Psychogenic non-epileptic seizures (PNES) can be defined as paroxysmal events that resemble or can be mistaken for epilepsy, without being associated with abnormal electroencephalogram (EEG) activity or any other primary physiological disturbance. Most are interpreted as a behavioural or experiential response to overwhelming distress (Reference ReuberReuber 2008). Psychogenic non-epileptic seizures sit uneasily within the current psychiatric classification systems, classified as a dissociative (conversion) disorder (‘dissociative convulsions’) in ICD-10 (World Health Organization 1992) and as a somatic symptom disorder in DSM-5 (American Psychiatric Association 2013). However, many patients also fulfil the criteria for mood and anxiety disorders, post-traumatic stress disorder, episodic dyscontrol and, in a minority, factitious disorder (Reference Bodde, Brooks and BakerBodde 2009). Some PNES-like events are probably malingered but the overwhelming majority of patients are thought to have seizures which are not wilfully produced.
At least 15 different terms have been used to describe this clinical phenomenon, including: pseudoseizures, dissociative seizures, functional seizures, hysterical seizures and non-epileptic attack disorder. Some of these terms (especially hysterical seizures and pseudoseizures) are unacceptable to patients (or question the veracity of their experience) and have been abandoned or should be discouraged (Reference Stone, Campbell and SharmaStone 2003). For the purpose of this article, we will use the term PNES, which has been used most commonly in recent research.
Here we offer an overview of the main aspects of PNES. Although informed as comprehensively as possible by published evidence, it must be made clear that the article reflects our own views and clinical experience.
Epidemiology
Epidemiological studies of PNES are difficult since most patients are initially misdiagnosed as having epilepsy. The eventual diagnosis often depends on the clinician questioning the diagnosis of epilepsy and considering that of PNES. For example, Szaflarski et al noted an increasing incidence of PNES during the course of their study, possibly reflecting a greater level of awareness of PNES on the part of referring physicians (Reference Szaflarski, Ficker and CahillSzaflarski 2000).
Several studies document that the misdiagnosis of PNES as epilepsy remains a significant problem (Reference Chadwick and SmithChadwick 2002). Community-based epidemiological studies have reported rates of misdiagnosis of epilepsy ranging from 20 to 26%, and PNES has been found to be the second most common condition to be mistaken for epilepsy after syncope (Reference Smith, Defalla and ChadwickSmith 1999). It takes a mean of 5–7 years from the manifestation of seizures for a diagnosis of PNES to be made, and over three-quarters of patients have been treated inappropriately with anti-epileptic drugs by the time the diagnosis is formulated (Reference Reuber, Fernandez and BauerReuber 2002a; Reference Hall-Patch, Brown and HouseHall-Patch 2010).
Three studies have estimated the annual incidence of PNES at between 1.4 and 6.7 episodes per 100 000 people (Reference Sigurdardottir and OlafssonSigurdardottir 1998; Reference Szaflarski, Ficker and CahillSzaflarski 2000; Reference Duncan, Razvi and MulhernDuncan 2011). These studies are likely to have underestimated the true incidence of PNES because they only counted patients diagnosed on the basis of video-EEG evidence.
Psychogenic non-epileptic seizures are particularly prevalent in certain settings. Up to 30% of patients with intractable epilepsy referred to an epilepsy specialist centre for further consideration of epilepsy surgery will eventually be diagnosed as having PNES, compared with 10–20% of new presentations to an epilepsy clinic (Reference Angus-LeppanAngus-Leppan 2008). Psychogenic non-epileptic seizures are not uncommonly seen in patients subjected to acute stressors including head injuries (Reference Hudak, Trivedi and HarperHudak 2004) or general anaesthetics (Reference Reuber, Enright and GouldingReuber 2000). They are also seen quite commonly in people with intellectual disabilities (Reference Chapman, Iddon and AtkinsonChapman 2011).
There is an emerging consensus that the coexistence of epilepsy and PNES is the exception rather than the rule. Research of patients with PNES diagnosed with video EEG has consistently shown that only about 10% of patients have concurrent epileptic seizures (Reference Jones, O'Brien and AdamsJones 2010; Reference McKenzie, Oto and RussellMcKenzie 2010). It is important to stress that even in cases where comorbidity is confirmed, the clinical picture is generally of frequent PNES in the context of underlying well-controlled epilepsy (Reference Duncan and OtoDuncan 2008). The frequency of concurrent epilepsy is higher in some patient subgroups, for instance in patients with intellectual disabilities and PNES.
