112 results
The effectiveness of the COVID-19 vaccines in the prevention of post-COVID conditions in children and adolescents: a systematic literature review and meta-analysis
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 19 April 2024, e54
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Research agenda for transmission prevention within the Veterans Health Administration, 2024–2028
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 11 April 2024, pp. 1-10
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The use of UV-C radiation for terminal disinfection of pathogenic Gram-negative rods: a pilot study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 21 December 2023, e247
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Spatiotemporal distribution of community-acquired phenotypic extended-spectrum beta-lactamase Escherichia coli in United States counties, 2010–2019
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 4 / April 2024
- Published online by Cambridge University Press:
- 11 December 2023, pp. 540-542
- Print publication:
- April 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Alcohol-based decontamination of gloved hands: A randomized controlled trial
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 4 / April 2024
- Published online by Cambridge University Press:
- 23 November 2023, pp. 467-473
- Print publication:
- April 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Using a human-factors engineering approach to evaluate environmental cleaning in Veterans’ Affairs acute and long-term care facilities: A qualitative analysis
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 3 / March 2024
- Published online by Cambridge University Press:
- 24 October 2023, pp. 351-359
- Print publication:
- March 2024
-
- Article
- Export citation
Persistence of potential ST398 MSSA in outpatient settings among US veterans, 2010–2019
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 20 October 2023, e177
