Clinicians, policy makers, and researchers increasingly recognize the importance of quality of life (QoL) as a health outcome in residents of long-term care (LTC) facilities (Burack, Weiner, Reinhardt, & Annunziato, Reference Burack, Weiner, Reinhardt and Annunziato2012; Carr & Higginson, Reference Carr and Higginson2001; Kane, Reference Kane2001; Kanwar et al., Reference Kanwar, Singh, Lennon, Ghanta, McNallan and Roger2013). QoL is associated with health status and physical and cognitive functioning (Abrahamson, Clark, Perkins, & Arling, Reference Abrahamson, Clark, Perkins and Arling2012; Abrahamson et al., Reference Abrahamson, Lewis, Perkins, Clark, Nazir and Arling2013; Andersen, Wittrup-Jensen, Lolk, Andersen, & Kragh-Sørensen, Reference Andersen, Wittrup-Jensen, Lolk, Andersen and Kragh-Sørensen2004; Degenholtz, Rosen, Castle, Mittal, & Liu, Reference Degenholtz, Rosen, Castle, Mittal and Liu2008; Drageset et al., Reference Drageset, Natvig, Eide, Bondevik, Nortvedt and Nygaard2009); autonomy and self-determination (Duncan-Myers & Huebner, Reference Duncan-Myers and Huebner2000; Lachapelle et al., Reference Lachapelle, Wehmeyer, Haelewyck, Courbois, Keith and Schalock2005); and social engagement and support (Degenholtz, Kane, Kane, Bershadsky, & Kling, Reference Degenholtz, Kane, Kane, Bershadsky and Kling2006; Kuehner & Buerger, Reference Kuehner and Buerger2005). Quality of life is also affected by organizational factors, such as staffing levels, stability, and leadership (Castle & Engberg, Reference Castle and Engberg2006; Castle & Engberg, Reference Castle and Engberg2008; Chaneb, Reference Chaneb2008).
Canada’s aging population will create greater demands for LTC services, including admission into LTC facilities (Kanwar et al., Reference Kanwar, Singh, Lennon, Ghanta, McNallan and Roger2013). Admission to LTC facilities may be a disempowering experience for residents due to their increasing dependence on facility staff for all aspects of their care (Tu, Wang, & Yeh, Reference Tu, Wang and Yeh2006). Current cultural transformation initiatives in LTC facilities have already become evident (Koren, Reference Koren2010; White-Chu, Graves, Godfrey, Bonner, & Sloane, Reference White-Chu, Graves, Godfrey, Bonner and Sloane2009). Institution-like models of care are being transformed into “nurturing environments that are person-directed” (Burack et al., Reference Burack, Weiner, Reinhardt and Annunziato2012). Such change is in part due to shifts in government policy and regulatory mechanisms placing greater emphasis on resident outcomes, including QoL, as well as unremitting advocacy efforts (Koren, Reference Koren2010; White-Chu et al., Reference White-Chu, Graves, Godfrey, Bonner and Sloane2009). These advocacy actions, combined with the lived experience of vocal residents, have helped shape the content (what is provided), process (how it is provided), and outcomes of residents’ care, including their QoL. These actions will add increasing support to the cultural movement in LTC for more home-like environments, person-centred care, and practices where personal autonomy and decision making drive the transformation of residents’ care from a medical to a more consumer-directed model (Robinson & Reinhard, Reference Robinson and Reinhard2009). Person-centred care emphasizes “maintaining personhood in spite of declining cognitive ability, striving to take the viewpoint of the patient, acknowledging personal experiences of life and relationships and including the social environment as a therapeutic agent” (Edvardsson, Koch, & Nay, Reference Edvardsson, Koch and Nay2010, p. 55). Person-centred care revolves around residents’ personal and individualized experience and emphasizes relationships and communication (Savundranayagam, Reference Savundranayagam2012). Consideration of residents’ self-reported QoL as a measure of their experience in the LTC facility would make a vital contribution to the successful implementation of person-centred care in LTC facilities.
As QoL is a complex, multifaceted, and subjective concept, clinicians and researchers might rely upon several sources of information for assessing the QoL of residents in LTC facilities. There is growing support that a direct assessment of residents’ perception of QoL is preferred due to its subjective nature. As an individual’s subjective world is idiosyncratic, it is not directly understood by others, even by close relatives. Direct measurement of QoL is also preferable to using external predictors (Degenholtz et al., Reference Degenholtz, Kane, Kane, Bershadsky and Kling2006) or proxy sources (Kane et al., Reference Kane, Kane, Bershadsky, Degenholtz, Kling and Totten2005). Individuals with moderate dementia and associated cognitive impairment are still able to report on their QoL, even when they have poor insight into and awareness of their dementia (Gerritsen, Steverink, Ooms, de Vet, & Ribbe, Reference Gerritsen, Steverink, Ooms, de Vet and Ribbe2007; Logsdon, Gibbons, McCurry, & Teri, Reference Logsdon, Gibbons, McCurry and Teri2002; Novella et al., Reference Novella, Jochum, Jolly, Morrone, Ankri and Bureau2001). It is estimated that 60 per cent of the residents would be able to reliably report on their QoL (Kane, Reference Kane2003). Thus, self-reports may be regarded as the “gold standard” approach to evaluating QoL.
Yet, despite an increased interest in the topic, there is relatively little research on residents’ self-reported QoL. The primary purpose of this study was to examine the self-reported QoL of LTC facility residents in Canada using the interRAI Self-Report Nursing Home Quality of Life Survey instrument. A secondary purpose is to test the instrument’s psychometric properties. This study will contribute to the cultural transformation efforts in LTC facilities by measuring QoL purely from the perspective of residents. It will also guide the development of evidence-informed clinical practice for making decisions about appropriate resident-directed interventions (Gerritsen et al., Reference Gerritsen, Steverink, Ooms, de Vet and Ribbe2007; Varricchio & Ferrans, Reference Varricchio and Ferrans2010). This study may also contribute to shaping public policy in mobilizing person-centred models of care in LTC facilities (McGilton et al., Reference McGilton, Heath, Chu, Boström, Mueller and Boscart2012).
