55 results
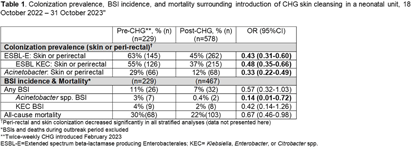
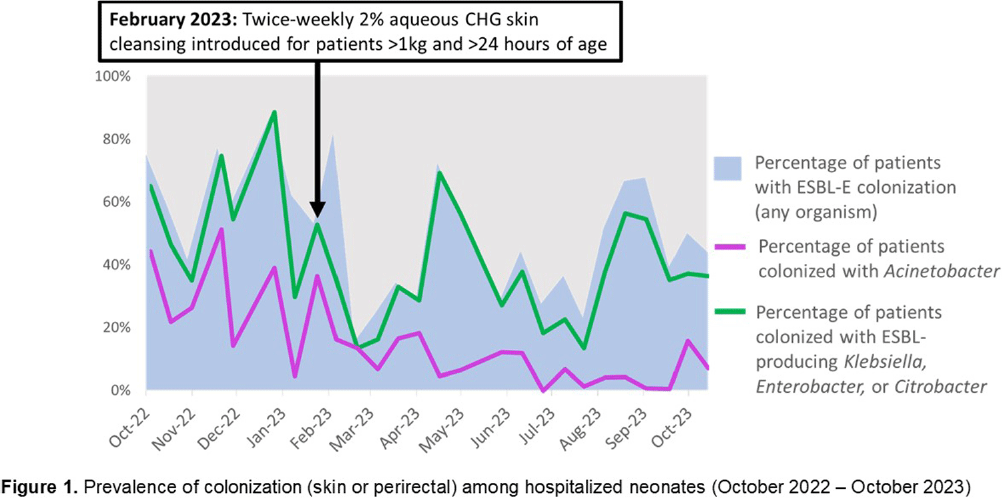
Temporal decreases in pathogen colonization and infection among hospitalized neonates following routine skin antisepsis with chlorhexidine gluconate: Botswana 2022 – 2023
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s12
-
- Article
-
- You have access
- Open access
- Export citation
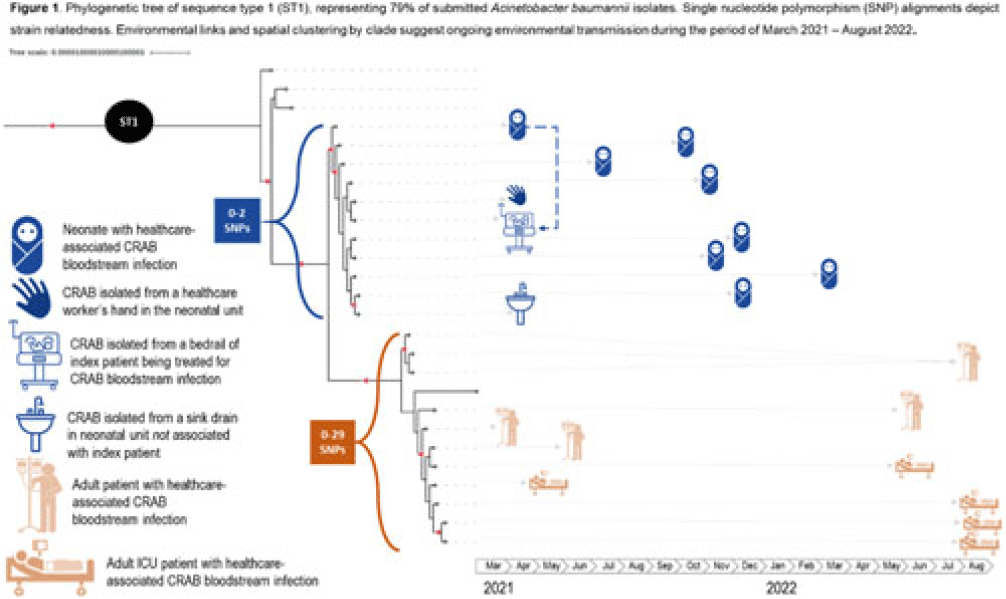
Hyperendemic carbapenem-resistant Acinetobacter baumannii at a hospital in Botswana: Insights from whole-genome sequencing
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s115-s116
-
- Article
-
- You have access
- Open access
- Export citation
Healthcare-associated respiratory syncytial virus infections in children’s hospitals
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s61
-
- Article
-
- You have access
- Open access
- Export citation
A national study of antibiotic use in Greek pediatric hematology oncology and bone marrow transplant units
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 26 April 2022, e71
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Evolution of severe acute respiratory coronavirus virus 2 (SARS-CoV-2) seroprevalence among employees of a US academic children’s hospital during coronavirus disease 2019 (COVID-19) pandemic
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 11 / November 2022
- Published online by Cambridge University Press:
- 02 December 2021, pp. 1647-1655
- Print publication:
- November 2022
-
- Article
- Export citation
The utility of paired upper and lower respiratory tract sampling for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) testing in patients with artificial airways
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 10 / October 2022
- Published online by Cambridge University Press:
- 10 May 2021, pp. 1482-1484
- Print publication:
- October 2022
-
- Article
- Export citation
Pediatric research priorities in healthcare-associated infections and antimicrobial stewardship
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 5 / May 2021
- Published online by Cambridge University Press:
- 26 November 2020, pp. 519-522
- Print publication:
- May 2021
-
- Article
- Export citation
Room for Improvement: Results of a Baseline Evaluation of Environmental Cleaning in a Resource-Limited Neonatal Unit
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s50-s51
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
The Burden of Gastroenteritis Outbreaks in Long-Term Care Settings in Philadelphia, 2009–2018
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s404
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
A Collaborative Public Health and Veterinary Facility Approach to an NDM-5 Escherichia coli Outbreak
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s452-s453
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Implementation of the Comprehensive Unit-Based Safety Program to Improve Hand Hygiene in Four NICUs in Pune, India
