centre to the other. The official discourses that put forward the homogeneous nature of practices in France in fact hide a certain known and accepted latitude for decision-making in the centres relative to situations that might be deemed less severe or surgically ‘reparable’. The latitude shown by the practitioners could also be seen in the way they ‘played’ with the standards and regulations. Each centre was trying to maintain autonomy for the aspects that suited its traditions and values, thus building its own unique identity. In the professional arena, certain centres had forged a reputation of permissiveness; their attitude demonstrated empathy and benevolence towards couples, underlying the suffering that families and children endured when coping with a disability in a normative society. Others would seem to have positioned themselves more as guardians against excessive practices; defending the value of life, they were challenging the boundaries of normality. These values, which used to cause conflict between individuals or specialisations,Footnote 80 would seem to have migrated towards collective bodies: the CPDPNs.
While it had not created any real homogeneity in practices, the new framework, in particular the obligation to collectively discuss decisions and to account for one’s activity, had led to a major change in practices for everyone concerned. Decision-making had de facto been removed from the doctor–patient encounter and took place in teams; and the latitude allowed to practitioners was no longer individual, but collective. The differences between the centres seem to demonstrate, within the regulatory and standardised framework proper to ‘therapeutic modernity’, the capacity of foetal medicine to preserve the varying sensibilities that have traversed its history. The identities of the centres, which have been developed over the long term under the influence of charismatic leaders, have replaced what used to be personal standpoints. Hence the non-mainstream attitude of the Paris centre, might find legitimacy in its rejection of a logic of choice that was based on the modern Western conception of a rational, responsible and autonomous individual,Footnote 81 and was particularly unsuited to the women from underprivileged and often migrant backgrounds who made up the majority of its patients. As for the form of discussions in the provincial centre, it may well stem from a strategy to protect practitioners who, with no safety net, gave their opinions in an open space over whose boundaries they had no control.
The law has taken the differences between centres into account; it is not designed to require all practitioners to share the same sensitivities and opinions. It states that ‘each CPDPN is responsible for its own opinions and maintains its autonomy of assessment’ – with women being able to ask another centre in cases where an MTP is refused.Footnote 82
Yet while the preservation of a centre’s autonomy would appear to explain differences (that vary by a factor of almost two) in the number of MTP authorisations for an indication of foetal malformation, it is interesting to note the minimal impact that these differences have with regard to the population as a whole. Indeed, compared to other regions of Europe, PND practices in France are extremely effective. The detection rate of Down syndrome is among the highest, as is the proportion of affected fœtuses aborted.Footnote
83
Above and beyond the medical, scientific and technical skills of the practitioners, this is due to the efficiency of the health system insurance in France. The autonomy of the centres, like that of the women and couples, while it respects singular choices, does not hinder – or even helps – the propagation of a ‘new eugenics’ that is unrestrictive, ‘pro-choice, gentle, liberal and democratic’.Footnote
84
In this situation, it was not necessary to impose homogeneous practices on practitioners, or direct women’s decisions. To explain this phenomenon, the concept of biological citizenship is here useful. It could be applied to both couples and practitioners and is conceived of as being ‘modes of subjectification in individuals
![]() $\ldots$
(that) can be explained as individual way of internalising the discourse of life and health, thereby acting responsibly in relation to questions about life and health’.Footnote
85
$\ldots$
(that) can be explained as individual way of internalising the discourse of life and health, thereby acting responsibly in relation to questions about life and health’.Footnote
85