Methods
Design and Settings
This was a cross-sectional, descriptive study of a convenience sample of 928 residents from 48 volunteer LTC facilities in the Canadian provinces of Alberta, British Columbia, Manitoba, Nova Scotia, Ontario, and Saskatchewan. While most of the participating LTC facilities were recruited by the researcher, a small number of facilities that became aware of the study volunteered to participate. In Ontario, an advertisement was placed in the electronic newsletters of the Ontario Long Term Care Association and the Ontario Association of Non-Profit Homes and Services. Other facilities self-initiated contact with the researcher upon learning of the study from others. A recruitment letter was prepared and e-mailed to those who expressed an interest. Overall, a convenience sample of 48 LTC facilities volunteered to participate within the recruitment timeframe of the study.
Ethics
This study received full ethics clearance from the Office of Research Ethics, University of Waterloo. While some LTC facilities obtained their own research ethics clearance using internal mechanisms, most accepted the University of Waterloo’s ethics clearance in lieu of conducting their own ethics review. The Office of Research Ethics also gave clearance to the training program for surveyors and LTC facility staff, which was specifically designed for this study.
Training of Surveyors and LTC Facility Representatives
Long-term care facilities designated potential surveyors who were to interview residents in their respective facilities. The designated surveyors did not need to have any professional credentials, except for the following, which were deemed as necessary qualities: (1) good interpersonal and communication skills, (2) ability to establish good rapport with residents, and (3) ability to put residents at ease.
The primary author provided the training program to the designated surveyors and LTC facility representatives through a series of webinar sessions. The training included a description of the scope and nature of the QoL study, the procedure for recruiting potential residents and obtaining informed consent, methods to conduct interviews without influencing residents’ responses, and instructions on completing the interRAI QoL Survey form. One essential rule that was stressed to the surveyors was that they could not conduct interviews with residents who depended on them for their personal or clinical care. A registry of the names of trained surveyors, their credentials, and their position in the LTC facility was developed. In addition to the training, a dedicated project website was developed where surveyors and LTC facility representatives could access all information relevant to the QoL study project, including the training material.
Criteria for Inclusion of LTC Facility and Resident Participants
LTC facilities were included in the study if they had been using interRAI’s Resident Assessment Instrument – Minimum Data Set 2.0 (RAI-MDS 2.0) (www.interRAI.org) for at least one year to allow for full and quarterly assessments. LTC facilities also had to provide a written consent for participation in the study and for researchers to have access to RAI-MDS 2.0 data.
Residents were included if they met the following criteria: (1) ability to communicate in English, (2) having a complete RAI-MDS assessment, and (3) a Cognitive Performance Scale (CPS)Footnote 1 score between 0 (intact) and 3 (moderate impairment) (Morris, Fries, Mehr, & Hawes, Reference Morris, Fries, Mehr and Hawes1994). The choice of CPS scores between 0 and 3 was made deliberately in recognition that some residents with mild to moderate cognitive impairments may be able to self-report on their QoL (Kane et al., Reference Kane, Kling, Bershadsky, Kane, Giles and Degenholtz2003; Logsdon et al., Reference Logsdon, Gibbons, McCurry and Teri2002).
LTC facility RAI coordinators first identified potential residents who met these inclusion criteria. Next, trained LTC facility staff most familiar with the residents explained the purpose of the study using a script provided with the training materials. Residents who agreed to participate signed the study consent form. Of the 1,828 residents who were originally approached, 55 per cent (n = 1,008) agreed to participate. However, of those who agreed to participate, only 928 were able to complete the QoL interview (completion rate = 51%). Anecdotal reports of reasons for the inability to complete included “fatigue”, “changed my mind”, and “needed a break”.
Source of Resident and LTC Facility Profiles
The RAI-MDS 2.0 was the source for data on residents’ socio-demographic and clinical characteristics. In Canada, RAI-MDS has been implemented for use in LTC facilities in seven provinces (Alberta, British Columbia, Manitoba, Newfoundland, Nova Scotia, Ontario, Saskatchewan), and the Yukon Territory. Of the six provinces that agreed to participate in this study, only Manitoba, Nova Scotia, and Ontario submit RAI-MDS 2.0 data to the Canadian Institute for Health Information (CIHI), which is a repository for health data from all health sectors, including RAI-MDS data from LTC facilities. Accordingly, three primary sources for the RAI-MDS 2.0 data were used: (1) CIHI for Manitoba, Nova Scotia, and Ontario; (2) provincial health authorities for Alberta and Saskatchewan; and (3) LTC facilities in British Columbia.
Measurement of QoL
The interRAI QoL Survey instrument (Morris, Reference Morris2009) consists of 50 items grouped under 10 domains with four to six items in each domain (see Table 5). These domains include privacy, food/meal, safety/security, comfort, making daily decisions (autonomy), respect, responsive staff, staff-resident bonding, activity option, and personal relationships (presence of friends). The 10 domains reflect items from Maslow’s (Reference Maslow1962) hierarchy of human needs, such as physiological needs (e.g., food, comfort), safety (e.g., freedom from harm), love (e.g., affection, meaningful relations), esteem (e.g., being appreciated by others), and self-actualization (e.g., self-fulfillment, learning). These domains and items describe various aspects of QoL that have substantial relevance to LTC facility residents and allow for the comprehensive assessment of their experience in an LTC facility.
The choice of the interRAI QoL Survey instrument was supported by several factors. The instrument is a companion to interRAI’s suite of assessment instruments comprising an integrated health information system (Gray et al., Reference Gray, Berg, Fries, Henrard, Hirdes and Steel2009; Hirdes et al., Reference Hirdes, Fries, Morris, Steel, Mor and Frijters1999). The research team designing the QoL instrument included collaborators from several countries, making the construction of the instrument’s items sensitive to cultural considerations. Another consideration was the instrument’s comprehensive content, which is a necessary element in the design of assessment instruments (Fayers & Machin, Reference Fayers and Machin2007). In addition, the instrument includes a global dispositional measure, “I tend to be happier than most other people”, which can be used as a “risk adjuster” to account for personality differences in QoL ratings (see, for example Stones et al., Reference Stones, Kozma, Hirdes, Gold, Arbuckle and Kolopack1996). Another item, “I would recommend this site or organization to others”, is considered a proxy measure for overall QoL rating, which is also desirable in the design of QoL instruments.