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The effectiveness of COVID-19 vaccine in the prevention of post-COVID conditions: a systematic literature review and meta-analysis of the latest research
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 13 October 2023, e168
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
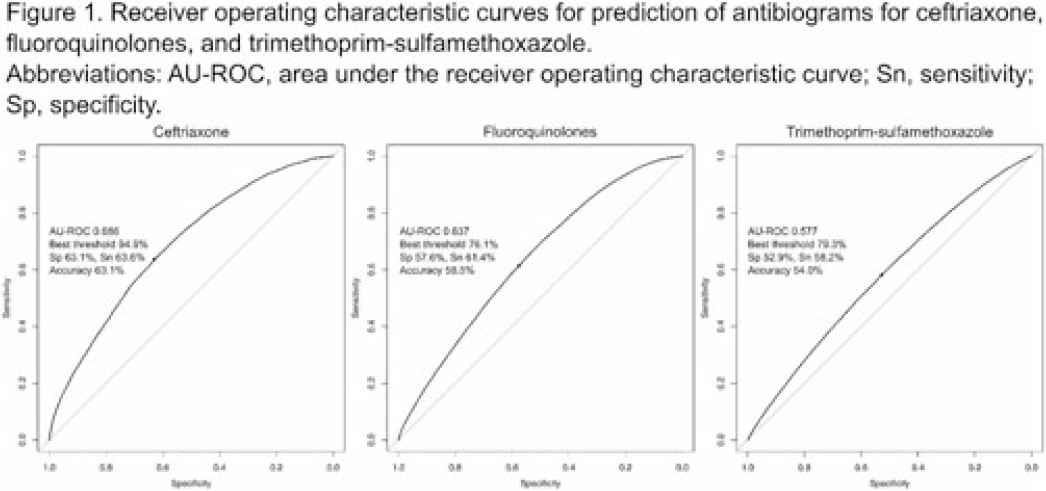
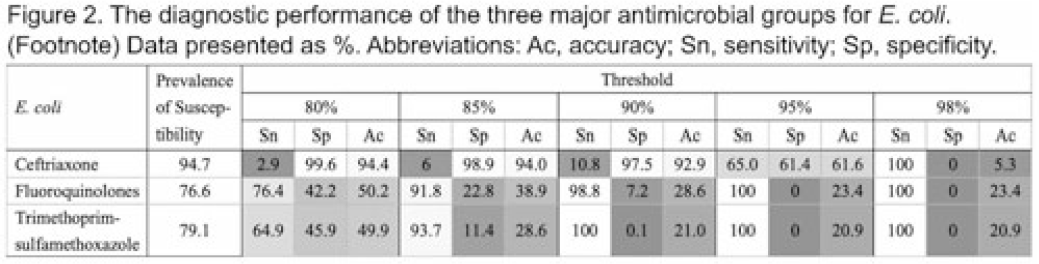
Diagnostic accuracy of antibiograms in predicting the risk of antimicrobial resistance for individual patients
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s42-s43
-
- Article
-
- You have access
- Open access
- Export citation
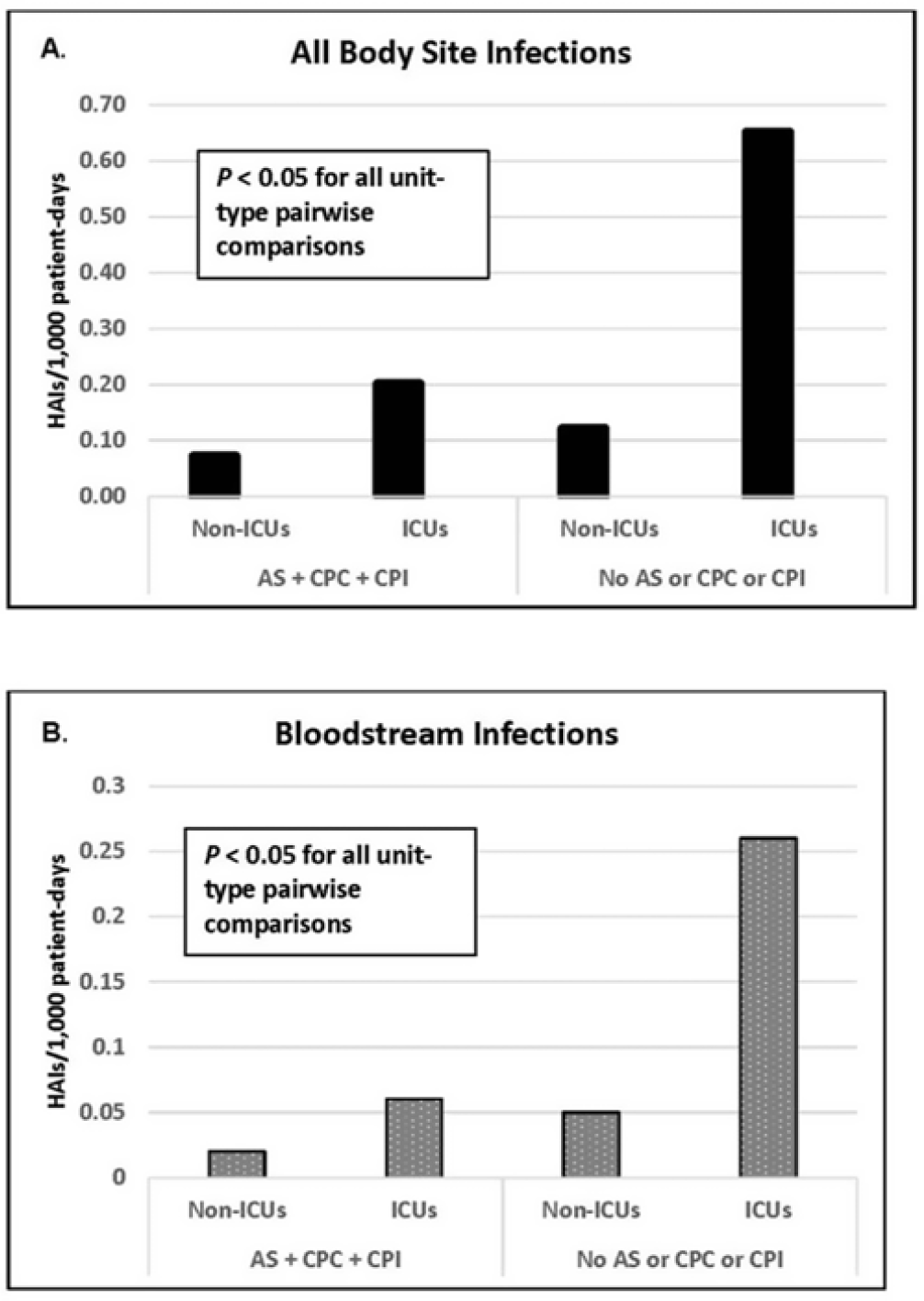
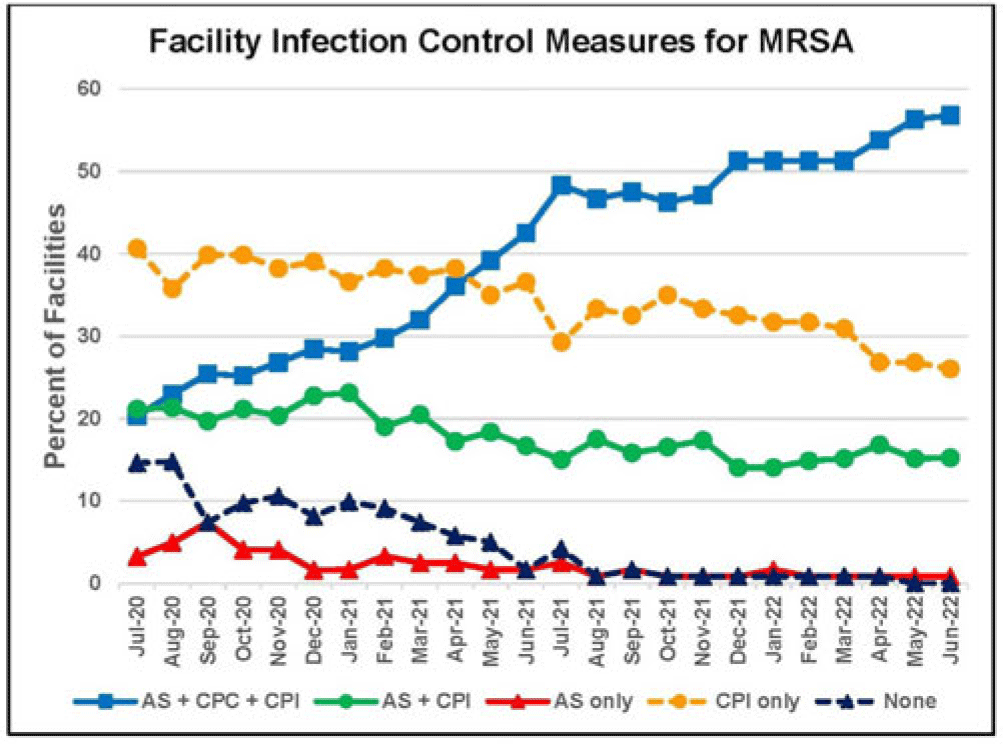
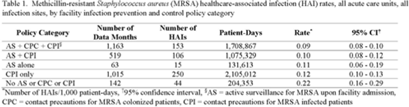
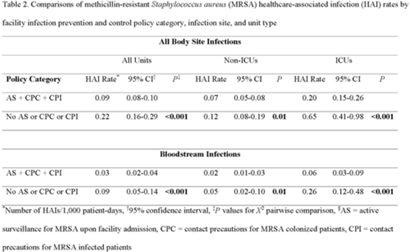
Active surveillance and contact precautions for preventing MRSA healthcare-associated infections during the COVID-19 pandemic
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s117-s118
-
- Article
-
- You have access
- Open access
- Export citation
Comparison of virus aerosol concentrations across a face shield worn on a healthcare personnel during a simulated patient cough
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 2 / February 2024
- Published online by Cambridge University Press:
- 23 August 2023, pp. 221-226
- Print publication:
- February 2024
-
- Article
- Export citation
Perceptions of an automated benchmarking dashboard for antimicrobial stewardship programs among antimicrobial stewards within the veterans’ health administration: a multicenter qualitative study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 10 July 2023, e118
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The use of telehealth-supported stewardship activities in acute-care and long-term care settings: An implementation effectiveness trial
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 14 June 2023, pp. 2028-2035
- Print publication:
- December 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Risk factors for long coronavirus disease 2019 (long COVID) among healthcare personnel, Brazil, 2020–2022
