21 results
The effectiveness of COVID-19 vaccine in the prevention of post-COVID conditions: a systematic literature review and meta-analysis of the latest research
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 13 October 2023, e168
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The effectiveness of coronavirus disease 2019 (COVID-19) vaccine in the prevention of post–COVID-19 conditions: A systematic literature review and meta-analysis
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 06 December 2022, e192
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Coronavirus disease 2019 (COVID-19) among nonphysician healthcare personnel by work location at a tertiary-care center, Iowa, 2020–2021
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 8 / August 2023
- Published online by Cambridge University Press:
- 02 June 2022, pp. 1351-1354
- Print publication:
- August 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The long-term effectiveness of coronavirus disease 2019 (COVID-19) vaccines: A systematic literature review and meta-analysis
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 14 February 2022, e22
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The short-term effectiveness of coronavirus disease 2019 (COVID-19) vaccines among healthcare workers: a systematic literature review and meta-analysis
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 21 October 2021, e33
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Bat intrusions at a tertiary care center in Iowa, 2018–2020
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 12 / December 2022
- Published online by Cambridge University Press:
- 16 August 2021, pp. 1948-1950
- Print publication:
- December 2022
-
- Article
- Export citation
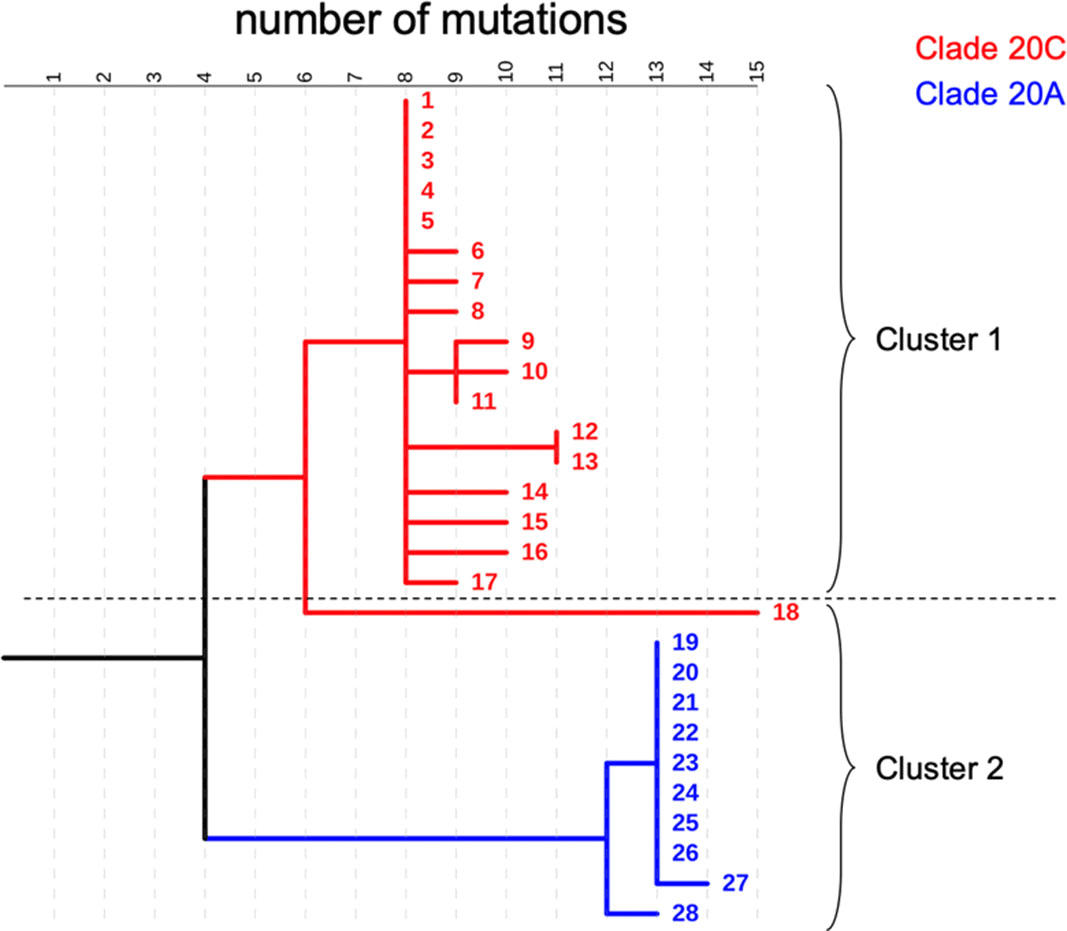