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s8-s10
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Site Visits Reveal Common Gaps in Instrument Reprocessing and Sterilization at Philadelphia Dental Clinics
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s389-s390
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
The burden of gastroenteritis outbreaks in long-term care settings in Philadelphia, 2009–2018
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 11 / November 2020
- Published online by Cambridge University Press:
- 17 August 2020, pp. 1310-1314
- Print publication:
- November 2020
-
- Article
- Export citation
The timing and redosing of perioperative antimicrobial prophylaxis in Greek children
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 11 / November 2019
- Published online by Cambridge University Press:
- 17 September 2019, pp. 1318-1319
- Print publication:
- November 2019
-
- Article
- Export citation
Inappropriate intravenous antimicrobial starts: An antimicrobial stewardship metric for hemodialysis facilities
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 10 / October 2019
- Published online by Cambridge University Press:
- 29 July 2019, pp. 1178-1180
- Print publication:
- October 2019
-
- Article
- Export citation
Threatened efficiency not autonomy: Prescriber perceptions of an established pediatric antimicrobial stewardship program
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 5 / May 2019
- Published online by Cambridge University Press:
- 28 March 2019, pp. 522-527
- Print publication:
- May 2019
-
- Article
- Export citation
Infections after pediatric ambulatory surgery: Incidence and risk factors
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 2 / February 2019
- Published online by Cambridge University Press:
- 30 January 2019, pp. 150-157
- Print publication:
- February 2019
-
- Article
- Export citation
Variability in antimicrobial use in pediatric ventilator-associated events
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 1 / January 2019
- Published online by Cambridge University Press:
- 09 November 2018, pp. 32-39
- Print publication:
- January 2019
-
- Article
- Export citation
Surveillance for central-line–associated bloodstream infections: Accuracy of different sampling strategies
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 39 / Issue 10 / October 2018
- Published online by Cambridge University Press:
- 29 August 2018, pp. 1210-1215
- Print publication:
- October 2018
-
- Article
- Export citation
Development of a novel prevention bundle for pediatric healthcare-associated viral infections
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 39 / Issue 9 / September 2018
- Published online by Cambridge University Press:
- 20 July 2018, pp. 1086-1092
- Print publication:
- September 2018
-
- Article
- Export citation