The interRAI QoL Survey instrument has a 5-point ordinal scale with response categories: (0) Never, (1) Rarely, (2) Sometimes, (3) Most of the time, and (4) Always. Participants also have the option of a “Don’t know” (6) response. In addition to these participant responses, surveyors may also use “Refused” (7) or “No response or cannot be coded from response” (8) codes as appropriate. Response categories 6, 7, and 8 were recoded as “Sometimes” with a value of 2 (Fayers & Machin, Reference Fayers and Machin2007). This recoding avoided the more extreme values (0, 1, 3, 4) and was also used in the pilot study of the interRAI QoL Survey instrument in Boston, Massachusetts, with acceptable results (Morris, Reference Morris2009). Thus, in calculating residents’ QoL scores, only ratings on the 5-point (0 to 4) scale were used. Two levels of scores were calculated: a domain-specific score, and an overall aggregate score for the whole instrument. To compute residents’ overall QoL scores, 49 of the 50 items included in the 10 domains were used. The global dispositional item was not included in the calculation of the overall QoL score. This item was used to examine the psychometric properties of the interRAI QoL Survey instrument, which will be discussed later in this article.
Procedure for Assessing Residents’ QoL
Resident interviews by trained surveyors were conducted between March and June 2010. Residents were interviewed in a manner that was sensitive to their comfort and privacy. A total of 103 surveyors were involved, including 68 per cent management staff, students, and volunteers; 22.3 per cent paraprofessionals (e.g., social workers, recreation staff, pastoral care); and 9.7 per cent registered nursing staff and personal support workers.
To help residents through the interview process and cue them to the possible response options, we provided them with a large-print copy of the six possible response options (ratings 0 to 4, plus “don’t know”) (Bradburn, Sudman, & Wansink, Reference Bradburn, Sudman and Wansink2004). Surveyors recorded residents’ responses on a scannable copy of the interRAI QoL Survey. Interviews were expected to be about 30–40 minutes in length, subject to residents’ comfort and preferences. Anecdotal reports received from surveyors confirmed completion of interviews within this timeframe with a few exceptions.
Each completed interRAI QoL Survey was reviewed for completeness, electronically scanned to generate an electronic data file, and assigned a unique study identification number for anonymity and confidentiality.
Data Analyses
Descriptive analyses were performed using SAS software, version 9.2 (SAS Institute Inc., 2002–2003). The distributional properties of resident and facility characteristics and residents’ self-reported QoL ratings were examined using frequencies, percentages, means, and standard deviations. The distribution of surveyors’ position in LTC facilities was examined to determine if their position had any influence on residents’ self-reported QoL ratings. Frequencies, percentages, overall mean QoL scores, and 95 per cent confidence intervals were calculated.
Two specific tests were conducted to establish the interRAI QoL Survey instrument’s reliability: test-retest and internal consistency. To establish the stability of the instrument over time, residents other than the 928 residents who participated in the general study were recruited. Of the 48 facilities involved in the study, 5 agreed to participate in this phase of the study: one in Alberta, one in British Columbia, and three in Ontario. For a critical effect size of 0.70, at 5 per cent level of significance, 90 per cent power, and using a two-tailed test, the approximate number of subjects required would be 16 (Knickman & Snell, Reference Knickman and Snell2002). A total of 22 residents agreed to participate, exceeding this minimum requirement.
The same informed consent procedure was used and written consents obtained. Each resident was interviewed twice by the same surveyor with an interval ranging from 3 to 26 days, with 77 per cent within 14 days, 14 per cent in 22 days, and 9 per cent in 26 days, depending on the availability of residents and the scheduling of the “retests” by the surveyors. Expert opinion on the time interval between test-retest suggests from one hour to a year, but a retest interval of 2 to 14 days is considered usual (Streiner & Norman, Reference Streiner and Norman2008). The level of agreement between the initial and retest QoL item scores was measured by calculating weighted kappa coefficients (Bowling, Reference Bowling2009; Landis & Koch, Reference Landis and Koch1977; Streiner & Norman, Reference Streiner and Norman2008). To test its internal consistency, Cronbach’s alpha was calculated.
The convergent validity of the instrument was assessed by two methods. First, the residents’ domain-specific mean QoL scores were compared with their ratings of the global disposition item. Second, the association between the overall mean QoL scores and the global disposition ratings was evaluated by calculating Pearson’s correlation coefficients. The underlying hypothesis was that residents who reported high scores in their global disposition would also report high QoL in each of the domains and in overall QoL, but expecting that correlations with domain-specific scores would be lower than the correlation with the overall QoL score.
To assess the content validity of the interRAI QoL Survey instrument, a content validity matrix (Streiner, Reference Streiner1993; Streiner & Norman, Reference Streiner and Norman2008) was constructed. Its domains and items were mapped against two other QoL instruments, namely, the Quality of Life Index (Kane, Reference Kane2003) and the Ontario Hospital Association’s (OHA) LTC Resident and Family Member Evaluation Surveys (Ontario Hospital Association, 2001). Kane et al.’s (Reference Kane, Kling, Bershadsky, Kane, Giles and Degenholtz2003) QoL Index has evidence of acceptable performance in both reliability and concurrent validity (e.g., Cronbach alphas ranged from .76 to .52; correlation with overall satisfaction item in instrument). The OHA’s survey instrument was designed by content experts and an advisory panel vetted its face validity (Ontario Hospital Association, 2001). The OHA survey is used across health care facilities in Ontario to directly measure patient and family perspectives on the care they receive.
Results
A convenience sample of 928 residents from a convenience sample of 48 LTC facilities from six Canadian provinces were involved in this study. The primary objective of the study was to describe residents’ QoL from their perspective. These results are discussed after those of the secondary objective, which was to test the psychometric properties of the interRAI QoL Survey instrument.
LTC Facility and Resident Characteristics
Forty-eight LTC facilities from six provinces in Canada participated. The majority was privately owned (66.7%), for-profit (62.5%), urban (87.5%), and accredited (91.7%). The number of beds in these facilities ranged from 10 to 357 (mean = 135.3, standard deviation [SD] = 65.9, median = 129), with medium-size facilities (95 to 159 beds) representing the largest category (45.8%).
Table 1 shows the distribution of participating residents’ socio-demographic characteristics. Almost 75 per cent of the residents were aged 75 or older; the mean age was 80.2 (SD = 11.1). Almost two-thirds of the sample was female and only 21 per cent was married, reflecting the older age of the participants. The majority of the sample (60%) was not involved in religious practices. Almost 45 per cent of the residents had not completed high school and over 60 per cent of the residents had been in the LTC facility for one year or longer.
Table 1: Resident socio-demographic characteristics in long-term care facilities in six Canadian provinces

Note:
1 Not all sample sizes (n) for the characteristics in this table add up to 928 (the study sample) due to missing data in RAI MDS.
