82 results
A new species of Ophiocoma (Echinodermata: Ophiuroidea) from Archipelago Trindade and Martin Vaz, Southeastern Atlantic, and redescription of Ophiocoma echinata
-
- Journal:
- Journal of the Marine Biological Association of the United Kingdom / Volume 103 / 2023
- Published online by Cambridge University Press:
- 10 July 2023, e49
-
- Article
- Export citation
Psychosis as alzheimer disease debut: a case report
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S883
-
- Article
-
- You have access
- Open access
- Export citation
Psychiatric Causes of Bariatric Surgery Exclusion: A Descriptive Study
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S586
-
- Article
-
- You have access
- Open access
- Export citation
Prevalence and covid 19 vaccination rate in a population of patients with schizophrenia and a substance use disorder
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S267
-
- Article
-
- You have access
- Open access
- Export citation
Conversion disorder in an 18-year-old boy: a case report
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S398
-
- Article
-
- You have access
- Open access
- Export citation
Schizofrenia: Study of Tendency and Distribution
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S131
-
- Article
-
- You have access
- Open access
- Export citation
Levetirazetam: antiepileptic-induced psychosis
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S732
-
- Article
-
- You have access
- Open access
- Export citation
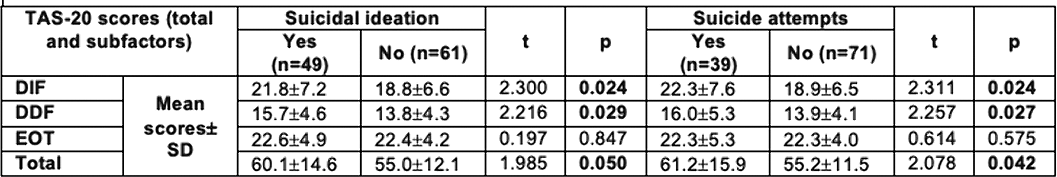
Patients with substance use disorder who have higher alexithymia levels present more suicidality history: Preliminary results in an outpatient addiction treatment center in Spain
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S581-S582
-
- Article
-
- You have access
- Open access
- Export citation
Insomnia at the onset of addiction treatment may be related to earlier relapses: A one-year follow-up study
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S561-S562
-
- Article
-
- You have access
- Open access
- Export citation
The fetal origins of disease: a prospective cohort study on the association of preeclampsia and childhood obesity
-
- Journal:
- Journal of Developmental Origins of Health and Disease / Volume 13 / Issue 1 / February 2022
- Published online by Cambridge University Press:
- 02 March 2021, pp. 68-74
-
- Article
- Export citation
P02-271 - Psychiatric Trainning as a “Rite of Passage”: a Field Study in Spain
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E897
-
- Article
-
- You have access
- Export citation
P03-330 Case Report: Serotonin Syndrome vs Neuroleptic Malignant Syndrom
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E936
-
- Article
-
- You have access
- Export citation
Treatment with glutamatergic drugs in the resistant schizophrenia
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 1447
-
- Article
-
- You have access
- Export citation
Prevalence of paranoid symptomatology in the elderly and relationship to organic brain factors
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 853
-
- Article
-
- You have access
- Export citation
Methodological limitations in research on late psychoses
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 1177
-
- Article
-
- You have access
- Export citation
A Controlled Randomized Study on the Efficacy of Short-Term Dinamic Psychotherapy in Borderline Personality Disorders (BPD). Preliminary Results
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 1040
-
- Article
-
- You have access
- Export citation
P02.324 Diagnosing psychiatric comorbidity in a drug-addiction unit
-
- Journal:
- European Psychiatry / Volume 15 / Issue S2 / October 2000
- Published online by Cambridge University Press:
- 16 April 2020, p. 410s
-
- Article
-
- You have access
- Export citation
Acculturation stress in immigrant population, migratory mourning and associated comorbidities
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 476
-
- Article
-
- You have access
- Export citation
Comorbidity of affective disorders
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 1714
-
- Article
-
- You have access
- Export citation
P01-208-Prevalence of hypomania in patients with diagnosis of affective disorder
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 209
-
- Article
-
- You have access
- Export citation