Iatrogenic and other associated harm
Pseudostatus
The most serious iatrogenic harm occurs in the context of ‘pseudostatus’. Pseudostatus refers to prolonged non-epileptic attacks, which can attract an erroneous diagnosis of status epilepticus. Up to 25% of patients with PNES will present in pseudostatus at some point (Reference Reuber, House and PukropReuber 2003a), and 25% of patients referred to a neurological unit with refractory seizure status turn out to have PNES (Reference Walker, Howard and SmithWalker 1996). Inappropriate use of intravenous anticonvulsants, general anaesthesia and intubation can cause injury and death (Reference Reuber, Baker and GillReuber 2004a).
Anti-epileptic drugs
The oral administration of anti-epileptic drugs may also have important unwanted effects. Acute, chronic and/or cumulative iatrogenic harm may result from inappropriate prescription of these drugs (Reference Bodde, Janssen and TheunsBodde 2007; Reference Duncan and OtoDuncan 2008). Many of these agents are teratogenic (some do not only increase the risk of congenital malformation but also have detrimental effects on the longer-term cognitive development of the child); a feature of particular importance given that the majority of patients with PNES are women of childbearing age (Reference Meador, Reynolds and CreanMeador 2008).
Polypharmacy
Given that their seizures tend to prove refractory to anti-epileptic drugs, many patients with PNES are treated with multiple drugs in higher dosages, and they report more side-effects or allergies compared with patients with epilepsy. Up to 22% of patients have been found to reach drug levels beyond their usual therapeutic range (Reference Hantke, Doherty and HaltinerHantke 2007).
Economic burden
An undoubtedly important associated harm of PNES is the substantial economic burden they place on patients, families and health services (Reference McKenzie, Oto and RussellMcKenzie 2010).
General characteristics of patients
Although patients with PNES form a heterogeneous group (Reference Baslet, Roiko and PrenskyBaslet 2010) and do not fit neatly into the categorical scheme of the currently used psychiatric nosologies, some common characteristics have been consistently reported.
Women are overrepresented among patients with PNES, with most studies reporting a female to male ratio of about 4:1 (Reference Oto, Conway and McGonigalOto 2005). Psychogenic non-epileptic seizures most commonly manifest between 20 and 40 years of age (Reference Reuber and ElgerReuber 2003b) (however, it is important to bear in mind that PNES can start at any age, including in children and older adults; Reference Duncan, Oto and MartinDuncan 2006).
High levels of comorbid psychopathology and other medically unexplained symptoms have also been described in this group (Reference Reuber, House and PukropReuber 2003a).
Diagnosis
In many cases, an expert can be reasonably certain of the diagnosis of PNES on the basis of the patient’s history and witness accounts of the seizure (Reference Plug and ReuberPlug 2009a). Unfortunately, the process of diagnosing PNES and communicating this diagnosis is often complicated by the fact that most patients come with a previous diagnosis of epilepsy, which may have gone unquestioned for many years (Reference Reuber, Fernandez and BauerReuber 2002a; Reference Bodde, Janssen and TheunsBodde 2007; Reference Duncan and OtoDuncan 2008). In such cases, therefore, the diagnostic process not only involves making the diagnosis of PNES, but also removing the firmly attached label of epilepsy.
Taking account of this as well as the potential consequences of a misdiagnosis, video-EEG confirmation of the clinical diagnosis is often helpful. A home video recording without EEG can be useful as well (Reference Samuel and DuncanSamuel 1994; Reference Chen, Graber and AndersonChen 2008). The availability of a positive diagnostic test can be of great value when the diagnosis of PNES is communicated to the patient.
Psychogenic non-epileptic seizures must also be distinguished from other paroxysmal events, mediated by primarily physiological or emotional causes. There are a number of conditions that can present with sudden changes of behaviour or level of consciousness. Syncope is the most common but the differential diagnosis is wide. This article will not expand further on the differential diagnosis of blackouts; however, this topic has been reviewed extensively elsewhere (Reference RobertsRoberts 1998; Reference BenbadisBenbadis 2009; Reference Malmgren, Appleton and ShorvonMalmgren 2012).
Clinical diagnosis
The semiology and clinical features of the seizures can contain important pointers to the clinical diagnosis. Several studies have investigated this issue and reported a range of features that should alert clinicians to the possibility of PNES. The most common features that distinguish PNES from epileptic attacks are listed in Box 1. It is important to recognise, however, that no single semiological feature is pathognomonic for PNES, and that no symptom should be considered in isolation when making the clinical diagnosis of PNES.
