Epidemiological studies have suggested a positive association between intake of trans-fatty acids (TFA) from partially hydrogenated vegetable oil and the risk of CHD(Reference Micha and Mozaffarian1). These findings have resulted in a restriction of the content of industrially produced TFA (I-TFA) in manufactured food in some Western countries, including Denmark, whereas in several other countries, popular foods such as fast food, biscuits, cakes, wafers and popcorn still contain high amounts of I-TFA(Reference Stender, Dyerberg and Bysted2).
The intake of I-TFA has been suggested to be more important than intake of SFA in predicting the risk of CHD(Reference Erkkila, de Mello and Riserus3). Evidence suggests that I-TFA intake may result in altered lipid profiles (increased LDL-cholesterol and TAG and decreased HDL-cholesterol)(Reference Mensink, Zock and Kester4, Reference Mensink5). Also, a study in monkeys has suggested that I-TFA induces abdominal obesity(Reference Kavanagh, Jones and Sawyer6), which could hypothetically affect insulin sensitivity and plasma lipids. However, deposition of abdominal fat was not affected by TFA although LDL-cholesterol increased and HDL decreased in a short-term intervention study in healthy overweight postmenopausal women(Reference Bendsen, Chabanova and Thomsen7). Furthermore, I-TFA has been observed to be associated with endothelial dysfunction, systemic inflammation and insulin resistance, although evidence is conflicting(Reference Micha and Mozaffarian1, Reference Ghafoorunissa8). In contrast to I-TFA, the chemically distinct ruminant TFA (R-TFA) present in products from cow, calf, lamb and goat has either not been associated with or has been inversely associated with the risk of CHD(Reference Stender, Astrup and Dyerberg9). However, two randomised controlled trials have found that high R-TFA intakes (10·2 g/10·5 MJ and 11–12 g/d, respectively) have an unfavourable impact on plasma lipids(Reference Chardigny, Destaillats and Malpuech-Brugere10, Reference Motard-Belanger, Charest and Grenier11), whereas a moderate intake of R-TFA (4·2 g/10·5 MJ)(Reference Motard-Belanger, Charest and Grenier11) seemed to have a minor or even neutral effect. The health effect of I-TFA and R-TFA does not seem to differ.
Earlier studies on CHD risk markers have typically been based on relatively high intakes of I-TFA(Reference Mensink and Nestel12), and may therefore not reflect the normal average intake among persons even in countries without restrictions. The intake of I-TFA in the Danish population dropped to a level of 0·5–1 g/d between 1995 and 2003, until the Danish legislation effectively eliminated food products containing I-TFA(Reference Stender, Astrup and Dyerberg9, Reference Bysted, Mikkelsen and Leth13). The health consequences of a relatively low intake of I-TFA remain uncertain.
The aim of the present study was to investigate whether variations in the intake of total TFA, I-TFA and R-TFA – during the period before the legislation in Denmark – were associated with obesity-associated risk markers of CHD (abdominal fat deposition, low-grade systemic inflammation, lipid profile, blood pressure and glucose homeostasis) among middle-aged Danish men representing a broad range of BMI.
Experimental methods
Study population
The present study population derives from a population of 362 200 Danish men, registered at the mandatory draft boards from 1943 to 1977. Among these, two groups were manually selected: a random 1 % sample of all men (n 3601) and all obese men (with a BMI ≥ 31 kg/m2, n 1930)(Reference Christensen, Sonne-Holm and Sorensen14–Reference Sorensen and Sonne-Holm16). This sampling technique was carried out to obtain a study population, which enabled the study of a much wider range of BMI than usual. Half of the random sample (reduced for economical and logistic reasons) and all obese subjects were followed repeatedly until the last follow-up study conducted between 1998 and 2000, in which all subjects below 65 years, who reported to be healthy and receiving no regular medication, were included (n 557)(Reference Black, Holst and Astrup17). In addition to a thorough clinical examination at follow-up, 394 subjects had completed a 7 d dietary record. One subject was excluded due to an energy intake below 2000 kJ/d, hence leaving 393 subjects with dietary variables recorded at a given point during 1998–2000 available for the present study.