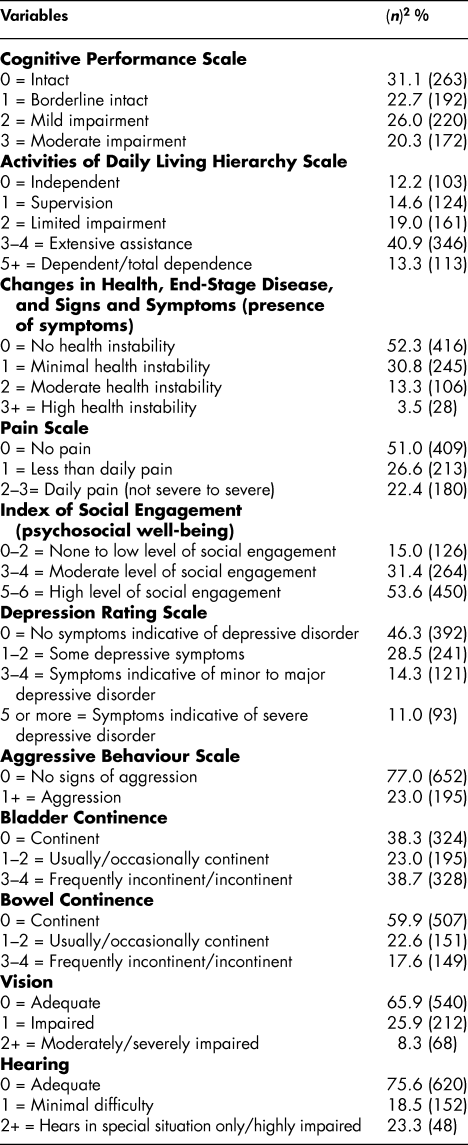
Forty-six per cent of the residents were assessed with mild to moderate impairment (see Table 2) and over half required extensive assistance or were totally dependent in their activities of daily living. The majority of the resident sample (over 80%) had relatively stable health, but 22 per cent reported daily pain. Over half (53%) had a high level of social engagement. Minor to major depressive symptoms were present in 14.3 per cent, and 11 per cent had severe depressive symptoms. On behavioural measures, only 23 per cent of the resident sample showed one or more signs of aggression. Almost 40 per cent suffered from frequent bladder incontinence but only 18 per cent from bowel incontinence. Sixty-six per cent had adequate vision, and 76 per cent had adequate hearing.
Table 2: Resident clinical characteristics in long-term care facilities in six Canadian provinces

Note:
2 Not all sample sizes (n) for the characteristics in this table add up to 928 (the study sample) due to missing data in RAI MDS.
Psychometric Properties of the interRAI QoL Survey Instrument
The psychometric properties of the instrument were examined by assessing its reliability and validity.
Reliability
The level of agreement (weighted kappa coefficients) between the initial and retest QoL item scores ranged from –0.10 to 0.80. Based on the interpretation categories proposed by Landis and Koch (Reference Landis and Koch1977), 58 per cent (n = 29) of the coefficients reflected moderate to substantial agreement and 22 per cent (n = 11) fair agreement. In 27 of the 50 items, there was stronger agreement between the two ratings for residents who were re-interviewed within 14 days compared to intervals longer than 14 days, but it did not change the agreement category. Based on these findings, the interRAI QoL Survey may be considered to have moderate test-retest reliability.
The internal consistency of the instrument was measured by Cronbach’s alpha, with coefficients for each domain ranging from .60 (Comfort domain) to .82 (Food/Meal domain); and an overall alpha coefficient of .93 (see Table 3). Values of .70 or higher indicate good internal consistency (Streiner & Norman, Reference Streiner and Norman2008). The Cronbach’s alpha coefficients in this study were compared to the ones computed by Morris (Reference Morris2009) in his pilot study of the interRAI QoL Survey in an LTC facility in Boston, Massachusetts. As shown in Table 3, with a few exceptions, the Cronbach alpha values in our study were comparable to those reported by Morris (domain alpha values ranging from .48 to .76; overall value .91) and demonstrated good internal consistency.
Table 3: interRAI QoL Survey’s internal consistency

Convergent Validity
Most residents (60.3%) scored positively, that is, reported “most of the time” or “always” to the global disposition item (“I tend to be happier than most other people”). These residents reported significantly higher domain-specific mean QoL scores compared to residents with lower global disposition ratings. As expected, we found the correlation of the global item was higher with the overall QoL score (r = .46; p < .0001) than with the domain-specific scores (r = .21 to r = .39; p < .0001). These r values are indicative of good convergent validity between the global disposition item and QoL subscales.
On the global item “I would recommend this site or organization to others”, almost 80 per cent of the residents rated positively. Domain-specific mean QoL scores were significantly higher for each domain in residents who rated this global recommendation item higher. The Pearson’s correlation between the domain-specific QoL ratings and the global recommendation item was moderately strong, ranging from r = .30 to r = .70 (p < .0001). The correlation between the global recommendation item and the overall mean QoL score was fairly strong with a Pearson’s r = .55 (p < .0001). This provides additional evidence for the convergent validity of the QoL subscales.
Content Validity
In comparing the interRAI QoL Survey with Kane’s (Reference Kane2003) QoL Index and OHA’s (2001) LTC Resident and Family Member Evaluation Survey, we found considerable overlap between the interRAI QoL domains and items and Kane’s and OHA’s survey instruments, but with a few distinct differences (see Table 4). For instance, Kane’s QoL Index places greater emphasis on spirituality with the inclusion of four items in this domain; the interRAI QoL Survey has only one item on spirituality under its “activity” domain, and OHA’s survey does not include any items on spirituality. OHA’s survey, however, places greater importance on residents’ environment than do the other two instruments. Kane’s QoL Index does not include a global dispositional item. In contrast, the interRAI QoL Survey includes a global dispositional item and OHA’s survey includes an overall quality rating. Based on the analysis of the psychometric properties of the interRAI QoL Survey instrument, we concluded that the instrument has sufficient content validity for assessing LTC facility residents’ QoL.
Table 4: Content validity matrix: Comparing interRAI QoL Survey to Kane’s QoL Index and OHA’s Long-Term Care Facility Resident & Family Survey

Notes:
OHA = Ontario Hospital Association; LTC = long-term care; QoL = quality of life
3 Domain name is “Enjoyment”.
4 One of the items states “This place feels like home to me”, which aligns with OHA’s “[The facility] is a wonderful place”.