Molecular Epidemiology of Large COVID-19 Clusters at an Academic Medical Center, March–October 2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s10-s11
-
- Article
-
- You have access
- Open access
- Export citation
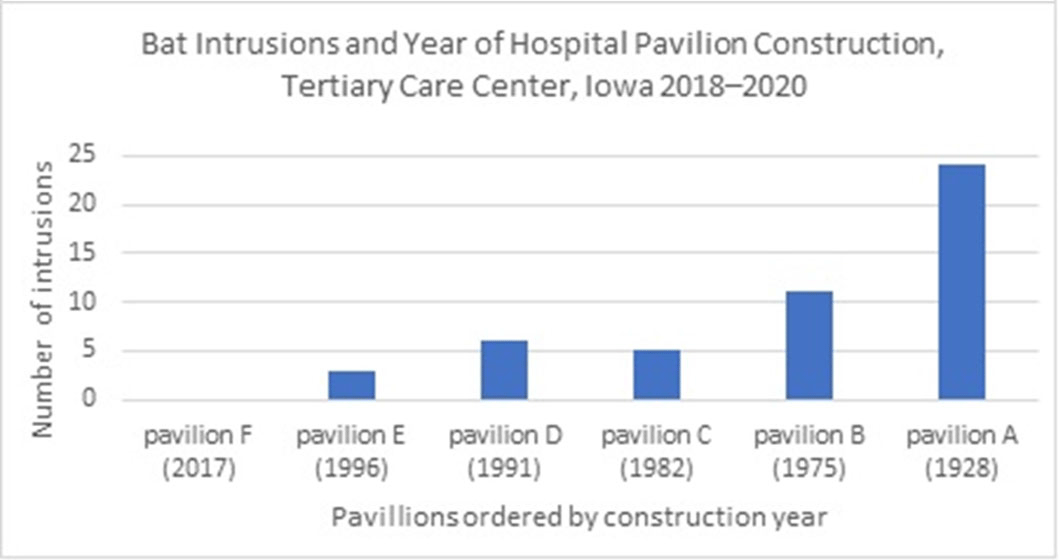
Bat Intrusions at a Tertiary Care Center, Iowa 2018–2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s16
-
- Article
-
- You have access
- Open access
- Export citation
COVID-19 Conversion after Exposure in a Semiprivate Room at a Tertiary Care Center in Iowa, July–December 2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s20-s21
-
- Article
-
- You have access
- Open access
- Export citation
Coronavirus Disease 2019 (COVID-19) Admission Screening at a Tertiary-Care Center, Iowa 2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s1
-
- Article
-
- You have access
- Open access
- Export citation
Suspected COVID-19 Reinfections at a Tertiary Care Center, Iowa 2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s19
-
- Article
-
- You have access
- Open access
- Export citation
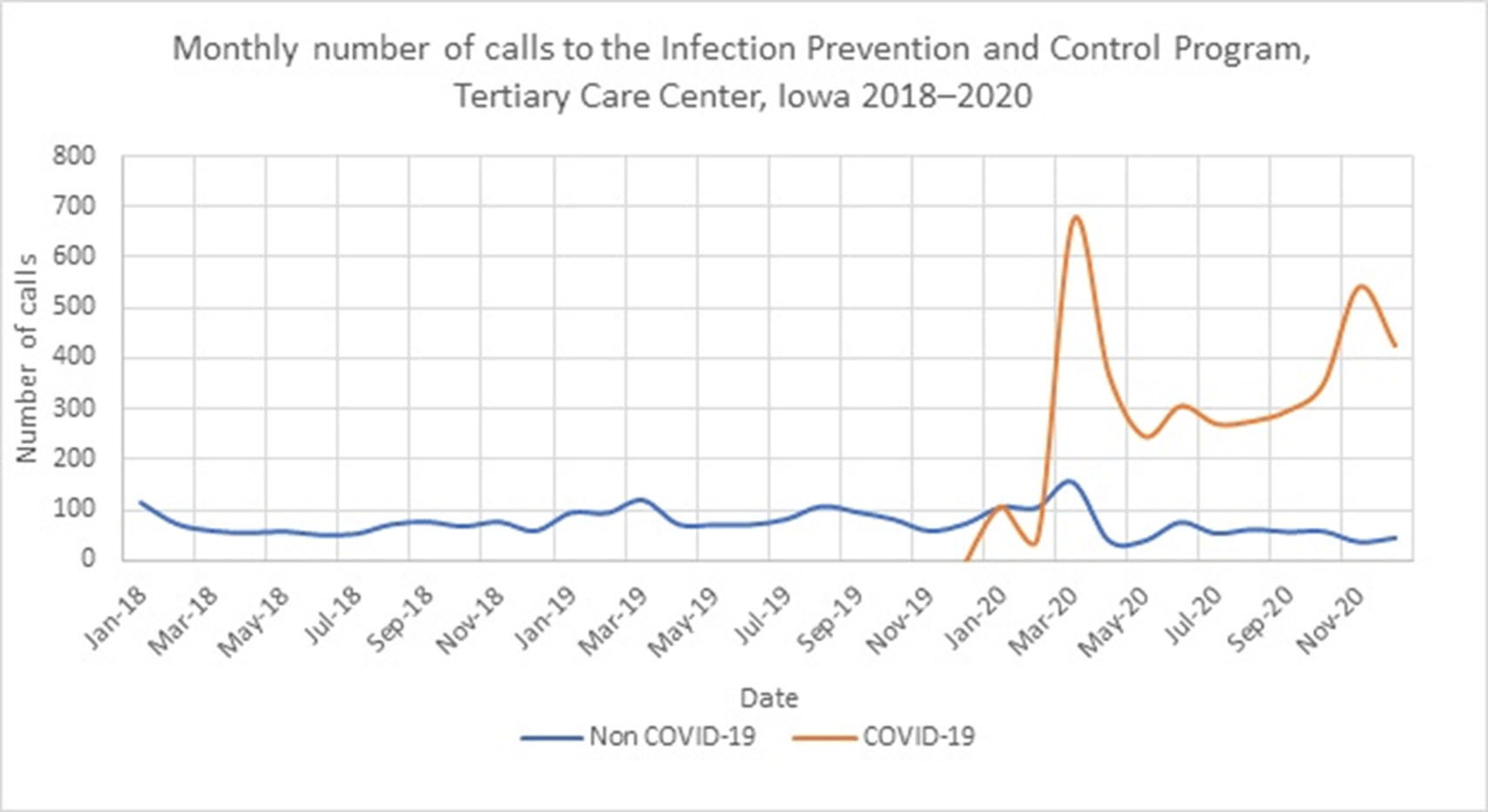
Impact of COVID-19 on Volume of Infection Prevention and Control Calls at a Tertiary-Care Center in Iowa, 2018–2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s53-s54
-
- Article
-
- You have access
- Open access
- Export citation
Coronavirus disease 2019 (COVID-19) incidence after exposures in shared patient rooms in a tertiary-care center in Iowa, July 2020–May 2021
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 12 / December 2022
- Published online by Cambridge University Press:
- 12 July 2021, pp. 1910-1913
- Print publication:
- December 2022
-
- Article
- Export citation
Coronavirus disease 2019 (COVID-19) admission screening and assessment of infectiousness at an academic medical center in Iowa, 2020
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 8 / August 2022
- Published online by Cambridge University Press:
- 24 June 2021, pp. 974-978
- Print publication:
- August 2022
-
- Article
- Export citation
Molecular epidemiology of large coronavirus disease 2019 (COVID-19) clusters before and after the implementation of routine serial testing at an academic medical center in Iowa, 2020
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 12 / December 2021
- Published online by Cambridge University Press:
- 24 June 2021, pp. 1514-1516
- Print publication:
- December 2021
-
- Article
- Export citation
Positive deviance in infection prevention and control: A systematic literature review
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 3 / March 2022
- Published online by Cambridge University Press:
- 11 November 2020, pp. 358-365
- Print publication:
- March 2022
-
- Article
- Export citation
Risk Factors and Mortality in Pediatric Patients with Stenotrophomonas maltophilia Bacteremia
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s374-s375
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Administrative Coding Methods Impact Surgical Site Infection Rates
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s111-s112
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Tuberculosis Exposure and Conversion Rates Can Guide Deimplementation of Annual Tuberculosis Screening
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s419
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Administrative coding methods impact surgical site infection rates
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 12 / December 2020
- Published online by Cambridge University Press:
- 10 August 2020, pp. 1461-1463
- Print publication:
- December 2020
-
- Article
- Export citation