The present study was conducted according to the guidelines laid down in the Declaration of Helsinki, and all procedures involving human subjects were approved by the Danish Surveillance Agency and the regional Ethics Committee. Written informed consent was obtained from all subjects.
Intake of trans-fatty acids
Extraction of information on dietary intake from 7 d dietary records has been described previously(Reference Nielsen, Nielsen and Toubro18). Total energy intake was calculated from the foods' content of protein (17 kJ/g), carbohydrate (17 kJ/g), fat (38 kJ/g) and alcohol (30 kJ/g).
The specific content of I-TFA in food products was estimated based on analyses of several samples of foods containing I-TFA sold in Danish retail during years 1995–2003(Reference Hansen, Knuthsen and Saxholt19–Reference van Poppel23). To determine the most reliable estimates of I-TFA in the study period, a linear decrease in mean I-TFA content from 1995 to 2003 was assumed. Since I-TFA was out of Danish household margarine in 1999, but still present in shortenings used in the food industry(Reference Leth, Bysted and Hansen20, Reference van Poppel23), an average value of 5·59 g I-TFA/100 g shortening (weighted after the sale of different categories of shortenings and corrected for water content and the 20 % cis/trans overlap between peaks in capillary GC(Reference Leth, Bysted and Hansen20)) was used to estimate I-TFA content. A weighed division between home-made (50 %) and ready-made foods (50 %) was applied.
Calculation of R-TFA content in distinct food products was based on analyses of the R-TFA content in butter(Reference Jakobsen, Bysted and Andersen24) and ruminant meat cuts(Reference Leth, Ovesen and Hansen25). The mean content of R-TFA in butterfat was found to be 4·48 g/100 g, inclusive of conjugated linoleic acid, and was considered representative of milk fat in dairy products and in composite products containing milk fat(Reference Jakobsen, Bysted and Andersen24). Conjugated linoleic acid was not included in the mean values of R-TFA in meat(Reference Leth, Ovesen and Hansen25). The amount of total TFA was calculated by adding together the contents of I-TFA and R-TFA.
Outcome assessment
Anthropometric measurements
The present weight and height were measured as described earlier(Reference Black, Petersen and Kreutzer26). Abdominal fat distribution was determined by (1) waist circumference (WC) measured according to the WHO standard(27), (2) sagittal abdominal diameter, measured as the maximal distance between the top of the examination table and a spirit level horizontally placed above the abdomen at the level of the iliac crest (in the expiration phase) and (3) truncal fat mass determined from measurements of body composition by dual-energy X-ray absorptiometry scans with a diagonal line passing through the middle of the femoral neck separating the lower body and truncal regions. Truncal fat mass in percentage of total tissue mass was calculated as: 100 × fat tissue mass (g)/(lean tissue mass (g)+fat tissue mass (g)+bone mineral content (g))(Reference Buemann, Sorensen and Pedersen28). The subjects were categorised as being normal weight, overweight and obese according to the WHO classification(29).
Blood lipids, inflammatory markers, glucose homeostasis and blood pressure
Blood samples for measurements of blood lipids and inflammatory markers were obtained in the morning after an overnight 12 h fast. Total cholesterol, TAG and HDL-cholesterol were measured in whole blood samples. LDL-cholesterol was calculated from the Friedewald equation:
excluding measurements with TAG >4 mmol/l(Reference Friedewald, Levy and Fredrickson30). C-reactive protein was measured by ELISA(Reference Skogstrand, Ekelund and Thorsen31) and IL-6 was measured by Luminex xMAP technology(Reference Skogstrand, Thorsen and Norgaard-Pedersen32).