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 05 June 2023, pp. 1972-1978
- Print publication:
- December 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Impacts of Hurricane Matthew Exposure on Infections and Antimicrobial Prescribing in North Carolina Veterans
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 17 / 2023
- Published online by Cambridge University Press:
- 20 March 2023, e357
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Tracking antimicrobial stewardship activities beyond days of therapy (DOT): Comparison of days of antibiotic spectrum coverage (DASC) and DOT at a single center
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 6 / June 2023
- Published online by Cambridge University Press:
- 10 January 2023, pp. 934-937
- Print publication:
- June 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The effectiveness of coronavirus disease 2019 (COVID-19) vaccine in the prevention of post–COVID-19 conditions: A systematic literature review and meta-analysis
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 06 December 2022, e192
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Is the number of prescriptions an appropriate metric for outpatient antimicrobial consumption? A comparison between the prescription counts and days supplied
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 6 / June 2023
- Published online by Cambridge University Press:
- 23 August 2022, pp. 941-944
- Print publication:
- June 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
“Our job is to break that chain of infection”: Challenges environmental management services (EMS) staff face in accomplishing their critical role in infection prevention
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 29 July 2022, e129
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Investigation of factors influencing inpatient antibiotic prescribing decisions in the Veterans’ Health Administration
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 23 June 2022, e99
-
- Article
-
- You have access
- Open access
- HTML
- Export citation