5 Domain name in Kane’s QoL Index is “Autonomy”.
6 One item in Kane’s “Dignity” domain relates to respect.
7 interRAI items align with Kane’s “Dignity” domain items.
8 OHA’s domain name is “Staff Domain”.
9 Domain name in Kane’s QoL Index is “Meaningful Activity”.
10 One item aligns with interRAI’s “Staff Resident Bonding”.
11 Only available in Kane’s QoL Index; interRAI has one item under “Activity Options” about religiosity.
12 All five items in Kane’s “Dignity” domain relate to how staff treat residents.
13 One of the three global quality indicator questions is about recommending the facility to others; the second one is about the facility being a wonderful place.
Distribution of Residents’ QoL Ratings
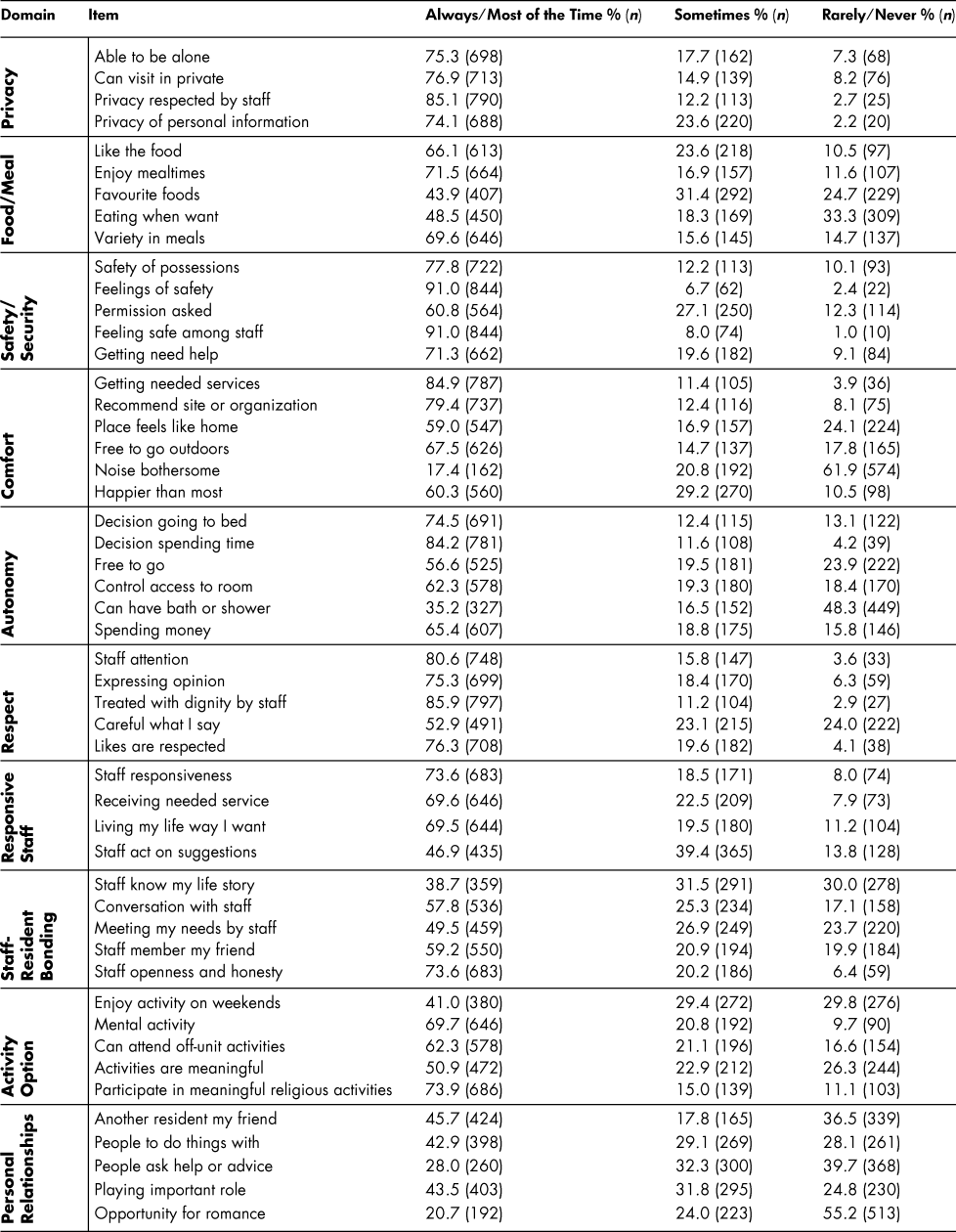
The distribution of residents’ responses for each of the interRAI QoL Survey instrument items is shown in Table 5 where positive scores (“always/most of the time”) were combined. Most residents rated positively having privacy during visits (76.9%), receiving care (85.1%), and the privacy of their personal information (74.1%). Although two-thirds of residents liked the food and enjoyed mealtimes (71.5%), only 43.9 per cent reported positively about getting their favourite foods, and only 48.5 per cent reported that they could eat whenever they wanted. The majority of residents felt that their possessions were safe (77.8%), but fewer residents felt they had control over who accessed their personal things (60.8%). Most residents felt safe when alone (91.0%) and that they could get help when needed (71.3%).
Table 5: Long-term care facility residents’ reports of quality of life by item and domain

Almost 60 per cent of the residents reported that the facility felt like home, and almost 80 per cent reported they would recommend the facility to others. Regarding decision-making autonomy about daily aspects of life in the facility, 74.5 per cent reported positively about having control over when to go to bed or get up, 56.6 per cent reported being able to go where they wanted on the “spur of the moment”, and 62.3 per cent reported having control over who entered their room. However, only 35.2 per cent of residents reported positively about being able to have a bath or shower as often as they wanted. In terms of being treated with respect, positive scores ranged from a low of 52.9 per cent (for being careful about what they say around staff) to a high of 85.9 per cent (for being treated with dignity by staff).
The majority of residents also reported positively on staff responsiveness when assistance was requested (73.6%), but only 46.9 per cent reported that staff acted on their suggestions. Nearly 70 per cent reported positively the promptness of services received, and 69.5 per cent reported positively about having the support needed to help them live their life in the way they wanted in the facility. Regarding opportunities for staff-resident bonding, only 38.7 per cent reported positively that staff knew about the story of their life, but 73.6 per cent reported that staff were open and honest with them. For activity options, 41 per cent of the residents had enjoyable things to do on weekends, 69.7 per cent did things that kept them mentally active, 50.9 per cent participated in meaningful activities, and 73.9 per cent could participate in religious activities that had meaning to them.