BOX 1 Clinical features of attacks suggestive of psychogenic non-epileptic seizures
-
• Gradual onset
-
• Abrupt ending
-
• Seizures with thrashing for more than 3 minutes
-
• Asynchronous shaking
-
• Undulating motor activity
-
• Sustained eye closing
-
• Side-to-side head movement
Some types of seizures are easily recognised as PNES: swooning attacks in which patients collapse in a limp, still and unresponsive state are unlikely to be caused by epilepsy or other physiological abnormalities, especially if prolonged. Seizures involving prolonged thrashing (more than 3 minutes), purposeful moments, rhythmic pelvic movements and preserved responsiveness are likely to be PNES. Stuttering or weeping during or immediately after the attack is seen more commonly in PNES than in epilepsy (Reference Bodde, Janssen and TheunsBodde 2007; Reference Hoerth, Wellik and DemaerschalkHoerth 2008). Shaking in PNES is typically caused by tremor (alternating activity of agonists and antagonists) and not by intermittent clonic muscle activity (rapid contractions of agonists followed by relaxation). The frequency of the shaking in PNES tends not to change during the course of a seizure (only the amplitude varies). The frequency of muscle contractions diminishes gradually in tonic–clonic epileptic seizures (Reference Vinton, Carino and VogrinVinton 2004).
It is important to note that certain clinical features considered typical of epilepsy often occur in PNES as well (Reference Reuber, Broadhurst and GrunewaldReuber 2011). These include autonomic manifestations such as tachycardia, flushing and sweating (Reference Goldstein and MellersGoldstein 2006), incontinence and injury, including tongue biting (Reference Reuber and ElgerReuber 2003b; Reference Stone and DuncanStone 2006), and provocation of seizures by specific triggers such as flashing lights (Reference Meierkord, Will and FishMeierkord 1991). Nocturnal attacks have often been thought to be a feature of epilepsy but are as frequently reported by patients with PNES (Reference Duncan, Oto and RussellDuncan 2004).
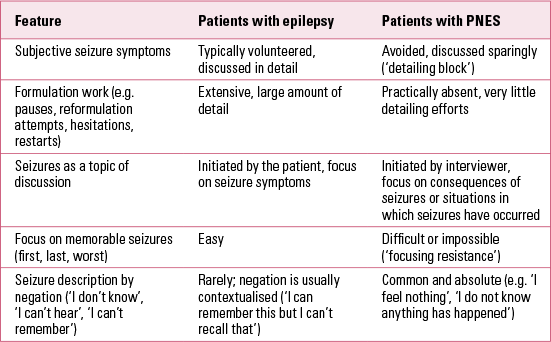
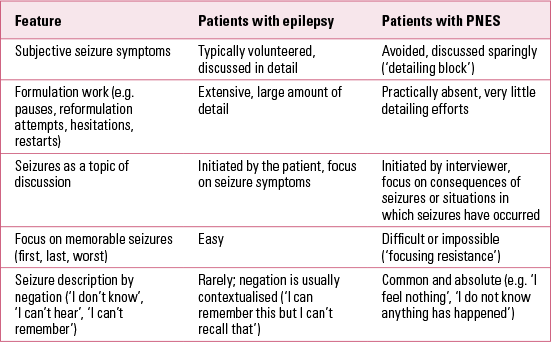
As well as the characteristics of the seizures, a number of recent studies have demonstrated that patients’ interactional behaviour (the way they talk to their doctor) can help with the differential diagnosis of epilepsy and PNES (Table 1). Most significantly, patients with epilepsy tend to focus on the symptoms of their seizures, whereas patients with PNES focus on the consequences or circumstances of their attacks. Patients with PNES provide little detail about the subjective seizure symptomatology and resist the focus on particularly memorable seizures (first, last, worst) (Reference Reuber, Monzoni and SharrackReuber 2009a). Patients with PNES also prefer to use different metaphoric conceptualisations for their seizures than patients with epilepsy. Whereas epileptic seizures are most commonly conceptualised as acting independently and on the patient (e.g. ‘The seizure came up inside me’), PNES are described as a space or place the patient travels through (e.g. ‘I go into a seizure’) (Reference Plug, Sharrack and ReuberPlug 2009b). Patients with epilepsy have a tendency to normalise, whereas patients with PNES are likely to catastrophise their seizure experiences (Reference Monzoni and ReuberMonzoni 2009; Reference Robson, Drew and WalkerRobson 2012).
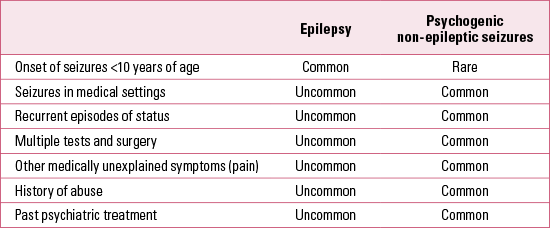
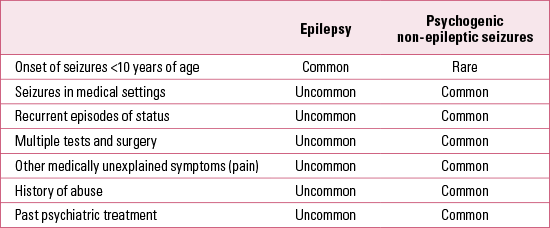
As detailed in Table 2, various factors in the history and background of patients can often indicate or support a diagnosis of PNES (Reference Reuber and ElgerReuber 2003b).
