24 results
Letter to the Editor: Disentangling cause and effect in the relationship between cannabis and psychosis: are we there yet?
-
- Journal:
- Psychological Medicine / Volume 46 / Issue 14 / October 2016
- Published online by Cambridge University Press:
- 25 July 2016, pp. 3061-3062
-
- Article
-
- You have access
- HTML
- Export citation
Hurricane Katrina's First Responders: The Struggle to Protect and Serve in the Aftermath of the Disaster
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 5 / Issue S2 / September 2011
- Published online by Cambridge University Press:
- 08 April 2013, pp. S214-S219
-
- Article
- Export citation
Bilateral, simultaneous cochlear implantation in children: surgical considerations
-
- Journal:
- The Journal of Laryngology & Otology / Volume 123 / Issue 8 / August 2009
- Published online by Cambridge University Press:
- 08 March 2017, pp. 837-839
- Print publication:
- August 2009
-
- Article
- Export citation
Mediastinal dissection in head and neck cancer
-
- Journal:
- The Journal of Laryngology & Otology / Volume 120 / Issue 10 / October 2006
- Published online by Cambridge University Press:
- 24 July 2006, pp. 865-867
- Print publication:
- October 2006
-
- Article
- Export citation
Neurodevelopmental outcome in children born to mothers with hypertension in pregnancy: the significance of suboptimal intrauterine growth
-
- Journal:
- Developmental Medicine and Child Neurology / Volume 48 / Issue 3 / March 2006
- Published online by Cambridge University Press:
- 17 February 2006, pp. 200-206
- Print publication:
- March 2006
-
- Article
- Export citation
Electron Cryo-microscopy and Image Reconstruction of Adeno-Associated Virus Type 2 empty Capsids
-
- Journal:
- Microscopy and Microanalysis / Volume 8 / Issue S02 / August 2002
- Published online by Cambridge University Press:
- 01 August 2002, pp. 212-213
- Print publication:
- August 2002
-
- Article
-
- You have access
- Export citation
Suprameatal approach: new surgical approach for cochlear implantation
-
- Journal:
- The Journal of Laryngology & Otology / Volume 115 / Issue 4 / April 2001
- Published online by Cambridge University Press:
- 08 March 2006, pp. 283-285
- Print publication:
- April 2001
-
- Article
- Export citation
Evidence for a major gene accounting for mild elevation in LDL cholesterol: The NHLBI Family Heart Study
-
- Journal:
- Annals of Human Genetics / Volume 63 / Issue 5 / September 1999
- Published online by Cambridge University Press:
- 01 September 1999, pp. 401-412
- Print publication:
- September 1999
-
- Article
- Export citation
Sialadenoma papilliferum of the parotid gland
-
- Journal:
- The Journal of Laryngology & Otology / Volume 103 / Issue 11 / November 1989
- Published online by Cambridge University Press:
- 29 June 2007, pp. 1089-1090
- Print publication:
- November 1989
-
- Article
- Export citation
Ad Senecam
-
- Journal:
- The Classical Quarterly / Volume 17 / Issue 1 / January 1923
- Published online by Cambridge University Press:
- 11 February 2009, pp. 42-49
- Print publication:
- January 1923
-
- Article
- Export citation
Ad Epicteti Dissertationes
-
- Journal:
- The Classical Quarterly / Volume 5 / Issue 2 / April 1911
- Published online by Cambridge University Press:
- 11 February 2009, pp. 91-92
- Print publication:
- April 1911
-
- Article
- Export citation
Ad Gellivm
-
- Journal:
- The Classical Quarterly / Volume 4 / Issue 1 / January 1910
- Published online by Cambridge University Press:
- 11 February 2009, pp. 23-24
- Print publication:
- January 1910
-
- Article
- Export citation
Ad Epictetvm
-
- Journal:
- The Classical Quarterly / Volume 3 / Issue 4 / October 1909
- Published online by Cambridge University Press:
- 11 February 2009, pp. 258-265
- Print publication:
- October 1909
-
- Article
- Export citation
Ad Epictetvm1
-
- Journal:
- The Classical Quarterly / Volume 3 / Issue 3 / July 1909
- Published online by Cambridge University Press:
- 11 February 2009, pp. 195-202
- Print publication:
- July 1909
-
- Article
- Export citation
Ad Apvleivm
-
- Journal:
- The Classical Quarterly / Volume 2 / Issue 4 / October 1908
- Published online by Cambridge University Press:
- 11 February 2009, pp. 304-312
- Print publication:
- October 1908
-
- Article
- Export citation
Ad Senecae Dialogos.
-
- Journal:
- The Classical Quarterly / Volume 2 / Issue 1 / January 1908
- Published online by Cambridge University Press:
- 11 February 2009, pp. 34-40
- Print publication:
- January 1908
-
- Article
- Export citation
Ad Senecae Libros De Beneficiis et De Clementia
-
- Journal:
- The Classical Quarterly / Volume 1 / Issue 4 / October 1907
- Published online by Cambridge University Press:
- 11 February 2009, pp. 284-289
- Print publication:
- October 1907
-
- Article
- Export citation
Ad Senecae Epistvlas Morales
-
- Journal:
- The Classical Quarterly / Volume 1 / Issue 2-3 / July 1907
- Published online by Cambridge University Press:
- 11 February 2009, pp. 205-215
- Print publication:
- July 1907
-
- Article
- Export citation
Ad Musonium Rufum
-
- Journal:
- The Classical Review / Volume 20 / Issue 8 / November 1906
- Published online by Cambridge University Press:
- 27 October 2009, pp. 394-395
- Print publication:
- November 1906
-
- Article
- Export citation
Ad Epictetum
-
- Journal:
- The Classical Review / Volume 20 / Issue 2 / March 1906
- Published online by Cambridge University Press:
- 27 October 2009, pp. 104-109
- Print publication:
- March 1906
-
- Article
- Export citation

 (seruorum offensiones et molestias);—
(seruorum offensiones et molestias);—
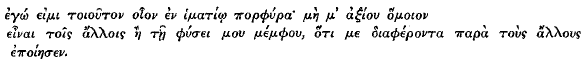 Si ita locutus esset E., profecto Stoicus esse desiisset oblitus
Si ita locutus esset E., profecto Stoicus esse desiisset oblitus 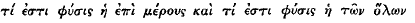 (I 20 16), i.e. quid esset inter naturam meam et naturam. Scio me uocatum iri ad III 1 30
(I 20 16), i.e. quid esset inter naturam meam et naturam. Scio me uocatum iri ad III 1 30 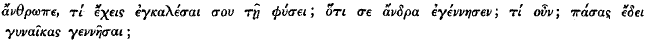 ; sed ego audacter affirmo et teneo non magis hie quam illic ferri posse pronomen (σον, μον); aut quid, rogo, est ‘Quid habes quod accuses naturam tuam, quod natura tua marem te genuit ? Num feminas omnes natura tua gignere debuit?’? Vide quod ex Athenaeo (XIII 565 c) citat editor.
; sed ego audacter affirmo et teneo non magis hie quam illic ferri posse pronomen (σον, μον); aut quid, rogo, est ‘Quid habes quod accuses naturam tuam, quod natura tua marem te genuit ? Num feminas omnes natura tua gignere debuit?’? Vide quod ex Athenaeo (XIII 565 c) citat editor.