HbA1c was measured and an oral glucose tolerance test (OGTT) was performed(33). The latter was used for calculation of the composite whole-body insulin sensitivity index, defined according to Matsuda & DeFronzo as(Reference Matsuda and DeFronzo34):
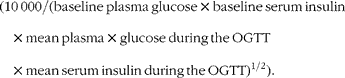
Blood pressure was measured with a digital blood pressure meter and a mean value of three consecutive measurements was calculated.
Potential confounders
Based on a review of the literature, the following potential confounders were included: age (years), self-reported smoking status (stated as present smoker or non-smoker), self-reported leisure-time physical activity (stated as almost passive, light activity 2–4 h, light activity >4 h or medium 2–4 h and hard activity)(Reference Buemann, Sorensen and Pedersen28), alcohol consumption (g/d), dietary fibre (g/d), total fat (g/d), SFA (g/d) and PUFA (g/d). After exclusion of subjects for whom information on one or more potential confounder was missing, the final population consisted of 386 subjects.
Statistical analysis
Characteristics of the participants are presented as medians with 10th and 90th percentiles. Associations between intake of total TFA, I-TFA and R-TFA (g/d) and each of the CHD-related risk factors (abdominal fat distribution (WC, n 384; percentage of truncal fat, n 380)), proxies for intra-abdominal fat mass (WC for given BMI, n 384; sagittal abdominal diameter, n 379), inflammatory markers (IL-6, n 379; C-reactive protein, n 372), blood lipids (total cholesterol, n 385; TAG, n 371; LDL-cholesterol, n 382; HDL-cholesterol, n 383; total cholesterol:HDL-cholesterol, n 383), blood pressure (systolic, n 382; diastolic, n 382) and glucose homeostasis (HbA1c, n 376; insulin sensitivity index, n 375) were analysed with linear regression models after testing for non-linearity in two-way scatterplots. β-Coefficients and 95 % CI were calculated and all analyses were carried out for the combined group representing the broad range of BMI, which according to the sampling design is allowable.
For examining the associations between TFA intake and the above-mentioned outcomes, three models were used. Model 1 is the raw model. Model 2 included total fat intake plus age, smoking status, leisure-time physical activity, alcohol and fibre intake. The total fat intake is included as we are interested in the effect of TFA, regardless of the intake of total fat. Model 3 included the same variables as model 2, with additional adjustment for intake of SFA and PUFA. I-TFA and R-TFA intakes were analysed in mutually adjusted models. Analyses of truncal fat mass and WC were rerun after additional adjustment for BMI.
Interactions between intake of TFA and the original sampling group were examined in all linear regression analyses and the distribution of residuals was investigated to ensure homogeneity in the data.
To investigate the potential influence of misreporting of dietary intake, all regression analyses and interaction between TFA and current BMI were rerun among those who were most likely to have reported an energy intake matching their energy expenditure (n 194, defined in an earlier study)(Reference Nielsen, Nielsen and Toubro18). Only minor differences from the results of the total group of men appeared, and thus misreporting did not seem to have had an influence on the results.
Data analyses were conducted using STATA statistical software, release 9.2 (STATA Corporation, College Station, TX, USA).
Results
The 393 men had a median age of 49 years and a median BMI of 28·4 kg/m2 (10–90th percentile 22·3–39·5), with 28·0 % being normal weight, 31·8 % overweight and 40·2 % obese (Table 1). Most subjects were lightly physically active for 2–4 h/week (51·9 %) in their leisure time.
Table 1 Dietary intake, age, BMI, level of physical activity and selected risk factors of CHD among Danish men representing a broad range of BMI
(Median values with 10–90th percentiles)

TFA trans-fatty acids; I-TFA, industrially produced TFA; R-TFA, ruminant TFA; E%, percentage of energy; SAD, sagittal abdominal diameter; LTPA, leisure-time physical activity.
* Values were significantly different from the corresponding median of the juvenile obese (P < 0·05). The difference in age is due to increasing prevalence of obesity over time during recruitment.