TABLE 1 Interactional and linguistic features which can help in the differential diagnosis of epilepsy and psychogenic non-epileptic seizures (PNES)
It is important to point out again that some of the features listed in Table 2 may also be noted in the background of patients with epilepsy; for example, a traumatic (as distinct from specifically sexually traumatic) past does not distinguish clearly between patients with or without epilepsy (Reference Fleisher, Staley and KrawetzFleisher 2002).
Diagnostic tests
Video-EEG recording of typical seizures remains the gold standard. Combined with the patient’s history, this diagnostic technique has a high specificity and sensitivity (Reference Syed, LaFrance and KahrimanSyed 2011). It consists of simultaneous video and EEG recording of typical attacks. The interpretation of video-EEG recordings requires considerable expertise. The ictal EEG is often obscured by muscle and movement artefacts, and the reporting reviewer must take account of the semiology of attacks, pre-ictal EEG findings (such as documented sleep), heart rate changes (which are typically more marked and rapid in epileptic seizures) and postictal EEG findings.
Unfortunately, video-EEG recording remains an expensive and scarce resource, but less time-consuming and resource-intensive diagnostic techniques have been proposed. Short video EEG is an out-patient test which uses activation or suggestion techniques (including photic stimulation and hyperventilation) aiming to induce a typical seizure. This test represents a cost-effective and accurate diagnostic technique for PNES, with a diagnostic yield of 50–60% (Reference McGonigal, Russell and MallikMcGonigal 2004).
Whether ‘spontaneous’ seizures were recorded during a period of video-EEG monitoring or whether a ‘provoked’ seizure was captured during an out-patient procedure, it is essential that the diagnostician ensures that the seizure seen during the recording was typical of the patient’s habitual attacks (this may involve asking the patient and showing the recording to patients and relatives/friends or carers).
TABLE 2 Differential characteristics
Other tests – such as postictal prolactin blood levels, single-photon emission computed tomography (SPECT) and personality profiles assessed with the Minnesota Multiphasic Personality Inventory (Reference Butcher, Dahlstrom and GrahamButcher 1989) – can only make a limited contribution to the diagnosis, as none of them have sufficiently high sensitivity or specificity to be used alone. Interictal or routine EEG is also of little help and can be misleading, since non-specific abnormalities are common in the general population and their misinterpretation has often led to the erroneous diagnosis of epilepsy in the first place (Reference Chadwick and SmithChadwick 2002; Reference Reuber, Fernandez and BauerReuber 2002b; Reference Benbadis and TatumBenbadis 2003; Reference Kotsopoulos, De Krom and KesselsKotsopoulos 2003).
Aetiology
Our understanding of the underlying causes of PNES remains limited, although recent evidence is beginning to shed some light on the possible aetiological factors relevant to the development or maintenance of PNES disorders.
Investigations carried out over the past 3 years have provided some fascinating first insights into the neurobiological underpinnings of PNES. Bakvis et al have conducted a series of experimental studies focusing on cognitive processes and their likely causes. They demonstrated that patients with PNES (especially those with a history of sexual trauma) had higher basal cortisol levels and lower heart rate variability than healthy controls at rest (Reference Bakvis, Spinhoven and RoelofsBakvis 2009a, Reference Bakvis, Spinhoven and Giltay2010a). The finding of reduced heart rate variability at rest (related to a lower parasympathetic and increased sympathetic tone) has also been replicated by others (Reference Ponnusamy, Marques and ReuberPonnusamy 2011; Reference Roberts, Burleson and WeberRoberts 2012).
Bakvis et al also carried out an experiment involving a masked emotional Stroop task, which revealed (preconscious) hypervigilance to angry faces in patients with PNES (compared with healthy controls) at baseline and after recovery but not during a stress condition (Reference Bakvis, Roelofs and KuykBakvis 2009b). There was a positive correlation between baseline cortisol levels and attentional bias to threat stimuli in these patients (Reference Bakvis, Roelofs and KuykBakvis 2009b).
In another study, Bakvis et al found that, compared with healthy controls, patients with PNES showed a greater reduction in performance on a working memory test when exposed to facial distractors in the baseline condition. Poorer performance in the working memory test generalised in a physiologically induced stress condition: when stressed, patients with PNES performed below the level of controls with or without facial distractors (Reference Bakvis, Roelofs and KuykBakvis 2010b).
