218 results
Scaling up the task-sharing of psychological therapies: A formative study of the PEERS smartphone application for supervision and quality assurance in rural India
-
- Journal:
- Cambridge Prisms: Global Mental Health / Volume 11 / 2024
- Published online by Cambridge University Press:
- 05 February 2024, e20
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Subsurface scientific exploration of extraterrestrial environments (MINAR 5): analogue science, technology and education in the Boulby Mine, UK – CORRIGENDUM
-
- Journal:
- International Journal of Astrobiology / Volume 23 / 2024
- Published online by Cambridge University Press:
- 06 November 2023, e2
-
- Article
-
- You have access
- HTML
- Export citation
Challenges and Factors Affecting Child, Adolescents, Young Adults, and Their Parents in Returning to School After Remote Learning in COVID Pandemic
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S406-S407
-
- Article
-
- You have access
- Open access
- Export citation
A parametric design approach for multi-lobed hybrid airships
-
- Journal:
- The Aeronautical Journal / Volume 128 / Issue 1319 / January 2024
- Published online by Cambridge University Press:
- 11 May 2023, pp. 1-36
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Glacier inventory and glacier changes (1994–2020) in the Upper Alaknanda Basin, Central Himalaya
-
- Journal:
- Journal of Glaciology / Volume 69 / Issue 275 / June 2023
- Published online by Cambridge University Press:
- 13 December 2022, pp. 591-606
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Estimating severe acute respiratory coronavirus virus 2 (SARS-CoV-2) seroprevalence from residual clinical blood samples, January–March 2021
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 22 September 2022, e159
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Bullying victimization in children and adolescents and its impact on academic outcomes
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S144