The median intake of total TFA was 1·3 g/d (10–90th percentile 0·6–2·5), composed of 0·4 g/d (10–90th percentile 0·0–1·0) of I-TFA and 0·9 g/d (10–90th percentile 0·4–1·8) of R-TFA. Interquartile ranges and medians of I-TFA and R-TFA intakes are illustrated in Fig. 1.

Fig. 1 Interquartile ranges (25–75th percentiles) and medians of industrial trans-fatty acid (I-TFA, ![]() ) and ruminant trans-fatty acid (R-TFA,
) and ruminant trans-fatty acid (R-TFA, ![]() ) intakes among middle-aged Danish men representing a broad range of BMI.
) intakes among middle-aged Danish men representing a broad range of BMI.
There were no associations between consumption of total TFA, I-TFA or R-TFA and abdominal obesity (waist), respectively, the proxies of intra-abdominal fat mass (waist for given BMI and sagittal abdominal diameter), nor with truncal fat mass (Table 2). No significant associations between intakes of TFA and pro-inflammatory markers, cholesterol levels, TAG and blood pressure were observed (Table 2). TFA intakes did not associate with the HbA1c level, whereas a tendency towards a positive association between R-TFA intakes and insulin sensitivity index was observed (model 3: β 1·14, 95 % CI − 0·13, 2·42; Table 2).
Table 2 Associations between intake of trans-fatty acids (TFA) (industrially produced TFA (I-TFA) or ruminant TFA (R-TFA)) and risk factors of CHD among Danish men representing a broad range of BMI

SAD, sagittal abdominal diameter.
* Log-transformed.† Model 1, unadjusted; model 2, adjusted for total fat intake (g/d), age (years), leisure-time physical activity (almost passive, light activity 2–4 h, light activity >4 h or medium 2–4 h and hard activity), smoking status (yes or no), alcohol intake (g/d) and fibre intake (g/d), and mutually adjusted for R-TFA and I-TFA, respectively; model 3 (same as model 2) and additional adjustment for intake of SFA (g/d) and PUFA (g/d).
Significant interactions between total TFA and the sampling group (P = 0·03) and between R-TFA and the sampling group (P = 0·02) were found for total cholesterol. These interactions may be attributed to multiple testing. No interactions between I-TFA intake and the sampling group were observed.
Discussion
In the present study of 393 middle-aged Danish men representing a broad range of BMI, low-to-moderate average intakes of TFA were not associated with abdominal fatness, pro-inflammatory markers, serum lipids, blood pressure or insulin homeostasis after adjustment for potential lifestyle confounders. This was the case when we examined total intake of TFA or separate intake of I-TFA and R-TFA.
The primary strength of the study was the availability of detailed clinical measurements and 7 d dietary records carried out in close proximity of each other from a unique sample of men representing a broad range of BMI and thereby a broad range of the obesity-related CHD risk markers of interest. According to the sampling fraction, the random sample represented 46 400 draftees, whereas the juvenile obese group represented all obese individuals in the original draft board population. Analyses for interaction confirmed that pooling the groups was acceptable and did not bias the examined associations. A potential limitation to the study was the assessment of men only. However, although risk factors of CHD may differ between women and men(Reference Silander, Alanne and Kristiansson35), epidemiological studies have not indicated that TFA should affect CHD risk differently in women and men and thereby compromise the generalisability of the present findings(Reference Oh, Hu and Manson36, Reference Oomen, Ocke and Feskens37). Still, we cannot rule out that the results from the present study may not transfer directly to women. Another potential limitation could be imprecise dietary measurement or dietary under-reporting. The use of a dietary record should diminish the risk of recall bias, but instead people might change their habitual intake, intentionally or unintentionally, during the reporting period. However, as long as such uncertainties are equally distributed throughout the study population, estimates may be weakened and hence conservative, but they should not be confounded. Misreporting is a main error in dietary research, but our analyses showed no difference between results of the total group of subjects and when excluding the most likely misreporters of energy intake.