The same group of authors carried out a study exploring avoidance behaviour by patients with PNES. In this study, patients and healthy controls made affect-congruent or affect-incongruent arm movements (arm flexion or extension) in response to pictures of angry or happy faces. The study provided experimental evidence for the previously described findings of self-report studies suggesting that patients with PNES show increased avoidance of social threat cues (Reference Goldstein, Drew and MellersGoldstein 2000; Reference Bakvis, Spinhoven and ZitmanBakvis 2011).
Further insights into the neurobiological underpinnings of PNES can be gleaned from a study which used the analysis of resting functional magnetic resonance imaging patterns in patients with PNES to suggest that this patient group may be characterised by brain networks with abnormally strong connections between areas involved in emotion and self-observation processes (insula), executive control (inferior frontal gyrus and parietal cortex) and movement (pre-central sulcus). Increased connectivity values were positively correlated with higher dissociation scores (Reference Van der Kruijs, Bodde and Vaessenvan der Kruijs 2012).
Although all of these studies were small and may not have captured the breadth of different PNES presentations, and although it is too early to say to what extent the changes described are specific to PNES or reflect the presence of dissociation tendencies or the consequences of traumatisation, most highlight the fact that patients with PNES do not only experience seizures but also differ from healthy controls in terms of interictal functioning and experiences. These studies do not replace the more established psychodynamic interpretation of PNES (based on aetiologically relevant predisposing, shaping, precipitating and perpetuating factors), but enhance this interpretation and provide some important building blocks for a more richly faceted biopsychosocial model (Reference ReuberReuber 2009b).
Predisposing factors
Past traumatic experience
Past traumatic experience is one of the most frequently reported associated factors and reports of childhood abuse are high among patients with PNES. Sexual abuse was considered at one point as one of the main causes of PNES. However, sexual abuse is only reported by a minority of patients with PNES (about 30% of women and 5% of men), and over the past 10 years there has been a shift towards a more non-specific but possibly more nuanced view of the role of trauma in PNES, with sexual abuse conceptualised as a marker of more severe emotional and physical neglect, rather than a specific cause in itself (Reference Reuber, Howlett and KhanReuber 2007; Reference Bakvis, Roelofs and KuykBakvis 2009b).
Personality traits and psychopathology
Pathological personality traits are frequently found in patients with PNES, with reports of proportions of patients fulfilling diagnostic criteria for personality disorder as high as 75–90% (Reference Binzer, Stone and SharpeBinzer 2004; Reference Reuber, Pukrop and BauerReuber 2004b). There is also evidence that certain premorbid personality traits and coping styles are associated with PNES, for example a relationship has been found between PNES and alexithymia or abnormally avoidant coping (Reference Goldstein, Drew and MellersGoldstein 2000; Reference Bewley, Murphy and MallowsBewley 2005). Associated psychopathology can also be seen as a possible predisposing factor, although it is often difficult to determine retrospectively whether psychopathology is part of the primary cause, consequence and/or perpetuating factor of PNES (Reference Reuber, Pukrop and BauerReuber 2004b).
Physical illness
Finally, physical illness and disability can also contribute to someone’s vulnerability to develop PNES, for example reports of minor head injury are common (Reference Westbrook, Devinsky and GeocadinWestbrook 1998; Reference Pakalnis and PaolicchiPakalnis 2000). Physical illnesses or health anxieties seem to be particularly important factors in older patients who develop PNES (Reference Duncan, Oto and MartinDuncan 2006).
Shaping factors
Many of the factors which appear to predispose patients to develop PNES also apply to other medically unexplained symptoms; however, why an individual patient happens to develop PNES is not clear. There is some evidence suggesting that a history of trauma is more common in patients with PNES than in patients with other medically unexplained neurological symptoms (Reference Stone, Sharpe and BinzerStone 2004).
The modelling theory is based on the fact that patient presentations mimic symptoms of others or themselves, and has been proposed as a possible explanation for a subgroup of patients. Bautista et al found that up to 60% of patients with PNES reported having witnessed a seizure in the past, and there is also evidence that, when compared with patients diagnosed with epilepsy, people with PNES report higher rates of a family history of epilepsy (Reference Bautista, Gonzales-Salazar and OchoaBautista 2008).
