22 results
SHEA NICU white paper series: Practical approaches for the prevention of viral respiratory infections
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 3 / March 2024
- Published online by Cambridge University Press:
- 25 October 2023, pp. 267-276
- Print publication:
- March 2024
-
- Article
-
- You have access
- HTML
- Export citation
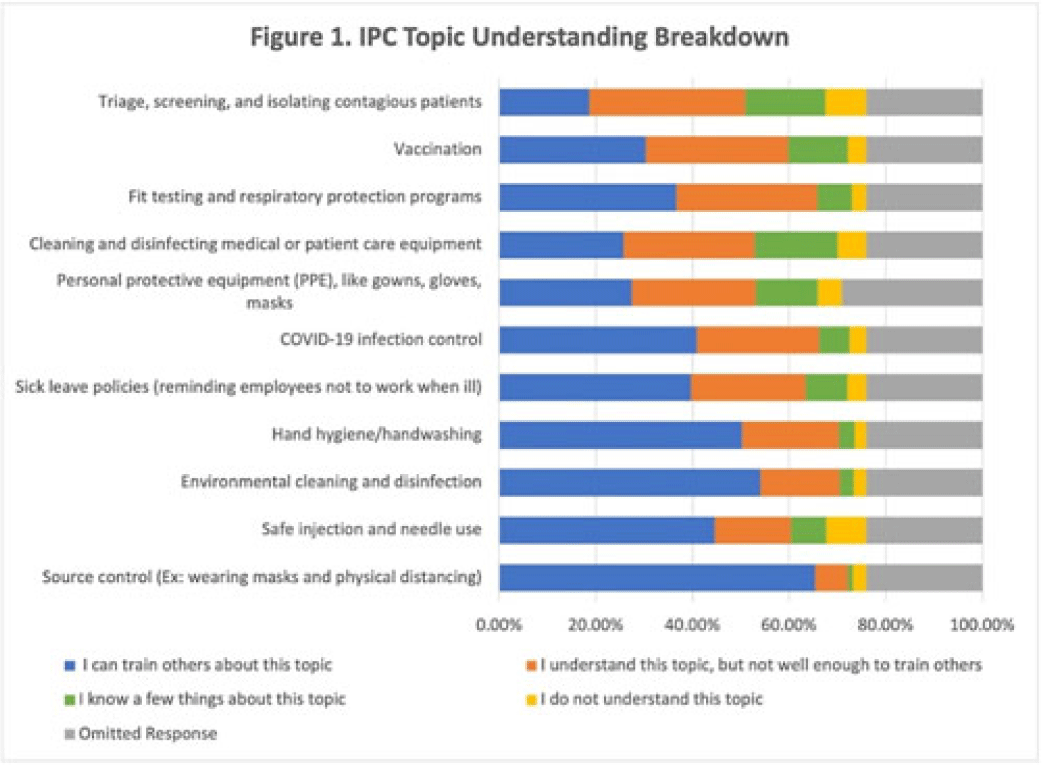
Oregon Project Firstline: A needs assessment of healthcare personnel infection prevention knowledge and training preferences
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s87-s88
-
- Article
-
- You have access
- Open access
- Export citation
Women in epidemiology
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 22 December 2022, e202
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
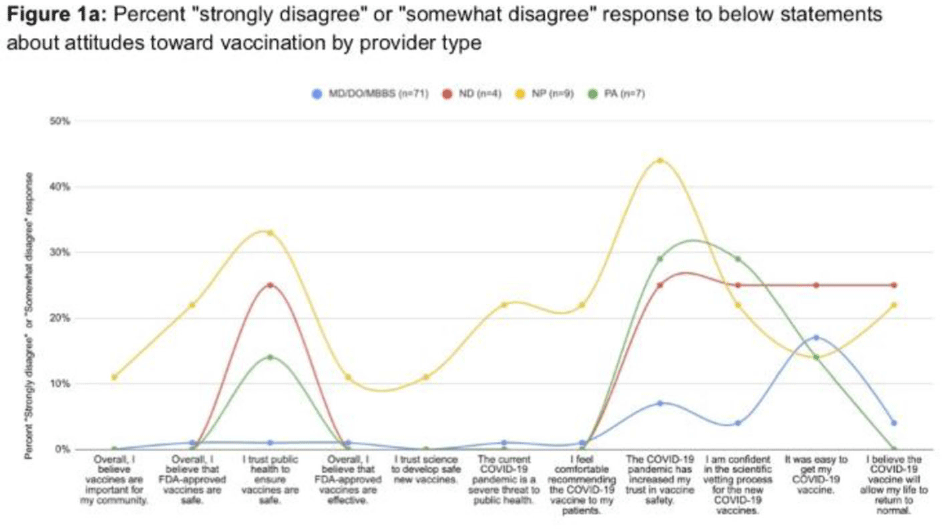
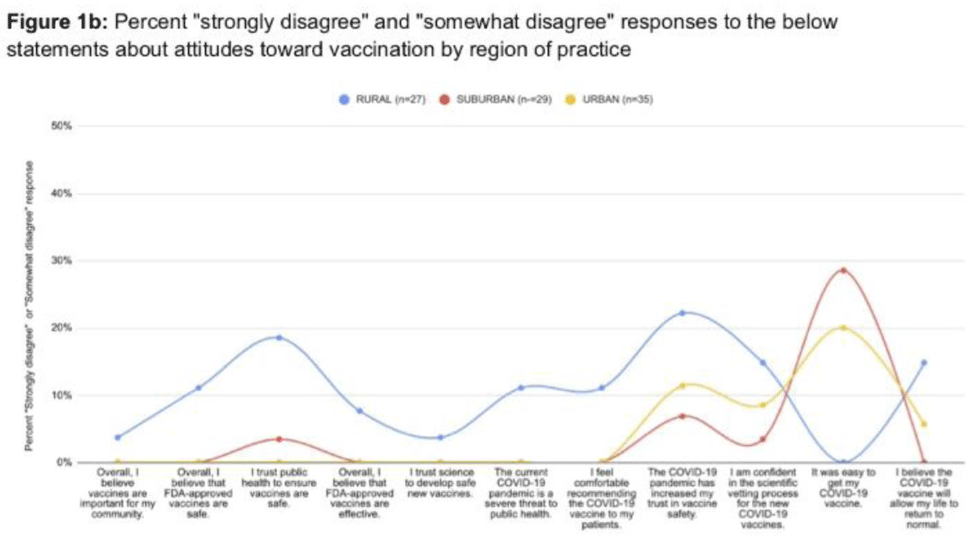
COVID-19 vaccine knowledge, beliefs and attitudes among Oregon healthcare provider types
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s76
-
- Article
-
- You have access
- Open access
- Export citation
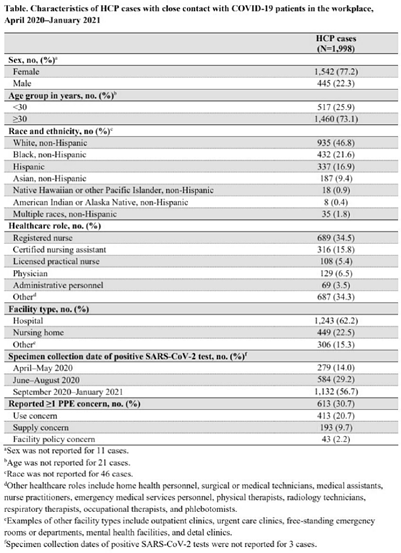
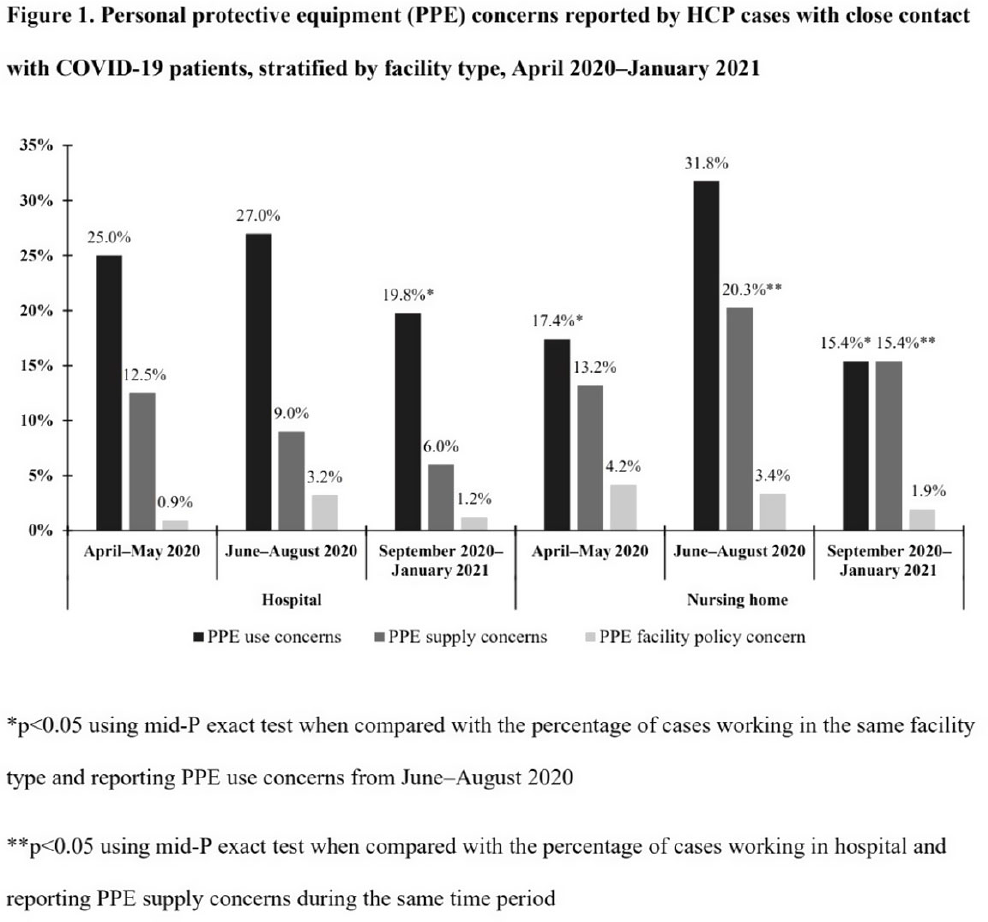
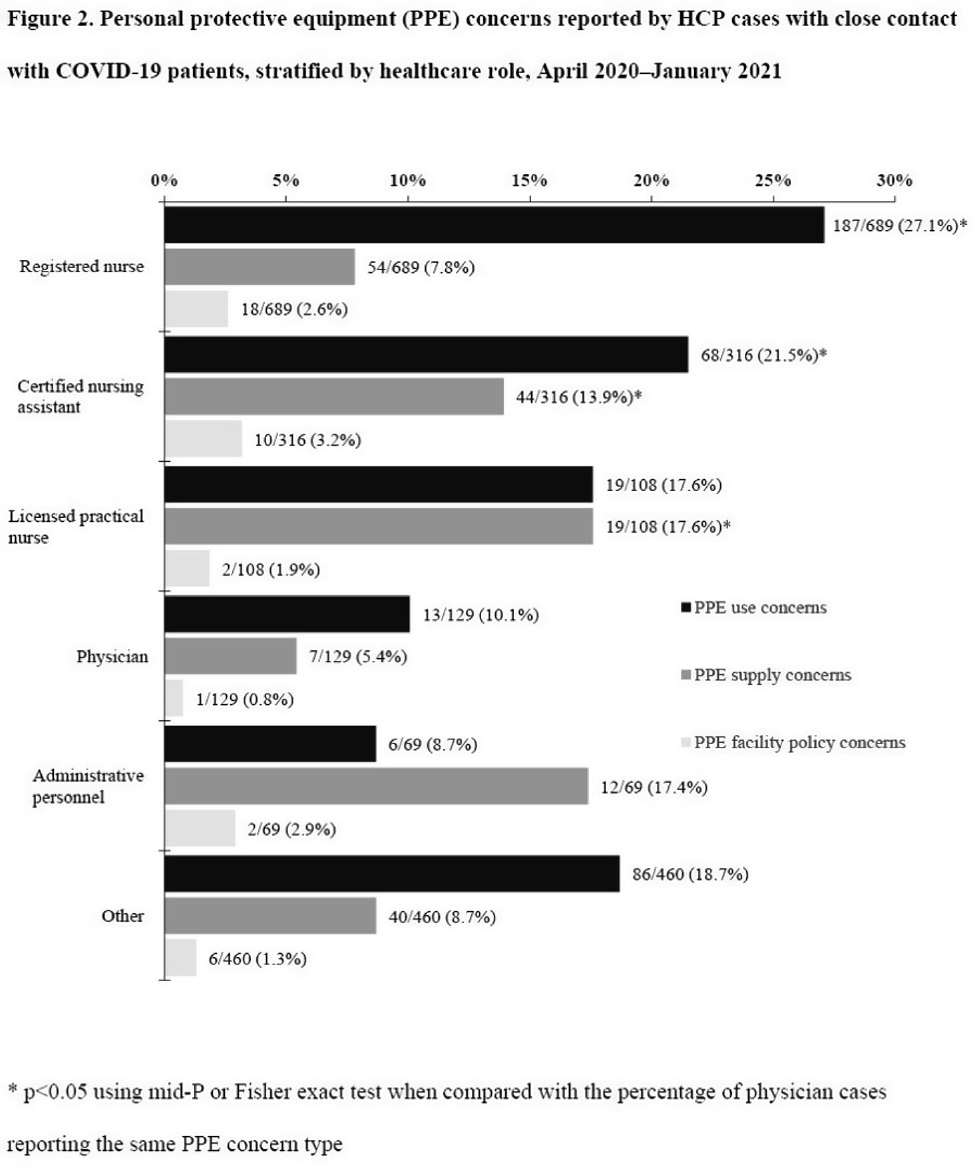
Characteristics of healthcare personnel who reported concerns related to PPE use during care of COVID-19 patients
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s8-s9
-
- Article
-
- You have access
- Open access
- Export citation
SHEA Pediatric Leadership Council commentary: Supporting well child care during the coronavirus disease 2019 (COVID-19) pandemic with personal protective equipment in the ambulatory setting
