8 results
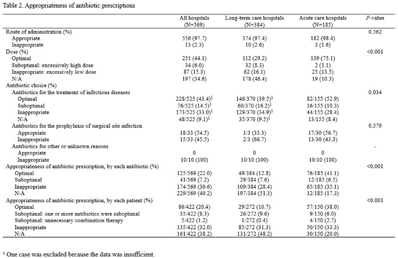
Prescriptions patterns and appropriateness of usage of antibiotics in small and medium- sized hospitals in Korea
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s19
-
- Article
-
- You have access
- Open access
- Export citation
Prevalence of mental illness among COVID-19 survivors in South Korea: nationwide cohort
-
- Journal:
- BJPsych Open / Volume 7 / Issue 6 / November 2021
- Published online by Cambridge University Press:
- 01 October 2021, e183
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Impact on National Policy on the Hand Hygiene Promotion Activities in Hospitals in Korea
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s267
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Differences in the Risk Factors for Surgical Site Infection between Total Hip Arthroplasty and Total Knee Arthroplasty in the Korean Nosocomial Infections Surveillance System (KONIS)
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 33 / Issue 11 / November 2012
- Published online by Cambridge University Press:
- 02 January 2015, pp. 1086-1093
- Print publication:
- November 2012
-
- Article
- Export citation
Prospective Nationwide Surveillance of Surgical Site Infections after Gastric Surgery and Risk Factor Analysis in the Korean Nosocomial Infections Surveillance System (KONIS)
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 33 / Issue 6 / June 2012
- Published online by Cambridge University Press:
- 02 January 2015, pp. 572-580
- Print publication:
- June 2012
-
- Article
-
- You have access
- Export citation
Healthy Twin: A Twin-Family Study of Korea — Protocols and Current Status
-
- Journal:
- Twin Research and Human Genetics / Volume 9 / Issue 6 / 01 December 2006
- Published online by Cambridge University Press:
- 21 February 2012, pp. 844-848
-
- Article
-
- You have access
- Export citation
Development of Blood Compatible Alpha-lipoic acid Coated Stent with a Good Adhesive by Low Temperature Plasma Polymerization
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 1132 / 2008
- Published online by Cambridge University Press:
- 15 March 2011, 1132-Z08-01
- Print publication:
- 2008
-
- Article
- Export citation
Large Field Emission from Vertically Well-aligned Carbon Nanotubes
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 633 / 2000
- Published online by Cambridge University Press:
- 15 March 2011, A14.9
- Print publication:
- 2000
-
- Article
- Export citation