-
- Article
-
- You have access
- Open access
- Export citation
Bright Light Therapy for MDD in Children and Adolescents: a narrative review of literature
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S554
-
- Article
-
- You have access
- Open access
- Export citation
Decreased mortality in coronavirus disease 2019 associated mucormycosis with aspirin use: a retrospective cohort study
-
- Journal:
- The Journal of Laryngology & Otology / Volume 136 / Issue 12 / December 2022
- Published online by Cambridge University Press:
- 14 June 2022, pp. 1309-1313
- Print publication:
- December 2022
-
- Article
- Export citation
Feasibility, acceptability and evaluation of meditation to augment yoga practice among persons diagnosed with schizophrenia
-
- Journal:
- Acta Neuropsychiatrica / Volume 34 / Issue 6 / December 2022
- Published online by Cambridge University Press:
- 19 May 2022, pp. 330-343
-
- Article
- Export citation
These Are Not the Droids You Are Looking For: Mechanical Variant of Cotard’s Syndrome
-
- Journal:
- CNS Spectrums / Volume 27 / Issue 2 / April 2022
- Published online by Cambridge University Press:
- 28 April 2022, p. 228
-
- Article
-
- You have access
- Export citation
Preliminary assessment of paediatric electrophysiology cardiac implantable electronic device resources around the world
-
- Journal:
- Cardiology in the Young / Volume 32 / Issue 12 / December 2022
- Published online by Cambridge University Press:
- 01 April 2022, pp. 1989-1993
-
- Article
- Export citation
Here Comes Everybody: Using a Data Cooperative to Understand the New Dynamics of Representation
-
- Journal:
- PS: Political Science & Politics / Volume 55 / Issue 2 / April 2022
- Published online by Cambridge University Press:
- 31 March 2022, pp. 300-302
- Print publication:
- April 2022
-
- Article
- Export citation
Key learnings from Institute for Clinical and Economic Review’s real-world evidence reassessment pilot
-
- Journal:
- International Journal of Technology Assessment in Health Care / Volume 38 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 14 March 2022, e32
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Overview and risk factors for postcraniotomy surgical site infection: A four-year experience
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 31 January 2022, e14
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Occupational exposure to severe acute respiratory coronavirus virus 2 (SARS-CoV-2) and risk of infection among healthcare personnel
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 12 / December 2022
- Published online by Cambridge University Press:
- 06 January 2022, pp. 1785-1789
- Print publication:
- December 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Computed tomography analysis of the anterior ethmoid genu of the frontal recess in non-diseased sinuses
-
- Journal:
- The Journal of Laryngology & Otology / Volume 137 / Issue 2 / February 2023
- Published online by Cambridge University Press:
- 20 December 2021, pp. 169-173
- Print publication:
- February 2023
-
- Article
- Export citation
Prevalence of latent structural heart disease in Nepali schoolchildren
- Part of
-
- Journal:
- Cardiology in the Young / Volume 32 / Issue 7 / July 2022
- Published online by Cambridge University Press:
- 04 November 2021, pp. 1151-1153
-
- Article
- Export citation
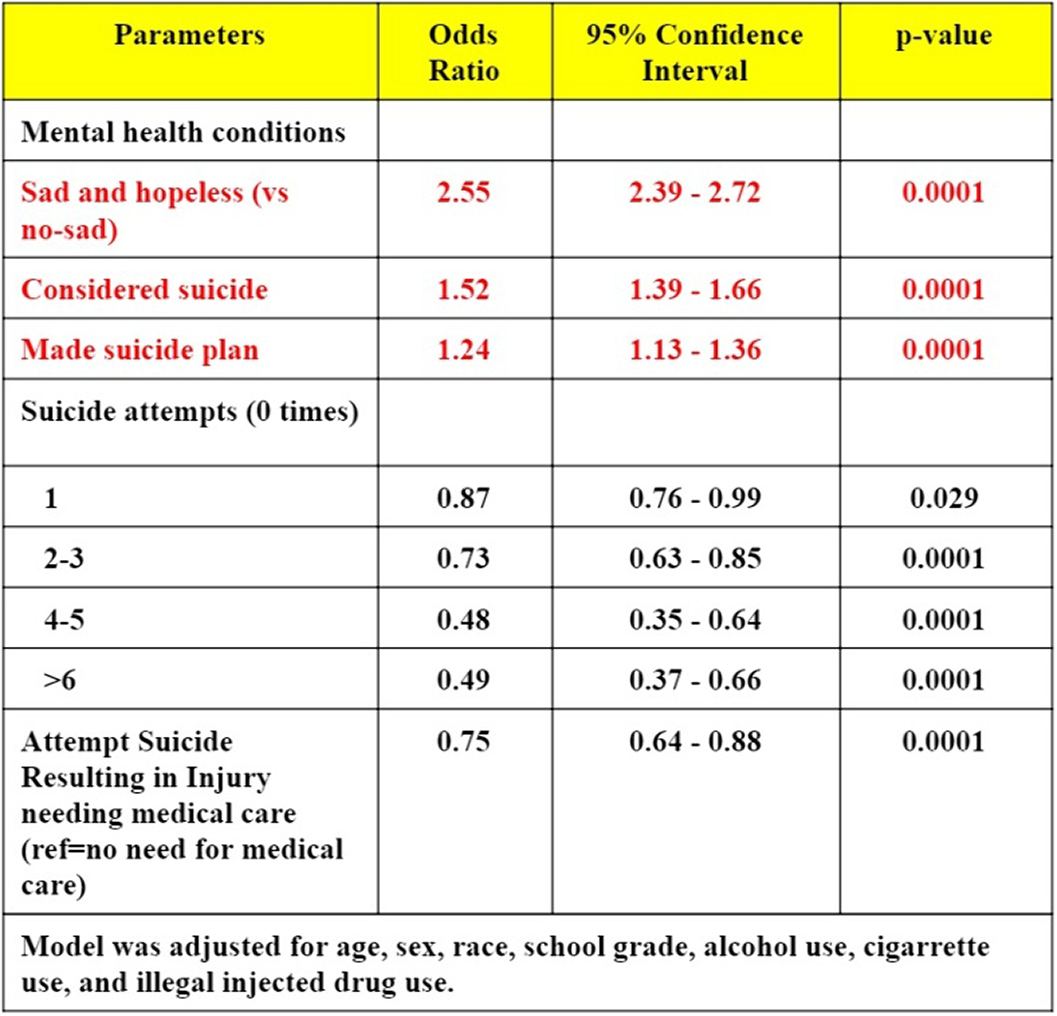
Mood and suicidality amongst cyberbullied adolescents- a cross-sectional study from youth risk behavior survey
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S85-S86
-
- Article
-
- You have access
- Open access
- Export citation
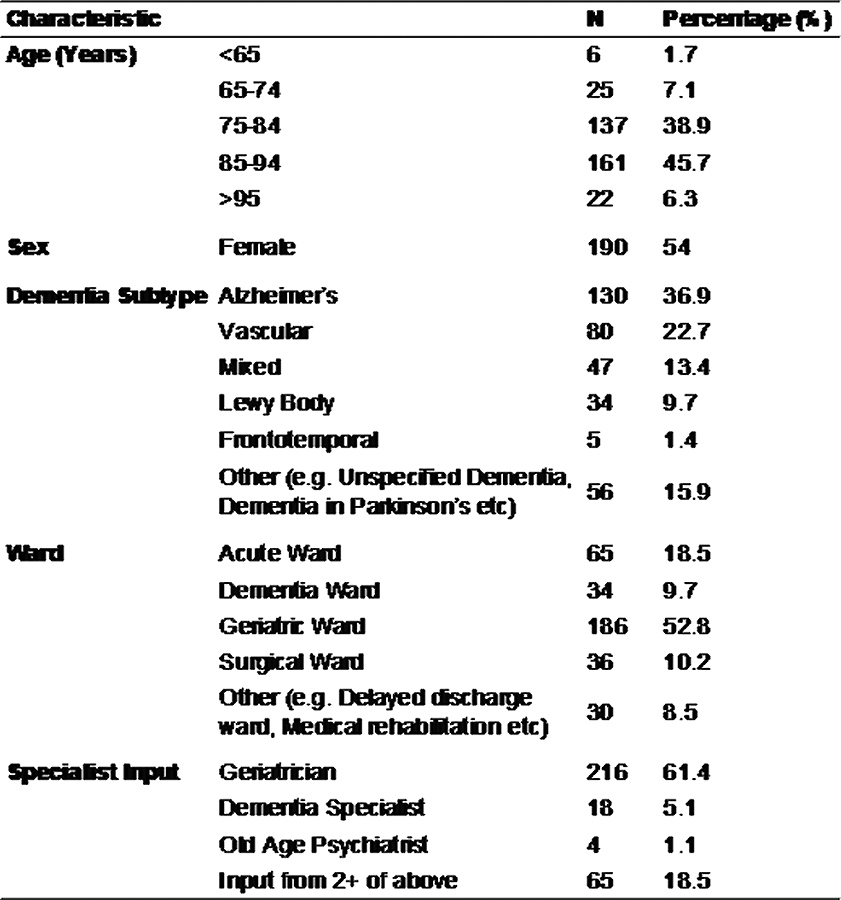
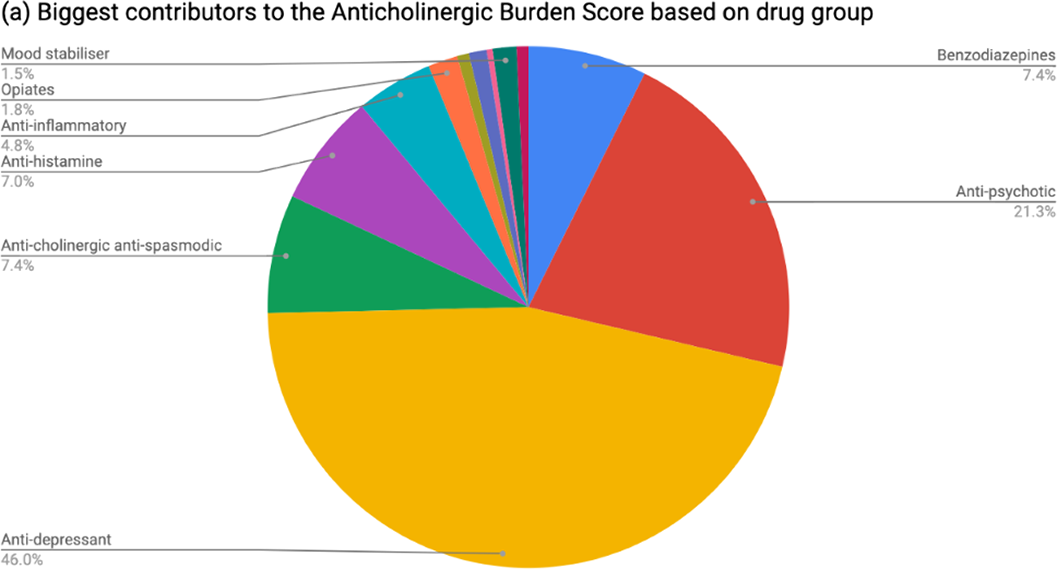
Dementia patients have greater anti-cholinergic drug burden on discharge from hospital: A multicentre cross-sectional study
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S422-S423
-
- Article
-
- You have access
- Open access
- Export citation