In the “personal relationships” domain, only 45.7 per cent of residents reported positively about having another resident in the facility as their close friend. Similarly, only 28 per cent reported positively as being sought after by others for help or advice, and only 43.5 per cent reported playing an important role in people’s lives. The lowest reported QoL level was related to affection or romance, with only 20.7 per cent reporting positively in this area. On the two global items, the majority of residents reported positively (60.3%) on the global disposition item, and 79.4 per cent would recommend their LTC facility to others.
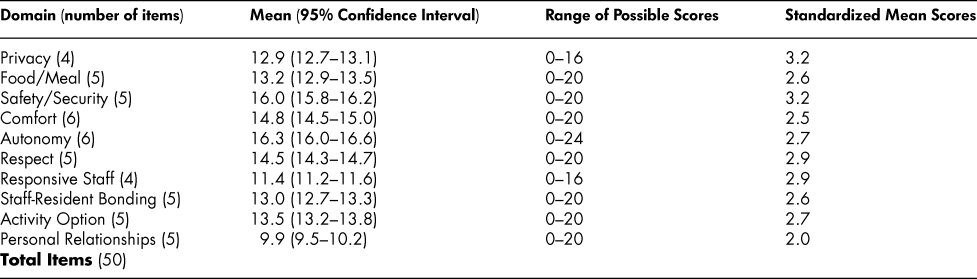
QoL ratings were highest in relation to “privacy” and “safety/security” domains, with standardized scores of 3.2 (see Table 6). These were followed by “respect” and “responsive staff” with standardized scores of 2.9. Residents’ QoL ratings were not as positive in the other domains. Residents reported lowest QoL scores in relation to “personal relationships”, one of the higher basic human needs in Maslow’s (Reference Maslow1962) hierarchy of needs.
Table 6: Standardized* overall quality of life scores in long-term care facility residents by domain

* As the items in each of the domains in the interRAI QoL Survey instrument varied from 4–6, standardized mean QoL values were calculated.
LTC = long-term care; OHA = Ontario Hospital Association; QoL = quality of life
The examination of the relationship between surveyor status in the LTC facility and the distribution of mean QoL scores by interRAI QoL Survey domains showed that surveyors’ status did not influence how residents rated their QoL. Although the overall mean reported QoL was higher in the group of residents who were interviewed by volunteers, it was not significantly different from the ratings in the other groups. There were no significant differences between the mean QoL scores among the other groups.
Discussion
This study was one of the largest of its kind in Canada to describe what residents in LTC facilities had to say about their QoL. The interRAI QoL Survey instrument was used successfully in measuring residents’ self-reported QoL, including residents with mild (26%; CPS = 2) and moderate cognitive impairment (20.3%; CPS = 3). This study affirms other research findings that direct measurement of QoL is the preferred approach (Crespo, Bernaldo de Quirós, Gómez, & Hornillos, Reference Crespo, Bernaldo de Quirós, Gómez and Hornillos2012; Kane et al., Reference Kane, Kane, Bershadsky, Degenholtz, Kling and Totten2005). The residents’ self-reported QoL ratings confirmed previously published reports that LTC facility residents value their autonomy, personal choice, and autonomy (Boisaubin, Chu, & Catalano, Reference Boisaubin, Chu and Catalano2007; Iris, DeBacker, Benner, Hammerman, & Ridings, Reference Iris, DeBacker, Benner, Hammerman and Ridings2012; Wulff et al., Reference Wulff, Kolzsch, Kalinowski, Kopke, Fischer and Kreutz2013) and that LTC facility staff may inadvertently neglect residents’ sense of autonomy in the course of delivering care (Mullins & Hartley, Reference Mullins and Hartley2002). In our study, only 35 per cent of residents provided positive ratings on their ability to have a bath or shower as often as they wanted, and only 62 per cent reported positively that they could control who entered their room. Whereas most LTC facilities have adopted resident-centred philosophies of care and have instituted measures in their physical design and programming to create “home-like” environments (Burack et al., Reference Burack, Weiner, Reinhardt and Annunziato2012; White-Chu et al., Reference White-Chu, Graves, Godfrey, Bonner and Sloane2009), only 59 per cent of the respondents in this study reported positively that the LTC facility felt like home to them. These are important findings considering that, for most residents, the LTC facility becomes their permanent residence for the balance of their lives (Holtkamp, Kerkstra, Ribbe, Van Campen, & Ooms, Reference Holtkamp, Kerkstra, Ribbe, Van Campen and Ooms2000).
It is apparent from these findings that, despite well-intended policy directions and efforts by LTC operators, there is a gap between philosophies of care and their translation into a care environment where care is truly resident-directed. While quality care has been a transformational goal in LTC and recognized as a necessary condition for QoL, residents may still not experience positive QoL (Edelman, Fulton, Kuhn, & Chang, Reference Edelman, Fulton, Kuhn and Chang2005). Evidence-based QoL measures should complement quality care measures to enhance residents’ QoL. For instance, active involvement in decisions concerning their care, exercising autonomy in aspects of their daily lives, and opportunity for personal relationships will contribute to shaping residents’ QoL. Older adults are more or equally likely to be concerned about their QoL as they are about the length of their lives (Kanwar et al., Reference Kanwar, Singh, Lennon, Ghanta, McNallan and Roger2013). While life expectancy in LTC facilities is relatively short, a great deal could still be accomplished to improve residents’ QoL by assessing their self-reported QoL, identifying gaps or problems, and, with the active engagement of the resident, instituting and implementing a plan of care to address these gaps. Further, identifying and implementing institutional or organizational measures are also necessary in creating resident-centred cultures in LTC facilities.
Psychometric Testing of the interRAI QoL Survey Instrument
Psychometric testing of the instrument provided evidence in support of its reliability and validity for assessing LTC facility residents’ QoL. Test-retest showed moderate reliability. Internal consistency was considered good based on overall Cronbach’s alpha coefficient (alpha = .93), but with variance in the values of the different domains (alpha values ranging from .60 to .82).