In our experience, a different paroxysmal event, for example syncope, hyperventilatory symptoms or a panic attack, may be the initial event that triggers and shapes the ongoing seizures in a substantial group of patients. When going through the history it is not unusual to find that the patient’s first event shares more typical elements with descriptions of a faint or panic attack than subsequent seizures. The level of distress and alarm will often have been compounded subsequently by the involvement of emergency services, the administration of powerful sedatives, and transfer to high-intensity medical environments (Box 2). The subsequent labelling of the attack as ‘epileptic’ and the apparently lifesaving intervention by medical authority figures, in concert with pre-existing vulnerabilities and experience, can potently influence illness beliefs and contribute to the rapid development of a PNES disorder.
BOX 2 Vignette
Mr M is a 29-year-old man who attends the psychogenic non-epileptic seizures (PNES) clinic having developed frequent ‘major’ seizures 4 months earlier.
Mr M describes the circumstances surrounding his first attack. He had been working very long hours to relieve financial pressures. Around the same time he was waiting for the results of a biopsy of a lump on his neck. He was anxious, exhausted and unable to sleep.
The day of his first seizure he woke up at 05.00 h, got out of bed quickly and remembers feeling light-headed and ‘strange’ (his wife noticed that he was very pale and started to over-breath). He then seemed to collapse and his wife, immediately sitting him up, noticed some jerking of his arms. His wife ‘panicked’ and telephoned for an ambulance.
When the ambulance arrived, Mr M had come round; however, he was still drowsy and very distressed. The paramedics mentioned epilepsy and attempted to insert a canula (Mr M has a needle phobia). By the time he got to the accident and emergency department he was ‘shaking’, breathing fast and complaining of a severe headache.
Four hours later and after many tests, including three failed attempts to perform a lumbar puncture, Mr M had a few more episodes of ‘body shaking’ which were thought to be epilepsy and he was treated with intravenous diazepam and started on anti-epileptic drugs.
Precipitating factors
Stressful or traumatic life events prior to the start of PNES can be identified in the majority of patients (Reference Binzer, Stone and SharpeBinzer 2004; Reference Reuber, Howlett and KhanReuber 2007). A wide variety of psychological and physical stressors have been reported as possible precipitating factors. It is likely, however, that these factors have to been seen in the context of the individual patient’s vulnerability and experiences (Reference Bowman, Ettinger and KannerBowman 2001).
Perpetuating factors
Financial/medical reward
Having an illness can excuse patients from certain responsibilities as well as entitling them to compensation in the form of financial and practical help. Secondary gain, the notion that behaviour is motivated by explicit material reward as well as implicit or unacknowledged psychic conflict is possibly needlessly pejorative and a substantial oversimplification of the plight of patients who get stuck in the sick role. However, receipt of state benefits could be a powerful disincentive to recovery and has certainly been reported as a factor associated with a poor prognosis (Reference Mayor, Howlett and GrünewaldMayor 2010; Reference McKenzie, Oto and RussellMcKenzie 2010).
Relatives’ beliefs and their reinforcement of the illness behaviour can also perpetuate the patient’s symptoms.
Clinical iatrogenesis and medicalisation
A potentially preventable perpetuating factor is clinical iatrogenesis, since healthcare professionals have an important role in the chronification of PNES. Medicalisation can have a powerful effect on any patient unfortunate enough to attract a diagnosis of epilepsy, erroneous or not, but is of particular relevance in a group of patients who already have a tendency to interpret their attacks as unpredictable and out of their control and who were keen to attribute their symptoms to physical causes in the first place (Reference Goldstein and MellersGoldstein 2006).
The patient’s feelings
Patients often report feelings of anger and uncertainty following a diagnosis of PNES (Reference Carton, Thompson and DuncanCarton 2003; Reference Thompson, Isaac and RowseThompson 2009). These problems are considerably compounded by ambiguous management (such as leaving patients on anti-epileptic drugs following the diagnosis), exposure to unhelpful attitudes of healthcare professionals (Reference Worsley, Whitehead and KandlerWorsley 2011), and repetition of redundant or unnecessary medical tests with low diagnostic yield in a fruitless attempt to bring about consensus.
Management and prognosis
Psychogenic non-epileptic seizures do not represent a disease entity but are a manifestation of a variety of underlying psychological and psychiatric problems likely to require a range of different treatments (Reference Cragar, Berry and SchmittCragar 2005; Reference Reuber, Howlett and KempReuber 2005; Reference Baslet, Roiko and PrenskyBaslet 2010). It is not surprising then that our knowledge of the most effective management strategies for PNES remains limited (Reference Brooks, Goodfellow and BoddeBrooks 2007).
Communicating the diagnosis
While acknowledging this therapeutic uncertainty, the initial management of PNES in terms of assessment and communication of the diagnosis is a generic intervention independent of associated psychopathology (Reference Shen, Bowman and MarkandShen 1990; Reference Hall-Patch, Brown and HouseHall-Patch 2010).