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 8 / August 2021
- Published online by Cambridge University Press:
- 14 June 2021, pp. 985-988
- Print publication:
- August 2021
-
- Article
- Export citation
SHEA Pediatric Leadership Council commentary: Personal protective equipment during care of children with multisystem inflammatory syndrome in children (MIS-C)
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 9 / September 2021
- Published online by Cambridge University Press:
- 14 June 2021, pp. 1108-1110
- Print publication:
- September 2021
-
- Article
- Export citation
SHEA Pediatric Leadership Council commentary: Ambulatory management of neonates born to mothers infected with severe acute respiratory coronavirus virus 2 (SARS-CoV-2)
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 9 / September 2021
- Published online by Cambridge University Press:
- 04 June 2021, pp. 1105-1107
- Print publication:
- September 2021
-
- Article
- Export citation
Practices and activities among healthcare personnel with severe acute respiratory coronavirus virus 2 (SARS-CoV-2) infection working in different healthcare settings—ten Emerging Infections Program sites, April–November 2020
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 8 / August 2022
- Published online by Cambridge University Press:
- 02 June 2021, pp. 1058-1062
- Print publication:
- August 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Medical facemasks are adequate for healthcare worker safety at outdoor coronavirus disease 2019 (COVID-19) drive-through testing centers
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 3 / March 2022
- Published online by Cambridge University Press:
- 12 January 2021, pp. 411-413
- Print publication:
- March 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Local, state and federal face mask mandates during the COVID-19 pandemic
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 4 / April 2021
- Published online by Cambridge University Press:
- 05 January 2021, pp. 455-456
- Print publication:
- April 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Pediatric research priorities in healthcare-associated infections and antimicrobial stewardship
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 5 / May 2021
- Published online by Cambridge University Press:
- 26 November 2020, pp. 519-522
- Print publication:
- May 2021
-
- Article
- Export citation
Service, science, and fortitude: Our thanks and salute to Dr. Anthony S. Fauci, October 2020
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 3 / March 2021
- Published online by Cambridge University Press:
- 05 November 2020, p. 331
- Print publication:
- March 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Preparing nursing homes for a second wave of coronavirus disease 2019 (COVID-19)
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 10 / October 2021
- Published online by Cambridge University Press:
- 20 October 2020, pp. 1251-1254
- Print publication:
- October 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Organizational strategies for managing COVID-19 survivors who return for care
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 3 / March 2021
- Published online by Cambridge University Press:
- 09 September 2020, pp. 332-333
- Print publication:
- March 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Whither immunity? The search for effective, durable immunity to coronavirus disease 2019 (COVID-19)
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 2 / February 2021
- Published online by Cambridge University Press:
- 04 September 2020, pp. 205-207
- Print publication:
- February 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The perplexing problem of persistently PCR-positive personnel
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 2 / February 2021
- Published online by Cambridge University Press:
- 20 July 2020, pp. 203-204
- Print publication:
- February 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Universal pandemic precautions—An idea ripe for the times
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 11 / November 2020
- Published online by Cambridge University Press:
- 03 July 2020, pp. 1321-1322
- Print publication:
- November 2020
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Shifting sands—Molecular coronavirus testing during a time of inconsistent resources
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 10 / October 2020
- Published online by Cambridge University Press:
- 05 June 2020, pp. 1190-1191
- Print publication:
- October 2020
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Outbreak Response and Incident Management: SHEA Guidance and Resources for Healthcare Epidemiologists in United States Acute-Care Hospitals
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 38 / Issue 12 / December 2017
- Published online by Cambridge University Press:
- 30 November 2017, pp. 1393-1419
- Print publication:
- December 2017
-
- Article
-
- You have access
- HTML
- Export citation