Uncertainties in estimating actual dietary intake of TFA may exist. Since rather few products contained I-TFA at the time of data collection, it is likely that the standardised dietary record, which was not specifically designed for obtaining detailed information on TFA intake, may have led to lower estimated intake than the actual intake. Although the content of I-TFA in the distinct food items may have errors, the estimation benefits from the thorough analysis of a variety of Danish food items at time points close to the dietary assessment.
Misreporting and the approximation of TFA in food items are thus not believed to have biased the association between TFA and the clinical outcomes substantially.
In the present study, the average intakes of TFA and I-TFA were relatively low (1·3 g/d, 10–90th percentile 0·6–2·5 g/d; 0·4 g/d, 10–90th percentile 0·0–1·0) compared with former epidemiological studies reporting an increased risk of CHD following intake of TFA(Reference Oh, Hu and Manson36, Reference Oomen, Ocke and Feskens37). Total TFA intake has previously been found to range from about 1·5 g in Greece and Italy to 5·4 g in Ireland(Reference Hulshof, van Erp-Baart and Anttolainen38). Intake of R-TFA in the present study was also lower than that in some former studies(Reference Jakobsen, Overvad and Dyerberg39, Reference Willett, Stampfer and Manson40).
Associations between I-TFA and markers of abdominal obesity (WC and percentage of truncal fat) and of the proxies of intra-abdominal obesity (sagittal abdominal diameter and WC for given BMI) tended to be negative, although applied measuring methods are found to correlate well with intra-abdominal fat(Reference Park, Heymsfield and Gallagher41, Reference Pouliot, Despres and Lemieux42), which is suggested to be the most harmful fat deposit from a metabolic perspective(Reference Pouliot, Despres and Lemieux42). To our knowledge, only a few epidemiological studies have formerly assessed TFA intake in relation to abdominal fat accumulation – with poorer measures of intra-abdominal fat – and the findings have been contradictive(Reference Koh-Banerjee, Chu and Spiegelman43, Reference Merchant, Anand and Vuksan44). A former study in human subjects has reported a significant but small waist gain of 0·77 cm/2 % increment in energy intake from any TFA source(Reference Koh-Banerjee, Chu and Spiegelman43). Similarly, TFA intake tended to increase WC more than a control fat in healthy overweight postmenopausal women, while the deposition of abdominal and liver fat did not differ(Reference Bendsen, Chabanova and Thomsen7). A randomised controlled trial in monkeys showed that a 6-year-long I-TFA-rich diets (approximately 8 % of energy) resulted in a significant increase in intra-abdominal fat mass(Reference Kavanagh, Jones and Sawyer6). Since energy intake was controlled in the latter trial, authors have concluded that TFA consumption might affect metabolism and adipogenesis. However, well-documented biological mechanisms behind the potential abdominal obesity-inducing effect of TFA are lacking. The difficulties in extrapolating from animal experiments to human subjects and the fact that the intake of I-TFA in the trial on monkey was extremely high compared with assumed average intake in populations may explain why the cited results were not confirmed in the present paper.
In the present study, no clear associations between TFA and levels of IL-6 or C-reactive protein were found. The findings conflict with the evidence from observational studies indicating that TFA consumption increases the levels of the pro-inflammatory markers IL-6 and C-reactive protein among overweight women(Reference Lopez-Garcia, Schulze and Meigs45, Reference Mozaffarian, Pischon and Hankinson46). Further studies within this area are warranted, but the cited literature and the present findings may suggest that TFA primarily induces inflammation in already obese individuals with high TFA intake.