Communicating the diagnosis in a clear and supportive manner is the only intervention required to stop PNES in at least 15–30% of cases (Reference Mayor, Brown and CockMayor 2012). Even when seizures persist, there is evidence that a confident diagnosis of PNES results in a significant reduction of healthcare utilisation by patients (Reference Hall-Patch, Brown and HouseHall-Patch 2010; Reference Duncan, Razvi and MulhernDuncan 2011). Giving patients a booklet about PNES or referring them to a website (e.g. www.nonepilepticattacks.info) may help them understand the diagnosis. A number of studies have shown how difficult it can be for patients to accept the diagnosis of PNES and for doctors to explain it (Reference Monzoni, Duncan and GrunewaldMonzoni 2011a, Reference Monzoni, Duncan and Grunewaldb). It may be appropriate to take more time over the explanation of the diagnosis than is typically available in a single appointment and to show seizure recordings to patients and family members, friends or carers. More extensive individual or group psychoeducation programmes (often implemented by nurses or junior psychologists) have been proposed (Reference Myers and ZaroffMyers 2004; Reference Thompson, Osorio and HunterThompson 2005; Reference Baxter, Mayor and BairdBaxter 2012). Although the successful explanation of the diagnosis may reduce seizure frequency and healthcare utilisation, there is no evidence that it improves functioning, psychopathology or quality of life more widely, and more extensive psychological treatment is likely to be indicated for most patients (Reference Mayor, Brown and CockMayor 2012).
As most patients with PNES are treated with anti-epileptic drugs, withdrawing these is the next logical step (Reference Oto, Espie and PelosiOto 2007). Up to 40% of patients, however, are left on anti-epileptics at this point (Reference Reuber, Pukrop and BauerReuber 2003c; Reference Hall-Patch, Brown and HouseHall-Patch 2010). This not only places them at an increased risk of iatrogenic harm but also contributes to feelings of confusion following the diagnosis. The results of a randomised controlled trial suggests that withdrawing anti-epileptics following diagnosis of PNES clarifies the diagnosis for the patient and reduces healthcare utilisation (Reference Oto, Espie and DuncanOto 2010).
Management following the delivery of diagnosis
Pharmacological treatment
The use of antidepressants has been recommended by some authors; however, a small randomised controlled trial evaluating the effect of sertraline proved inconclusive (Reference LaFrance, Keitner and PapandonatosLaFrance 2010). Evidence for the use of other psychotropic medication is anecdotal and in general the use of these drugs is indicated mostly on the basis of comorbid psychopathology (Reference LaFrance and DevinskyLaFrance 2004; Reference ReuberReuber 2008). The use of anti-epileptic drugs for other indications than seizures (e.g. as a mood stabiliser, anxiolytic or migraine preventative) is best avoided in this patient group (at least until the patient has fully accepted the diagnosis and is happy to communicate the diagnosis to other health professionals) because it increases the risk of mismanagement and inaccurate re-diagnosis with epilepsy (Reference Oto, Russell and McGonigalOto 2003).
Non-pharmacological treatment
If a diagnosis of PNES is established, most patients are referred on for further psychological treatment (Reference LaFrance, Rusch and MachanLaFrance 2008; Reference Mayor, Smith and ReuberMayor 2011), although there is little evidence in favour of any particular psychotherapeutic management strategy.
Two pilot randomised controlled studies of cognitive–behavioural therapy (CBT) have been reported. In a study by Reference Goldstein, Chalder and ChigwedereGoldstein et al (2010), 66 patients were randomised to 12 sessions of weekly CBT or standard medical care. The study demonstrated a significant reduction in seizure frequency at the end of the treatment period. However, no changes were detected in most of the psychosocial outcomes and the longer-term effectiveness of this approach remains uncertain.
LaFrance et al tested the effects of their CBT protocol specifically designed for patients with PNES and reported significant improvement in a range of clinical and psychological factors at the end of treatment, but have not reported any follow-up findings (Reference LaFrance, Miller and RyanLaFrance 2009).
A psychodynamically oriented treatment approach for PNES has also been described (Reference Howlett and ReuberHowlett 2009). It may be effective in the longer term, but a randomised trial of this intervention has not been carried out so far (Reference Mayor, Howlett and GrünewaldMayor 2010).
A Cochrane review on the treatment of PNES identified another three small randomised controlled trials, two comparing the effects of hypnotherapy and the third one comparing paradoxical intention treatment to regular diazepam. No overall conclusion could be reached (Reference Brooks, Goodfellow and BoddeBrooks 2007).