The instrument also showed good convergent validity by correlating domain-level QoL scores with the embedded global item: “I would recommend this site or organization to others”, and a global disposition item: “I tend to be happier than most other people”. While the inclusion of a global disposition item is supported (Michalos, Reference Michalos1991), there is a potential risk when comparing QoL scores with such an item and particularly one measuring happiness. The items in the interRAI QoL Survey instrument reflect aspects of residents’ daily life and closely align with Maslow’s (Reference Maslow1962) hierarchy of needs. On the other hand, the global disposition item has a different construct. Happiness is viewed as stable over the life course (Stones, Kozma, McNeil, & Worobetz, Reference Stones, Kozma, McNeil and Worobetz2011), while aspects of daily life as measures of QoL may be less stable due to possible changes in residents’ health and functional status, medications, or psychological well-being (e.g., depression).
Findings from the psychometric testing of the full interRAI QoL Survey instrument in this study contributed to interRAI’s deliberations, which resulted in shortening the instrument and refining some of its items (Morris, Reference Morris2009). It is now being piloted in several LTC homes in Canada and internationally.
Residents’ QoL Ratings
Based on the results of this study, most residents seem to be positive about various aspects of their QoL in the LTC facility where they reside. However, the findings also point to various aspects of residents’ experience that require particular attention. For instance, residents gave lower scores on their food and mealtime experience. Residents consider food and eating an important aspect of their daily life in LTC (Lengyel, Smith, Whiting, & Zello, Reference Lengyel, Smith, Whiting and Zello2004). Dissatisfaction with food often results in reduced food intake leading to malnutrition risk, morbidity, mortality, and depression (Carrier, West, & Ouellet, Reference Carrier, West and Ouellet2009; Crogan & Evans, Reference Crogan and Evans2006; Lengyel et al., Reference Lengyel, Smith, Whiting and Zello2004). There could be several factors for residents not being very satisfied with their food or mealtime. They may not have a choice in menu planning or dining companions (Carrier et al., Reference Carrier, West and Ouellet2009), and the physical environment of the dining room, such as noise and crowding, may not be appealing or conducive to pleasurable dining (Chaudhury, Hung, & Badger, Reference Chaudhury, Hung and Badger2013). LTC facilities serving culturally diverse residents may find it challenging to plan menus that recognize residents’ cultural diversity and accommodate diverse preferences (Ducak & Keller, Reference Ducak and Keller2011). Aging-related changes in the oral cavity may be associated with loss of taste (Timiras, Reference Timiras2007), which in turn may lead to lack of enjoyment and, hence, less satisfaction with food. A resident-centred approach combined with a holistic model of care may be most responsive to residents’ needs.
From Maslow’s (Reference Maslow1962) hierarchy of basic human needs, personal relationships are very important for QoL, particularly in LTC facilities where residents may be isolated from their familiar relationships and may find it difficult to form new relationships in their new surroundings. The findings of this study showed that personal relationships remain a substantial area of concern for the majority of residents. LTC facilities need to create meaningful social engagement opportunities for residents. The finding supports previous studies showing that social engagement has been associated with QoL in older adults (Degenholtz et al., Reference Degenholtz, Kane, Kane, Bershadsky and Kling2006).
QoL ratings in the “responsive staff” domain also require particular attention considering that LTC facilities are mandated to be resident-centred in their care planning. These findings support the work of other researchers who reported that life in LTC facilities is disempowering (Boisaubin et al., Reference Boisaubin, Chu and Catalano2007; Iris et al., Reference Iris, DeBacker, Benner, Hammerman and Ridings2012; Wulff et al., Reference Wulff, Kolzsch, Kalinowski, Kopke, Fischer and Kreutz2013). It appears from the findings of this study that despite best efforts from facility staff, residents do not feel that they have a voice in matters affecting their personal life in the LTC facility.
Strengths and Limitations
The resident sample size and the number of participating LTC facilities from six provinces made this study one of the largest of its kind in Canada. This study successfully demonstrated that conducting a large-scale, national survey on QoL in LTC was possible. It further demonstrated that residents’ QoL could be assessed through self-reports, including reports from those with mild to moderate cognitive impairments.
Trained surveyors with a variety of associations with the facility (e.g., volunteers, students, and administrative staff) conducted the QoL surveys. It is a common concern in QoL research that residents’ responses may be biased due to social desirability or possible intimidation (Streiner & Norman, Reference Streiner and Norman2008), particularly when surveyors are clinical staff providing direct care to them. However, in our study, surveyors’ status in the facility did not have a significant impact on residents’ overall QoL ratings.
While this study had several strengths, it also had limitations. One limitation was the cross-sectional nature of the data. However, as an aim of the study was to describe the distribution of LTC facility residents’ self-reported QoL, this design was appropriate to meet that objective. Resident sample recruitment was another limitation. Because of the large and cross-national scope of the study, LTC facility staff members were responsible for recruiting residents into the study. While facility staff members were provided with a script to standardize messaging during recruitment, the extent of adherence was not determined. There were no measures to determine if facility staff were selective in their choice of the residents whom they approached, with the exception of eligibility criteria for cognitive function (CPS score of 0–3). This may have contributed to selection bias due to differences in perceptions of QoL in those residents who were invited compared to those who were not. Another limitation was the choice of a convenience rather than representative sample of residents and LTC facilities, with implications for the generalizability of the study findings. Exclusion of residents with CPS scores greater than three (i.e., those with greater than moderate impairment) also influenced the generalizability of our findings. The proportion of residents with cognitive impairments who are being admitted into the LTC facilities is increasing given the introduction of alternative community-based models of care (e.g., aging in place). Research has suggested that individuals with moderate dementia are able to report on their QoL, even when they have poor insight into and awareness of their dementia (Crespo et al., Reference Crespo, Bernaldo de Quirós, Gómez and Hornillos2012; Logsdon et al., Reference Logsdon, Gibbons, McCurry and Teri2002). Future studies on QoL in LTC facility residents should explore the inclusion of residents who have more severe cognitive abilities (i.e., CPS score greater than 3).
