11 results
New-onset mental illness and long-term survival in survivors of critical illness: population-based cohort study in South Korea
-
- Journal:
- BJPsych Open / Volume 10 / Issue 2 / March 2024
- Published online by Cambridge University Press:
- 22 March 2024, e70
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Is spiritual well-being related to survival time of inpatients with advanced cancer? An East Asian cohort study
-
- Journal:
- Palliative & Supportive Care / Volume 21 / Issue 3 / June 2023
- Published online by Cambridge University Press:
- 27 June 2022, pp. 483-491
-
- Article
- Export citation
Prevalence and risk factors for suicide in patients with sepsis: nationwide cohort study in South Korea
-
- Journal:
- BJPsych Open / Volume 8 / Issue 2 / March 2022
- Published online by Cambridge University Press:
- 10 March 2022, e61
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Comparison of Objective Prognostic Score and Palliative Prognostic Score performance in inpatients with advanced cancer in Japan and Korea
-
- Journal:
- Palliative & Supportive Care / Volume 20 / Issue 5 / October 2022
- Published online by Cambridge University Press:
- 05 October 2021, pp. 662-670
-
- Article
- Export citation
Prevalence of mental illness among COVID-19 survivors in South Korea: nationwide cohort
-
- Journal:
- BJPsych Open / Volume 7 / Issue 6 / November 2021
- Published online by Cambridge University Press:
- 01 October 2021, e183
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
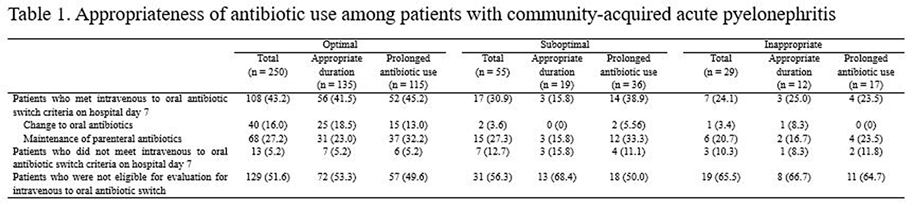
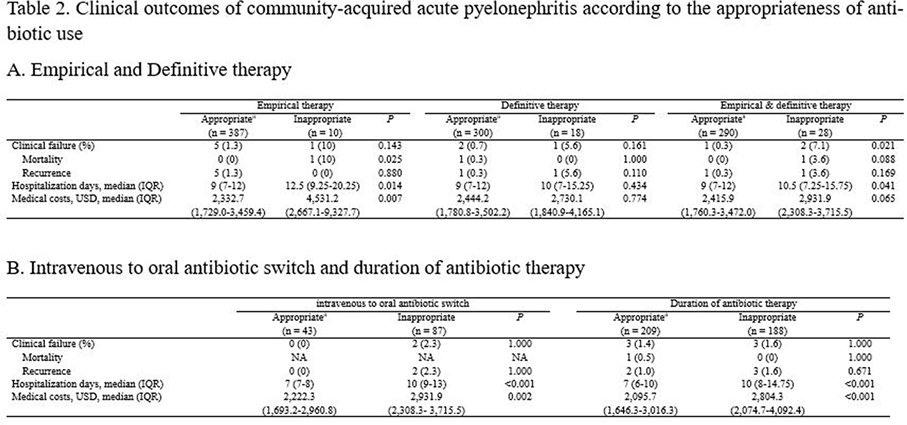
Differences in the Clinical Outcome of Community-Acquired APN According to the Appropriateness of Antibiotic Use
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s6
-
- Article
-
- You have access
- Open access
- Export citation
“The surprise questions” using variable time frames in hospitalized patients with advanced cancer
-
- Journal:
- Palliative & Supportive Care / Volume 20 / Issue 2 / April 2022
- Published online by Cambridge University Press:
- 17 June 2021, pp. 221-225
-
- Article
- Export citation
Is spirituality related to survival in advanced cancer inpatients in Korea?
-
- Journal:
- Palliative & Supportive Care / Volume 16 / Issue 6 / December 2018
- Published online by Cambridge University Press:
- 21 December 2017, pp. 669-676
-
- Article
- Export citation
Periventricular white matter hyperintensities and the risk of dementia: a CREDOS study
-
- Journal:
- International Psychogeriatrics / Volume 27 / Issue 12 / December 2015
- Published online by Cambridge University Press:
- 27 July 2015, pp. 2069-2077
-
- Article
- Export citation
Inadequate calcium intake is highly prevalent in Korean children and adolescents: the Korea National Health and Nutrition Examination Survey (KNHANES) 2007–2010
-
- Journal:
- Public Health Nutrition / Volume 17 / Issue 11 / November 2014
- Published online by Cambridge University Press:
- 28 October 2013, pp. 2489-2495
-
- Article
-
- You have access
- HTML
- Export citation
Effects of education on the progression of early- versus late-stage mild cognitive impairment
-
- Journal:
- International Psychogeriatrics / Volume 25 / Issue 4 / April 2013
- Published online by Cambridge University Press:
- 04 December 2012, pp. 597-606
-
- Article
- Export citation