Lithium was one of the earliest effective psychiatric treatments and continues to be widely prescribed. It has been shown to be effective in a wide range of psychiatric disorders, including bipolar disorder (Reference Davis, Janicak and HoganDavis et al, 1999; Reference Burgess, Geddes and HawtonBurgess et al, 2001), treatment-resistant depression (Reference Heit and NemeroffHeit & Nemeroff, 1998) and recurrent depression (Reference Greil, Ludwig-Mayerhofer and ErazoGreil et al, 1996; Reference Davis, Janicak and HoganDavis et al, 1999). Some research has suggested that lithium reduces suicidality and admission rates in patients with bipolar disorder, although these findings have been disputed (Reference Tondo, Jamison and RossTondo et al, 1997; Reference Burgess, Geddes and HawtonBurgess et al, 2001). Lithium also appears to be efficacious in the elderly (Reference Chen, Altshuler and MelnykChen et al, 1999; Reference Wilkinson, Holmes and WoolfordWilkinson et al, 2002). However, it has a narrow therapeutic range and lithium toxicity carries a high mortality. Elderly people and those with organic brain disease are particularly vulnerable to such toxicity (Reference Stoudemire, Hill and LewisonStoudemire et al, 1998). Lithium has important effects on renal and thyroid function, which necessitate screening for renal and thyroid impairment.
Used carefully, lithium still has an important place in the management of affective disorders, but regular monitoring is important to ensure safe use. To aid safe prescribing, the East Riding Health Authority set up a prescribing framework for lithium in March 2000 (Box 1). This emphasised the ‘shared care’ nature of prescribing, and laid down recommendations for monitoring lithium therapy in primary and secondary care. Because management of these patients is often shared between psychiatrists and general practitioners, there is a potential for a breakdown in the effective monitoring of therapy. We undertook to audit the implementation of this framework in eastern Hull (in the East Riding of Yorkshire) involving patients from both primary and secondary care.
Method
There was no simple way to locate all the patients in secondary care who were being prescribed lithium. The current state of information technology in the Humber Mental Health Teaching Trust is unsatisfactory but similar to that in many secondary care National Health Service (NHS) trusts. Major improvements are due to be implemented shortly. Primary care, however, has been well ahead of secondary care in information technology for many years. Practice computerised records are an accurate source of information. All 29 practices within the Eastern Hull Primary Care Trust were contacted by letter, explaining the purpose of the audit and requesting lists from their computerised prescribing records of all patients currently receiving prescriptions for lithium salts. Individual practices were also contacted by telephone to maximise response rates, and reminder letters were sent to non-responders.
Box 1. Summary of the prescribing framework relating to this audit
The framework outlines the respective roles of the general practitioner and consultant psychiatrist. It contains advice about the side-effects and contraindications to lithium and the action to be taken should these occur. The framework also outlines the symptoms of lithium toxicity, which patients should be asked to report. It includes the following specific recommendations:
-
• Lithium blood levels:
-
(i) levels should be measured 12 h post dose
-
(ii) levels should be measured every 3 months
-
(iii) target range 0.4-1.0 mmol/l for patients under 65, 0.4-0.6 mmol/l for those over 65
-
-
• Urea and electrolytes should be measured annually
-
• Thyroid function should be measured annually
All blood monitoring in the area is done by one central laboratory at Hull Royal Infirmary, and results are stored on computer. Each patient was individually identified on the computer by a clinical audit assistant and the records were examined for the most recent reports of lithium level, urea and electrolytes, and thyroid function tests. Records of all patients of that name were identified and the date of birth checked to ensure that the correct patient's record was used. Providing details are correctly entered on the original request form, this is a highly accurate way of locating results. Results were then compared with the following standards, arbitrarily defined for the purpose of this audit:
-
• Urea and electrolytes assessment and thyroid function tests should have been done within the past year for all patients receiving lithium therapy for any psychiatric indication.
-
• All patients receiving lithium for any psychiatric indication should have had their serum lithium level measured within the preceding 3 months, and the level should be within the defined therapeutic range (0.4-1.0 mmol/l for those under 65 years old, 0.4-0.6 mmol/l for those 65 years old and over).
-
• At least 90% of patients taking lithium should have been given a copy of the community trust's patient information leaflet on lithium (the authors felt there was likely to be a small proportion of patients who might reasonably be exempted, for example patients with significant cognitive impairment or those not under the care of the community trust).
Patients’ knowledge about lithium, its uses, side-effects and how to take it safely were examined in a patient survey conducted in association with this audit. Questionnaires were sent by post to 29 patients under the care of eastern Hull consultant psychiatrists (the full questionnaire is available from the authors upon request). Questions were asked about the following areas:
-
• whether the patient had received the community trust's patient information leaflet on lithium treatment;
-
• the patient's understanding of the purpose of taking lithium;
-
• the patient's understanding of the signs and symptoms of lithium toxicity;
-
• the patient's understanding of how to prevent lithium toxicity;
-
• the patient's knowledge of what to do in case of lithium toxicity;
-
• the perceived adequacy of information about treatment with lithium.
Results
Monitoring
Of 29 practices in the Eastern Hull Primary Care Trust, 19 were identified from trust prescribing data as having patients taking lithium on their lists. Eighteen of these practices agreed to participate, and a total of 50 patients were identified: 34 patients were under 65 years old and 16 patients were aged 65 years or over. Only just over half the patients had received adequate monitoring of lithium levels, and - alarmingly - 2 patients had no lithium level at all on record. Screening for complications of lithium therapy was a little better, with approximately two-thirds of patients having had their thyroid and renal function tested within the past year. The results of the audit are summarised in Tables 1 and 2.