Although the interviews were conducted by trained surveyors, there were no procedures in place to assess their qualifications for participation in the study, or to monitor the quality of the interviews they conducted. Other researchers have also recognized the importance of monitoring the quality of interviews (Degenholtz et al., Reference Degenholtz, Kane, Kane, Bershadsky and Kling2006). Finally, refusal of residents to participate in the study may have also introduced non-response bias, with respondents not representative of all eligible LTC residents. Reasons for refusal were not documented. Although a 51 per cent response rate is relatively low, in a population-based study on QoL in the United Kingdom researchers achieved a response rate of 62 per cent with representative results (Bowling & Gabriel, Reference Bowling and Gabriel2004). As well, other researchers have argued that QoL data obtained from a representative sample of LTC facilities would result in QoL ratings similar to those from a non-representative sample (Degenholtz et al., Reference Degenholtz, Kane, Kane, Bershadsky and Kling2006). However, future studies should analyze reasons for refusal to participate.
Potential Implications
The results of this study are of relevance to LTC facility staff, educators, policy makers, and researchers. Information from this study will benefit facility care staff by raising their awareness of the importance of residents’ self-reported QoL and what residents have to say about their life in the facility. QoL domains that did not receive high ratings could be targets for intervention as noted above. As the interRAI QoL Survey instrument allows for QoL assessment from a multidimensional perspective, it will assist facility staff to identify issues and concerns from a diverse set of measures. Early identification of reported gaps in QoL could lead to timely interventions and improved QoL.
The study findings can also inform educators on the design of appropriate curricula in the preparation of health care professionals for a dedicated career in LTC. Such curricula could potentially include gerontology, QoL, quality care, and fostering positive attitudes towards working with older adults in either institutional or community settings. Research has identified lack of gerontological knowledge as the most frequent barrier for fostering positive attitudes to working with older adults (Fox, Reference Fox2013). In the work setting, employers must create an organizational culture where staff can apply evidence-based knowledge in their practice rather than simply adhering to organizational routines. To enhance continued competence, current and prospective facility staff should be offered ongoing continuing education programs. The findings of this study have the potential to inform the content of such programs as well. To increase the capacity of LTC facility staff to be sensitive to residents’ QoL and to design targeted interventions, the facility leadership should adopt strategies for sustained knowledge transfer, such as management support, designated time for QoL activities, and availability of staff skilled and trained in QoL (Stolee et al., Reference Stolee, McAiney, Hillier, Harris, Hamilton and Kessler2009). Research on factors associated with the effectiveness of continuing education in LTC underscores the important role that management and organizational support play in introducing innovation in the workplace environment (Stolee et al., Reference Stolee, Esbaugh, Aylward, Cathers, Harvey and Hillier2005). For QoL to be integrated into the care and service environment of LTC facilities, the model of communities of practice of the Seniors Health Research Transfer Network (SHRTN), which is designed to improve the health and care of seniors, could be adopted (Conklin et al., Reference Conklin, Kothari, Stolee, Chambers, Forbes and Le Clair2011).
Further, the findings of this study can inform public policy development. First, this study demonstrated that measurement of QoL on a large scale nationwide is possible. Given the importance of QoL as an outcome measure, public policy could support the adoption of a standardized QoL assessment instrument. The interRAI QoL Survey instrument was shown to have reliability and validity. Ongoing efforts by interRAI resulted in a shorter version of the survey used in this study that will be more amenable for acceptance by LTC facilities. As well, policy makers may recognize the use of standardized instruments for measuring QoL for public reporting of LTC facility performance. The use of standardized instruments will ensure consistency of reporting; however, fair comparisons would require risk adjustment to control for confounding factors and their distribution across facilities (Mor, Angelelli, Gifford, Morris, & Moore, Reference Mor, Angelelli, Gifford, Morris and Moore2003; Rosen et al., Reference Rosen, Wu, Chang, Berlowitz, Rakovski and Ash2001). As subjective self-appraisals are considered by many to be the “gold standard” for QoL measurement (Bankole et al., Reference Bankole, Cohen, Vahia, Diwan, Kehn and Ramirez2007), their adoption for use in LTC facilities will contribute to resident empowerment. Such a process will support and encourage residents’ active engagement in decisions that affect their care and daily life in the LTC facility. This study demonstrated that residents do have a voice, and they are not shy about expressing views about their care and relationships. As baby boomers age and become the future residents of LTC facilities, they will be vocal about their wishes, and will be strong advocates in shaping the environment where they will receive care, services, and accommodation. The availability of a standardized QoL measurement instrument may provide them with the means to do so.
Recommendations for Future Research
Future research should consider addressing the aforementioned limitations. Residents may not always have the choice of the facility into which they are admitted. Future studies should include a qualitative component to assess whether the facility was a resident’s first choice, and if not, what its impact on their relationships with family and friends has been. Residents’ perception of admission to an LTC facility should also be explored, and its relationship to QoL should be evaluated as it may have a profound effect on their QoL. Future research should also be directed at risk adjustment. Such research would contribute to identifying those QoL factors that would need to be adjusted to make fair comparisons between facilities to support choice of facilities and public reporting.
As public policy will support aging at home with appropriate community support, the design of future QoL assessment instruments should allow for assessment of future residents who may be more frail and have more severe cognitive impairments. The present study excluded residents with severe cognitive impairment. Further research should include these residents to test the reliability and validity of QoL instruments. Sample selection in this study was also limited to English-speaking residents. As cultural diversity increases in LTC facilities, future research should test the application of such an instrument in different languages.
The cross-sectional design of this study was appropriate for its intended purpose; however, future research needs to move beyond cross-sectional analyses. The effect of nursing interventions on the QoL of residents in LTC facilities, for instance, should be investigated through longitudinal studies. The interRAI QoL Survey may be a useful new tool for evaluating the impact of initiatives aimed at improving QoL in randomized trials.
Conclusion
This study makes a unique contribution to the measurement of LTC facility residents’ QoL. The use of a dedicated, standardized instrument that measures residents’ QoL purely from their perspective is an important development in the LTC system. Psychometric testing of the instrument provided evidence in support of its reliability and validity for assessing LTC facility residents’ QoL. Residents with mild to moderate cognitive impairments were able to participate in direct measurement of QoL and self-report on their life in the LTC facility from their own perspective. In addition, this study demonstrated that QoL assessment on a large scale is possible.
The findings of this study have the potential to contribute to the cultural transformational efforts in the LTC sector for improving residents’ quality care through a resident-centred approach. The results clearly demonstrated how residents perceived their QoL in LTC facilities. Residents rated positively many aspects of their daily lives, but also identified some serious gaps that, if addressed, may potentially enhance their QoL. The study findings have the potential to inform evidence-based practice for the care of older adults in LTC facilities and LTC policy development for the adoption of a standardized QoL assessment instrument integral to a quality care information system.