Although intensive interventions appear to result in seizure freedom in a high proportion of patients in the short term, gains may not be maintained and patients may relapse over subsequent follow-up (Reference O'Sullivan, Sweeney and McNamaraO’Sullivan 2006). To date, it remains uncertain whether psychotherapy is associated with better long-term outcomes, as regardless of the intervention most studies report similar results, with a third to a half of patients achieving seizure freedom 2 or more years after the diagnosis (Reference Reuber, Pukrop and BauerReuber 2003c; Reference De Paola, Silvado and MaderDePaola 2006).
Outcome measures
The usefulness of much of the literature is somewhat reduced by the limitations of seizure freedom or, more importantly, reduction as an outcome. There is evidence that reduction or cessation of seizures, although useful as an objective clinical outcome measure, may not correlate with psychosocial recovery or quality of life, and the importance of including comprehensive and relevant psychosocial measures of outcome has been stressed by a number of authors (Reference LaFrance, Rusch and MachanLaFrance 2008; Reference ReuberReuber 2008; Reference Lawton, Reuber, Schachter and LaFranceLawton 2010).
Several studies have reported prognostic factors for the outcome in PNES. Methodological problems are generally apparent (Reference Ettinger, Dhoon and WeisbrotEttinger 1999). All that can be said with confidence is that measures reflecting good premorbid social adjustment and functioning, as well as lower levels of psychopathology and lack of receipt of health-related benefits correlate with a better outcome.
Conclusions
Psychogenic non-epileptic seizures are not uncommon but are underrecognised and represent a significant problem for clinicians. The clinical presentation of PNES is diverse and there is no single pathognomonic sign. However, certain features of the seizures should alert the clinician to this diagnostic possibility, for example convulsive events continuing for more than 3 minutes or collapses without movement in which the patient lies still, as if asleep, for more than 2 minutes. Although experienced clinicians are able to make an accurate diagnosis on clinical grounds in most cases, it is advisable to confirm it by recording a typical seizure if at all possible.
As in other medically unexplained symptoms, iatrogenic harm is a major issue in patients with PNES. At present the majority of patients is initially treated (inappropriately) with anti-epileptic drugs. The treatment of prolonged PNES as status epilepticus is particularly dangerous.
Our understanding of potential aetiological factors relevant to the development and maintenance of PNES is gradually improving, particularly through recent research exploring the possible neurobiological underpinning of the disorder. Nevertheless, there is still no high-quality evidence in favour of particular management strategies. There is increasing evidence, however, that an initial clear and unambiguous communication of the diagnosis of PNES (combined with the withdrawal of inappropriate anti-epileptic drug treatment) is an important therapeutic step which can reduce healthcare utilisation and may be the only intervention required for some patients.
Although PNES are not uncommon in certain medical settings, we realise that they represent only a small part of a psychiatrist’s clinical workload. However, many of the issues discussed in this article, particularly the risk of iatrogenic harm associated with the medicalisation of medically unexplained physical symptoms, should be relevant to most practising psychiatrists.
MCQs
Select the single best option for each question stem
-
1 Which feature of a paroxysmal attack is pathognomonic of PNES:
-
a preservation of consciousness during the event
-
b side-to-side head movement
-
c a seizure lasting more than 2 minutes
-
d there is not a single unique feature of PNES
-
e crying during an event.
-
-
2 As regards PNES and comorbid epilepsy:
-
a most patients with PNES also have epilepsy
-
b about 50% of patients with PNES also have epilepsy
-
c patients with an intellectual disability and PNES are less likely to have comorbid epilepsy
-
d 10% of patients with PNES also have epilepsy
-
e PNES and epilepsy never coincide.
-
-
3 Common interactional and linguistic features of patients with PNES include:
-
a discussing subjective seizure symptoms in great detail
-
b giving seizure description by negation (e.g. ‘I feel nothing’)
-
c easily focusing on a memorable seizure
-
d initiating discussions about seizures
-
e volunteering subjective symptoms of their seizures.
-
-
4 In terms of the management of PNES:
-
a delivering the diagnosis is an important therapeutic step
-
b withdrawing anti-epileptic medication following the diagnosis may be harmful
-
c there is good evidence for the use of selective serotonin reuptake inhibitors for PNES
-
d there are no randomised controlled trials on the management of PNES
-
e hypnosis should be the first-line treatment.
-
-
5 When considering possible predisposing factors for PNES:
-
a a history of trauma is rare
-
b most patients with PNES have a history of sexual abuse
-
c a history of minor head injury is unusual in patients with PNES
-
d a background of personality disorder is uncommon in patients with PNES
-
e physical or intellectual disability can contribute to someone’s vulnerability to develop PNES.
-
MCQ answers
| 1 | d | 2 | d | 3 | b | 4 | a | 5 | e |





eLetters
No eLetters have been published for this article.