Table 1. Results of monitoring audit
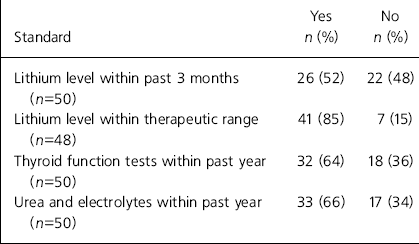
| Standard | Yes n (%) | No n (%) |
|---|---|---|
| Lithium level within past 3 months (n=50) | 26 (52) | 22 (48) |
| Lithium level within therapeutic range (n=48) | 41 (85) | 7 (15) |
| Thyroid function tests within past year (n=50) | 32 (64) | 18 (36) |
| Urea and electrolytes within past year (n=50) | 33 (66) | 17 (34) |
Table 2. Results of audit compared by age
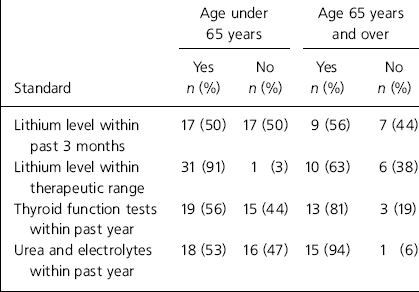
| Age under 65 years | Age 65 years and over | |||
|---|---|---|---|---|
| Standard | Yes n (%) | No n (%) | Yes n (%) | No n (%) |
| Lithium level within past 3 months | 17 (50) | 17 (50) | 9 (56) | 7 (44) |
| Lithium level within therapeutic range | 31 (91) | 1 (3) | 10 (63) | 6 (38) |
| Thyroid function tests within past year | 19 (56) | 15 (44) | 13 (81) | 3 (19) |
| Urea and electrolytes within past year | 18 (53) | 16 (47) | 15 (94) | 1 (6) |
Questionnaire results
Out of 29 questionnaires, 27 were returned, giving a 93% response rate. Just 8 patients (30%) reported having been given the community trust's patient information leaflet about lithium treatment and only 4 patients had received it before starting treatment. Although 23 patients (85%) felt that they understood the reason for being prescribed lithium, only just over a quarter (n=7) felt that they could recognise the signs and symptoms of lithium toxicity, and just over a third (n=10) felt that they knew what course of action to take if they suspected that they might be experiencing lithium toxicity. Less than half (12 patients) felt that they knew how to reduce the risk of lithium levels becoming too high. Three-quarters (20 patients) felt that they had been provided with too little information about lithium.
Discussion
This audit revealed poor levels of lithium monitoring, despite the introduction of a local prescribing framework. Potentially, patients could be at risk of serious adverse events, and practitioners at risk from litigation. The audit included elderly patients, who present a special risk, and results suggest some possible confusion among practitioners about the different therapeutic range for this age group. However, the prescribing framework does set a high standard of 3-monthly monitoring. Although this is certainly appropriate for elderly patients, 6-monthly monitoring is probably adequate for younger patients and is the recommended frequency in the new general practitioner contract.
There may be reasons for failure to monitor lithium therapy, such as the patient refusing to comply with blood testing. However, if a patient cannot comply with the regimen of monitoring required, this should raise questions about the suitability of lithium for that patient. Alternatives exist that do not require such intensive monitoring: these include other mood stabilisers, longterm antidepressant therapy and antipsychotic therapy.
Advice about safety with lithium needs to be reiterated if patients are to avoid potentially serious complications. This study suggests that patients’ knowledge about their medication was low. The questionnaire asked specifically about receipt of the trust leaflet. Most patients should also have received a drug information leaflet inside their medication packet. Despite this, levels of knowledge about lithium were still inadequate. Patients had not retained sufficient information to recognise signs of lithium toxicity or know what to do if this arose. Educating patients about their medication is an ongoing process, and doctors involved in prescribing drugs have a responsibility to ensure that patients take them safely. Knowledge is enhanced by giving written information about the treatment, but this is not a substitute for face-to-face advice tailored to the needs of the individual patient. Although information about lithium will be provided by the psychiatrist at the initiation of therapy, the general practitioner also has a part to play in educating and informing the patient about this medication. It is therefore imperative that primary care staff themselves have good, up-to-date knowledge about lithium and other psychotropic drugs, and psychiatric services should have a full and active role in achieving this.
It is not known to what extent these findings reflect practice in other British cities. However, the shared care model of lithium prescribing described here is to be found in many places. We should not be complacent that introduction of prescribing frameworks, guidelines or shared care protocols will automatically improve standards; indeed, they may lull practitioners into a false sense of security. The NHS Centre for Reviews and Dissemination (1999) published a review of a variety of strategies aimed at changing professional behaviour, which concluded that ‘dissemination activities by themselves are unlikely to lead to changes in behaviour’, although raising awareness can have an important role in changing behaviour. Multifaceted interventions aimed at addressing specific barriers to change tend to be more effective but also more expensive. Regular audit needs to be coupled with measures such as drug registers, automatic recall systems and lithium monitoring cards to ensure that practice is of the highest standard.
Declaration of interest
None.
Acknowledgements
We thank Mrs Sue Norman (Clinical Audit Assistant) and other members of the Clinical Audit Department at Hull and East Riding Community NHS Trust for assisting in data collection for this audit. We also thank Mr Mike Rymer, Pharmaceutical Adviser, Eastern Hull Primary Care Trust for facilitating the project.





eLetters
No eLetters have been published for this article.