The most well-documented effect of I-TFA on CHD risk markers is the effect on serum lipids(Reference Micha and Mozaffarian1). In the present study, the relatively low I-TFA intake was not associated with lipid levels. In contrast, a meta-analysis of controlled trials – with I-TFA intakes ranging from 0·0 to 10·9 % of total energy – found a negative impact on cholesterol homeostasis(Reference Mensink, Zock and Kester4). Similarly, in a prospective observational study, increasing TFA intake (mean intake 3·0 g/d) was associated with an increase in LDL-cholesterol and a decrease in HDL-cholesterol levels(Reference Sun, Ma and Campos47). In the present study, R-TFA was not associated with serum lipids either. Consistent with this, two recent cross-over, randomised, controlled trials demonstrated that high levels of R-TFA (approximately 10 g/d) affect cholesterol homeostasis negatively, whereas moderate intakes had neutral effects(Reference Chardigny, Destaillats and Malpuech-Brugere10, Reference Motard-Belanger, Charest and Grenier11).
We found no association between intake of TFA of either source and systolic and diastolic blood pressure, in accordance with former intervention studies of even higher intake(Reference Mensink, de Louw and Katan48, Reference Raff, Tholstrup and Sejrsen49).
Also, no association with HbA1c was observed, whereas a trend towards a positive association between R-TFA and insulin sensitivity index was seen. A very high intake of TFA has formerly been demonstrated to affect insulin sensitivity in short-term trials of obese subjects with or without diabetes(Reference Lefevre, Lovejoy and Smith50–Reference Christiansen, Schnider and Palmvig52), whereas lower intake of TFA intake was not associated with insulin resistance among abdominal obese women(Reference Tardy, Lambert-Porcheron and Malpuech-Brugere53), overweight men and women(Reference Lovejoy, Champagne and Smith54) or healthy subjects(Reference Lovejoy, Smith and Champagne55). Epidemiological data on the risk of type 2 diabetes in human subjects following a high intake of TFA are conflicting(Reference Lefevre, Lovejoy and Smith50, Reference Hu, Manson and Stampfer56–Reference van Dam, Willett and Rimm59). In monkeys, Kavanagh et al. (Reference Kavanagh, Jones and Sawyer6) demonstrated that high TFA consumption for 6 years changed insulin sensitivity through impaired glucose disposal. Potentially, both level and duration of TFA exposure and underlying predisposition to insulin resistance influence the effect of TFA on glucose homeostasis.
In conclusion, our cross-sectional study on healthy men representing a broad range of BMI suggests that variation around a relatively low contribution of TFA to energy intake is not associated with a panel of cardiovascular risk markers – in contrast to earlier findings from high-dose intervention trials of selected subpopulations. We hypothesise that the level and duration of TFA intake as well as the individual's health stage influence the effect of TFA on risk markers of CHD and that the out-phasing of I-TFA in Denmark has had a positive impact on health at the population level. Future studies from countries where similar restrictions are introduced should assess this hypothesis.
Acknowledgements
The present study was carried out as part of the research programme of the Danish Obesity Research Centre (DanORC, see www.danorc.dk). DanORC is supported by the Danish Council for Strategic Research (grant no. 2101-06-0005). The authors declare that they have no conflicts of interest in relation to the present study. T. I. A. S. initiated, designed, coordinated and, among others, conducted the initial draft board study and the follow-up studies. A. A. and T. I. A. S. conceived the present follow-up examination. The present study was initiated by T. J. in collaboration with M. U. J. and T. I. A. S.; M. M. N. and C. J. N. examined the dietary data and program for errors and conducted the initial analyses; M. M. N performed further analyses under the supervision of C. H.; M. U. J., T. I. A. S. and T. J. helped to interpret the results; M. M. N. drafted the manuscript, which was further edited by all co-authors and finished by B. M. N.; M. M. N. and T. J. have the primary responsibility for the final content. All authors contributed to and accepted the final manuscript. We thank Dr Eva Black, PhD for her assistance in collection of the follow-up data and professor Berit L. Heitmann is thanked for her valuable inputs through the conduct of the present study. B. M. N. and M. M. N. contributed equally to this work.





