22 results
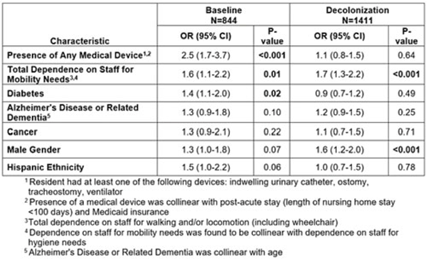
Does universal nasal/skin decolonization in nursing homes affect risk factors for MRSA carriage?
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s78
-
- Article
-
- You have access
- Open access
- Export citation
Post-discharge decolonization of patients harboring methicillin-resistant Staphylococcus aureus (MRSA) USA300 strains: secondary analysis of the CLEAR Trial
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 2 / February 2023
- Published online by Cambridge University Press:
- 16 December 2021, pp. 315-318
- Print publication:
- February 2023
-
- Article
- Export citation
Double-swab 5% versus single-swab 10% iodophor for reducing methicillin-resistant Staphylococcus aureus with routine chlorhexidine bathing
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 12 / December 2022
- Published online by Cambridge University Press:
- 26 August 2021, pp. 1937-1939
- Print publication:
- December 2022
-
- Article
- Export citation
Impact of empiric antibiotics for methicillin-resistant Staphylococcus aureus (MRSA) infection and associated Clostridioides difficile infection (CDI) risk: Secondary analysis of the CLEAR trial
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 12 / December 2021
- Published online by Cambridge University Press:
- 16 April 2021, pp. 1493-1496
- Print publication:
- December 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Cost Savings Associated With Decolonization of Postdischarge MRSA Carriers: Results From the CLEAR Randomized Trial
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s28-s29
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Universal Decolonization Reduces MDRO Burden on High-Touch Objects in Nursing Home Resident Rooms and Common Areas
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s54-s55
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Impact of Roommates on MDRO Spread in Nursing Homes
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s66-s67
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Decreased Hospitalizations and Costs From Infection in Sixteen Nursing Homes in the SHIELD OC Regional Decolonization Initiative
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s7-s8
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Unintended Consequences of MRSA Infection: Empiric Non-MRSA Antibiotic Use and Resultant Clostridioides difficile Infection
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s421-s422
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Tracking the spread of carbapenem-resistant Enterobacteriaceae (CRE) through clinical cultures alone underestimates the spread of CRE even more than anticipated
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 6 / June 2019
- Published online by Cambridge University Press:
- 28 March 2019, pp. 731-734
- Print publication:
- June 2019
-
- Article
- Export citation
Practical methods for effective vancomycin-resistant enterococci (VRE) surveillance: experience in a liver transplant surgical intensive care unit
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 39 / Issue 10 / October 2018
- Published online by Cambridge University Press:
- 05 September 2018, pp. 1178-1182
- Print publication:
- October 2018
-
- Article
- Export citation
The Economic Value of the Centers for Disease Control and Prevention Carbapenem-Resistant Enterobacteriaceae Toolkit
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 39 / Issue 5 / May 2018
- Published online by Cambridge University Press:
- 19 March 2018, pp. 516-524
- Print publication:
- May 2018
-
- Article
- Export citation
Secular Trends in Nosocomial Vancomycin-Resistant Enterococcal Bloodstream Infections Among United States Veterans Affairs Hospitals, Fiscal Years 2004 through 2014
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 38 / Issue 9 / September 2017
- Published online by Cambridge University Press:
- 11 July 2017, pp. 1114-1116
- Print publication:
- September 2017
-
- Article
- Export citation
Prevalence of and Factors Associated With Multidrug Resistant Organism (MDRO) Colonization in 3 Nursing Homes
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 37 / Issue 12 / December 2016
- Published online by Cambridge University Press:
- 27 September 2016, pp. 1485-1488
- Print publication:
- December 2016
-
- Article
- Export citation
Reply to O’Riordan et al
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 36 / Issue 7 / July 2015
- Published online by Cambridge University Press:
- 17 June 2015, pp. 857-858
- Print publication:
- July 2015
-
- Article
-
- You have access
- HTML
- Export citation
Cost-Benefit Analysis from the Hospital Perspective of Universal Active Screening Followed by Contact Precautions for Methicillin-Resistant Staphylococcus aureus Carriers
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 36 / Issue 1 / January 2015
- Published online by Cambridge University Press:
- 05 January 2015, pp. 2-13
- Print publication:
- January 2015
-
- Article
- Export citation
Survey of Preoperative Infection Prevention for Coronary Artery Bypass Graft Procedures
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 35 / Issue 6 / 01 June 2014
- Published online by Cambridge University Press:
- 10 May 2016, pp. 736-737
- Print publication:
- 01 June 2014
-
- Article
- Export citation
Variation in Antibiotic Prophylaxis Selection for Coronary Artery Bypass Graft Procedures in an Era of Increasing Methicillin-Resistant Staphylococcus aureus Prevalence
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 35 / Issue 6 / 01 June 2014
- Published online by Cambridge University Press:
- 10 May 2016, pp. 737-740
- Print publication:
- 01 June 2014
-
- Article
- Export citation
A Systematic Literature Review and Meta-Analysis of Factors Associated with Methicillin-Resistant Staphylococcus aureus Colonization at Time of Hospital or Intensive Care Unit Admission
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 34 / Issue 10 / October 2013
- Published online by Cambridge University Press:
- 02 January 2015, pp. 1077-1086
- Print publication:
- October 2013
-
- Article
- Export citation
Quantifying the Impact of Extranasal Testing of Body Sites for Methicillin-Resistant Staphylococcus aureus Colonization at the Time of Hospital or Intensive Care Unit Admission
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 34 / Issue 2 / February 2013
- Published online by Cambridge University Press:
- 02 January 2015, pp. 161-170
- Print publication:
- February 2013
-
- Article
- Export citation